Abstract
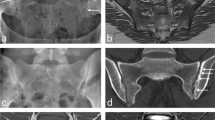
This case describes a 46-year-old woman with local pelvic and perineal pain, persisting for 2 years at presentation. The pain worsened during the night and morning and was alleviated during daily activities. Low back pain was associated with morning stiffness lasting longer than 2 h. Sometimes, she felt pain and numbness along her left S1 dermatome, without overt bladder or bowel incontinence. Lasegue’s sign was negative. Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) were elevated (35 mm/h and 9.4, respectively) and Mennel’s sign was present on both sides, indicating possible inflammation of the sacroiliac joints. However, radiographs of the lumbosacral spine and sacroiliac joints were normal. Magnetic resonance imaging (MRI) revealed a large spinal meningeal cyst in the sacrum (60 × 37 × 22 mm) consisting of multiple perineural cysts. The cyst eroded the surrounding sacral bone structures, narrowed several sacral foramina, and compressed neighboring nerve fibers. MRI findings on sacroiliac and hip joints were normal.
Zusammenfassung
In der vorliegenden Kasuistik geht es um eine 46 Jahre alte Frau mit lokalisierten Schmerzen im Becken- und Dammbereich, die bei Vorstellung seit 2 Jahren bestanden. Nachts und morgens nahmen die Schmerzen zu und verringerten sich am Tag. Die Lumbalgie ging mit Morgensteifigkeit für mehr als 2 h einher. Manchmal empfand die Patientin Schmerzen und ein Taubheitsgefühl im linken Dermatom S1, aber ohne Harn- oder Stuhlinkontinenz. Das Lasègue-Zeichen war negativ. Die Blutkörperchensenkungsgeschwindigkeit (BSG) und C-reaktives Protein (CRP) waren erhöht (35 mm/h bzw. 9,4) und das Mennel-Zeichen beidseits positiv, was auf eine mögliche Entzündung der Sakroiliakalgelenke hinweist. Die Röntgenaufnahmen der Lendenwirbelsäule und der Sakroiliakalgelenke waren jedoch unauffällig. Allerdings zeigte sich in der Magnetresonanztomographie (MRT) eine große spinale meningeale Zyste im Kreuzbein (60 × 37 × 22 mm), die aus mehreren perineuralen Zysten bestand. Durch die Zyste kam es zur Erosion der umgebenden Strukturen des Kreuzbeins, mehreren verengten Foramina sacralia und komprimierter benachbarter Nervenfasern. Die MRT-Befunde des Sakroiliakal- und Hüftgelenks waren normal.

Similar content being viewed by others
References
Tarlov IM (1938) Perineural cyst of the spinal nerve root. Arch Neurol Psychiatry 40:1067–1074
Park HJ, Jeon YH, Rho MH et al (2011) Incidental findings of the lumbar spine at MRI during herniated intervertebral disk disease evaluation. Am J Roentgenol 196:1151–1155
Paulsen RD, Call GA, Murtagh FR (1994) Prevalence and percutaneous drainage of cysts of the sacral nerve root sheet (Tarlov cysts). Am J Neuroradiol 15:293–299
Guo D, Shu K, Chen R et al (2007) Microsurgical treatment of symptomatic sacral perineural cysts. Neurosurgery 60:1059–1066
Lucantoni C, Than K, Wang A et al (2011) Tarlov cysts: a controversial lesion of the sacral spine. Neurosurg Focus 31(6):1–6
Sieper J, Heijde D van der, Landewe R et al (2009) New criteria for inflammatory back pain in patients with chronic back pain: a real patient exercise by experts from the Assessment of SpondyloArthritis international Society (ASAS). Ann Rheum Dis 68(6):784–788
Rudwaleit M, Metter A, Listing J et al (2006) Inflammatory back pain in ankylosing spondylitis: a reassessment of the clinical history for application as classification and diagnostic criteria. Arthritis Rheum 54(2):569–578
Calin A, Porta J, Fries JF et al (1977) Clinical history as screening test for ankylosing spondylitis. JAMA 237(24):2613–2614
Davis SW, Levy LM, LeBihan DJ et al (1993) Sacral meningeal cysts: evaluation with MR imaging. Radiology 187(2):445–448
Hiers RH, Long D, North RB et al (2010) Hiding in plain sight: a case of Tarlov perineural cyst. J Pain 11(9):833–837
Megalhaes E, Mecarenhas AM, Kraychete DC et al (2004) Gabapentin to treat sacral perineal cyst—induced pain. Case report. Rev Bras Anestesiol 54(1):73–77
North RB, Kidd DH, Farrokhi F et al (2005) Spinal cord stimulation versus repeated lumbosacral spine surgery for chronic pain: a randomized controlled trial. Neurosurgery 56:98–106
Sen RK, Goyal T, Tripathy SK et al (2012) Tarlov cysts: a report of two cases. J Orthop Surg 20(1):87–89
Caspar W, Papavero L, Nabhan A et al (2003) Microsurgical excision of symptomatic perineurial cysts: a study of 15 cases. Surg Neurol 59:101–106
Mummaneni PV, Pitts LH, McCormack BM et al (2000) Microsurgical treatment of symptomatic sacral Tarlov cysts. J Neurosurg 47:74–79
Compliance with ethical guidelines
Conflict of interest. P. Ostojic states that there are no conflicts of interest. The accompanying manuscript does not include studies on humans or animals.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ostojic, P. Sacral perineural cyst mimicking inflammatory low back pain. Z. Rheumatol. 74, 75–77 (2015). https://doi.org/10.1007/s00393-014-1507-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00393-014-1507-8