Abstract
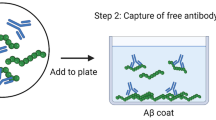
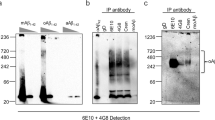
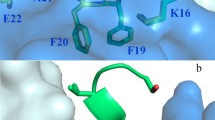
Reducing amyloid-β peptide (Aβ) burden at the pre-symptomatic stages of Alzheimer’s disease (AD) is currently the advocated clinical strategy for treating this disease. The most developed method for targeting Aβ is the use of monoclonal antibodies including bapineuzumab, solanezumab and crenezumab. We have synthesized these antibodies and used surface plasmon resonance (SPR) and mass spectrometry to characterize and compare the ability of these antibodies to target Aβ in transgenic mouse tissue as well as human AD tissue. SPR analysis showed that the antibodies were able to bind Aβ with high affinity. All of the antibodies were able to bind Aβ in mouse tissue. However, significant differences were observed in human brain tissue. While bapineuzumab was able to capture a variety of N-terminally truncated Aβ species, the Aβ detected using solanezumab was barely above detection limits while crenezumab did not detect any Aβ. None of the antibodies were able to detect any Aβ species in human blood. Immunoprecipitation experiments using plasma from AD subjects showed that both solanezumab and crenezumab have extensive cross-reactivity with non-Aβ related proteins. Bapineuzumab demonstrated target engagement with brain Aβ, consistent with published clinical data. Solanezumab and crenezumab did not, most likely as a result of a lack of specificity due to cross-reactivity with other proteins containing epitope overlap. This lack of target engagement raises questions as to whether solanezumab and crenezumab are suitable drug candidates for the preventative clinical trials for AD.




Similar content being viewed by others
References
Hardy J, Selkoe DJ (2002) The amyloid hypothesis of alzheimer’s disease: progress and problems on the road to therapeutics. Science 297:353–356. doi:10.1126/science.1072994
Masters CL, Cappai R, Barnham KJ, Villemagne VL (2006) Molecular mechanisms for alzheimer’s disease: implications for neuroimaging and therapeutics. J Neurochem 97:1700–1725
Miles LA, Crespi GAN, Doughty L, Parker MW (2013) Bapineuzumab captures the n-terminus of the alzheimer’s disease amyloid-beta peptide in a helical conformation. Sci Rep 3. http://www.nature.com/srep/2013/130218/srep01302/abs/srep01302.html#supplementary-information
Blennow K, Zetterberg H, Rinne JO et al (2012) Effect of immunotherapy with bapineuzumab on cerebrospinal fluid biomarker levels in patients with mild to moderate alzheimer disease. Arch Neurol 69:1002–1010. doi:10.1001/archneurol.2012.90
Rinne JO, Brooks DJ, Rossor MN et al (2010) 11c-pib pet assessment of change in fibrillar amyloid-β load in patients with alzheimer’s disease treated with bapineuzumab: a phase 2, double-blind, placebo-controlled, ascending-dose study. Lancet Neurol 9:363–372. doi:10.1016/S1474-4422(10)70043-0
Sperling R, Salloway S, Brooks DJ et al (2012) Amyloid-related imaging abnormalities in patients with alzheimer’s disease treated with bapineuzumab: a retrospective analysis. Lancet Neurol 11:241–249. doi:10.1016/s1474-4422(12)70015-7
Imbimbo BP, Ottonello S, Frisardi V et al (2012) Solanezumab for the treatment of mild-to-moderate alzheimer’s disease. Expert Rev Clin Immunol 8:135–149. doi:10.1586/eci.11.93
Seubert P, Barbour R, Khan K et al (2008) Antibody capture of soluble abeta does not reduce cortical abeta amyloidosis in the pdapp mouse. Neurodegener Dis 5:65–71. doi:10.1159/000112834
Citron M (2010) Alzheimer’s disease: strategies for disease modification. Nat Rev Drug Discov 9:387–398. doi:10.1038/nrd2896
DeMattos RB, Bales KR, Cummins DJ, Dodart JC, Paul SM, Holtzman DM (2001) Peripheral anti-a beta antibody alters cns and plasma a beta clearance and decreases brain a beta burden in a mouse model of alzheimer’s disease. Proc Natl Acad Sci USA 98:8850–8855. doi:10.1073/pnas.151261398
Mullard A (2012) Sting of alzheimer’s failures offset by upcoming prevention trials. Nat Rev Drug Discov 11:657–660. doi:10.1038/nrd3842
Adolfsson O, Pihlgren M, Toni N et al (2012) An effector-reduced anti-β-amyloid (aβ) antibody with unique aβ binding properties promotes neuroprotection and glial engulfment of aβ. J Neurosci 32:9677–9689. doi:10.1523/jneurosci.4742-11.2012
Reiman EM, Langbaum JB, Fleisher AS et al (2011) Alzheimer’s prevention initiative: a plan to accelerate the evaluation of presymptomatic treatments. J Alzheimers Dis 26(Suppl 3):321–329. doi:10.3233/jad-2011-0059
World Health Organisation (2008) Proposed inn: List 100. WHO Drug Inform 22
World Health Organisation (2011) Poposed inn: List 105. WHO Drug Inform 25
Schroeter S, Games KD (2008) Prevention and treatment of cerebral amyloid angiopathy: Us 12/106,206. US Patent Application
Bales KR, Demattos R, Holtzman DM, Paul SM, Tsurushita N, Vasquez M (2001) Humanized antibodies that sequester amyloid beta peptide. US Patent Application
Pfeifer A, Pihlgren M, Muhs AW, Ryan, Nicolau C, Greferath R (2008) Humanized antibodies to amyloid beta. US Patent Application
Kok WM, Scanlon DB, Karas JA et al (2009) Solid-phase synthesis of homodimeric peptides: Preparation of covalently-linked dimers of amyloid [small beta] peptide. Chem Commun. doi:10.1039/B912784D (6228-6230)
Watt AD, Perez KA, Rembach A et al (2013) Oligomers, fact or artefact? Sds-page induces dimerization of beta-amyloid in human brain samples. Acta Neuropathol 125:549–564. doi:10.1007/s00401-013-1083-z
Ellis KA, Bush AI, Darby D et al (2009) The australian imaging, biomarkers and lifestyle (aibl) study of aging: methodology and baseline characteristics of 1112 individuals recruited for a longitudinal study of alzheimer’s disease. Int Psychogeriatr 21:672–687. doi:10.1017/S1041610209009405
Villemagne VL, Perez KA, Pike KE et al (2010) Blood borne amyloid-beta dimer correlates with clinical markers of alzheimer’s disease. J Neurosci 30:6315–6322
Koenig T, Menze BH, Kirchner M et al (2008) Robust prediction of the mascot score for an improved quality assessment in mass spectrometric proteomics. J Proteome Res 7:3708–3717. doi:10.1021/pr700859x
Perkins DN, Pappin DJC, Creasy DM, Cottrell JS (1999) Probability-based protein identification by searching sequence databases using mass spectrometry data. Electrophoresis 20:3551–3567. doi:10.1002/(SICI)1522-2683(19991201)20:18<3551:AID-ELPS3551>3.0.CO;2-2
Kandimalla KK, Curran GL, Holasek SS, Gilles EJ, Wengenack TM, Poduslo JF (2005) Pharmacokinetic analysis of the blood-brain barrier transport of 125i-amyloid β protein 40 in wild-type and alzheimer’s disease transgenic mice (app, ps1) and its implications for amyloid plaque formation. J Pharmacol Exp Ther 313:1370–1378. doi:10.1124/jpet.104.081901
Blennow K, de Leon MJ, Zetterberg H (2006) Alzheimer’s disease. Lancet 368:387–403
Villemagne VL, Burnham S, Bourgeat P et al (2013) Amyloid β deposition, neurodegeneration, and cognitive decline in sporadic alzheimer’s disease: a prospective cohort study. Lancet Neurol 12:357–367. doi:10.1016/S1474-4422(13)70044-9
Selkoe DJ (2011) Resolving controversies on the path to alzheimer’s therapeutics. Nat Med 17:1060–1065
Sperling RA, Jack CR, Aisen PS (2011) Testing the right target and right drug at the right stage. Sci Transl Med 3:111–133. doi:10.1126/scitranslmed.3002609
Watt AD, Villemagne VL, Barnham KJ (2013) Metals, membranes, and amyloid-beta oligomers: key pieces in the alzheimer’s disease puzzle? J Alzheimers Dis 33(Suppl 1):283–293. doi:10.3233/jad-2012-129017
Pontecorvo M, Joshi A, Lu Met al. (2013) Relationship between solanezumab treatment and amyloid burden in mild to moderate ad patients. In: 7th Human Amyloid Imaging (HAI)
Vom Berg J, Prokop S, Miller KR et al (2012) Inhibition of il-12/il-23 signaling reduces alzheimer’s disease-like pathology and cognitive decline. Nat Med 18:1812–1819. doi:10.1038/nm.2965
Berglund L, Andrade J, Odeberg J, Uhlén M (2008) The epitope space of the human proteome. Protein Sci 17:606–613. doi:10.1110/ps.073347208
Bonnycastle LL, Mehroke JS, Rashed M, Gong X, Scott JK (1996) Probing the basis of antibody reactivity with a panel of constrained peptide libraries displayed by filamentous phage. J Mol Biol 258:747–762. doi:10.1006/jmbi.1996.0284
James LC, Roversi P, Tawfik DS (2003) Antibody multispecificity mediated by conformational diversity. Science 299:1362–1367. doi:10.1126/science.1079731
Acknowledgments
This work was funded by the National Health and Medical Research Council of Australia (NHMRC) and we thank the AIBL Flagship Study of Aging for the provision of blood samples. Funding was also received from the Victorian Government Operational Infrastructure Support Scheme to St Vincent’s Institute. D.B.A was supported by a Victoria Fellowship from the Victorian Government and a Leslie (Les) J. Fleming Churchill Fellowship from The Winston Churchill Memorial Trust. M.W.P. is an NHMRC Research Fellow.
Author information
Authors and Affiliations
Corresponding authors
Additional information
K. J. Barnham and L. A. Miles contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Watt, A.D., Crespi, G.A.N., Down, R.A. et al. Do current therapeutic anti-Aβ antibodies for Alzheimer’s disease engage the target?. Acta Neuropathol 127, 803–810 (2014). https://doi.org/10.1007/s00401-014-1290-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00401-014-1290-2