Abstract
Introduction
Fracture impaction is a surgical technique used to support the fractured humerus with locking plate or intramedullary nail when treating proximal humeral fractures. However, few studies have investigated the mechanical difference between fracture impaction with locking plate and with intramedullary nail. The mechanism of fracture impaction to increase stability is still unclear. The aim of this study was to use numerical methods to compare the biomechanical effect of treating proximal humeral fracture.
Methods
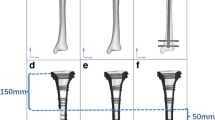
Six different humerus models, including intact and fractured humeri with various fixation patterns were used in this study. Fracture impaction was simulated by moving the distal fragment of the humeral shift upwards directly until touching the inferior surface of the proximal fragment. We also considered both poor- and normal-quality bone in the simulation.
Results
Results confirmed that fracture impaction increases fracture stabilityand decreases peak stress in both implant and bone. Also, fracture impaction and plating with medial shift of the humeral shaft provides the highest stability. The metallic implant shared loading with the bone in the impacted models, while implants sustained all the loading alone in the nonimpacted models.
Conclusions
Based on the results, the technique of fracture impaction is suggested for both nail and plate to reduce stresses on bone and implants and to increase structural stability. Furthermore, impaction with medial shift of the humeral shaft with plate is found to achieve the highest stability when treating proximal humeral fractures.











Similar content being viewed by others
References
Baron JA, Karagas M, Barrett J, Kniffin W, Malenka D, Mayor M, Keller RB (1996) Basic epidemiology of fractures of the upper and lower limb among Americans over 65 years of age. Epidemiology (Cambridge, Mass) 7(6):612–618
Bouchet R, Block D, D’Ollonne T, Gadea F, Gaillot J, Sirveaux F, Saragaglia D (2016) Non-operative treatment of four-part fractures of the proximal end of the humerus: results of a prospective and retrospective multicentric study. Int Orthop 40(8):1669–1674. doi:10.1007/s00264-015-3090-2
Savin DD, Zamfirova I, Iannotti J, Goldberg BA, Youderian AR (2016) Survey study suggests that reverse total shoulder arthroplasty is becoming the treatment of choice for four-part fractures of the humeral head in the elderly. Int Orthop 40(9):1919–1925. doi:10.1007/s00264-016-3227-y
Doursounian L, Le Sant A, Mauprivez R, Miquel A, Beauthier-Landauer V (2016) Open reduction and internal fixation of three- and four-part proximal humeral fractures by intra-focal distraction: observational study of twenty five cases. Int Orthop. doi:10.1007/s00264-015-3109-8
Gradl G, Knobe M, Pape HC, Neuhaus PV, Ring D, Guitton T (2015) Decision making in displaced fractures of the proximal humerus: fracture or surgeon based? Int Orthop 39(2):329–334. doi:10.1007/s00264-014-2630-5
Owsley KC, Gorczyca JT (2008) Fracture displacement and screw cutout after open reduction and locked plate fixation of proximal humeral fractures [corrected]. J Bone Joint Surg Am 90(2):233–240. doi:10.2106/jbjs.f.01351
Muckter H, Herzog L, Becker M, Vogel W, Meeder PJ, Buchholz J (2001) Angle- and rotation-stable internal fixation of proximal humerus fractures with the humerus fixator plate. Early clinical experience with a newly developed implant. Der Chirurg; Zeitschrift fur alle Gebiete der Operativen Medizen 72(11):1327–1335
Lill H, Hepp P, Rose T, Konig K, Josten C (2004) The angle stable locking-proximal-humerus-plate (LPHP) for proximal humeral fractures using a small anterior-lateral-deltoid-splitting-approach - technique and first results. Zentralbl Chir 129(1):43–48. doi:10.1055/s-2004-44870
Kwon BK, Goertzen DJ, O’Brien PJ, Broekhuyse HM, Oxland TR (2002) Biomechanical evaluation of proximal humeral fracture fixation supplemented with calcium phosphate cement. J Bone Joint Surg Am 84-A(6):951–961
Koike Y, Komatsuda T, Sato K (2008) Internal fixation of proximal humeral fractures with a Polarus humeral nail. J orthop Traumatol: Off J Ital Soc Orthop Traumatol 9(3):135–139. doi:10.1007/s10195-008-0019-1
Cuny C, Scarlat MM, Irrazi M, Beau P, Wenger V, Ionescu N, Berrichi A (2008) The Telegraph nail for proximal humeral fractures: a prospective four-year study. J shoulder elb Surg/Am Shoulder Elb Surg [et al] 17(4):539–545. doi:10.1016/j.jse.2008.02.004
Laflamme GY, Rouleau DM, Berry GK, Beaumont PH, Reindl R, Harvey EJ (2008) Percutaneous humeral plating of fractures of the proximal humerus: results of a prospective multicenter clinical trial. J Orthop Trauma 22(3):153–158. doi:10.1097/BOT.0b013e3181694f7d
Hirschmann MT, Quarz V, Audige L, Ludin D, Messmer P, Regazzoni P, Gross T (2007) Internal fixation of unstable proximal humerus fractures with an anatomically preshaped interlocking plate: a clinical and radiologic evaluation. J Trauma 63(6):1314–1323. doi:10.1097/01.ta.0000240457.64628.38
Gracitelli ME, Malavolta EA, Assuncao JH, Kojima KE, Dos Reis PR, Silva JS, Ferreira Neto AA, Hernandez AJ (2016) Locking intramedullary nails compared with locking plates for two- and three-part proximal humeral surgical neck fractures: a randomized controlled trial. J Shoulder Elb Surg/Am Shoulder Elb Surg [et al] 25(5):695–703. doi:10.1016/j.jse.2016.02.003
Brunner F, Sommer C, Bahrs C, Heuwinkel R, Hafner C, Rillmann P, Kohut G, Ekelund A, Muller M, Audige L, Babst R (2009) Open reduction and internal fixation of proximal humerus fractures using a proximal humeral locked plate: a prospective multicenter analysis. J Orthop Trauma 23(3):163–172. doi:10.1097/BOT.0b013e3181920e5b
Osterhoff G, Baumgartner D, Favre P, Wanner GA, Gerber H, Simmen HP, Werner CM (2011) Medial support by fibula bone graft in angular stable plate fixation of proximal humeral fractures: an in vitro study with synthetic bone. J Shoulder Elb Surg/Am Shoulder Elb Surg [et al] 20(5):740–746. doi:10.1016/j.jse.2010.10.040
Yang P, Zhang Y, Liu J, Xiao J, Ma LM, Zhu CR (2015) Biomechanical effect of medial cortical support and medial screw support on locking plate fixation in proximal humeral fractures with a medial gap: a finite element analysis. Acta Orthop Traumatol Turc 49(2):203–209. doi:10.3944/aott.2015.14.0204
Tolat AR, Amis A, Crofton S, Sinha J (2006) Failure of humeral fracture fixation plate in a young patient using the Philos system: case report. J Shoulder Elb Surg/Am Shoulder Elb Surg [et al] 15(6):e44–e47. doi:10.1016/j.jse.2006.01.014
Smith WR, Ziran BH, Anglen JO, Stahel PF (2007) Locking plates: tips and tricks. J Bone Joint Surg Am 89(10):2298–2307
Plecko M, Kraus A (2005) Internal fixation of proximal humerus fractures using the locking proximal humerus plate. Oper Orthop Traumatol 17(1):25–50. doi:10.1007/s00064-005-1120-8
Kettler M, Biberthaler P, Braunstein V, Zeiler C, Kroetz M, Mutschler W (2006) Treatment of proximal humeral fractures with the PHILOS angular stable plate. Presentation of 225 cases of dislocated fractures. Unfallchirurg 109(12):1032–1040. doi:10.1007/s00113-006-1165-7
Gardner MJ, Evans JM, Dunbar RP (2009) Failure of fracture plate fixation. J Am Acad Orthop Surg 17(10):647–657
Fankhauser F, Boldin C, Schippinger G, Haunschmid C, Szyszkowitz R (2005) A new locking plate for unstable fractures of the proximal humerus. Clin Orthop Relat Res 430:176–181
Drosdowech DS, Faber KJ, Athwal GS (2008) Open reduction and internal fixation of proximal humerus fractures. Orthop Clin N Am 39(4):429–439. doi:10.1016/j.ocl.2008.06.003, vi
Weeks CA, Begum F, Beaupre LA, Carey JP, Adeeb S, Bouliane MJ (2013) Locking plate fixation of proximal humeral fractures with impaction of the fracture site to restore medial column support: a biomechanical study. J Shoulder Elb Surg/Am Shoulder Elb Surg [et al] 22(11):1552–1557. doi:10.1016/j.jse.2013.02.003
Gardner MJ, Weil Y, Barker JU, Kelly BT, Helfet DL, Lorich DG (2007) The importance of medial support in locked plating of proximal humerus fractures. J Orthop Trauma 21(3):185–191. doi:10.1097/BOT.0b013e3180333094
Chow RM, Begum F, Beaupre LA, Carey JP, Adeeb S, Bouliane MJ (2012) Proximal humeral fracture fixation: locking plate construct +/− intramedullary fibular allograft. J Shoulder Elb Surg/Am Shoulder Elb Surg [et al] 21(7):894–901. doi:10.1016/j.jse.2011.04.015
Panchal K, Jeong JJ, Park SE, Kim WY, Min HK, Kim JY, Ji JH (2016) Clinical and radiological outcomes of unstable proximal humeral fractures treated with a locking plate and fibular strut allograft. Int Orthop 40(3):569–577. doi:10.1007/s00264-015-2950-0
Falez F, Papalia M, Greco A, Teti A, Favetti F, Panegrossi G, Casella F, Necozione S (2016) Minimally invasive plate osteosynthesis in proximal humeral fractures: one-year results of a prospective multicenter study. Int Orthop 40(3):579–585. doi:10.1007/s00264-015-3069-z
Lee YH, Chung CJ, Wang CW, Peng YT, Chang CH, Chen CH, Chen YN, Li CT (2016) Computational comparison of three posterior lumbar interbody fusion techniques by using porous titanium interbody cages with 50% porosity. Comput Biol Med 71:35–45. doi:10.1016/j.compbiomed.2016.01.024
Chen Y-N, Lee P-Y, Chang C-H, Chang C-W, Ho Y-H, Li C-T, Peng Y-T (2016) Computational comparison of tibial diaphyseal fractures fixed with various degrees of prebending of titanium elastic nails and with and without end caps. Injury. doi:10.1016/j.injury.2016.07.001
Chen YN, Chang CW, Li CT, Chang CH, Lin CF (2015) Finite element analysis of plantar fascia during walking: a quasi-static simulation. Foot Ankle Int 36(1):90–97. doi:10.1177/1071100714549189
Chang CW, Chen YN, Li CT, Peng YT, Chang CH (2015) Role of the compression screw in the dynamic hip-screw system: A finite-element study. Med Eng Phys 37(12):1174–1179. doi:10.1016/j.medengphy.2015.10.001
Zhang YK, Wei HW, Lin KP, Chen WC, Tsai CL, Lin KJ (2016) Biomechanical effect of the configuration of screw hole style on locking plate fixation in proximal humerus fracture with a simulated gap: A finite element analysis. Injury 47(6):1191–1195. doi:10.1016/j.injury.2016.02.028
Rho JY, Ashman RB, Turner CH (1993) Young’s modulus of trabecular and cortical bone material: ultrasonic and microtensile measurements. J Biomech 26(2):111–119
Maldonado ZM, Seebeck J, Heller MO, Brandt D, Hepp P, Lill H, Duda GN (2003) Straining of the intact and fractured proximal humerus under physiological-like loading. J Biomech 36(12):1865–1873
Seide K, Triebe J, Faschingbauer M, Schulz AP, Puschel K, Mehrtens G, Jurgens C (2007) Locked vs. unlocked plate osteosynthesis of the proximal humerus - a biomechanical study. Clin Biomech (Bristol, Avon) 22(2):176–182. doi:10.1016/j.clinbiomech.2006.08.009
Brianza S, Plecko M, Gueorguiev B, Windolf M, Schwieger K (2010) Biomechanical evaluation of a new fixation technique for internal fixation of three-part proximal humerus fractures in a novel cadaveric model. Clin Biomech (Bristol, Avon) 25(9):886–892. doi:10.1016/j.clinbiomech.2010.06.015
Ries Z, Hansen K, Bottlang M, Madey S, Fitzpatrick D, Marsh JL (2013) Healing results of periprosthetic distal femur fractures treated with far cortical locking technology: a preliminary retrospective study. Iowa Orthop J 33:7–11
Moazen M, Leonidou A, Pagkalos J, Marghoub A, Fagan MJ, Tsiridis E (2016) Application of Far cortical locking technology in periprosthetic femoral fracture fixation: a biomechanical study. J Arthroplast. doi:10.1016/j.arth.2016.02.013
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
There is no funding source.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Yen-Nien Chen and Chih-Wei Chang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Chen, YN., Chang, CW., Lin, CW. et al. Numerical investigation of fracture impaction in proximal humeral fracture fixation with locking plate and intramedullary nail. International Orthopaedics (SICOT) 41, 1471–1480 (2017). https://doi.org/10.1007/s00264-017-3401-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-017-3401-x