Abstract
Purpose
The increased efficacy of cancer treatments has led to a greater survival rate of patients with pediatric brain cancers. Therefore, it is imperative to explore the long-term consequences of therapies employed to treat pediatric brain tumors. The goal of this study was to provide a review of literature regarding the downstream psychological and psychiatric consequences experienced by adult survivors of pediatric brain cancer as a result of treatment, tumor type, or tumor location.
Methods
A PubMed MeSH search and additional online database searches were conducted to include pertinent studies that discussed psychological deficits in childhood brain cancer survivors. The studies included were subjected to data extraction to quantify relevant information for further analysis.
Results
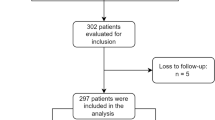
A total of 17 papers with 5320 pediatric brain tumor patients were incorporated in our review. Mean age at diagnosis (8.13 ± 0.77 years), mean follow-up time (9.98 ± 3.05 years), and male-to-female ratios (1.08:1) were compiled from studies reporting this information. Incidences of depression (19 %), anxiety (20 %), suicidal ideation (10.9 %), schizophrenia and its related psychoses (9.8 %), and behavioral problem (28.7 %) were higher among pediatric brain cancer survivors than in the normal population. Craniospinal radiotherapy and/or surgery corresponded to an increased likelihood of developing adverse deficits. Astrocytomas or other glial tumors were linked to poorer outcomes.
Conclusion
Physicians treating pediatric brain tumor patients should be aware of the possible consequences associated with treatment. Psychiatric monitoring is warranted in survivors of pediatric brain tumors, but further investigation is needed to elucidate late outcomes regarding tumor type and location.





Similar content being viewed by others
References
Bamford FN, Jones PM, Pearson D, Ribeiro GG, Shalet SM, Beardwell CG (1976) Residual disabilities in children treated for intracranial space-occupying lesions. Cancer 37:1149–1151
Brinkman TM, Liptak CC, Delaney BL, Chordas CA, Muriel AC, Manley PE (2013) Suicide ideation in pediatric and adult survivors of childhood brain tumors. J Neurooncol 113:425–432
Carpentieri SC, Meyer EA, Delaney BL, Victoria ML, Gannon BK, Doyle JM et al (2003) Psychosocial and behavioral functioning among pediatric brain tumor survivors. J Neurooncol 63:279–287
CBTRUS. Statistical report: primary brain tumors in the United States, 2012. Source: Central Brain Tumor Registry of the United States, Hinsdale, IL. (www.cbtrus.org/2012…/CBTRUS_Report_2004-2008_3-23-2012.pdf). Accessed 14 April 2014
Daszkiewicz P, Maryniak A, Roszkowski M, Barszcz S (2009) Long term functional outcome of surgical treatment of juvenile pilocytic astrocytoma of the cerebellum in children. Childs Nerv Syst 25:855–860
De Smet HJ, Paquier P, Verhoeven J, Mariën P (2013) The cerebellum: its role in language and related cognitive and affective functions. Brain Lang 127:334–342
Foreman NK, Faestel PM, Pearson J, Disabato J, Poole M, Wilkening G et al (1999) Health status in 52 long-term survivors of pediatric brain tumors. J Neurooncol 41:47–53
Frange P, Alapetite C, Gaboriaud G, Bours D, Zucker JM, Zerah M et al (2009) From childhood to adulthood: long-term outcome of medulloblastoma patients. The Institut Curie Experience (1980–2000). J Neurooncol 95:271–279
Hewitt M, Weiner SL (2003) Simone JV (eds): Childhood cancer survivorship: improving care and quality of life. National Academies Press, Washington, DC
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5:13
Knab B, Connell PP (2007) Radiotherapy for pediatric brain tumors: when and how. Expert Rev Anticancer Ther 7:S69–S77
Lannering B, Marky I, Lundberg A, Olsson E (1990) Long-term sequelae after pediatric brain tumors: their effect on disability and quality of life. Med Pediatr Oncol 18:304–310
Oeffinger KC, Mertens AC, Sklar CA, Kawashima T, Hudson MM, Meadows AT et al (2006) Chronic health conditions in adult survivors of childhood cancer. N Engl J Med 355:1572–1582
Radcliffe J, Bennett D, Kazak AE, Foley B, Phillips PC (1996) Adjustment in childhood brain tumor survival: child, mother, and teacher report. J Pediatr Psychol 21:529–539
Recklitis CJ, Diller LR, Li X, Najita J, Robison LL, Zeltzer L (2010) Suicide ideation in adult survivors of childhood cancer: a report from the childhood cancer survivor study. J Clin Oncol 28:655–661
Ross L, Johansen C, Dalton SO, Mellemkjaer L, Thomassen LH, Mortensen PB et al (2003) Psychiatric hospitalizations among survivors of cancer in childhood or adolescence. N Engl J Med 349:650–657
Sands SA, Milner JS, Goldberg J, Mukhi V, Moliterno JA, Maxfield C et al (2005) Quality of life and behavioral follow-up study of pediatric survivors of craniopharyngioma. J Neurosurg 103:302–311
Sands SA, Zhou T, O'Neil SH, Patel SK, Allen J, McGuire Cullen P et al (2012) Long-term follow-up of children treated for high-grade gliomas: Children’s Oncology Group L991 Final Study Report. J Clin Oncol 30:943–949
Schultz KA, Ness KK, Whitton J, Recklitis C, Zebrack B, Robison LL et al (2007) Behavioral and social outcomes in adolescent survivors of childhood cancer: a report from the Childhood Cancer Survivor Study. J Clin Oncol 25:3649–3656
Steinlin M, Imfeld S, Zulauf P, Boltshauser E, Lövblad KO, Ridolfi Lüthy A et al (2003) Neuropsychological long-term sequelae after posterior fossa tumor resection during childhood. Brain 126:1998–2008
Turkel SB, Tishler D, Tavare CJ (2007) Late onset psychosis in survivors of pediatric central nervous system malignancies. J Neuropsychiatry Clin Neurosci 19:293–297
Turner CD, Chordas CA, Liptak CC, Rey-Casserly C, Delaney BL, Ullrich NJ et al (2009) Medical, psychological, cognitive and educational late-effects in pediatric low-grade glioma survivors treated with surgery only. Pediatr Blood Cancer 53:417–423
Turner CD, Rey-Casserly C, Liptak CC, Chordas C (2009) Late effects of therapy for pediatric brain tumor survivors. J Child Neurol 24:1455–1463
van der Geest IM, van Dorp W, Hop WC, Neggers SJ, de Vries AC, Pieters R et al (2013) Emotional distress in 652 Dutch very long-term survivors of childhood cancer, using the Hospital Anxiety and Depression Scale (HADS). J Pediatr Hematol Oncol 35:525–529
Zebrack BJ, Gurney JG, Oeffinger KC, Whitton J, Packer RJ, Mertens AC et al (2004) Psychological outcomes in long-term survivors of childhood brain cancer: a report from the Childhood Cancer Survivor Study. J Clin Oncol 22:999–1006
Zeltzer LK, Lu Q, Leisenring W, Tsao JC, Recklitis C, Armstrong G et al (2008) Psychosocial outcomes and health-related quality of life in adult childhood cancer survivors: a report from the Childhood Cancer Survivor Study. Cancer Epidemiol Biomarkers Prev 17:435–446
Zeltzer LK, Recklitis C, Buchbinder D, Zebrack B, Casillas J, Tsao JC et al (2009) Psychological status in childhood cancer survivors: a report from the Childhood Cancer Survivor Study. J Clin Oncol 27:2396–2404
Acknowledgments
We would like to extend our thanks to Dr. Sanjiv Bhatia of Miami Children’s Hospital and Dr. Sudheer Ambekar for their valuable insight and comments regarding this study.
Conflict of interest
The authors report no conflict of interest concerning the materials or methods used in this study or the finding specified in this paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shah, S.S., Dellarole, A., Peterson, E.C. et al. Long-term psychiatric outcomes in pediatric brain tumor survivors. Childs Nerv Syst 31, 653–663 (2015). https://doi.org/10.1007/s00381-015-2669-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-015-2669-7