Abstract
Purpose
Hydranencephaly is a congenital condition characterized by the complete or near-complete absence of the cerebral cortex and basal ganglia, while central diabetes insipidus (CDI) is a condition characterized by the inability to concentrate urine due to a deficiency in antidiuretic hormone (ADH). CDI is known to occur in midline congenital malformations such as holoprosencephaly and septo-optic dysplasia, but its association with hydranencephaly is less well-established.
Methods
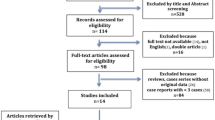
We reported two cases of hydranencephaly complicated by CDI. We also performed a systematic review of the SCOPUS and PubMed databases for case reports and case series of patients with hydranencephaly and CDI, and compiled data on the clinical features and treatment options.
Results
Seven cases of hydranencephaly complicated by CDI were identified from the systematic review in addition to the two cases reported here, resulting in a total of nine cases. The patients’ age ranged from 4 days to 4 years, and there was a female sex predilection (3.5:1). Patients most commonly presented with macrocephaly, developmental delay, and seizures, with dysmorphic features noted in 33%. In addition to CDI, other endocrinologic derangements included hypothyroidism (22%), hypocortisolemia (22%), and panhypopituitarism (22%). CDI was treated using sublingual or oral desmopressin while hypopituitarism was treated with the appropriate hormone replacement therapy. Insertion of a ventriculoperitoneal (VP) shunt was reported in 44% of cases.
Conclusion
The case reports and systematic review suggest a previously unknown association between hydranencephaly and CDI. Clinicians managing cases of hydranencephaly are advised to have a high index of suspicion for CDI in patients presenting with the characteristic signs and symptoms.



Similar content being viewed by others
References
Chinsky JM (2012) Hydranencephaly: transillumination may not illuminate diagnosis. Neoreviews 13:e233–e240. https://doi.org/10.1542/neo.13-4-e233
Quek Y-W, Su P-H, Tsao T-F, Chen JY, Ng YY, Hu JM, Chen SJ (2008) Hydranencephaly associated with interruption of bilateral internal carotid arteries. Pediatr Neonatol 49:43–47. https://doi.org/10.1016/S1875-9572(08)60011-X
Segawa Y, Itokazu N, Hirose A, Nakagawa S, Takashima S (2007) A case of partial 14q- with facial features of holoprosencephaly and hydranencephaly. Pediatr Neurol 37:51–54. https://doi.org/10.1016/j.pediatrneurol.2007.02.010
Dublin AB, French BN (1980) Diagnostic image evaluation of hydranencephaly and pictorially similar entities, with emphasis on computed tomography. Radiology 137:81–91. https://doi.org/10.1148/radiology.137.1.7422865
Kelly TG, Sharif UM, Southern JF, Gururajan K, Segall HD (2011) An unusual case of hydranencephaly presenting with an anterior midline cyst, a posterior calcified mass, cerebellar hypoplasia and occlusion of the posterior cerebral arteries. Pediatr Radiol 41:274–277. https://doi.org/10.1007/s00247-010-1894-1
Cecchetto G, Milanese L, Giordano R, Viero A, Suma V, Manara R (2013) Looking at the missing brain: hydranencephaly case series and literature review. Pediatr Neurol 48:152–158. https://doi.org/10.1016/j.pediatrneurol.2012.10.009
Dabrowski E, Kadakia R, Zimmerman D (2016) Diabetes insipidus in infants and children. Best Pract Res Clin Endocrinol Metab 30:317–328. https://doi.org/10.1016/j.beem.2016.02.006
Kasim N, Bagga B, Diaz-Thomas A (2018) Intracranial pathologies associated with central diabetes insipidus in infants. J Pediatr Endocrinol Metab 31:951–958. https://doi.org/10.1515/jpem-2017-0300
Di Iorgi N, Napoli F, Allegri AEM et al (2012) Diabetes insipidus: diagnosis and management. Horm Res Paediatr 77:69–84. https://doi.org/10.1159/000336333
Pavone P, Praticò AD, Vitaliti G, Ruggieri M, Rizzo R, Parano E, Pavone L, Pero G, Falsaperla R (2014) Hydranencephaly: cerebral spinal fluid instead of cerebral mantles. Ital J Pediatr 40:79. https://doi.org/10.1186/s13052-014-0079-1
Santiprabhob J, Likitmaskul S, Boonyasiri A, Boonsathorn S, Buddawong T (2005) Etiologies of central diabetes insipidus in Thai children. J Pediatr Endocrinol Metab 18:653–661
Wang LC, Cohen ME, Duffner PK (1994) Etiologies of central diabetes insipidus in children. Pediatr Neurol 11:273–277. https://doi.org/10.1016/0887-8994(94)90001-9
Poe LB, Coleman L (1989) MR of hydranencephaly. Am J Neuroradiol 10:S61
Negi M, Kobayashi D, Kumagai J, Kuroiwa T, Shiraishi J, Takemura T, Irahara K, Hayashi M, Eishi Y (2010) An autopsy case of congenital hydrocephalus and severe thinning of the cerebral cortex in a 4-year-old boy. Neuropathology 30(5):559–563. https://doi.org/10.1111/j.1440-1789.2010.01138.x
Marin G, Baspineiro B, Vilca I (2018) Treatment with sublingual desmopressin in two infants with hydranencephaly and central diabetes insipidus. Arch Argent Pediatr 116:e93–e97. https://doi.org/10.5546/aap.2018.e93
Omar AT, Khu KO (2019) Hydranencephaly complicated by central diabetes insipidus: report of two cases and systematic review of literature. Childs Nerv Syst (in review)
Krebs VLJ, Damiani D, Albuquerque Diniz EM et al (1998) Central diabetes insipidus as a complication of neonatal pathology: report of three cases. Pediatr Int 40:146–149. https://doi.org/10.1111/j.1442-200X.1998.tb01900.x
Borenstein-Levin L, Koren I, Kugelman A, Bader D, Toropine A, Riskin A (2014) Post-hemorrhagic hydrocephalus and diabetes insipidus in preterm infants. J Pediatr Endocrinol Metab 27(11-12):1261–1263. https://doi.org/10.1515/jpem-2014-0098
Antunes JL, Muraszko K (1990) The vascular supply of the hypothalamus-pituitary axis. In: Neuroendocrinological aspects of neurosurgery. Springer Vienna, Vienna, pp 42–47
Karadag A, Erdeve O, Atasay B, Arsan S, Deda G, Ince E, Ocal G, Berberoglu M (2006) Isolated central diabetes insipidus in a newborn with congenital toxoplasmosis. J Pediatr Endocrinol Metab 19(2):173–175. https://doi.org/10.1515/JPEM.2006.19.2.173
Jones G, Muriello M, Patel A, Logan L (2015) Enteroviral meningoencephalitis complicated by central diabetes insipidus in a neonate: a case report and review of the literature. J Pediatric Infect Dis Soc 4:155–158. https://doi.org/10.1093/jpids/pit055
Torres MDAM, Kazee MDAM, Simon MDH et al (2000) Central diabetes insipidus due to herpes simplex in a patient immunosuppressed by Cushing’s syndrome. Endocr Pract 6:26–28. https://doi.org/10.4158/EP.6.1.26
Ribeiro S, Domingues V, Faria RM, Mendonca T (2013) Invasive pneumococcal disease complicated by cerebral vasculitis, transient diabetes insipidus and spondylodiscitis. Case Reports 2013:bcr2013010336–bcr2013010336. https://doi.org/10.1136/bcr-2013-010336
Juffermans NP, Verbon A, Van der Poll T (2002) Diabetes insipidus as a complication of cryptococcal meningitis in an HIV-infected patient. Scand J Infect Dis 34:397–398
Chellen S, Whittaker E, Eisenhut M, Grandjean L (2018) Cerebral tuberculomas in a 6-year-old girl causing central diabetes insipidus. BMJ Case Rep 2018:bcr-2018-226590. https://doi.org/10.1136/bcr-2018-226590
Malhotra A, Bajpai A, Hunt RW (2010) Central diabetes insipidus in association with neonatal brain abscess. J Pediatr Endocrinol Metab 23(3):235–236. https://doi.org/10.1515/JPEM.2010.23.3.235
Dribin T, McAdams RM (2014) A neonate with gastroschisis and hydrocephalus complicated by central diabetes insipidus. J Pediatr Surg Case Rep 2:366–368. https://doi.org/10.1016/j.epsc.2014.07.011
Menzies DG, Shaw JF, Kean DM, Campbell IW (1988) Cranial diabetes insipidus secondary to arrested hydrocephalus. Postgrad Med J 64:300–302. https://doi.org/10.1136/pgmj.64.750.300
Merker B (2008) Life expectancy in hydranencephaly. Clin Neurol Neurosurg 110:213–214. https://doi.org/10.1016/j.clineuro.2007.11.011
Acknowledgments
The authors would like to thank Dr. Juan Silvestre G. Pascual for contributing the cases reported in the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Omar, A.T., Khu, K.J.O. Hydranencephaly complicated by central diabetes insipidus: report of two cases and systematic review of literature. Childs Nerv Syst 35, 1165–1171 (2019). https://doi.org/10.1007/s00381-019-04137-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-019-04137-9