Abstract
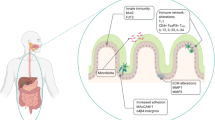
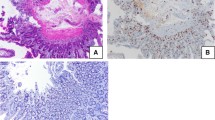
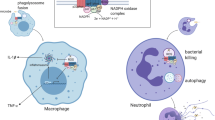
Megacolon is frequently observed in patients who develop the digestive form of Chagas disease. It is characterized by dilation of the rectum–sigmoid portion and thickening of the colon wall. Microscopically, the affected organ presents denervation, which has been considered as consequence of an inflammatory process that begins at the acute phase and persists in the chronic phase of infection. Inflammatory infiltrates are composed of lymphocytes, macrophages, natural killer cells, mast cells, and eosinophils. In this study, we hypothesized that mast cells producing tryptase could influence the migration and the activation of eosinophils at the site, thereby contributing to the immunopathology of the chronic phase. We seek evidence of interactions between mast cells and eosinophils through (1) evaluation of eosinophils, regarding the expression of PAR2, a tryptase receptor; (2) correlation analysis between densities of mast cells and eosinophils; and (3) ultrastructural studies. The electron microscopy studies revealed signs of activation of mast cells and eosinophils, as well as physical interaction between these cells. Immunohistochemistry and correlation analyses point to the participation of tryptase immunoreactive mast cells in the migration and/or survival of eosinophils at the affected organ.





Similar content being viewed by others
References
Albert EJ, Duplisea J, Dawicki W, Haidl ID, Marshall JS (2011) Tissue eosinophilia in a mouse model of colitis is highly dependent on TLR2 and independent of mast cells. Am J Pathol 178:150–160. doi:10.1016/j.ajpath.2010.11.041
Bolton SJ, Mcnulty CA, Thomas RJ, Hewitt CRA, Wardlaw AJ (2003) Expression of and functional responses to protease-activated receptors on human eosinophils. J Leukoc Biol 74:60–68. doi:10.1189/jlb.0702351.http
Christerson U, Keita AV, Söderholm JD, Gustafson-Svärd C (2009) Increased expression of protease-activated receptor-2 in mucosal mast cells in Crohn’s ileitis. J Crohns Colitis 3:100–108. doi:10.1016/j.crohns.2008.11.003
Cleator JH, Zhu WQ, Vaughan DE, Hamm HE (2006) Differential regulation of endothelial exocytosis of P-selectin and von Willebrand factor by protease-activated receptors and cAMP. Blood 107:2736–2744. doi:10.1182/blood-2004-07-2698
Côbo Ede C, Silveira TP, Micheletti AM, Crema E, Adad SJ (2012) Research on Trypanosoma cruzi and analysis of inflammatory infiltrate in esophagus and colon from chronic chagasic patients with and without mega. J Trop Med 232646. doi:10.1155/2012/232646
Cox G, Ohtoshi T, Vancheri C, Denburg JA, Dolovich J, Gauldie J, Jordana M (1991) Promotion of eosinophil survival by human bronchial epithelial cells and its modulation by steroids. Am J Respir Cell Mol Biol 4:525–531. doi:10.1165/ajrcmb/4.6.525
d’Avila Reis D, Lemos EM, Silva GC, Adad SJ, McCurley T, Correa-Oliveira R, Machado CR (2001) Phenotypic characterization of the inflammatory cells in chagasic megaoesophagus. Trans R Soc Trop Med Hyg 95:177–178
da Silveira ABM, Arantes RME, Vago AR, Lemos EM, Adad SJ, Correa-Oliveira R, d’Avila Reis D (2005) Comparative study of the presence of Trypanosoma cruzi kDNA, inflammation and denervation in chagasic patients with and without megaesophagus. Parasitology 131:627–634
da Silveira A, Lemos E, Adad SJ, Correa-Oliveira R, Furness JB, d’Avila Reis D (2007a) Megacolon in Chagas disease: a study of inflammatory cells, enteric nerves, and glial cells. Hum Pathol 38:1256–1264. doi:10.1016/j.humpath.2007.01.020
da Silveira ABM, Adad SJ, Correa-Oliveira R, Furness J, d’Avila Reis D (2007b) Morphometric study of eosinophils, mast cells, macrophages and fibrosis in the colon of chronic chagasic patients with and without megacolon. Parasitology 134:789–796. doi:10.1017/S0031182007002296
de Boer JD, Yang J, van den Boogaard FE, Hoogendijk AJ, de Beer R, van der Zee JS, van der Poll T (2014) Mast cell-deficient kit mice develop house dust mite-induced lung inflammation despite impaired eosinophil recruitment. J Innate Immun 6:219–226. doi:10.1159/000354984
Dias JCP (2006) Chagas disease: successes and challenges. Cad Saude Publica 22:2020–2021
Elishmereni M, Alenius HT, Bradding P, Mizrahi S, Shikotra A, Minai-Fleminger Y, Levi-Schaffer F (2011) Physical interactions between mast cells and eosinophils: a novel mechanism enhancing eosinophil survival in vitro. Allergy 66:376–385. doi:10.1111/j.1398-9995.2010.02494.x
Gleich GJ (2000) Mechanisms of eosinophil-associated inflammation. J Allergy Clin Immunol 105:651–663. doi:10.1067/mai.2000.105712
Gröger M, Klemens C, Wendt S, Becker S, Canis M, Havel M, Kramer MF (2012) Mediators and cytokines in persistent allergic rhinitis and nonallergic rhinitis with eosinophilia syndrome. Int Arch Allergy Immunol 159:171–178. doi:10.1159/000336169
Hogan SP (2007) Recent advances in eosinophil biology. Int Arch Allergy Immunol 143(Suppl):3–14. doi:10.1159/000101398
Hyun E, Andrade-Gordon P, Steinhoff M, Vergnolle N (2008) Protease-activated receptor-2 activation: a major actor in intestinal inflammation. Gut 57:1222–1229. doi:10.1136/gut.2008.150722
Itoh Y, Sendo T, Oishi R (2005) Physiology and pathophysiology of proteinase-activated receptors (PARs): role of tryptase/PAR-2 in vascular endothelial barrier function. J Pharmacol Sci 1:14–19
Jacobsen EA, Taranova AG, Lee NA, Lee JJ (2007) Eosinophils: singularly destructive effector cells or purveyors of immunoregulation? J Allergy Clin Immunol 119:1313–1320. doi:10.1016/j.jaci.2007.03.043
Kato M, Kephart GM, Talley NJ, Wagner JM, Sarr MG, Bonno M, Gleich GJ (1998) Eosinophil infiltration and degranulation in normal human tissue. Anat Rec 252:418–425
Köberle F (1968) Chagas’ disease and Chagas’ syndromes: the pathology of American trypanosomiasis. Adv Parasitol 6:63–116
Macedo AM, Machado CR, Oliveira RP, Pena SD (2004) Trypanosoma cruzi: genetic structure of populations and relevance of genetic variability to the pathogenesis of Chagas disease. Mem Inst 99:1–12
Malamud V, Vaaknin A, Abramsky O, Mor M, Burgess LE, Ben-Yehudah A, Lorberboum-Galski H (2003) Tryptase activates peripheral blood mononuclear cells causing the synthesis and release of TNF-α, IL-6 and IL-1β: possible relevance to multiple sclerosis. J Neuroimmunol 138:115–122. doi:10.1016/S0165-5728(03)00090-0
Manoel-Caetano FS, Silva AE (2007) Implications of genetic variability of Trypanosoma cruzi for the pathogenesis of Chagas disease. Cad Saude Publica 23:2263–2274
Martins PR, Nascimento RD, de Souza Lisboa A, Martinelli PM, d’Ávila Reis D (2014) Neuroimmunopathology of Trypanosoma cruzi-induced megaoesophagus: is there a role for mast cell proteases? Hum Immunol 75:302–305. doi:10.1016/j.humimm.2014.02.003
Matos NA, Silva JF, Matsui TC, Damasceno KA, Duarte IDG, Lemos VS, Klein A (2013) Mast cell tryptase induces eosinophil recruitment in the pleural cavity of mice via proteinase-activated receptor 2. Inflammation 36:1260–1267. doi:10.1007/s10753-013-9664-5
Meyer MC, Creer MH, Mchowat J, Maureen C (2005) Potential role for mast cell tryptase in recruitment of inflammatory cells to endothelium. Am J Physiol 63104:1485–1491. doi:10.1152/ajpcell.00215.2005
Miike S, Kita H (2003) Human eosinophils are activated by cysteine proteases and release inflammatory mediators. J Allergy Clin Immunol 111:704–713. doi:10.1067/mai.2003.1332
Miike S, McWilliam AS, Kita H (2001) Trypsin induces activation and inflammatory mediator release from human eosinophils through protease-activated receptor-2. J Immunol 167:6615–6622
Molina HA, Kierszenbaum F (1987) A study of human myocardial tissue in Chagas’ disease: distribution and frequency of inflammatory cell types. Int J Parasitol 17:1297–1305
Molina HA, Kierszenbaum F (1988) Kinetics of development of inflammatory lesions in myocardial and skeletal muscle in experimental Trypanosoma cruzi infection. J Parasitol 74:370–374
Molina HA, Kierszenbaum F (1989) Eosinophil activation in acute and chronic chagasic myocardial lesions and deposition of toxic eosinophil granule proteins on heart myofibers. J Parasitol 75:129–133
Nystedt S, Ramakrishnan V, Sundelin J (1996) The proteinase-activated receptor 2Is induced by inflammatory mediators in human endothelial cells. Comparison with the thrombin receptor. J Biol Chem 271:14910–14915. doi:10.1074/jbc.271.25.14910
Raithel M, Winterkamp S, Pacurar A, Ulrich P, Hochberger J, Hahn EG (2001) Release of mast cell tryptase from human colorectal mucosa in inflammatory bowel disease. Scand J Gastroenterol 36:174–179
Ramachandran R, Noorbakhsh F, Defea K, Hollenberg MD (2012) Targeting proteinase-activated receptors: therapeutic potential and challenges. Nat Rev Drug Discov 11:69–86. doi:10.1038/nrd3615
Rothenberg ME, Mishra A, Brandt EB, Hogan SP (2001) Gastrointestinal eosinophils. Immunol Rev 179:139–155
Schmidlin F, Amadesi S, Dabbagh K, Lewis DE, Knott P, Bunnett NW, Stevens ME (2002) Protease-activated receptor 2 mediates eosinophil infiltration and hyperreactivity in allergic inflammation of the airway. J Immunol 169:5315–5321
Shakoory B, Fitzgerald SM, Lee SA, Chi DS, Krishnaswamy G (2004) The role of human mast cell-derived cytokines in eosinophil biology. J Interferon Cytokine Res 24:271–281. doi:10.1089/107999004323065057
Smyth CM, Akasheh N, Woods S, Kay E, Morgan RK, Thornton MA, Costello RW (2013) Activated eosinophils in association with enteric nerves in inflammatory bowel disease. PLoS One 8:e64216. doi:10.1371/journal.pone.0064216
Stasikowska-Kanicka O, Danilewicz M, Głowacka A, Wągrowska-Danilewicz M (2012) Mast cells and eosinophils are involved in activation of ulcerative colitis. Adv Med Sci 57:230–236. doi:10.2478/v10039-012-0029-3
Steinhoff M, Vergnolle N, Young SH, Tognetto M, Amadesi S, Ennes HS, Bunnett NW (2000) Agonists of proteinase-activated receptor 2 induce inflammation by a neurogenic mechanism. Nat Med 6:151–158. doi:10.1038/72247
Stoyanova II, Gulubova MV (2002) Mast cells and inflammatory mediators in chronic ulcerative colitis. Acta Histochem 104:185–192. doi:10.1078/0065-1281-00641
Teixeira ARL, Hecht MM, Guimaro MC, Guimaro MC, Sousa AO, Nitz N (2011) Pathogenesis of chagas’ disease: parasite persistence and autoimmunity. Clin Microbiol Rev 24:592–630. doi:10.1128/CMR.00063-10
Vergnolle N (1999) Proteinase-activated receptor-2-activating peptides induce leukocyte rolling, adhesion, and extravasation in vivo. J Immunol 163:5064–5069
Vliagoftis H, Lacy P, Luy B, Adamko D, Hollenberg M, Befus D, Moqbel R (2004) Mast cell tryptase activates peripheral blood eosinophils to release granule-associated enzymes. Int Arch Allergy Immunol 135:196–204. doi:10.1159/000081304
Zhang A, Chi X, Luo G, Hei Z, Xia H, ss C, Xia Z (2013) Mast cell stabilization alleviates acute lung injury after orthotopic autologous liver transplantation in rats by downregulating inflammation. PLoS One 8:e75262. doi:10.1371/journal.pone.0075262
Acknowledgments
This work was supported by Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq) and Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES).
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Martins, P.R., Nascimento, R.D., Lopes, J.G. et al. Mast cells in the colon of Trypanosoma cruzi-infected patients: are they involved in the recruitment, survival and/or activation of eosinophils?. Parasitol Res 114, 1847–1856 (2015). https://doi.org/10.1007/s00436-015-4371-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00436-015-4371-9