Abstract
Introduction
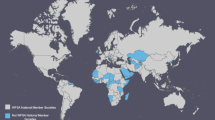
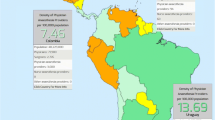
Current guidelines for the provision of safe anaesthesia from the World Health Organization and the World Federation of Societies of Anaesthesiologists (WFSA) are unachievable in a majority of low and middle-income countries (LMICs) worldwide.
Methods
Current guidelines for anaesthesia and patient safety provisions from the WHO and WFSA are compared with local ability to achieve these recommendations in LMICs.
Conclusions
Influential international organizations have historically published anaesthesia guidelines, but for the most part, without impacting substantial documentable changes or outcomes in low-income environments. This analysis, and subsequent recommendations, reviews the effectiveness of existing strategies for international guidelines, and proposes practical, step-wise implementation of patient safety approaches for LMICs.

Similar content being viewed by others
References
Eichorn JH (1989) Prevention of intraoperative anesthesia accidents and related severe injury through safety monitoring. Anesthesiology 70:572–577
Merry AF et al (2010) International Standards for a Safe Practice of Anesthesia 2010. Can J Anaesth 57(11):1027–1034
Bainbridge D et al (2012) Perioperative and anaesthetic-related mortality in developed and developing countries: a systematic review and meta-analysis. Lancet 380(9847):1075–1081
Mackay P, Cousins M (2006) Safety in anaesthesia. Anaesth Intensive Care 34(3):303–304
Hodges SC et al (2007) Anaesthesia services in developing countries: defining the problems. Anaesthesia 62(1):4–11
Walker IA et al (2010) Paediatric surgery and anaesthesia in south-western Uganda: a cross-sectional survey. Bull World Health Organ 88(12):897–906
Bosenberg AT (2007) Pediatric anesthesia in developing countries. Curr Opin Anaesthesiol 20(3):204–210
Lebrun DG et al (2013) Measuring global surgical disparities: a survey of surgical and anesthesia infrastructure in Bangladesh. World J Surg 37(1):24–31. doi:10.1007/s00268-012-1806-7
Kushner AL et al (2010) Addressing the Millennium Development Goals from a surgical perspective: essential surgery and anesthesia in 8 low- and middle-income countries. Arch Surg 145(2):154–159
Walker I, Wilson I, Bogod D (2007) Anaesthesia in developing countries. Anaesthesia 62(Suppl 1):2–3
Jochberger S et al (2008) Anesthesia and its allied disciplines in the developing world: a nationwide survey of the Republic of Zambia. Anesth Analg 106(3):942–948
Vo D, Meena CN, Bianchi S et al (2012) Anesthesia capacity in 22 low and middle income countries. J Anesth Clin Res 3(4):207
Linden AF et al (2012) Challenges of surgery in developing countries: a survey of surgical and anesthesia capacity in Uganda’s public hospitals. World J Surg 36(5):1056–1065. doi:10.1007/s00268-012-1482-7
Hansen D, Gausi SC, Merikebu M (2000) Anaesthesia in Malawi: complications and deaths. Trop Doct 30(3):146–149
Heywood AJ, Wilson IH, Sinclair JR (1989) Perioperative mortality in Zambia. Ann R Coll Surg Engl 71(6):354–358
McKenzie AG (1996) Mortality associated with anaesthesia at Zimbabwean teaching hospitals. S Afr Med J 86(4):338–342
Ouro-Bang’na Maman AF et al (2005) Deaths associated with anaesthesia in Togo, West Africa. Trop Doct 35(4):220–222
Vasdev GM et al (2008) Management of the difficult and failed airway in obstetric anesthesia. J Anesth 22(1):38–48
Cherian M et al (2010) Building and retaining the neglected anaesthesia health workforce: is it crucial for health systems strengthening through primary health care? Bull World Health Organ 88(8):637–639
Dutton RP (2013) A.S.o.A.A.Q. Institue, Editor
Greene NM (1991) Anesthesia in underdeveloped countries: a teaching program. Yale J Biol Med 64(4):403–407
Enright A, Wilson IH, Moyers JR (2007) The World Federation of Societies of Anaesthesiologists: supporting education in the developing world. Anaesthesia 62(Suppl 1):67–71
Dubowitz G, Evans FM (2012) Developing a curriculum for anaesthesia training in low- and middle-income countries. Best Pract Res Clin Anaesthesiol 26(1):17–21
Kinnear JA et al (2013) A new partnership for anesthesia training in Zambia: reflections on the first year. Can J Anaesth 60(5):484–491
Twagirumugabe T, Carli F (2010) Rwandan anesthesia residency program: a model of north-south educational partnership. Int Anesthesiol Clin 48(2):71–78
Rwanda MOH. HRH Strategic Plan 2011–2016: can be accessed on line at http://www.hrhresourcecenter.org/node/3738. Accessed 12 Dec 2014
Newton MB, Bird P (2010) Impact of parallel anesthesia and surgical provider training in Subsaharan Africa: a model for a resource-poor setting. World J Surg 34(3):445
Machine TUA. Available from: http://www.gradianhealth.org/universal-anaesthesia-machine/
Box L. Life box gap 2014. Available from: http://www.lifebox.org/about-lifebox/faq-2/what-is-the-pulse-oximetry-gap/. Accessed Feb 2014
Beringer RM, Eltringham RJ (2008) The Glostavent: evolution of an anaesthetic machine for developing countries. Anaesth Intensive Care 36(3):442–448
Thoms GM, McHugh GA, O’Sullivan E (2007) The global oximetry initiative. Anaesthesia 62(Suppl 1):75–77
WHO (2009) WHO guidelines for safe surgery. Safe surgery saves lives. WHO Press: World Health Organization, Geneva. http://whqlibdoc.who.int/publications/2009/9789241598552_eng.pdf
WHO (2009) Surgical safety checklist
WHO (2013) WHO model lists of essential medicines
World Health Organization (2003) Surgical care at the district hospital. World Health Organization, Geneva, Switzerland
Hodges AM, Hodges SC (2000) A rural cleft project in Uganda. Br J Plast Surg 53(1):7–11
Henderson K (2007) Lessons from working overseas. Anaesthesia 62(Suppl 1):113–117
Hodges SC, Hodges AM (2000) A protocol for safe anesthesia for cleft lip and palate surgery in developing countries. Anaesthesia 55(5):436–441
Funk LM et al (2010) Global operating theatre distribution and pulse oximetry supply: an estimation from reported data. Lancet 376(9746):1055–1061
Notrica MR et al (2011) Rwandan surgical and anesthesia infrastructure: a survey of district hospitals. World J Surg 35(8):1770–1780. doi:10.1007/s00268-011-1125-4
Lancet, Lancet Commission on Global Surgery
DCP, Disease control priorities in developing countries, 3rd edition
Finch LC et al (2014) Evaluation of a large-scale donation of Lifebox pulse oximeters to non-physician anaesthetists in Uganda. Anaesthesia 69(5):445–451
Haynes AB et al (2009) A surgical safety checklist to reduce morbidity and mortality in a global population. N Engl J Med 360(5):491–499
World Health Organization (2011) Patient safety: surgical safety Web map. Available from: http://maps.cga.harvard.edu:8080/Hospital/. 9 Feb 2011
Conley DM et al (2011) Effective surgical safety checklist implementation. J Am Coll Surg 212(5):873–879
Rydenfalt C et al (2013) Compliance with the WHO Surgical Safety Checklist: deviations and possible improvements. Int J Qual Health Care 25(2):182–187
Rydenfalt C, Ek A, Larsson PA (2014) Safety checklist compliance and a false sense of safety: new directions for research. BMJ Qual Saf 23(3):183–186
Walker IA, Reshamwalla S, Wilson IH (2012) Surgical safety checklists: do they improve outcomes? Br J Anaesth 109(1):47–54
Manecke GR Jr et al (1999) The effect of halothane on the amplitude and frequency characteristics of heart sounds in children. Anesth Analg 88(2):263–267
Dobson MB (2000) Anaesthesia at the district hospital, 2nd edn. World Health Organization, Geneva
Tusman G et al (2012) Atelectasis and perioperative pulmonary complications in high-risk patients. Curr Opin Anaesthesiol 25(1):1–10
Beecher HK, Todd DP (1954) A study of the deaths associated with anesthesia and surgery: based on a study of 599, 548 anesthesias in ten institutions 1948–1952, inclusive. Ann Surg 140(1):2–35
Penoyar T et al (2012) Emergency and surgery services of primary hospitals in the United Republic of Tanzania. BMJ Open 2(1):e000369
Green SM, Clem KJ, Rothrock SG (1996) Ketamine safety profile in the developing world: survey of practitioners. Acad Emerg Med 3(6):598–604
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
McQueen, K., Coonan, T., Ottaway, A. et al. The Bare Minimum: The Reality of Global Anaesthesia and Patient Safety. World J Surg 39, 2153–2160 (2015). https://doi.org/10.1007/s00268-015-3101-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-015-3101-x