Abstract
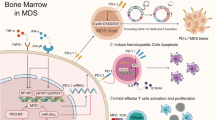
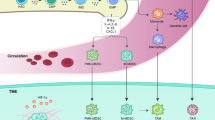
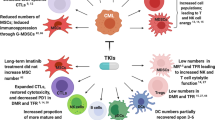
Myeloproliferative neoplasms (MPNs) are clonal hematopoietic diseases that belong to the spectrum of myeloid malignancies (MyMs), which also include myelodysplastic syndromes (MDS), acute myeloid leukemia (AML), and chronic myelogenous leukemia (CML). While hematopoietic stem cell transplantation (HSCT) is a potentially curative therapeutic approach to many MyMs, the associated morbidity and mortality have necessitated the development of non-HSCT therapeutics for symptom management and disease course modification. Immune checkpoint inhibition, in particular along the programmed cell death protein 1 (PD-1)/B7-H1 (PD-L1) axis, is an established strategy in solid tumors with potential as an adjunctive therapy in hematologic malignancies. Seminal studies suggest that the pro-inflammatory microenvironment of MyMs can suppress T lymphocyte-mediated immunity via PD-1 signaling and that response to mainstay epigenetic therapies for MyMs may be governed by PD-1 gene regulation. Although the role of PD-1 signaling in MPN pathogenesis and progression is as yet unclear, research in MPN patients has revealed expansion of myeloid-derived suppressor cells (MDSCs), which may effect host immune tolerance of tumor via temporally and spatially specific activation of PD-1/PD-L1 signaling. The current understanding of immune dysfunction in MPNs and analogous MyMs offers a compelling rationale to study PD-1/PD-L1 inhibition in patients as a novel treatment option.

Similar content being viewed by others
References
Ciurea SO, Merchant D, Mahmud N, Ishii T, Zhao Y, Hu W et al (2007) Pivotal contributions of megakaryocytes to the biology of idiopathic myelofibrosis. Blood 110(3):986–993
Arber DA, Orazi A, Hasserjian R, Thiele J, Borowitz MJ, Le Beau MM et al (2016) The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia. Blood 127(20):2391–2405
Hanahan D, Weinberg RA (2011) Hallmarks of cancer: the next generation. Cell 144(5):646–674
Freeman GJ, Long AJ, Iwai Y, Bourque K, Chernova T, Nishimura H et al (2000) Engagement of the PD-1 immunoinhibitory receptor by a novel B7 family member leads to negative regulation of lymphocyte activation. J Exp Med 192(7):1027–1034
Butte MJ, Keir ME, Phamduy TB, Sharpe AH, Freeman GJ (2007) Programmed death-1 ligand 1 interacts specifically with the B7-1 costimulatory molecule to inhibit T cell responses. Immunity 27(1):111–122
Keir ME, Butte MJ, Freeman GJ, Sharpe AH (2008) PD-1 and its ligands in tolerance and immunity. Annu Rev Immunol 26:677–704
Dong H, Strome SE, Salomao DR, Tamura H, Hirano F, Flies DB et al (2002) Tumor-associated B7-H1 promotes T-cell apoptosis: a potential mechanism of immune evasion. Nat Med 8(8):793–800
Zou W, Chen L (2008) Inhibitory B7-family molecules in the tumour microenvironment. Nat Rev Immunol. 8(6):467–477
Administration USFaD (2014) FDA approves Keytruda for advanced melanoma
Administration USFaD (2015) FDA approves Keytruda for advanced non-small cell lung cancer
Administration USFaD (2014) FDA approves Opdivo for advanced melanoma
Administration USFaD (2015) FDA expands approved use of Opdivo to treat lung cancer
Administration USFaD (2015) Nivolumab (Opdivo) for Hodgkin lymphoma. 2016
Administration USFaD (2015) FDA approves Opdivo to treat advanced form of kidney cancer
Administration USFaD (2016) FDA approves Keytruda (pembrolizumab) for head and neck cancer
Blank C, Brown I, Peterson AC, Spiotto M, Iwai Y, Honjo T et al (2004) PD-L1/B7H-1 inhibits the effector phase of tumor rejection by T cell receptor (TCR) transgenic CD8+ T cells. Cancer Res 64(3):1140–1145
Robert C, Schachter J, Long GV, Arance A, Grob JJ, Mortier L et al (2015) Pembrolizumab versus ipilimumab in advanced melanoma. N Engl J Med 372(26):2521–2532
Garon EB, Rizvi NA, Hui R, Leighl N, Balmanoukian AS, Eder JP et al (2015) Pembrolizumab for the treatment of non-small-cell lung cancer. N Engl J Med 372(21):2018–2028
Westin JR, Chu F, Zhang M, Fayad LE, Kwak LW, Fowler N et al (2014) Safety and activity of PD1 blockade by pidilizumab in combination with rituximab in patients with relapsed follicular lymphoma: a single group, open-label, phase 2 trial. Lancet Oncol 15(1):69–77
Armand P, Shipp MA, Ribrag V, Michot JM, Zinzani PL, Kuruvilla J, et al. (2016) Programmed death-1 blockade with pembrolizumab in patients with classical Hodgkin lymphoma after brentuximab vedotin failure. J Clin Oncol
Ansell SM, Lesokhin AM, Borrello I, Halwani A, Scott EC, Gutierrez M et al (2015) PD-1 blockade with nivolumab in relapsed or refractory Hodgkin’s lymphoma. N Engl J Med 372(4):311–319
Green MR, Monti S, Rodig SJ, Juszczynski P, Currie T, O’Donnell E et al (2010) Integrative analysis reveals selective 9p24.1 amplification, increased PD-1 ligand expression, and further induction via JAK2 in nodular sclerosing Hodgkin lymphoma and primary mediastinal large B-cell lymphoma. Blood 116(17):3268–3277
Kondo A, Yamashita T, Tamura H, Zhao W, Tsuji T, Shimizu M et al (2010) Interferon-gamma and tumor necrosis factor-alpha induce an immunoinhibitory molecule, B7-H1, via nuclear factor-kappaB activation in blasts in myelodysplastic syndromes. Blood 116(7):1124–1131
Aggarwal S, van de Loosdrecht AA, Alhan C, Ossenkoppele GJ, Westers TM, Bontkes HJ (2011) Role of immune responses in the pathogenesis of low-risk MDS and high-risk MDS: implications for immunotherapy. Br J Haematol 153(5):568–581
Schnorfeil FM, Lichtenegger FS, Emmerig K, Schlueter M, Neitz JS, Draenert R et al (2015) T cells are functionally not impaired in AML: increased PD-1 expression is only seen at time of relapse and correlates with a shift towards the memory T cell compartment. J Hematol Oncol 8:93
Nagaraj S, Gupta K, Pisarev V, Kinarsky L, Sherman S, Kang L et al (2007) Altered recognition of antigen is a mechanism of CD8+ T cell tolerance in cancer. Nat Med 13(7):828–835
Wang JC, Sindhu H, Chen C, Kundra A, Kafeel MI, Wong C et al (2015) Immune derangements in patients with myelofibrosis: the role of Treg, Th17, and sIL2Ralpha. PLoS One 10(3):e0116723
Kong Y, Zhang J, Claxton DF, Ehmann WC, Rybka WB, Zhu L et al (2015) PD-1(hi)TIM-3(+) T cells associate with and predict leukemia relapse in AML patients post allogeneic stem cell transplantation. Blood Cancer J 5:e330
Kronig H, Kremmler L, Haller B, Englert C, Peschel C, Andreesen R et al (2014) Interferon-induced programmed death-ligand 1 (PD-L1/B7-H1) expression increases on human acute myeloid leukemia blast cells during treatment. Eur J Haematol 92(3):195–203
Norde WJ, Maas F, Hobo W, Korman A, Quigley M, Kester MG et al (2011) PD-1/PD-L1 interactions contribute to functional T-cell impairment in patients who relapse with cancer after allogeneic stem cell transplantation. Cancer Res 71(15):5111–5122
Berthon C, Driss V, Liu J, Kuranda K, Leleu X, Jouy N et al (2010) In acute myeloid leukemia, B7-H1 (PD-L1) protection of blasts from cytotoxic T cells is induced by TLR ligands and interferon-gamma and can be reversed using MEK inhibitors. Cancer Immunol Immunother 59(12):1839–1849
Oestreich KJ, Yoon H, Ahmed R, Boss JM (2008) NFATc1 regulates PD-1 expression upon T cell activation. J Immunol 181(7):4832–4839
Kao C, Oestreich KJ, Paley MA, Crawford A, Angelosanto JM, Ali MA et al (2011) Transcription factor T-bet represses expression of the inhibitory receptor PD-1 and sustains virus-specific CD8+ T cell responses during chronic infection. Nat Immunol 12(7):663–671
Lu P, Youngblood BA, Austin JW, Mohammed AU, Butler R, Ahmed R et al (2014) Blimp-1 represses CD8 T cell expression of PD-1 using a feed-forward transcriptional circuit during acute viral infection. J Exp Med 211(3):515–527
Yang H, Bueso-Ramos C, DiNardo C, Estecio MR, Davanlou M, Geng QR et al (2014) Expression of PD-L1, PD-L2, PD-1 and CTLA4 in myelodysplastic syndromes is enhanced by treatment with hypomethylating agents. Leukemia 28(6):1280–1288
Saunthararajah Y (2013) Key clinical observations after 5-azacytidine and decitabine treatment of myelodysplastic syndromes suggest practical solutions for better outcomes. Hematology Am Soc Hematol Educ Program 2013:511–521
Orskov AD, Treppendahl MB, Skovbo A, Holm MS, Friis LS, Hokland M et al (2015) Hypomethylation and up-regulation of PD-1 in T cells by azacytidine in MDS/AML patients: a rationale for combined targeting of PD-1 and DNA methylation. Oncotarget 6(11):9612–9626
Hasselbalch HC, Bjorn ME (2015) MPNs as inflammatory diseases: the evidence, consequences, and perspectives. Mediat Inflamm 2015:102476
Riley CH, Jensen MK, Brimnes MK, Hasselbalch HC, Bjerrum OW, Straten PT et al (2011) Increase in circulating CD4(+)CD25(+)Foxp3(+) T cells in patients with Philadelphia-negative chronic myeloproliferative neoplasms during treatment with IFN-alpha. Blood 118(8):2170–2173
Christiansson L, Soderlund S, Svensson E, Mustjoki S, Bengtsson M, Simonsson B et al (2013) Increased level of myeloid-derived suppressor cells, programmed death receptor ligand 1/programmed death receptor 1, and soluble CD25 in Sokal high risk chronic myeloid leukemia. PLoS One 8(1):e55818
Parampalli Yajnanarayana S, Stubig T, Cornez I, Alchalby H, Schonberg K, Rudolph J et al (2015) JAK1/2 inhibition impairs T cell function in vitro and in patients with myeloproliferative neoplasms. Br J Haematol 169(6):824–833
De Veirman K, Van Valckenborgh E, Lahmar Q, Geeraerts X, De Bruyne E, Menu E et al (2014) Myeloid-derived suppressor cells as therapeutic target in hematological malignancies. Front Oncol 4:349
Zhang B, Wang Z, Wu L, Zhang M, Li W, Ding J et al (2013) Circulating and tumor-infiltrating myeloid-derived suppressor cells in patients with colorectal carcinoma. PLoS One 8(2):e57114
Pinton L, Solito S, Damuzzo V, Francescato S, Pozzuoli A, Berizzi A et al (2016) Activated T cells sustain myeloid-derived suppressor cell-mediated immune suppression. Oncotarget 7(2):1168–1184
Gabrilovich DI, Nagaraj S (2009) Myeloid-derived suppressor cells as regulators of the immune system. Nat Rev Immunol 9(3):162–174
Chen X, Eksioglu EA, Zhou J, Zhang L, Djeu J, Fortenbery N et al (2013) Induction of myelodysplasia by myeloid-derived suppressor cells. J Clin Invest 123(11):4595–4611
Giallongo C, Parrinello N, Tibullo D, La Cava P, Romano A, Chiarenza A et al (2014) Myeloid derived suppressor cells (MDSCs) are increased and exert immunosuppressive activity together with polymorphonuclear leukocytes (PMNs) in chronic myeloid leukemia patients. PLoS One 9(7):e101848
Sun H, Li Y, Zhang ZF, Ju Y, Li L, Zhang BC et al (2015) Increase in myeloid-derived suppressor cells (MDSCs) associated with minimal residual disease (MRD) detection in adult acute myeloid leukemia. Int J Hematol 102(5):579–586
Kundra A, Baptiste S, Chen C, Sindhu H, Wang J-C. Programmed cell death receptor (PD-1), PD-1 ligand (PD-L1) expression and myeloid derived suppressor cells (MDSC) in myeloid neoplasms implicate the mechanism of IMiD treatment of myelofibrosis. Blood. 2013;122(21):2837-.
Wang JC, Kundra A, Andrei M, Baptiste S, Chen C, Wong C et al (2016) Myeloid-derived suppressor cells in patients with myeloproliferative neoplasm. Leuk Res 43:39–43
Mussai F, Egan S, Higginbotham-Jones J, Perry T, Beggs A, Odintsova E et al (2015) Arginine dependence of acute myeloid leukemia blast proliferation: a novel therapeutic target. Blood 125(15):2386–2396
Chevolet I, Speeckaert R, Schreuer M, Neyns B, Krysko O, Bachert C et al (2015) Characterization of the in vivo immune network of IDO, tryptophan metabolism, PD-L1, and CTLA-4 in circulating immune cells in melanoma. Oncoimmunology. 4(3):e982382
Favaloro J, Liyadipitiya T, Brown R, Yang S, Suen H, Woodland N et al (2014) Myeloid derived suppressor cells are numerically, functionally and phenotypically different in patients with multiple myeloma. Leuk Lymphoma 55(12):2893–2900
Gorgun G, Samur MK, Cowens KB, Paula S, Bianchi G, Anderson JE et al (2015) Lenalidomide enhances immune checkpoint blockade-induced immune response in multiple myeloma. Clin Cancer Res 21(20):4607–4618
Zhou Q, Munger ME, Highfill SL, Tolar J, Weigel BJ, Riddle M et al (2010) Program death-1 signaling and regulatory T cells collaborate to resist the function of adoptively transferred cytotoxic T lymphocytes in advanced acute myeloid leukemia. Blood 116(14):2484–2493
Mumprecht S, Schurch C, Schwaller J, Solenthaler M, Ochsenbein AF (2009) Programmed death 1 signaling on chronic myeloid leukemia-specific T cells results in T-cell exhaustion and disease progression. Blood 114(8):1528–1536
Zhou Q, Munger ME, Veenstra RG, Weigel BJ, Hirashima M, Munn DH et al (2011) Coexpression of Tim-3 and PD-1 identifies a CD8+ T-cell exhaustion phenotype in mice with disseminated acute myelogenous leukemia. Blood 117(17):4501–4510
Poh SL, Linn YC (2016) Immune checkpoint inhibitors enhance cytotoxicity of cytokine-induced killer cells against human myeloid leukaemic blasts. Cancer Immunol Immunother 65(5):525–536
Bellucci R, Martin A, Bommarito D, Wang K, Hansen SH, Freeman GJ et al (2015) Interferon-gamma-induced activation of JAK1 and JAK2 suppresses tumor cell susceptibility to NK cells through upregulation of PD-L1 expression. Oncoimmunology 4(6):e1008824
Schonberg K, Rudolph J, Vonnahme M, Parampalli Yajnanarayana S, Cornez I, Hejazi M et al (2015) JAK inhibition impairs NK cell function in myeloproliferative neoplasms. Cancer Res 75(11):2187–2199
Schmohl JU, Nuebling T, Wild J, Kroell T, Salih HR, Schmetzer H (2016) RANK-L expression on blasts in patients with acute myeloid leukemia is associated with survival, PD-1/PD-1L expression has no impact. Eur J Haematol
Craig R, Tripp SR, Deininger M, Salama ME (2016) Programmed death ligand (PD-L1) expression is increased in spleens of myelofibrosis patients. United States and Canadian Academy ofy 2016 Annual Meeting. Seattle, Washington. Abstract 1353
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Choi, D., Tremblay, D., Iancu-Rubin, C. et al. Programmed cell death-1 pathway inhibition in myeloid malignancies: implications for myeloproliferative neoplasms. Ann Hematol 96, 919–927 (2017). https://doi.org/10.1007/s00277-016-2915-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-016-2915-4