Abstract
Purpose
We evaluated the current practice of ultra-low anterior resection (uLAR) in patients with lower rectal cancer and compared uLARs using mostly transabdominal approach with or without intersphincteric resection (ISR).
Methods
A total of 624 consecutive lower rectal cancer patients undergoing curative uLAR were prospectively enrolled as ISR+ vs. ISR− groups (329 vs. 295 patients) between 2005 and 2012. The ISR+ group additionally received levator-sphincter reinforcement after distal resection.
Results
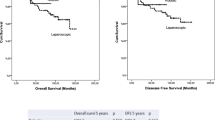
The circumferential resection margin (CRM) + rate (≤1 mm) was 2.1 % in the two groups. Postoperative ileus occurred more in the ISR– group than in the ISR+ group (p = 0.02). Substantial erectile dysfunction occurred 1.8 times more frequently in the ISR– group than in the ISR+ group (32 vs. 18.1 %; p = 0.01) among male patients at 2 years postoperatively. The urge to defecate volume and maximal tolerance volume, closely correlated with maximal squeezing pressure and/or mean resting pressure, did not differ between patients with and without chemoradiotherapy until 24 months postoperatively. Nevertheless, the urge to defecate volume was lesser in the ISR− group than in the ISR+ group at 24 months postoperatively (p = 0.022). For 301 patients in which >5 years had elapsed postoperatively, the mean 5-year local recurrence rate was 4.3 %, and the 5-year disease-free and overall survival rates were 78.9 and 92 %, respectively, without differences between the two groups.
Conclusions
Compared with uLAR without ISR, the transabdominal ISR with levator-sphincter reinforcement provides a safe resection plane with competent CRM, concurrently reduces substantial complications, and marginally promotes recovery of neorectal function.


Similar content being viewed by others
Abbreviations
- uLAR:
-
Ultra-low anterior resection
- SSO:
-
Sphincter-saving operation
- ISR:
-
Intersphincteric resection
- CRT:
-
Chemoradiotherapy
- AV:
-
Anal verge
- ECOG:
-
Eastern Cooperative Oncology Group
- CT:
-
Computed tomography
- MRI:
-
Magnetic resonance imaging
- EUS:
-
Endorectal ultrasonography
- FL:
-
5-fluoroural and leucovorin
- TME:
-
Total mesorectal excision
- CRM:
-
Circumferential resection margin
- OR:
-
Odds ratio
- CI:
-
Confidence interval
- LVI:
-
Lymphovascular invasion
- PNI:
-
Perineural invasion
- DFS:
-
Disease-free survival
- OS:
-
Overall survival
- s-CEA:
-
Serum carcinoembryonic antigen
- APR:
-
Abdominoperineal resection
References
Bokey EL (2013) Carcinoma of the rectum. In: Corman ML (ed) Colon and rectal surgery, 6th edn. Wolter Kluwer, Philadelphia, pp 864–990
Baik SH, Kim NK, Lee KY, Sohn SK, Cho CH (2005) Hand-sewn coloanal anastomosis for distal rectal cancer: long-term clinical outcomes. J Gastrointest Surg 9:775–780
Schiessel R, Karner-Hanusch J, Herbst F, Teleky B, Wunderlich M (1994) Intersphincteric resection for low rectal tumours. Br J Surg 81:1376–1378
Martin ST, Heneghan HM, Winter DC (2012) Systematic review of outcomes after intersphincteric resection for low rectal cancer. Br J Surg 99:603–612
Kim JC, Lim SB, Yoon YS, Park IJ, Kim CW, Kim CN (2014) Completely abdominal intersphincteric resection for lower rectal cancer: feasibility and comparison of robot-assisted and open surgery. Surg Endosc 28:2734–2744
Pucciani F (2013) A review on functional results of sphincter-saving surgery for rectal cancer: the anterior resection syndrome. Updates Surg 65:257–263
Kim JC, Yu CS, Lim SB, Kim CW, Kim JH, Kim TW (2013) Abdominoperineal resection and low anterior resection: comparison of long-term oncologic outcome in matched patients with lower rectal cancer. Int J Colorectal Dis 28:493–501
Kim JC, Kim CW, Yoon YS, Lee HO, Park IJ (2012) Levator-sphincter reinforcement after ultralow anterior resection in patients with low rectal cancer: the surgical method and evaluation of anorectal physiology. Surg Today 42:547–553
Jorge JM, Wexner SD (1993) Etiology and management of fecal incontinence. Dis Colon Rectum 36:77–97
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Goligher J, Duthie H (1984) Surgical anatomy and physiology of the anus, rectum and colon. In: Goligher J (ed) Surgery of the anus, rectum and colon, 5th edn. Ballière Tindall, London, pp 1–47
Stein E (2003) Anatomy of the anorectal region. In: Stein E (ed) Anorectal and colon disease, 1st edn. Springer, Berlin, pp 4–11
Tiret E, Poupardin B, McNamara D, Dehni N, Parc R (2003) Ultralow anterior resection with intersphincteric dissection—what is the limit of safe sphincter preservation? Colorectal Dis 5:454–457
Williams NS, Murphy J, Knowles CH (2008) Anterior perineal plane for ultra-low anterior resection of the rectum (the APPEAR technique): a prospective clinical trial of a new procedure. Ann Surg 247:750–758
Nagtegaal ID, Quirke P (2008) What is the role for the circumferential margin in the modern treatment of rectal cancer? J Clin Oncol 26:303–312
Trakarnsanga A, Gonen M, Shia J, Goodman KA et al (2013) What is the significance of the circumferential margin in locally advanced rectal cancer after neoadjuvant chemoradiotherapy? Ann Surg Oncol 20:1179–1184
Park JS, Huh JW, Park YA et al (2014) A circumferential resection margin of 1 mm is a negative prognostic factor in rectal cancer patients with and without neoadjuvant chemoradiotherapy. Dis Colon Rectum 57:933–940
Bown EJ, Lloyd GM, Boyle KM, Miller AS (2014) Rectal cancer: prognostic indicators of long-term outcome in patients considered for surgery. Int J Colorectal Dis 29:147–155
Akagi Y, Kinugasa T, Shirouzu K (2013) Intersphincteric resection for very low rectal cancer: a systematic review. Surg Today 43:838–847
Chang JS, Lee Y, Lim JS et al (2014) Preoperative chemoradiotherapy effects on anastomotic leakage after rectal cancer resection: a propensity score matching analysis. Ann Surg 259:516–521
Mirnezami A, Mirnezami R, Chandrakumaran K, Sasapu K, Sagar P, Finan P (2011) Increased local recurrence and reduced survival from colorectal cancer following anastomotic leak: systematic review and meta-analysis. Ann Surg 253:890–899
Kinugasa Y, Sugihara K (2009) Why does levator ani nerve damage occur during rectal surgery? J Clin Oncol 27:999–1000
Lange MM, van de Velde CJ (2011) Urinary and sexual dysfunction after rectal cancer treatment. Nat Rev Urol 8:51–57
Keating JP (2004) Sexual function after rectal excision. ANZ J Surg 74:248–259
Timmcke AE (1990) Objectives and methodology of manometry. In Smith LE (ed) Practical guideline to anorectal testing. 1st edn. Igaku-shoin, New York · Tokyo, pp 23-30
Loos M, Quentmeier P, Schuster T et al (2013) Effect of preoperative radio(chemo)therapy on long-term functional outcome in rectal cancer patients: a systematic review and meta-analysis. Ann Surg Oncol 20:1816–1828
Gamagami R, Istvan G, Cabarrot P, Liagre A, Chiotasso P, Lazorthes F (2000) Fecal continence following partial resection of the anal canal in distal rectal cancer: long-term results after coloanal anastomoses. Surgery 127:291–295
Saito N, Ito M, Kobayashi A et al (2014) Long-term outcomes after intersphincteric resection for low-lying rectal cancer. Ann Surg Oncol 21:3608–3615
Peng J, Sheng W, Huang D et al (2011) Perineural invasion in pT3N0 rectal cancer: the incidence and its prognostic effect. Cancer 117:1415–1421
Fujita S, Nakanisi Y, Taniguchi H et al (2007) Cancer invasion to Auerbach’s plexus is an important prognostic factor in patients with pT3-pT4 colorectal cancer. Dis Colon Rectum 50:1860–1866
Jessup JM, Thomas P (1998) CEA and metastasis: a facilitator or site-specific metastasis. In: Stanners CP (ed) Cell adhesion and communication mediated by the CEA family, 1st edn. Harwood Academic, Amsterdam, pp 195–223
Gastinger I, Marusch F, Steinert R et al (2005) Protective defunctioning stoma in low anterior resection for rectal carcinoma. Br J Surg 92:1137–1142
Acknowledgement
This work was supported by the Grants (to J. C. Kim) from the Korea Research Foundation (2013R1A2A1A03070986); Ministry of Science, ICT, and Future Planning; the Korea Health 21 R&D Project (HI06C0868 and HI13C1750), and the Center for Development and Commercialization of Anti-Cancer Therapeutics (HI10C2014), Ministry of Health and Welfare, Republic of Korea.
Conflict of interest
The authors declare that they have no competing interests.
Role of the funding source
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kim, J.C., Yu, C.S., Lim, SB. et al. Outcomes of ultra-low anterior resection combined with or without intersphincteric resection in lower rectal cancer patients. Int J Colorectal Dis 30, 1311–1321 (2015). https://doi.org/10.1007/s00384-015-2303-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-015-2303-x