Abstract
Purpose
To investigate the prevalence of human papillomavirus (HPV) in cervical samples of pregnant and non-pregnant women in South-Brazil.
Methods
A prospective study of 91 pregnant and 92 non-pregnant women with no previous history of cervical dysplasia or cancer was carried out. Cervical samples for HPV testing and cytology were collected in each trimester of pregnancy and in the puerperium for pregnant women and at matched intervals for the non-pregnant women. All samples were analyzed through PCR with consensus primers GP5+/GP6+. Genotyping was performed using specific primers. To control for confounding factors, the analysis of multivariate logistic regression was applied. The measure of odds ratio (OR) and the 95 % confidence interval (95 % CI) were used. The level of statistical significance was set at 5 % (P ≤ 0.05).
Results
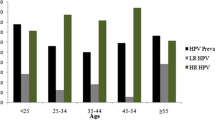
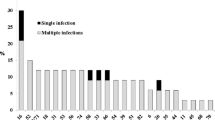
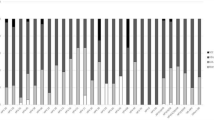
HPV DNA was detected in 23/91 (25.3 %) cervical samples from the pregnant women and in 12/92 (13 %) cervical samples from non-pregnant women (P = 0.035). There was a significant association among cervical HPV infection and young age, number of lifetime sexual partners, and the presence of abnormal cervical cytology. HPV16 and HPV18 were the viral types more frequently detected. Out of the 23 HPV-positive pregnant women, 17 (73.9 %) had normal cervical cytology.
Conclusion
Our results suggest a higher prevalence of HPV infection in pregnant vs. non-pregnant women. This finding may be related to the relative immunosuppression observed in pregnant women, outlining the importance of the appropriate monitoring of the viral infection in this specific population.
Similar content being viewed by others
References
International Agency for Research on Cancer IARC (1995). Human papillomaviruses. IARC monographs on the evaluation of carcinogenic risk to humans, vol 64. Lyon, France: I, 1995. Avaliable from http://monographs.iarc.fr/ENG/Monographs/vol64/. Cited 19 Feb 2014
zur Hausen H (2009) Papillomavirus in the causation of human cancers—a brief historical account. Virology 384:260–265
Wolf JK, Ramirez PT (2001) The molecular biology of cervical cancer. Cancer Invest 19(6):621–629
Loomis DM, Pastore PA, Rejman K, Gutierrez KL, Bethea B (2009) Cervical cytology in vulnerable pregnant women. J Am Acad Nurse Pract 21(5):287–294
Gajewska M, Marianowski L, Wielgos M, Malejczyk M, Majewski S (2005) The occurrence of genital types of human papillomavirus in normal pregnancy and in pregnant women with pregestational insulin dependent diabetes mellitus. Neuro Endocrinol Lett 26(6):766–770
Armbruster-Moraes E, Ioshimoto LM, Leao E, Zugaib M (2000) Prevalence of “high risk” human papillomavirus in the lower genital tract of Brazilian gravidas. Int J Gynecol Obstet 69(3):223–227
Chan PK, Chang AR, Tam WH, Cheung JL, Cheng AF (2002) Prevalence and genotype distribution of cervical human papillomavirus infection: comparison between pregnant women and non-pregnant controls. J Med Virol 67(4):583–588
Medeiros LR, Ethur ABM, Hilgert JB, Zanini RR, Berwanger O, Bozzetti MC et al (2005) Vertical transmission of the human papillomavirus: a systematic quantitative review. Cad Saude Publica 21(4):953–964
Richards B, Skoletsky J, Schuber AP, Balfour R, Stern RC, Dorkin RC et al (1993) Multiplex PCR amplification from the CFTR gene using DNA prepared from bucal brushes/swabs. Hum Mol Genet 2(2):159–163
Damin DC, Caetano MB, Rosito MA, Schwartsmann G, Damin AS, Frazzon AP et al (2007) Evidence for an association of human papillomavirus infection and colorectal cancer. Eur J Surg Oncol 33:569–574
Sotlar K, Diemer D, Dethleffs A, Hack Y, Stubner A, Vollmer N et al (2004) Detection and typing of human papillomavirus by E6 nested multiplex PCR. J Clin Microbiol 42(7):3176–3184
Creasman WT (2001) Cancer and pregnancy. Ann N Y Acad Sci 943:281–286
Instituto Nacional do Câncer – INCA. (2014) Brasil. Ministério da Saúde. Rio de Janeiro: INCA. Available from: http://www.inca.gov.br, http://www.inca.gov.br/estimativa/2014. Cited 19 Feb 2014
Bassal R, Schejter E, Bachar R, Shapira H, Sandbank J, Supino Rosin L et al (2014) Cervical Pap screening among Israeli women, 2005–2010. Arch Gynecol Obstet 289(3):615–622
Muñoz N (2000) Human papillomavirus and cancer: the epidemiological evidence. J Clin Virol 19(1–2):1–5
Fife KH, Katz BP, Roush J, Handy VD, Brown DR, Hansell R (1996) Cancer-associated human papillomavirus types are selectively increased in the cervix of women in the first trimester of pregnancy. Am J Obstet Gynecol 174(5):1487–1493
Morrison EA, Gammon MD, Goldberg GL, Vermund SH, Burk RD (1996) Pregnancy and cervical infection with human papillomaviruses. Int J Gynaecol Obstet 54(2):125–130
Nobbenhuis M, Helmerhorst TJM, van den Brule AJC, Rozendaal L, Bezemer PD, Voorhorst FJ et al (2002) High-risk human papillomavirus clearance in pregnant women: trends for lower clearance during pregnancy with a catch-up postpartum. Br J Cancer 87:75–80
Sethi S, Müller M, Schneider A, Blettner M, Smith E, Turek L et al (1998) Serologic response to the E4, E6 and E7 proteins of human papillomavirus type 16 in pregnant women. Am J Obstet Gynecol 178(2):360–364
Banura C, Franceschi S, van Doorn LJ, Arsian A, Kleter B, Wabwire-Mangen F et al (2008) Prevalence, incidence and clearance of human papillomavirus infection among young primiparous pregnant women in Kampala Uganda. Int J Cancer 123(9):2180–2187
Boyle DCM, Smith JR (1999) Infection and cervical intraepithelial neoplasia. Int J Gynecol Cancer 9:177–186
Spitzer M, Burk RD (2005) Human papillomavirus acog practice bulletin. clinical management guidelines for obstetrician-gynecologists. Obstet Gynecol 105(4):905–918
Acknowledgments
The authors thank the medical students Mauren Fronckowiak Salis and Razyane Audibert Silveira by the assistance in the Laboratory of Molecular Biology.
Conflict of interest
We declare that we have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Salcedo, M.M.B.P., Damin, A.P.S., Agnes, G. et al. Prevalence of human papillomavirus infection in pregnant versus non-pregnant women in Brazil. Arch Gynecol Obstet 292, 1273–1278 (2015). https://doi.org/10.1007/s00404-015-3752-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-015-3752-8