Abstract
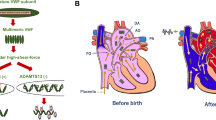
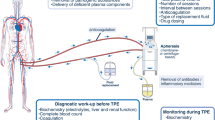
Thrombotic microangiopathy (TMA) in patients with sickle cell disease (SCD) is a rare complication. These patients manifest microangiopathic hemolytic anemia (MAHA) with laboratory evidence of hemolytic anemia, schistocytosis, and thrombocytopenia. This is the first report of the syndrome in a group of these patients. A retrospective chart analysis of 10 consecutively diagnosed patients in SCD crisis who were referred for therapeutic plasma exchange (TPE) after developing MAHA was done. Patients had chest pain, respiratory distress, fever, pulmonary infiltrates, jaundice, and neurological dysfunction with abnormal liver function and coagulation tests. MAHA was diagnosed after a median hospital stay of 5 days. Nine patients recovered completely following TPE with fluid replacement by fresh frozen plasma with or without cryo-poor plasma. Incomplete response to TPE in one case was due to the development of fresh complications. During a median follow-up period of 77 months, there was one recurrent episode and one death in SCD crisis but without evidence of MAHA. TMA is not a very rare complication among Bahraini SCD patients in crisis. Characteristic features of this disorder are acute chest syndrome, organ failure, leuco-erythroblastosis, and a combination of thrombocytopenia, LDH level >1,000 U/l, and schistocytes in blood smears. Management with TPE usually leads to complete recovery with little chance of short-term recurrence. Multiple pathogenetic mechanisms leading to increased von Willebrand factor and its multimers may form the basis of this syndrome.



Similar content being viewed by others
References
Levine SP (2004) Thrombotic thrombocytopenic purpura and other forms of nonimmunologic platelet destruction. In: Greer JP, Lee GR, Foerster J, Lukens JN, Rodgers GM, Paraskevas F, Glader B (eds) Wintrobe’s Clinical Hematology, 11th edn. Lippincott, Philadelphia, pp 1555–1564
Nguyen TC, Han YY (2011) Plasma exchange therapy for thrombotic microangiopathies. Organogenesis 7:28–31
Sadler JE (2008) Von Willebrand factor, ADAMTS13, and thrombotic thrombocytopenic purpura. Blood 112:11–18
Zheng XL, Sadler JE (2008) Pathogenesis of thrombotic microangiopathies. Annu Rev Pathol 3:249–277
Sadler JE (2006) Thrombotic thrombocytopenic purpura: a moving target. Hematology Am Soc Hematol Educ Program 2006:415–420
Sadler JE, Moake JL, Miyata T, George JN (2004) Recent advances in thrombotic thrombocytopenic purpura. Hematology Am Soc Hematol Educ Program 2004:407–423
Fujimura Y, Matsumoto M (2010) Registry of 919 patients with thrombotic microangiopathies across Japan: database of Nara Medical University during 1998–2008. Intern Med 49:7–15
Bolanos-Meade J, Keung YK, Lopez-Arvizu C, Florendo R, Cobos E (1999) Thrombotic thrombocytopenic purpura in a patient with sickle cell crisis. Ann Hematol 78:558–559
Geigel EJ, Francis CW (1997) Reversal of multiorgan dysfunction in sickle cell disease with plasma exchange. Acta Anaesthesiol Scand 41:647–650
Chehal A, Taher A, Shamseddine A (2002) Sicklemia with multiorgan failure syndrome and thrombotic thrombocytopenic purpura. Hemoglobin 26:345–351
Chinowsky MS (1994) Thrombotic thrombocytopenic purpura associated with sickle cell-hemoglobin C disease. South Med J 87:1168–1171
Lee HE, Marder VJ, Logan LJ, Friedman S, Miller BJ (2003) Life threatening thrombotic thrombocytopenic purpura (TTP) in a patient with sickle cell-hemoglobin C disease. Ann Hematol 82:702–704
Shome DK, Al Ajmi A, Darwish FA, Ravishekhar K, Zaman A, Malik N (2004) Microangiopathic haemolytic anaemia in sickle cell disease. Abstract Book 9th Congress of the European Hematology Association. Haematologica 89(supplement no. 5):S80
Al-Arrayed S, Hafadh N, Amin S, Al-Mukhareq H, Sanad H (2003) Student screening for inherited blood disorders in Bahrain. East Mediterr Health J 9:344–352
Platt OS, Brambilla DJ, Rosse WF, Milner PF, Castro O, Steinberg MH, Klug PP (1994) Mortality in sickle cell disease—life expectancy and risk factors for early death. N Engl J Med 330:1639–1644
Allford SL, Hunt BJ, Rose P, Machin SJ, Haemostasis and Thrombosis Task Force, British Committee for Standards in Haematology (2003) Guidelines on the diagnosis and management of the thrombotic microangiopathic haemolytic anaemias. Br J Haematol 120:556–573
Franchini M, Lippi G, Manzato F (2006) Recent acquisitions in the pathophysiology, diagnosis and treatment of disseminated intravascular coagulation. Thromb J 4:4
Vichinsky EP, Neumayr LD, Earles AN, Williams R, Lennette ET, Dean D, Nickerson B, Orringer E, McKie V, Daeschner C, Manci EA (2000) Causes and outcomes of the acute chest syndrome in sickle cell disease. N Engl J Med 342:1855–1865
Boga C, Kozanoglu I, Ozdogu H, Ozyurek E (2007) Plasma exchange in critically ill patients with sickle cell disease. Transfus Apher Sci 37:17–22
Hassell KL, Eckman JR, Lane PA (1994) Acute multiorgan failure syndrome: a potentially catastrophic complication of severe sickle cell pain episodes. Am J Med 96:155–162
Hiran S (2005) Multiorgan dysfunction in sickle cell disease. J Assoc Phys India 53:19–22
Hovinga JA, Studt JD, Alberio L, Lämmle B (2004) von Willebrand factor-cleaving protease (ADAMTS-13) activity determination in the diagnosis of thrombotic microangiopathies: the Swiss experience. Semin Hematol 41:75–82
Lämmle B, Kremer Hovinga JA, Alberio L (2005) Thrombotic thrombocytopenic purpura. J Thromb Haemost 3:1663–1675
Schnog JJ, Hovinga JA, Krieg S, Akin S, Lämmle B, Brandjes DP, Mac Gillavry MR, Muskiet FD, Duits AJ, CURAMA Study Group (2006) ADAMTS13 activity in sickle cell disease. Am J Hematol 81:492–498
Shelat SG (2010) Thrombotic thrombocytopenic purpura and sickle cell crisis. Clin Appl Thromb Hemost 16:224–227
Mannucci PM, Capoferri C, Canciani MT (2004) Plasma levels of von Willebrand factor regulate ADAMTS-13, its major cleaving protease. Br J Haematol 126:213–218
Zhou Z, Han H, Cruz MA, López JA, Dong JF, Guchhait P (2009) Haemoglobin blocks von Willebrand factor proteolysis by ADAMTS-13: a mechanism associated with sickle cell disease. Thromb Haemost 101:1070–1077
Ono T, Mimuro J, Madoiwa S, Soejima K, Kashiwakura Y, Ishiwata A, Takano K, Ohmori T, Sakata Y (2006) Severe secondary deficiency of von Willebrand factor-cleaving protease (ADAMTS13) in patients with sepsis-induced disseminated intravascular coagulation: its correlation with development of renal failure. Blood 107:528–534
Buseri FI, Jeremiah ZA, Shokunbi WA (2006) Plasma levels of some blood coagulation parameters in Nigerian homozygous sickle cell patients (HbSS) in steady state. Hematology 11:375–379
Ataga KI, Key NS (2007) Hypercoagulability in sickle cell disease: new approaches to an old problem. Hematology Am Soc Hematol Educ Program 91–96
Cappellini MD (2007) Coagulation in the pathophysiology of hemolytic anemias. Hematology Am Soc Hematol Educ Program 2007:74–78
Hagger D, Wolff S, Owen J, Samson D (1995) Changes in coagulation and fibrinolysis in patients with sickle cell disease compared with healthy black controls. Blood Coagul Fibrinolysis 6:93–99
Acknowledgments
The contribution of Transfusion Medicine technologists Abdulla Ebrahim and Ahmed Al Sekri to the data retrieval of these cases is gratefully acknowledged.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shome, D.K., Ramadorai, P., Al-Ajmi, A. et al. Thrombotic microangiopathy in sickle cell disease crisis. Ann Hematol 92, 509–515 (2013). https://doi.org/10.1007/s00277-012-1647-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-012-1647-3