Abstract
Background
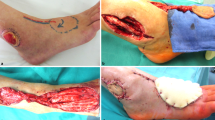
Bulky appearance is a major shortcoming after surface coverage using free muscle flaps. The one-stage thinning procedure at the time of transfer can improve the appearance and avoid additional debulking surgery. We present our experiences in the reconstruction of complex lower extremity defects using thinned free muscle flaps.
Methods
Latissimus dorsi muscle flaps (LDMs) and rectus abdominis muscle flaps (RAMs), which have vessel pedicles running deep in the muscles, were raised and the superficial tissue layers were removed to thin the flaps. These thinned muscle flaps were then used to resurface the wounds on lower extremities followed by coverage of skin autografts on the muscle surfaces.
Results
Fourteen LDMs and four RAMs were thinned used for resurfacing eight, five, and three defects on feet, ankles, and pretibial regions, respectively, with wounds that ranged from 6 × 4 cm2 to 23 × 9 cm2. All muscle flaps survived the tangential thinning procedures uneventfully. High take rates were observed for most skin grafts, except that a partial skin loss was found in one case. During the 1–20 months follow-up, the skin surface contours over the thinned muscle flaps matched well with adjacent areas.
Conclusions
Intraoperative immediate thinning of LDMs and RAMs can be safely accomplished during the primary reconstruction procedure and may provide an alternative for coverage of complex lower extremity defects.
Level of Evidence V
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.




Similar content being viewed by others
References
Kauhanen MSC, Salmi AM, Von Boguslawsky EK, Leivo IVV, Asko-Seljavaara SL (1998) Muscle fiber diameter and muscle type distribution following free microvascular muscle transfers: a prospective study. Microsurg 18(2):137–144. doi:10.1002/(SICI)1098-2752(1998)18:2<137:AID-MICR13>3.0.CO;2-Z
Kauhanen MS, Lorenzetti F, Leivo IV, Tukiainen E, Asko-Seljavaara SL (2004) Long-term morphometric and immunohistochemical findings in human free microvascular muscle flaps. Microsurgery 24(1):30–38. doi:10.1002/micr.10189
Chowdary RP, Murphy RX (1992) Delayed debulking of free muscle flaps for aesthetic contouring debulking of free muscle flaps. Br J Plast Surg 45(1):38–41
Parmaksizoglu AF, Unal MB, Cansu E (2011) The reconstruction of foot soft tissue defects by tangential debulking of the latissimus dorsi flap. J Reconstr Microsurg 27(4):211–214. doi:10.1055/s-0031-1272961
Parrett BM, Bou-Merhi JS, Buntic RF, Safa B, Buncke GM, Brooks D (2010) Refining outcomes in dorsal hand coverage: consideration of aesthetics and donor-site morbidity. Plast Reconstr Surg 126(5):1630–1638. doi:10.1097/PRS.0b013e3181ef8ea3
Rowsell AR, Eisenberg N, Davies DM, Taylor GI (1986) The anatomy of the thoracodorsal artery within the latissimus dorsi muscle. Br J Plast Surg 39(2):206–209
Rowsell AR, Godfrey AM, Richards MA (1986) The thinned latissimus dorsi free flap: a case report. Br J Plast Surg 39(2):210–212
Cassel JM (1989) Intramuscular anatomy of the latissimus dorsi muscle. Br J Plast Surg 42(5):607–609
Ooi A, Wong CH, Ong YS (2013) Combined use of liposuction and arthroscopic shaver in lower-limb fasciocutaneous flap contouring. J Plast Reconstr Aesthet Surg 66(4):538–542. doi:10.1016/j.bjps.2012.12.026
Hallock GG (1985) Defatting of flaps by means of suction-assisted lipectomy. Plast Reconstr Surg 76(6):948–952
Hui-Chou HG, Sulek J, Bluebond-Langner R, Rodriguez ED (2011) Secondary refinements of free perforator flaps for lower extremity reconstruction. Plast Reconstr Surg 127(1):248–257. doi:10.1097/PRS.0b013e3181f95b67
Lin TS, Jeng SF (2006) Full-thickness skin graft as a one-stage debulking procedure after free flap reconstruction for the lower leg. Plast Reconstr Surg 118(2):408–412. doi:10.1097/01.prs.0000227624.99710.ee
Hong JP, Yim JH, Malzone G, Lee KJ, Dashti T, Suh HS (2014) The thin gluteal artery perforator free flap to resurface the posterior aspect of the leg and foot. Plast Reconstr Surg 133(5):1184–1191. doi:10.1097/PRS.0000000000000127
Bhadkamkar MA, Wolfswinkel EM, Hatef DA, Albright SB, Echo A, Hsu PW, Izaddoost SA (2014) The ultra-thin, fascia-only anterolateral thigh flap. J Reconstr Microsurg 30(9):599–606. doi:10.1055/s-0033-1361843
Goh TL, Park SW, Cho JY, Choi JW, Hong JP (2015) The search for the ideal thin skin flap: superficial circumflex iliac artery perforator flap—a review of 210 cases. Plast Reconstr Surg 135(2):592–601. doi:10.1097/PRS.0000000000000951
Prasetyono TO, Bangun K, Buchari FB, Rezkini P (2014) Practical considerations for perforator flap thinning procedures revisited. Arch Plast Surg 41(6):693–701. doi:10.5999/aps.2014.41.6.693
Moon HK, Taylor GI (1988) The vascular anatomy of rectus abdominis musculocutaneous flaps based on the deep superior epigastric system. Plast Reconstr Surg 82(5):815–832
Rozen WM, Ashton MW, Pan WR, Taylor GI (2007) Raising perforator flaps for breast reconstruction: the intramuscular anatomy of the deep inferior epigastric artery. Plast Reconstr Surg 120(6):1443–1449. doi:10.1097/01.prs.0000282030.77894.bb
Colohan S, Wong C, Lakhiani C, Cheng A, Maia M, Arbique G, Saint-Cyr M (2012) The free descending branch muscle-sparing latissimus dorsi flap: vascular anatomy and clinical applications. Plast Reconstr Surg 130(6):776e–787e. doi:10.1097/PRS.0b013e31826d9c5e
Acknowledgments
We thank Huixian Zeng for providing the basis of the schematics.
Sources of Financial Support
This study was financially supported by the National Natural Science Foundation of China (#81571906).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
Baoqiang Song and Jianwu Chen have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Song, B., Chen, J., Han, Y. et al. Reconstruction of Complex Defects of Lower Extremities Using Thinned Free Muscle Flaps. Aesth Plast Surg 40, 519–525 (2016). https://doi.org/10.1007/s00266-016-0641-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-016-0641-x