Abstract
Object
Overdrainage is a chronic complication in shunted pediatric patients with hydrocephalus. The use of adjustability of differential pressure (DP) valves in combination with antisiphoning devices may help to overcome this sequela and may diminish the rate of possible shunt failures. The purpose of this retrospective study is to report our experience on shunt survival and infection rate with an adjustable DP valve with integrated gravitational unit in pediatric hydrocephalus.
Methods
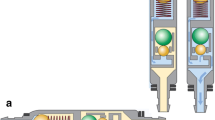
The proGAV consists of an adjustable differential pressure (DP) valve and a gravitational unit. During the time period of July 2004 and December 2009, a total of 237 adjustable gravitational valves were used in 203 children (age, 6.5 ± 6.54; 0–27 years). In the follow-up period, valve and shunt failures as well as rate of infection were recorded.
Results
Within the average follow-up time of 21.9 ± 10.3 months (range, 6–72 months), the valve survival rate was 83.8 %. The overall shunt survival rate including all necessary revisions was 64.3 %. Looking at the group of infants (<1 year of age) within the cohort, the valve survival rate was 77.3 % and the shunt survival rate was 60.9 %. The overall infection rate was 4.6 %.
Conclusion
In a concept of avoiding chronic overdrainage by using the proGAV in hydrocephalic children, we observed a good rate of valve and shunt survival. Compared to previous reported series, we experienced the proGAV as a reliable tool for the treatment of pediatric hydrocephalus.


Similar content being viewed by others
References
Abott R (1991) Chronic headache associated with a functioning shunt: usefulness of pressure monitoring. Neurosurgery 28:72–77
Akbar M (2005) Magnetic resonance imaging and cerebrospinal fluid shunt valves. N Engl J Med 353:1413–1414
Allin D (2006) In vitro hydrodynamic properties of the Miethke proGAV hydrocephalus shunt. Cerebrospinal Fluid Res 3:9
Allin D (2008) Investigation of the hydrodynamic properties of a new MRI-resistant programmable hydrocephalus shunt. Cerebrospinal Fluid Res 5:8
Aschoff A (1995) Overdrainage and shunt technology. A critical comparison of programmable, hydrostatic and variable-resistance valves and flow-reducing devices. Childs Nerv Syst 11:193–202
Browd S (2006) Failure of cerebrospinal fluid shunts: part II: overdrainge, loculation, and abdominal complications. Pediatr Neurol 34(3):171–176
Czonsnyka ZH (1998) Posture-related overdrainage: comparison of the performance of 10 hydrocephalus shunts in vitro. Neurosurgery 42:327–333
Czonsnyka ZH (2001) Laboratory evaluation of the phoenix CRx diamond valve. Neurosurgery 48:689–694
Drake J (1995) The shunt book. Blackwell, Camebridge
Drake J (1996) Rationale and methodology of the multicenter pediatric cerebrospinal fluid shunt design trial. Child’s Nerv Syst 12(8):434–447
Drake J (1998) Randomized trial of cerebrospinal fluid shunt valve design in pediatric hydrocephalus. Neurosurgery 43:294–303
Faulhauer K (1978) Overdrainage phenomena in shunt treated hydrocephalus. Acta Neurochir (Wien) 45:89–101
Gruber R (1980) The problem of chronic overdrainage of the ventriculoperitoneal shunt in congenital hydrocephalus. Z Kinderchir 31:362–369
Gruber R (1984) Experiences with the anti-siphon device (ASD) in shunt therapy of pediatric hydrocephalus. J Neurosurg 61:156–162
Haberl E (2009) Experiences with a gravity-assisted valve in hydrocephalic children. J Neurosurg Pediatr 4:288–293
Hanlo PW (2003) Treatment of hydrocephalus determined by the European orbis sigma valve II survey: a multicenter prospective 5-year shunt survival study in children and adults in whom a flow-regulating shunt was used. J Neurosurg 99:52–57
Hatlen TJ (2012) Nonprogrammable and programmable cerebrospinal fluid shunt valves: a 5-year study. J Neurosurg Pediatr 9:462–467
Higashi S (1994) Effects of head elevation on intracranial hemodynamics in patients with ventriculoperitoneal shunts. J Neurosurg 81:829–836
Hirsch JF (1992) Surgery of hydrocephalus: past, present and future. Acta Neurochir (Wien) 116:155–160
Kestle JRW (2005) A multicenter prospective cohort study of the strata valve for the management of hydrocephalus in pediatric patients. J Neurosurg 102(Pediatrics 2):141–145
Khan RA (2010) Role of shunts with antisiphon device in treatment of pediatric hydrocephalus. Clin Neurol Neurosurg 112:687–690
Lavinio A (2008) Magnetic field interactions in adjustable hydrocephalus shunts. J Neurosurg Pediatr 2:222–228
Lindner D (2005) Effect of 3 T MRI on the function of shunt valves—evaluation of paediGAV, dual switch and proGAV. Eur J Radiol 56:56–59
McGirt MJ (2007) Adjustable vs set-pressure valves decrease the risk of proximal shunt obstruction in the treatment of pediatric hydrocephalus. Child’s Nerv Syst 23:289–295
Meier U (2007) Clinical experience in the treatment of idiopathic normal-pressure hydrocephalus using the new programmable gravity-assisted valves (proGAV Aesculap). Akt Neurol 34:147–150
Meling TR (2005) The gravity-assisted paedi-GAV valve in the treatment of pediatric hydrocephalus. Pediatr Neurosurg 41:8–14
Nakashima K (2011) Programmable shunt valves: in vitro assessment of safety of the magnetic field generated by a portable game machine. Neurol Med Chir 51:635–638
Oi S (1987) Infantile hydrocephalus and the slit ventricle syndrome in early infancy. Child’s Nerv Syst 3:145–150
Oi S (1989) Hydrocephalus in premature infants. Characteristics and therapeutic problems. Child’s Nerv Syst 5:76–82
Park J (2007) Valve inclination influences the performance of gravity-assisted valve. Surg Neurol 68:14–18
Petrella G (2009) In vivo assessment of hydrocephalus shunt. Acta Neurol Scand 120:317–323
Pollack I (1999) A randomized controlled study of a programmable shunt valve versus a conventional valve for patients with hydrocephalus. Hakim Medos Investigator Group. Neurosurgery 45:1399–1408
Pudenz R (1991) Hydrocephalus: overdrainage by ventricular shunts. A review and recommendations. Surg Neurol 35:200–212
Rhode V (2009) First experiences with an adjustable gravitational valve in childhood hydrocepalus. J Neurosurg Pediatrics 3:90–93
Sainte-Rose C (1987) A new approach in the treatment of hydrocephalus. J Neurosurg 66:213–226
Sprung C (1996) The dual-switch valve. A new hydrostatic valve for the treatment of hydrocephalus. Child’s Nerv Syst 12:573–581
Sprung C (2005) The enigma of underdrainage in shunting with hydrostatic valves and possible solutions. Acta Neurochir 95:229–235
Sprung C (2005) Shuntingof hydrocephalus with the new adjustable gravitational proGAV—advantages compared to other devices. Cerebros Fluid Research 2(Suppl 1):37
Sprung C (2010) The adjustable proGAV shunt: a prospective safety and reliability multicenter study. Neurosurgery 66:465–474
Stellman-Ward GR (1997) The incidence of chronic headache in children with shunted hydrocephalus. Eur J Pediatr Surg 7:12–14
Toma AK (2011) Use of the proGAV shunt valve in normal-pressure hydrocephalus. Operative Neurosurgery 2:245–249
Zemack G (2000) Seven years of clinical experience with the programmable Codman Hakim valve: a retrospective study of 583 patients. J Neurosurg 92:941–948
Zemack G (2003) Clinical experience with the use of a shunt with an adjustable valve in children with hydrocephalus. J Neurosurg 98:471–476
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Thomale, UW., Gebert, A.F., Haberl, H. et al. Shunt survival rates by using the adjustable differential pressure valve combined with a gravitational unit (proGAV) in pediatric neurosurgery. Childs Nerv Syst 29, 425–431 (2013). https://doi.org/10.1007/s00381-012-1956-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-012-1956-9