Abstract
Background
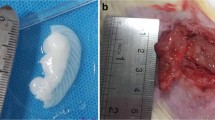
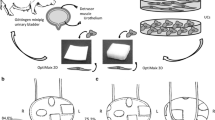
Finding a proper scaffold for augmentation is a serious challenge in bladder tissue engineering. We hereby aimed to determine the histological aspects of a decellularized colon graft for bladder augmentation in healthy rats.
Methods
Rat colon tissues were decellularized using perfusion-based method. After partial cystectomy, bladders were grafted with a patch of decellularized colon. Bladder specimens were investigated in 12 rats at 1, 3, and 9 months postoperatively for further histological changes and immunohistochemistry analyses were also performed.
Results
One month after implantation, partial seeding of new cells was observed. After 3 months continuity of transitional epithelium of natural bladder on the decellularized grafted colon tissue was confirmed with histological and immunohistochemical examinations. All augmented bladders demonstrated a spherical shape without stone formation, necrosis or graft rejection. The presence of urothelium with similar morphology to the natural urothelium and visible blood vessels were found within 3 months of operation. All immunohistochemical markers (except markers of colonic stem cells) were expressed in biopsies obtained 3 months after surgery demonstrating a progressive vascular and smooth muscle cell infiltration into the graft after implantation.
Conclusion
This study suggests that decellularized colon may provide a viable material for bladder augmentation in rats to pave the road for future applications of this natural collagen scaffold.





Similar content being viewed by others
Abbreviations
- α-SMA:
-
α-Smooth muscle actin
- BAMG:
-
Bladder acellular matrix graft
- ECM:
-
Extra cellular matrix
- H&E:
-
Hematoxylin and eosin
- IHC:
-
Immunohistochemical
- PBS:
-
Phosphate buffered saline
- SDS:
-
Sodium dodecyl sulfate
- sGAG:
-
Sulfated glycosaminoglycan
- SIS:
-
Small intestinal submucosa
- RQ-TRAP:
-
Real-time quantitative telomerase repeat amplification protocol
References
Biers SM, Venn SN, Greenwell TJ (2012) The past, present and future of augmentation cystoplasty. BJU Int 109(9):1280–1293. doi:10.1111/j.1464-410X.2011.10650.x
Gilbert SM, Hensle TW (2005) Metabolic consequences and long-term complications of enterocystoplasty in children: a review. J Urol 173(4):1080–1086. doi:10.1097/01.ju.0000155248.57049.4e
Ayyildiz A, Akgul KT, Huri E, Nuhoglu B, Kilicoglu B, Ustun H, Gurdal M, Germiyanoglu C (2008) Use of porcine small intestinal submucosa in bladder augmentation in rabbit: long-term histological outcome. ANZ J Surg 78(1–2):82–86. doi:10.1111/j.1445-2197.2007.04361.x
Song L, Murphy SV, Yang B, Xu Y, Zhang Y, Atala A (2014) Bladder acellular matrix and its application in bladder augmentation. Tissue Eng Part B Rev 20(2):163–172. doi:10.1089/ten.TEB.2013.0103
Elbahnasy AM, Shalhav A, Hoenig DM, Figenshau R, Clayman RV (1998) Bladder wall substitution with synthetic and non-intestinal organic materials. J Urol 159(3):628–637
Atala A, Bauer SB, Soker S, Yoo JJ, Retik AB (2006) Tissue-engineered autologous bladders for patients needing cystoplasty. Lancet 367(9518):1241–1246. doi:10.1016/S0140-6736(06)68438-9
Atala A (2011) Tissue engineering of human bladder. Br Med Bull 97:81–104. doi:10.1093/bmb/ldr003
Joseph DB, Borer JG, De Filippo RE, Hodges SJ, McLorie GA (2014) Autologous cell seeded biodegradable scaffold for augmentation cystoplasty: phase II study in children and adolescents with spina bifida. J Urol 191(5):1389–1395. doi:10.1016/j.juro.2013.10.103
Horst M, Madduri S, Gobet R, Sulser T, Milleret V, Hall H, Atala A, Eberli D (2013) Engineering functional bladder tissues. J Tissue Eng Regen Med 7(7):515–522. doi:10.1002/term.547
Kajbafzadeh AM, Masoumi A, Hosseini M, Borjian MA, Akbarzadeh A, Mohseni MJ (2014) Sheep colon acellular matrix: immunohistologic, biomechanical, scanning electron microscopic evaluation and collagen quantification. J Biosci Bioeng 117(2):236–241. doi:10.1016/j.jbiosc.2013.07.006
Badylak SF, Weiss DJ, Caplan A, Macchiarini P (2012) Engineered whole organs and complex tissues. Lancet 379(9819):943–952. doi:10.1016/S0140-6736(12)60073-7
Probst M, Dahiya R, Carrier S, Tanagho EA (1997) Reproduction of functional smooth muscle tissue and partial bladder replacement. Br J Urol 79(4):505–515
Kajbafzadeh AM, Payabvash S, Salmasi AH, Sadeghi Z, Elmi A, Vejdani K, Tavangar SM, Tajik P, Mahjoub F (2007) Time-dependent neovasculogenesis and regeneration of different bladder wall components in the bladder acellular matrix graft in rats. J Surg Res 139(2):189–202. doi:10.1016/j.jss.2006.11.003
Lin HK, Godiwalla SY, Palmer B, Frimberger D, Yang Q, Madihally SV, Fung KM, Kropp BP (2014) Understanding roles of porcine small intestinal submucosa in urinary bladder regeneration: identification of variable regenerative characteristics of small intestinal submucosa. Tissue Eng Part B Rev 20(1):73–83. doi:10.1089/ten.TEB.2013.0126
Sutherland RS, Baskin LS, Hayward SW, Cunha GR (1996) Regeneration of bladder urothelium, smooth muscle, blood vessels and nerves into an acellular tissue matrix. J Urol 156(2 Pt 2):571–577
Zhang Y, Frimberger D, Cheng EY, Lin HK, Kropp BP (2006) Challenges in a larger bladder replacement with cell-seeded and unseeded small intestinal submucosa grafts in a subtotal cystectomy model. BJU Int 98(5):1100–1105. doi:10.1111/j.1464-410X.2006.06447.x
Zhang F, Liao L (2014) Tissue engineered cystoplasty augmentation for treatment of neurogenic bladder using small intestinal submucosa: an exploratory study. J Urol 192(2):544–551. doi:10.1016/j.juro.2014.01.116
Schaefer M, Kaiser A, Stehr M, Beyer HJ (2013) Bladder augmentation with small intestinal submucosa leads to unsatisfactory long-term results. J Pediatr Urol 9(6 Pt A):878–883. doi:10.1016/j.jpurol.2012.12.001
Ashley RA, Roth CC, Palmer BW, Kibar Y, Routh JC, Fung KM, Frimberger D, Lin HK, Kropp BP (2010) Regional variations in small intestinal submucosa evoke differences in inflammation with subsequent impact on tissue regeneration in the rat bladder augmentation model. BJU Int 105(10):1462–1468. doi:10.1111/j.1464-410X.2009.08965.x
Tu DD, Chung YG, Gil ES, Seth A, Franck D, Cristofaro V, Sullivan MP, Di Vizio D, Gomez P, Adam RM, Kaplan DL, Estrada CR, Mauney JR (2013) Bladder tissue regeneration using acellular bi-layer silk scaffolds in a large animal model of augmentation cystoplasty. Biomaterials 34(34):8681–8689. doi:10.1016/j.biomaterials.2013.08.001
Kajbafzadeh AM, Esfahani SA, Sadeghi Z, Elmi A, Monajemzadeh M (2012) Application of different scaffolds for bladder wall regeneration: the bladder as a natural bioreactor. Tissue Eng Part A 18(7–8):882–887. doi:10.1089/ten.TEA.2011.0202
Sloff M, Simaioforidis V, de Vries R, Oosterwijk E, Feitz W (2014) Tissue engineering of the bladder—reality or myth? A systematic review. J Urol 192(4):1035–1042. doi:10.1016/j.juro.2014.03.116
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Funding
This work received no funding from any extra-institutional or commercial source.
Ethical approval
All applicable international, national, and institutional guidelines for the care and use of animals were followed. Principles of laboratory animal care were followed and the Animal Ethics Committee of the Tehran University of Medical Sciences, School of Medicine and Education Section of Basic Sciences, approved the animal selection, managements and surgical protocols.
Rights and permissions
About this article
Cite this article
Kajbafzadeh, AM., Khorramirouz, R., Sabetkish, S. et al. In vivo regeneration of bladder muscular wall using decellularized colon matrix: an experimental study. Pediatr Surg Int 32, 615–622 (2016). https://doi.org/10.1007/s00383-016-3871-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-016-3871-8