Abstract
Objective
This study was designed to evaluate the effectiveness of endovascular treatment (EVAR) for ruptured abdominal aortic aneurysms (rAAAs).
Methods
Between September 2005 and December 2012, 44 patients with rAAA suitable for endovascular repair underwent emergency EVAR. We did not consider hemodynamic instability to be a contraindication for EVAR.
Results
Successful stent-graft deployment was achieved in 42 patients, whereas 2 required open surgical conversion. The overall 30-day mortality was 10 of 44 patients (5/34 in stable patients, 5/10 in unstable patients). Postoperative complications were observed in 7 of 44 patients (16 %): 5 patients developed abdominal compartment syndrome requiring decompressive laparotomy; 1 patient developed bowel ischemia; 1 patient had limb ischemia, and 1 had hemodynamic shock. Mean length of intensive care unit stay was 2.9 (range 2–8) days, and mean length of hospital stay was 8.6 (range 0–18) days. At a mean follow-up of 22.2 (range 1–84) months, the overall incidence of endoleak was 23.5 %: 1 type I and 7 type II endoleaks.
Conclusions
Our study demonstrates that EVAR of rAAA is associated with acceptable mortality and morbidity rates in dedicated centers.
Similar content being viewed by others
Introduction
Abdominal aortic aneurysms (AAAs) are an important cause of death in western countries. They occur in 1 % of women and 6 % of men older than age 64 years [1] and the incidence of rupture ranges between 5.6 and 17.5 per 100,000 person-years [2]. Many patients with an AAA remain asymptomatic until rupture occurs: rupture of an AAA (rAAA) is associated with significant mortality and morbidity [3–5]. The overall mortality rate for rAAA is 80–90 %, the mortality rate before hospital admission is 66 %, and the survival rate is 30–65 % for those patients admitted to the hospital alive [4, 5]. Rupture is proportionally related to the rapid enlargement of the aneurism and its diameter [6, 7].
Open surgery repair (OR) is the assessed treatment for rAAA, but it has been associated with an average in-hospital mortality of 50 % without a significant improvement in the survival rate in the last two decades [8].
Since the advent in 1991 of endovascular aneurysm repair (EVAR), large, prospective registries and multicenter trials have demonstrated significant reduction in perioperative mortality, especially in high-risk patients [9]. Since the first published report of EVAR for rAAA (rEVAR) in 1994 [10], several studies have demonstrated its feasibility and a strong correlation between rEVAR and improved 30-day mortality outcomes compared with OR [11, 12]. Although several case series have demonstrated reduction in mortality and morbidity with rEVAR compared with OR, most of the data are few, retrospectively evaluated, and limited by bias in the selection of patients [13]. In June 2013, the first randomized, controlled trial of 32 patients with rAAA has been published [14], failing to demonstrate the superiority of rEVAR in reduction of the mortality rate. The AJAX trial, recently published [15], randomized 116 patients with ruptured aneurysm either treated with open surgery or with EVAR; this trial did not show a significant difference in combined death and severe complications between EVAR and OR. More detailed information about the real effectiveness in the EVAR treatment of rAAA will be provided from the ongoing IMPROVE trial that brings together selected centers in the United Kingdom [16]; patients with a clinical diagnosis of ruptured AAA will be individually randomized to either endovascular repair or OR. Given the limited literature data, the objective of this study was to report our experience in treating rAAA by endovascular means.
Materials and Methods
This was a nonrandomized, retrospective, single-centre study. Between September 2005 and December 2012, a total of 44 patients [39 men, 5 women; median age 78.7 (range 65.4–91) years] with a rAAA underwent emergency rEVAR.
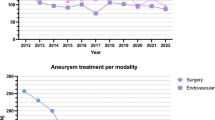
This unit has a significant aneurysm workload. During the study period we treated, elective and emergency, intravascularly, a total of 270 patients with AAA [17], 60 patients with TAA [18], and 36 patients with isolated iliac aneurysms [19].
Suspicion of rAAA was made on the basis of history and clinical examination and confirmed, when possible, by CT imaging. Aneurysms were defined ruptured if there was extravasation of blood that surrounded the aneurysm visible at the angio-CT scan evaluation or a large haematoma without extravasation of contrast medium (contained retroperitoneal rupture). Symptomatic but unruptured AAA were excluded from this retrospective evaluation. All patients with a diagnosis of rAAA were evaluated for endovascular suitability by a dedicated vascular team consisting of vascular surgeons, vascular interventional radiologists, and dedicated vascular anesthesiologists with a separate emergency rota.
Patients whose aneurysm anatomy was not suitable for EVAR underwent OR (48 in the same period); criteria used to assess anatomic suitability for rEVAR were: (1) proximal neck diameter <32 mm; (2) infrarenal neck length >7 mm; (3) calcification <50 % of the neck; and (4) iliac diameter >6 and <20 mm [20]. In line with the recent published data [21], we did not consider hemodynamic instability to be a contraindication for endovascular repair; hemodynamic instability was defined as loss of consciousness with a systolic blood pressure <80 mmHg. Different treatment strategies were applied for stable and unstable patients.
Hemodynamic stable patients (34/44, 77.2 %) underwent 16-slice multidetector CT scan (Philips Medical System, Best, the Netherlands) with intravenous contrast medium injection (Iomeron 350 or Iomeron 400, Bracco, Milan, Italy) performed in the emergency radiology department located in the emergency room, placed near the shielded operating room used for these treatments. Scanning parameters were: slice thickness 1.0 mm; reconstruction interval 0.8 mm. Only an arterial phase was acquired (100 ml of 350 mgI/ml iodinated contrast media followed by 40 ml of saline solution; injection rate: 4 ml/s) with the bolus-tracking technique by positioning a ROI on the aortic arch, with a threshold 100 HU higher than baseline density (Fig. 1). The mean dose of contrast medium administered in the perioperative phase (preoperative angio-CT and intraoperative angiography) was 200 ml.
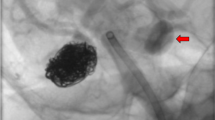
The protocol we have adopted does not account for the execution of angio-CT in the immediate postoperative phase. Hemodynamic unstable patients (10/44, 22.8 %) were taken directly to the operating room for intraoperative angiographic evaluation and for positioning of an aortic occlusion balloon (Equalizer 27, 33, 40 mm, Boston Scientific, Natick, MA, USA; Reliant AB 46, Medtronic, Sunrise, FL, USA) above the renal arteries. The main goal was to stabilize the rupture and save the patient’s life. A decision was made regarding the feasibility of EVAR, based on several inclusion criteria: infrarenal neck length >7 mm and diameter <32 mm; no bilateral iliac artery occlusion [20] (Fig. 2).
The procedures were performed under local, epidural, or general anesthesia according to clinical conditions and the ability of the patient to hold breath. Intravenous fluids and blood transfusion were minimized before aneurysm exclusion. When possible, we adopted a permissive hypotension state before EVAR, maintaining systolic blood pressure between 80 and 100 mmHg.
In 21 cases (47.7 %), procedure was performed under general anesthesia, in 13 cases (29.5 %) under epidural anesthesia, and in 10 cases under local anesthesia (22.7 %). General anesthesia was chosen in particular in patients with short necks (<10 mm), requiring the use of endoprosthesis with proximal suprarenal free-flow; in these cases it is important the absolute accuracy in deploying the endoprosthesis. This degree of accuracy can only be obtained with the proper apnea and it has allowed us to observe only a single case of type I endoleak, we encountered no complications related to general anesthesia. In these past years, with a greater experience with EVAR, local anesthesia has been preferred in selected cases (stable patients, noncalcified femoral arteries). It is important to underline that general anesthesia is not related to adverse outcome from rEVAR.
EVAR was performed by a 24 h/7 days available vascular team consisted of vascular specialists (vascular surgeon and interventional radiologist and vascular anesthesiologists), nurses, and radiological technicians in a dedicated vascular operating room with facilities for both EVAR and OR.
The procedures were performed with a mobile C-arm (BV 300, Philips Medical System); 40.9 % (18/44) of the procedures were performed by percutaneous access using an hemostatic system (Perclose Proglide, Abbott Vascular, Redwood City, CA, USA). In the remaining 59.1 % of patients, mono or bilateral open-groin accesses were performed due to the presence of severe and diffuse femoral calcifications, seen at the preoperative angio-CT scan that excluded the percutaneous approach. This pretreatment evaluation prevented any surgical conversion of the percutaneous access. The average access time for bilateral surgical inguinal access was 15 min, and the average time for percutaneous access was 10 min. We made a statistical comparison of time needed for open and percutaneous access, using Student’s t test, which showed a significant difference in favour of percutaneous access (p = 0.003). A meta-analysis recently published [22] has documented that “the preclose technique in PEVAR has a high technical success rate and a low groin complication rate. Technical success tends to increase with ultrasound-guided arterial access and decrease with larger access. When failure occurs, it is unilateral in the majority of cases, and conversion to surgical cutdown does not appear to increase the operative risk” [22]. We agree and believe percutaneous access a viable option in selected patients, even considering the increased costs.
An angiography was performed through common femoral artery puncture (5-F introducer, Terumo, Tokyo, Japan), placement of a scaling pig-tail catheter in the abdominal aorta, and administration of iodinated contrast media (Iomeron 350, Iomeron 400, Bracco, Milan, Italy). After preliminary angiography, stent-graft placement was done through employment of large-diameter introducers (18, 20, 22 F) and 0.035″ Backup Meier steerable guidewires (Boston Scientific). In our department, we have a large number of stent-graft components (main body, extensions, and distal branches) of different diameter and length always ready to perform emergency procedures.
Commercially available stent-graft systems, such as the Talent (Medtronic, Sunrise, FL, USA), the Excluder (W.L. Gore, Flagstaff, AZ, USA), the Zenith (Cook, Bloomington, IN, USA), and the E-Vita (Jotec, Hechingen, Germany), were used depending on anatomic characteristics and device availability. No C3 Excluder (WL Gore) prosthesis or Zenith Flex (Cook) prothesis have been used during the period of our study. Endoprosthesis diameter was oversized by 10–20 % in the proximal aortic neck (4–6 mm) and in the iliac artery (2–3 mm). If an aortouniliac stent-graft was placed, an occluding plug was deployed in the contralateral iliac artery and the procedure was completed with a femoro-femoral bypass graft (Vascular/Propaten, W.L. Gore). After stent-graft deployment, an angiogram was performed to confirm aneurysm exclusion, adequate proximal, and distal sealing and the absence of endoleaks.
A total of 44 stent-grafts were deployed: 37 bifurcated and 7 aortouniliac graft. Aortouniliac grafts were preferred in critically unstable patients (Table 1). In stable patients, a bifurcated device was preferred to restore the direct flow in both lower limbs despite a modest lengthening of the operation time. In fact, we found a mean operation time with bifurcated graft of 50 (range 40–60) min versus 30 (range 20–40) min of aortomonoiliac (main body and occluder contralateral iliac leg) to which the surgical time of the femoro-femoral bypass must be added (average surgical time: 30 min). We made a statistical comparison of time needed for placement of bifurcated or aortomonoiliac graft using Student’s t test, which showed a significant difference in favour of aortouniiliac graft (p = 0.001). The anti-aggregating protocol we used for all patients includes the administration of ASA 100 mg/day quod vitam.
Primary technical success was defined on an intent-to-treat basis, according to the standards for EVAR of the Society for Vascular Surgery/American Association for Vascular Surgery [19], as the successful deployment of the device in the absence of type I and type III endoleaks, graft limb occlusion, surgical conversion, or mortality through the first 24-h period.
Primary outcome events that we evaluated included: in-hospital mortality, 30-day mortality, morbidity, length of hospital, intensive care unit stay, and EVAR-related outcome (successful exclusion, endoleak rates, reintervention rates, migration rates).
The follow-up protocol included an angio-CT examination at 1, 6, and 12 months and hereafter every year. Literature data [23] recommends to execute follow-up by Doppler ultrasound and contrast-enhanced US. We are now aligned with these data, and in the past year follow-up examinations have been performed using CEUS.
A statistical comparison of mortality in hemodynamically stable and unstable patients was made with a two-proportion z test, considering the alpha threshold = 0.05. Also, a statistical comparison of preoperative and postoperative serum creatinine levels using Student’s t test was made, considering threshold alpha = 0.05.
Results
Successful stent-graft deployment was obtained in 42 of 44 patients (95.4 %); 2 cases required immediate surgical conversion for failure in stent-graft deployment. In the first case, the highly angled neck has determined a slip of the main body of the prosthesis therefore requiring a surgical conversion of the procedure; in this patient, who had previously performed the preoperative angio-CT, we underestimated the degree of the neck angle in the CT (Fig. 3). In the second case, the preoperative angio-CT was not performed and under emergency circumstances the presence of a nitinol stent, barely visible under fluoroscopy in the obese patient, was not recognized, which resulted in the imprisonment of the device thus requiring open intervention (Fig. 4). Table 2 summarizes patients and aneurysms characteristics.
Technical failure during positioning of the endoprosthesis. An unstable patient who did not undergo preliminary CT-scan evaluation had a preexisting stent in the left common iliac artery that was not seen in the preoperative phase but only after the positioning of the main body of the prosthesis from the right and of the contralateral iliac extension from the left. During the withdrawal of the device of the left iliac extension (Cook), it occurred the imprisonment of the same inside the stent (A, B). An acute surgical conversion was needed
Primary technical success rate was 78.6 % (33/42); nine patients required unplanned additional maneuvers, such as aortic cuff and distal extensions (Table 3).
Five patients (11.3 %) died in the immediate postoperative period (<24 h after EVAR) from multiple organ failure triggered by intractable intraoperative hypovolemic shock. Another five patients died during the first 30 postoperative days: two for severe respiratory failure, one for bowel ischemia, one for myocardial infarction, and the last one for hemodynamic shock without angiographic abnormalities, thus giving an overall postoperative mortality rate of 23.8 %.
The 30-day mortality rate was 14.7 % (5/34 patients) in hemodynamic stable patients and 50 % (5/10 patients) in hemodynamic unstable patients. The statistical comparison of mortality in the two treatment groups (stable vs. unstable patients), performed by two-proportion z test, showed a statistically significant difference (p = 0.02 with alpha value of 0.05).
The postoperative complications rate was 16 % (7/44): five patients developed abdominal compartment syndrome (ACS) (11.3 %) requiring laparotomic evacuation; one patient developed bowel ischemia (2.2 %); and another patient a limb ischemia (2.2 %). We encountered 4 of 44 cases of CIN (9 %): one patient developed acute renal failure that required hemodialysis, and in three cases we observed increase in serum creatinine treated by supportive therapy (control of volume and electrolyte balance, prevention of further pharmacological nephrotoxic insults, nutritional support, and control of complications). Overall, we found no statistically significant differences in creatinine preoperative and postoperative (mean value of preoperative creatinine: 1.37, range 0.8–2.2, mean postoperative creatinine values: 1:48, range 0.8–2.6, P = 0.06 with alpha 0.05).
Mean length of intensive care unit stay was 2.9 (range 2–8) days, and mean length of hospital stay was 8.6 (range 0–18) days (Table 2). In hemodynamically stable patients (34/44), the ICU stay was 2 days. All patients treated under general anesthesia were extubated after 24 h, maintained in spontaneous breathing, and subsequently were transferred to the vascular surgery ward. In hemodynamically unstable patients (10/44), the ICU stay varied from 2 to 8 days; five of these were mechanically ventilated. Thirty-four patients survived the operation and were evaluated at follow-up. At a mean follow-up of 22.2 (range 1–84) months, the overall incidence of endoleak was 23.5 %.
One patient developed a type Ia endoleak (2.9 %) due to migration of the stent-graft and was immediately treated endovascularly with a proximal aortic cuff. Seven patients developed type II endoleak (20.5 %) without increase of the aneurismal sac and so not requiring treatment. No stent-graft fractures were observed. Overall mortality during follow-up was 20 of 44 patients (45.4 %): 3 patients died from AMI, 7 from acute lung failure, 5 from progression of neoplastic disease, 3 from sepsis, and 2 from terminal kidney failure.
Discussion
Since the first description of endovascular repair in a case of a rAAA in 1994 (13), rEVAR has not been widely adopted: as suggested by the European Society of Vascular Surgery [20] “there is no level I evidence to support the widespread adoption of EVAR in unselected population of patients who present with rAAA.” The main problem is that is difficult, if not impossible, to make a randomized, controlled trial comparing EVAR and OR. Another problem is the inclusion of symptomatic AAAs in data of ruptured AAAs into a lot of studies about emergency EVAR, thus improving the results of outcome data. In this circumstance, retrospective, single-centre reports are important to better understand the real effectiveness of EVAR in rAAA. The first randomized trial failed to demonstrate any benefit of EVAR over OR [14]. Similar results were provided by the recent AJAX trial [15], which has actually suggested no benefit of EVAR for rAAA. In this situation of lack of reliable data about the actual effectiveness in the EVAR treatment of rAAA, we want to provide our experience.
In experienced centers, rEVAR has become the first-line treatment option, giving better results than open surgery [24, 25]. Mortality rates lower than OR have been observed with rEVAR, ranging from 6.7 to 45 %, with several study reporting mortality rates of 20 % or less [10, 20–28]. In a systematic review comparing rEVAR to OR, Visser et al. [28] observed postoperative 30-day mortality rates of 22 % for EVAR and 38 % for OR; similar results were presented by Resch et al. [29] and Lee et al. [30], showing an important reduction in mortality rates after EVAR. In our experience, we noted an overall 30-day mortality rate of 23.8 %, in line with literature data [20–30] and very low compared with those reported after OR. Comparison of EVAR versus OR for rAAA is misleading, because EVAR cannot be performed on all patients. However, it is important to point out that centers adopting an endovascular approach for rAAAs have demonstrated an improvement in the overall results. In a meta-analysis of published series, the pooled mortality of endovascular rAAA repair was 24.5 %, whereas the pooled mortality after open repair in centers performing both techniques was 44.4 % and the overall pooled mortality after both open and endovascular repair was 35 %. Even though the samples EVAR and OR are not comparable for different indications, the peak strength of a dedicated center is represented by the possibility of executing both treatments.
It also is essential that the EVAR is performed, both in election and in emergency/urgency, in centres with a high volume of patients. This statement is a subject of great debate in the literature [31, 32] and still cannot find definitive answer: we believe, however, that the experience of the operators in centers with large volumes increases the chance of success.
In agreement with the literature data [27–33], in our institute EVAR has become the first-line treatment for rAAA.
Literature data suggest [20] that technical success in rEVAR ranges between 96 and 100 %. In our experience, stent-graft deployment resulted successful in 42 of 44 cases (95.4 %). We had two complications in unstable patients: in one case for a distal migration of the endograft, after the deployment, that kinked into the sac of the aneurysm (Fig. 3). The second case was connected to a technical error: an unstable patient did not underwent preliminary CT-scan evaluation and a preexisting stent in the left common iliac artery was not seen (Fig. 4).
These kinds of technical failures show the importance of angio-CT scan in rAAA: except for extreme and selected cases, we believe that CT scan remains first-choice imaging assessment for rAAA, offering a sure diagnosis of rupture and a rapid evaluation of EVAR suitability. The availability of a multislice CT in the emergency department is an important asset and total time for CT scanning and evaluation of images in our series was less than 15 min. This protocol is in line with the recent data of the literature, as confirmed by the ongoing IMPROVE trial [16].
Lloyd et al. [34], in a time-to-death study in not operated patients with rAAAs, saw that the majority of patients (87.5 %) survived more than 2 h after admission to the hospital, with a median time interval of about 11 h. These data show that most patients with a rAAA who reach the hospital alive can undergo CT scanning for further therapy setting. In our series, the median time from admission to arrival in the operating room was 70 (range 40–150) min; if we consider unstable patients the median time was ~50 versus ~80 min for stable patients: according to Lloyd data [34] we suggest to make a preoperative angio-CT with mdc evaluation when possible. The CT study makes it possible to make accurate measurements using curve MPR that allow to properly assess diameter and length of the proximal and distal neck, the patient’s anatomy and the adequate choice of the devices to be used. The measurements of the length of the neck must be particularly careful in order to allow choice of over or infrarenal device. In our series, due to the length of the neck, it was necessary to perform placement of suprarenal device with a proximal free-flow in 29 of 44 cases (66 %; Table 1). The CT reconstructions are not always able to give correct assessments of the length of the vessel to be covered, especially in the presence of tortuous iliac vessels; in our series, in fact it was necessary to provide for the placement of unexpected iliac extensions in 6 of 44 cases (13.6 %).
The most important negative prognostic factor is the presence of hemodynamic instability at presentation: we observed a 30-day mortality rate of 14.7 % in hemodynamic stable patients and of 50 % in hemodynamic instable patients, with statistically significant difference (p = 0.02 with a two proportion z test). Several centers, particularly during initial experience, considered hemodynamic instability to be a contraindication for EVAR. According to literature data [25], we believe that unstable patients may particularly benefit from endovascular techniques and should not be excluded. In our experience, unstable patients are those who did worst after EVAR, but these patients have also high mortality rate with OR and minimally invasive endovascular repair can offer more chances of survival. We think that hemodynamic instability should not preclude EVAR. As in our centre, in several institutes EVAR is now the first-line treatment for shocked patients [35]. Among the factors that most affect mortality after rEVAR, a recently published study [36] showed that the bifurcated endograft approach is the only perioperative variable significantly associated with a better chance of survival; immediate conversion to open repair is associated with higher mortality and finally: type of anesthesia, haemodynamic instability, intra-aortic balloon occlusion as well as the development of a postoperative ACS significantly influence the perioperative mortality [36]. In our experience, the bifurcated graft approach is the first therapeutic option in relation to the clinical condition and the patient’s anatomy. It also has been suggested that the ability to perform an emergency EVAR procedure for rAAA under local anaesthesia may represent one of the most significant factors for improving outcome [37].
Although several studies have shown a decreased rate of systemic complications with rEVAR compared with OR [38], significant morbidity still exists. A frequent and potentially fatal complication is represented by an ACS. ACS develops in an estimated 20–30 % of patients undergoing surgery for rAAA and is associated with a high (>70 %) mortality [39]. As reported by the guidelines of the IMPROVE trial for ACS [16], normal intra-abdominal pressure (IAP) of critically ill patients is 5–7 mmHg and pressures >12 mmHg are associated with organ dysfunction. Therefore, ACS may be defined as: (1) IAP >20 mmHg associated with a new onset organ dysfunction; (2) abdominal perfusion pressure (the difference between mean systemic pressure and intra-abdominal pressure) <60 mmHg with new onset organ dysfunction [39]. For IAP >12 mmHg, recommendations are: improve abdominal wall compliance (sedation and analgesia, neuromuscular blocking, avoid head of bed >30°); evacuate intraluminal contents (nasogastric and/or rectal decompression, gastro-/colo-prokinetic agents); correct positive fluid balance (avoid excessive fluid resuscitation, colloids/hypertonic fluids, hemodialysis/ultrafiltration); organ Support (maintain APP >60 mmHg with vasopressors, optimize ventilation, alveolar recruitment); and evacuate abdominal fluid collections (paracentesis, percutaneous drainage), with a key role played by the interventional radiologist in the performance of percutaneous drainage [40]. Acute compartment syndrome, with IAP >20 mmHg and new onset organ dysfunction or IAP >30 mmHg requires decompressive laparotomy [40].
In our series, ACS has been observed in 5 of 44 patients (11.3 %) and has been successfully treated with decompressive abdominal laparotomy without any ACS-related deaths.
A topic of great interest is the incidence of CIN in patients undergoing EVAR, especially if suffering from preexisting chronic renal failure: in our experience we encountered 4 of 44 cases of CIN (9 %) but no statistically significant differences in creatinine preoperatively and postoperatively was observed (mean value of preoperative creatinine: 1.37, range 0.8–2.2, mean postoperative creatinine values: 1:48, range 0.8–2.6, P = 0.06 with alpha 0.05). These results are in line with the literature data [41] and show that “EVAR with contrast agents can be accomplished in patients with chronic renal insufficiency without hemodialysis; therefore, elevated creatinine levels may not be a contraindication in EVAR” [41].
Follow-up is necessary to evaluate the development of early and late endoleaks, which can affect the effectiveness of EVAR [20]. In our experience, given the limited number of the sample and the short follow-up, we observed one case of type I endoleak (2.9 %), which was emergency treated with proximal aortic cuff, and seven cases of type II endoleaks (20.5 %) that were not associated with enlargement of the aneurismal sac and were managed conservatively.
The capability to perform EVAR in ruptured aneurysms depends on the presence of a vascular dedicated team consisting of vascular surgeons, vascular interventional radiologists, anesthesiologists, radiological technicians, and nurses with experience in endovascular treatments. This team in our centre is available 24/7. It should be noted, however, that in smaller centres where 24-h presence of vascular IR may not be available, endovascular surgeons can still undertake such procedures. As suggested in the literature [35], the setup of standardized protocols for endovascular treatment of rAAA, including a multidisciplinary approach has been demonstrated successfully and should be employed. A “rupture kit” for rEVAR with large-diameter main-body devices with short and long limb lengths should be maintained and should suffice in most emergent cases [35].
The limitations of our study are the number of patients treated, the short follow-up, and the absence of data before the introduction of EVAR that enables a real comparison of periprocedural morbidity and mortality pre- and post-EVAR, it should be noted, however, that the current team of vascular surgeons and interventional radiologists in our hospital has been in active since 2005 and that the topic under discussion is a matter of interesting debate in the literature, especially given the latest data provided by the study AJAX [15]. We therefore thought it useful to report our experience in the treatment of rAAA.
In conclusion, our results agree with the data in the literature suggesting that the endovascular approach should be the first-line option for patients with ruptured, abdominal, aortic aneurysm. It also is clear that the success of the procedure is directly correlated with the clinical and radiological assessment and especially by the presence of a team always available with an adequate cultural and operational background.
References
Mastracci TM, Cinà CS (2007) Screening for abdominal aortic aneurysm in Canada: review and position statement of the Canadian Society for Vascular Surgery. J Vasc Surg 45(6):1268–1276
Acosta S, Ogren M, Bengtsson H et al (2006) Increasing incidence of ruptured abdominal aortic aneurysm: a population-based study. J Vasc Surg 44(2):237–243
Verhoeven EL, Kapma MR, Groen H et al (2008) Mortality of ruptured abdominal aortic aneurysm treated with open or endovascular repair. J Vasc Surg 48(6):1396–1400
Arko FR, Lee WA, Hill BB et al (2002) Aneurysm-related death: primary endpoint analysis for comparison of open and endovascular repair. J Vasc Surg 36(2):297–304
Van Dongen HP, Leusink JA, Moll FL et al (1998) Ruptured abdominal aortic aneurysms: factors influencing postoperative mortality and long-term survival. Eur J Vasc Endovasc Surg 15(1):62–66
Badger SA, O’Donnell ME, Makar RR et al (2006) Aortic necks of ruptured abdominal aneurysms dilate more than asymptomatic aneurysms after endovascular repair. J Vasc Surg 44(2):244–249
Resch T, Ivancev K, Brunkwall J et al (2000) Midterm changes in aortic aneurysm morphology after endovascular repair. J Endovasc Ther 7(4):279–285
Peppelenbosch N, Cuypers PW, Vahl AC et al (2005) Emergency endovascular treatment for ruptured abdominal aortic aneurysm and the risk of spinal cord ischemia. J Vasc Surg 42(4):608–614
Moore R, Nutley M, Cina CS et al (2007) Improved survival after introduction of an emergency endovascular therapy protocol for ruptured abdominal aortic aneurysms. J Vasc Surg 45(3):443–450
Yusuf SW, Whitaker SC, Chuter TA et al (1994) Emergency endovascular repair of leaking aortic aneurysm. Lancet 344:1645
Nedeau AE, Pomposelli FB, Hamdan AD et al (2012) Endovascular vs. open repair for ruptured abdominal aortic aneurysm. J Vasc Surg 56(1):15–20
Kubin K, Sodeck GH, Teufelsbauer H et al (2008) Endovascular therapy of ruptured abdominal aortic aneurysm: mid- and long-term results. Cardiovasc Intervent Radiol 31(3):496–503
Towne JB (2005) Endovascular treatment of abdominal aortic aneurysms. Am J Surg 189(2):140–149
Hinchliffe RJ, Bruijstens L, MacSweeney ST, Braithwaite BD (2006) A randomised trial of endovascular and open surgery for ruptured abdominal aortic aneurysm—results of a pilot study and lessons learned for future studies. Eur J Vasc Endovasc Surg 32(5):506–513
Powell JT, Thompson SG, Thompson MM et al (2009) The immediate management of the patient with rupture: open versus endovascular repair (IMPROVE) aneurysm trial–ISRCTN 48334791 IMPROVE trialists. Acta Chir Belg 109(6):678–680
Fossaceca R, Guzzardi G, Cerini P et al (2013) Endovascular treatment of abdominal aortic aneurysms: 6 years of experience at a single centre. Radiol Med 118(4):616–632
Fossaceca R, Guzzardi G, Cerini P et al (2013) Endovascular treatment of thoracic aortic aneurysm: a single-center experience. Ann Vasc Surg 27(8):1020–1028. doi:10.1016/j.avsg.2012.07.032
Fossaceca R, Guzzardi G, Di Terlizzi M et al (2013) Long-term efficacy of endovascular treatment of isolated iliac artery aneurysms. Radiol Med 118(1):62–73
Moll FL, Powell JT, Fraedrich G et al (2011) Management of abdominal aortic aneurysms clinical practice guidelines of the European society for vascular surgery. Eur J Vasc Endovasc Surg 41(Suppl 1):S1–S58
Carrafiello G, Piffaretti G, Laganà D et al (2012) Endovascular treatment of ruptured abdominal aortic aneurysms: aorto-uni-iliac or bifurcated endograft? Radiol Med 117(3):410–425
Jaffan AA, Prince EA, Hampson CO, Murphy TP (2013) The preclose technique in percutaneous endovascular aortic repair: a systematic literature review and meta-analysis. Cardiovasc Intervent Radiol 36(3):567–577
Chaudhuri A (2012) Commentary on: use of colour duplex ultrasound as a first line surveillance tool following EVAR is associated with a reduction in cost without compromising accuracy. Eur J Vasc Endovasc Surg 44(2):151–152
Lesperance K, Andersen C, Singh N et al (2008) Expanding use of emergency endovascular repair for ruptured abdominal aortic aneurysms: disparities in outcomes from a nationwide perspective. J Vasc Surg 47(6):1165–1170
Veith FJ, Ohki T (2002) Endovascular approaches to ruptured infrarenal aorto-iliac aneurysms. J Cardiovasc Surg (Torino) 43(3):369–378
Laganà D, Carrafiello G, Mangini M et al (2006) Emergency endovascular treatment of abdominal aortic aneurysms: feasibility and results. Cardiovasc Intervent Radiol 29(2):241–248
Brandt M, Walluscheck KP, Jahnke T et al (2005) Endovascular repair of ruptured abdominal aortic aneurysm: feasibility and impact on early outcome. J Vasc Interv Radiol 16(10):1309–1312
Visser JJ, Bosch JL, Hunink MG et al (2006) Endovascular repair versus open surgery in patients with ruptured abdominal aortic aneurysms: clinical outcomes with 1-year follow-up. J Vasc Surg 44(6):1148–1155
Resch T, Malina M, Lindblad B et al (2003) Endovascular repair of ruptured abdominal aortic aneurysms: logistics and short-term results. J Endovasc Ther 10(3):440–446
Lee WA, Hirneise CM, Tayyarah M et al (2004) Impact of endovascular repair on early outcomes of ruptured abdominal aortic aneurysms. J Vasc Surg 40(2):211–215
Haulon S, Barillà D, Tyrrell M (2013) Part one: For the motion. Fenestrated endografts should be restricted to a small number of specialized centers. Eur J Vasc Endovasc Surg 45(3):200–203
Tsilimparis N, Ricotta JJ 2nd (2013) Part two: Against the motion. Fenestrated endografts should not be restricted to a small number of specialized centers. Eur J Vasc Endovasc Surg 45(3):204–207
Karkos CD, Harkin DW, Giannakou A, Gerassimidis TS (2009) Mortality after endovascular repair of ruptured abdominal aortic aneurysms: a systematic review and meta-analysis. Arch Surg 144:770–778
Lloyd GM, Brown MJ, Norwood MG et al (2004) Feasibility of preoperative computer tomography in patients with ruptured abdominal aortic aneurysm: a time-to-death study in patients without operation. J Vasc Surg 39(4):788–791
Mehta M, Taggert J, Darling RC III et al (2006) Establishing a protocol for endovascular treatment of ruptured abdominal aortic aneurysms: outcomes of a prospective analysis. J Vasc Surg 44(1):1–8
Karkos CD, Sutton AJ, Bown M, Sayers RD (2011) A meta-analysis and meta-regression analysis of factors influencing mortality after endovascular repair of ruptured abdominal aortic aneurysms. Eur J Vasc Endovasc Surg 42:775–786
Karkos CD, Karamanos D, Papazoglou KO et al (2008) Usefulness of the Hardman Index in predicting outcome after endovascular repair of ruptured abdominal aortic aneurysms. J Vasc Surg 48:788–794
Greco G, Egorova N, Anderson PL et al (2006) Outcomes of endovascular treatment of ruptured abdominal aortic aneurysms. J Vasc Surg 43(3):453–459
Djavani Gidlund K, Wanhainen A, Björck M (2011) Intra-abdominal hypertension and abdominal compartment syndrome after endovascular repair of ruptured abdominal aortic aneurysm. Eur J Vasc Endovasc Surg 41(6):742–747
Kirkpatrick AW, Roberts DJ, De Waele J et al (2013) Intra-abdominal hypertension and the abdominal compartment syndrome: updated consensus definitions and clinical practice guidelines from the World Society of the Abdominal Compartment Syndrome. Intensive Care Med 39(7):1190–1206
Guntani A, Okadome J, Kawakubo E et al (2012) Clinical results of endovascular abdominal aortic aneurysm repair in patients with renal insufficiency without hemodialysis. Ann Vasc Dis 5(2):166–171
Conflict of interest
All authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fossaceca, R., Guzzardi, G., Cerini, P. et al. Endovascular Treatment of Ruptured Abdominal Aortic Aneurysms: Is Now EVAR the First Choice of Treatment?. Cardiovasc Intervent Radiol 37, 1156–1164 (2014). https://doi.org/10.1007/s00270-013-0782-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-013-0782-0