Abstract
Introduction
Several operative techniques have been developed for the treatment of Hirschsprung’s disease (HD) in the past decades. Since one-stage transanal pull-through (TAPT) was first performed in 1998, multiple studies have shown favourable short-and midterm results compared to other techniques with shorter operation length, shorter hospital stay and lower complication rates. The aim of this meta-analysis was to determine the longterm results following TAPT for HD.
Methods
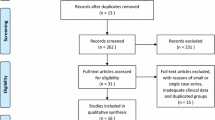
A systematic literature search for relevant articles was performed in four databases using the following terms “Hirschsprung/Hirschsprung’s disease”, “aganglionosis”, “transanal”, “pullthrough/pull-through”, “longterm/long-term” “results”, “follow-up” and “outcome”. A meta-analysis was conducted for relevant articles for one-stage transanal pull-through for HD with a minimal follow-up of median 36 months regarding constipation, incontinence/soiling, enterocolitis and secondary operations. Odds ratio (OR) with 95 % confidence intervals (CI) were calculated.
Results
Six studies with 316 patients matched the set criteria and were included in this analysis. Overall 45 (14.2 %) patients had disturbances of bowel function (OR 0.05, 95 % CI 0.03–0.07, p < 0.00001). Of these, 24 (53.3 %) patients experienced constipation, 8 (17.8 %) incontinence/soiling and 13 (28.9 %) enterocolitis. 10 (3.2 %) patients developed complications requiring secondary surgery. Most patients had a daily defecation frequency of 1–3 bowel movements 3 years postoperatively, resembling the stooling patterns of healthy controls.
Conclusion
Nearly 15 % of all patients operated with TAPT for HD continue to experience persistent bowel symptoms with constipation as the main problem. Further studies on the long-term outcome of children operated with this technique for HD are necessary to evaluate stooling patterns, urinary and sexual function as well as general quality of life during adolescence and adulthood.



Similar content being viewed by others
References
Dasgupta R, Langer JC (2008) Evaluation and management of persistent problems after surgery for Hirschsprung disease in a child. J Pediatr Gastroenterol Nutr 46(1):13–19. doi:10.1097/01.mpg.0000304448.69305.28
Swenson O, Bill AH Jr (1948) Resection of rectum and rectosigmoid with preservation of the sphincter for benign spastic lesions producing megacolon; an experimental study. Surgery 24(2):212–220
de La Torre-Mondragon L, Ortega-Salgado JA (1998) Transanal endorectal pull-through for Hirschsprung’s disease. J Pediatr Surg 33(8):1283–1286
Tannuri AC, Tannuri U, Romao RL (2009) Transanal endorectal pull-through in children with Hirschsprung’s disease–technical refinements and comparison of results with the Duhamel procedure. J Pediatr Surg 44(4):767–772. doi:10.1016/j.jpedsurg.2008.08.002
Kim AC, Langer JC, Pastor AC et al (2010) Endorectal pull-through for Hirschsprung’s disease-a multicenter, long-term comparison of results: transanal vs transabdominal approach. J Pediatr Surg 45(6):1213–1220. doi:10.1016/j.jpedsurg.2010.02.087
Dahal GR, Wang JX, Guo LH (2011) Long-term outcome of children after single-stage transanal endorectal pull-through for Hirschsprung’s disease. World J Pediatr 7(1):65–69. doi:10.1007/s12519-011-0247-y
Romero P, Kroiss M, Chmelnik M et al (2011) Outcome of transanal endorectal vs. transabdominal pull-through in patients with Hirschsprung’s disease. Langenbecks Arch Surg 396(7):1027–1033. doi:10.1007/s00423-011-0804-9
Chen Y, Nah SA, Laksmi NK et al (2013) Transanal endorectal pull-through versus transabdominal approach for Hirschsprung’s disease: a systematic review and meta-analysis. J Pediatr Surg 48(3):642–651. doi:10.1016/j.jpedsurg.2012.12.036
Mustafawi A, Hassan ME (2012) Quality of life and parents’ satisfaction with Duhamel’s versus transanal endorectal pull-through for the treatment of Hirschsprung’s disease in children. Ann Pediatr Surg 8(4):105–110. doi:10.1097/01.XPS.0000418468.33021.15
Gunnarsdottir A, Larsson LT, Arnbjornsson E (2010) Transanal endorectal vs. Duhamel pull-through for Hirschsprung’s disease. Eur J Pediatr Surg 20(4):242–246. doi:10.1055/s-0030-1252006
Ortiz-Rubio I, Pérez-Aguilera M, Granéli C et al (2013) literature review of the outcome after one-stage transanal endorectal pull-through procedure for Hirschsprung’s disease in children. Surg Sci 04(05):258–262. doi:10.4236/ss.2013.45050
Kim HY, Oh JT (2009) Stabilization period after 1-stage transanal endorectal pull-through operation for Hirschsprung disease. J Pediatr Surg 44(9):1799–1804. doi:10.1016/j.jpedsurg.2008.10.070
Khalil M (2015) Long-term health-related quality of life for patients with Hirschsprung’s disease at 5 years after transanal endorectal pull-through operation. Qual Life Res 24(11):2733–2738. doi:10.1007/s11136-015-1012-9
Kohno M, Ikawa H, Konuma K et al (2007) Is high amplitude propagated contraction present after transanal endorectal pull-through for Hirschsprung’s disease? Pediatr Surg Int 23(10):981–986. doi:10.1007/s00383-007-1981-z
Yang L, Tang ST, Cao GQ et al (2012) Transanal endorectal pull-through for Hirschsprung’s disease using long cuff dissection and short V-shaped partially resected cuff anastomosis: early and late outcomes. Pediatr Surg Int 28(5):515–521. doi:10.1007/s00383-012-3071-0
Dutta HK (2010) Clinical experience with a new modified transanal endorectal pull-through for Hirschsprung’s disease. Pediatr Surg Int 26(7):747–751. doi:10.1007/s00383-010-2629-y
Graneli C, Stenstrom P, Borjesson A et al (2015) Development of frequency of stools over time in children with Hirschsprung disease posttransanal endorectal one-stage pull-through. Eur J Pediatr Surg 25(4):359–364. doi:10.1055/s-0034-1376396
Yanchar NL, Soucy P (1999) Long-term outcome after Hirschsprung’s disease: patients’ perspectives. J Pediatr Surg 34(7):1152–1160
Aworanti OM, McDowell DT, Martin Im et al (2016) Does functional outcome improve with time postsurgery for Hirschsprung disease? Eur J Pediatr Surg 26(2):192–199. doi:10.1055/s-0034-1544053
Langer JC (2012) Laparoscopic and transanal pull-through for Hirschsprung disease. Semin Pediatr Surg 21(4):283–290. doi:10.1053/j.sempedsurg.2012.07.002
Conway SJ, Craigie RJ, Cooper LH et al (2007) Early adult outcome of the Duhamel procedure for left-sided Hirschsprung disease–a prospective serial assessment study. J Pediatr Surg 42(8):1429–1432. doi:10.1016/j.jpedsurg.2007.03.046
Heikkinen M, Rintala RJ, Louhimo I (1995) Bowel function and quality of life in adult patients with operated Hirschsprung’s disease. Pediatr Surg Int 10(5–6):342–344. doi:10.1007/BF00182219
Jarvi K, Laitakari EM, Koivusalo A et al (2010) Bowel function and gastrointestinal quality of life among adults operated for Hirschsprung disease during childhood: a population-based study. Ann Surg 252(6):977–981. doi:10.1097/SLA.0b013e3182018542
Ieiri S, Nakatsuji T, Akiyoshi J et al (2010) Long-term outcomes and the quality of life of Hirschsprung disease in adolescents who have reached 18 years or older–a 47-year single-institute experience. J Pediatr Surg 45(12):2398–2402. doi:10.1016/j.jpedsurg.2010.08.040
Zhang SC, Bai YZ, Wang W et al (2005) Stooling patterns and colonic motility after transanal one-stage pull-through operation for Hirschsprung’s disease in children. J Pediatr Surg 40(11):1766–1772. doi:10.1016/j.jpedsurg.2005.07.027
Athanasakos E, Starling J, Ross F et al (2006) An example of psychological adjustment in chronic illness: Hirschsprung’s disease. Pediatr Surg Int 22(4):319–325. doi:10.1007/s00383-006-1651-6
Ralls MW, Coran AG, Teitelbaum DH (2012) Reoperative surgery for Hirschsprung disease. Semin Pediatr Surg 21(4):354–363. doi:10.1053/j.sempedsurg.2012.07.011
Elhalaby EA, Hashish A, Elbarbary MM et al (2004) Transanal one-stage endorectal pull-through for Hirschsprung’s disease: a multicenter study. J Pediatr Surg 39(3):345–351 (discussion 345–51)
Mills JL, Konkin DE, Milner R et al (2008) Long-term bowel function and quality of life in children with Hirschsprung’s disease. J Pediatr Surg 43(5):899–905. doi:10.1016/j.jpedsurg.2007.12.038
Stensrud KJ, Emblem R, Bjornland K (2015) Anal endosonography and bowel function in patients undergoing different types of endorectal pull-through procedures for Hirschsprung disease. J Pediatr Surg 50(8):1341–1346. doi:10.1016/j.jpedsurg.2014.12.024
Ruttenstock E, Puri P (2010) Systematic review and meta-analysis of enterocolitis after one-stage transanal pull-through procedure for Hirschsprung’s disease. Pediatr Surg Int 26(11):1101–1105. doi:10.1007/s00383-010-2695-1
Ralls MW, Freeman JJ, Rabah R et al (2014) Redo pullthrough for Hirschsprung disease: a single surgical group’s experience. J Pediatr Surg 49(9):1394–1399. doi:10.1016/j.jpedsurg.2014.04.009
Fortuna RS, Weber TR, Tracy TF Jr et al (1996) Critical analysis of the operative treatment of Hirschsprung’s disease. Arch Surg 131(5):520–524 (discussion 524–525)
Nah SA, de Coppi P, Kiely EM et al (2012) Duhamel pull-through for Hirschsprung disease: a comparison of open and laparoscopic techniques. J Pediatr Surg 47(2):308–312. doi:10.1016/j.jpedsurg.2011.11.025
Pini-Prato A, Mattioli G, Giunta C et al (2010) Redo surgery in Hirschsprung disease: what did we learn? Unicentric experience on 70 patients. J Pediatr Surg 45(4):747–754. doi:10.1016/j.jpedsurg.2009.08.001
Wang NL, Lee HC, Yeh ML et al (2004) Experience with primary laparoscopy-assisted endorectal pull-through for Hirschsprung’s disease. Pediatr Surg Int 20(2):118–122. doi:10.1007/s00383-003-1102-6
Langer JC, Minkes RK, Mazziotti MV et al (1999) Transanal one-stage Soave procedure for infants with Hirschsprung’s disease. J Pediatr Surg 34(1):148–151 (discussion 152)
de La Torre L, Langer JC (2010) Transanal endorectal pull-through for Hirschsprung disease: technique, controversies, pearls, pitfalls, and an organized approach to the management of postoperative obstructive symptoms. Semin Pediatr Surg 19(2):96–106. doi:10.1053/j.sempedsurg.2009.11.016
Wester T, Rintala RJ (2004) Early outcome of transanal endorectal pull-through with a short muscle cuff during the neonatal period. J Pediatr Surg 39(2):157–160 (discussion 157–60)
Dickie BH, Webb KM, Eradi B et al (2014) The problematic Soave cuff in Hirschsprung disease: manifestations and treatment. J Pediatr Surg 49(1):77–80. doi:10.1016/j.jpedsurg.2013.09.034 (discussion 80–1)
Gunnarsdottir A, Sandblom G, Arnbjornsson E et al (2010) Quality of life in adults operated on for Hirschsprung disease in childhood. J Pediatr Gastroenterol Nutr 51(2):160–166. doi:10.1097/MPG.0b013e3181cac1b6
Neuvonen MI, Kyrklund K, Lindahl HG et al (2015) A population-based, complete follow-up of 146 consecutive patients after transanal mucosectomy for Hirschsprung disease. J Pediatr Surg 50(10):1653–1658. doi:10.1016/j.jpedsurg.2015.02.006
Neuvonen MI, Kyrklund K, Rintala RJ et al (2016) Bowel function and quality of life after transanal endorectal pull-through for Hirschsprung disease: controlled outcomes up to adulthood. Ann Surg. doi:10.1097/SLA.0000000000001695
Xiong X, Chen X, Wang G et al (2015) Long term quality of life in patients with Hirschsprung’s disease who underwent heart-shaped anastomosis during childhood: a twenty-year follow-up in China. J Pediatr Surg 50(12):2044–2047. doi:10.1016/j.jpedsurg.2015.08.027
Zhang SC, Bai YZ, Wang W et al (2007) Long-term outcome, colonic motility, and sphincter performance after Swenson’s procedure for Hirschsprung’s disease: a single-center 2-decade experience with 346 cases. Am J Surg 194(1):40–47. doi:10.1016/j.amjsurg.2006.10.018
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Zimmer, J., Tomuschat, C. & Puri, P. Long-term results of transanal pull-through for Hirschsprung’s disease: a meta-analysis. Pediatr Surg Int 32, 743–749 (2016). https://doi.org/10.1007/s00383-016-3908-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-016-3908-z