Abstract
Objective
To determine whether patient-specific 3D printed renal tumor models change pre-operative planning decisions made by urological surgeons in preparation for complex renal mass surgical procedures.
Materials and methods
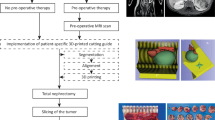
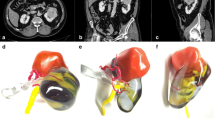
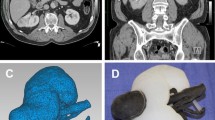
From our ongoing IRB approved study on renal neoplasms, ten renal mass cases were retrospectively selected based on Nephrometry Score greater than 5 (range 6–10). A 3D post-contrast fat-suppressed gradient-echo T1-weighted sequence was used to generate 3D printed models. The cases were evaluated by three experienced urologic oncology surgeons in a randomized fashion using (1) imaging data on PACS alone and (2) 3D printed model in addition to the imaging data. A questionnaire regarding surgical approach and planning was administered. The presumed pre-operative approaches with and without the model were compared. Any change between the presumed approaches and the actual surgical intervention was recorded.
Results
There was a change in planned approach with the 3D printed model for all ten cases with the largest impact seen regarding decisions on transperitoneal or retroperitoneal approach and clamping, with changes seen in 30%–50% of cases. Mean parenchymal volume loss for the operated kidney was 21.4%. Volume losses >20% were associated with increased ischemia times and surgeons tended to report a different approach with the use of the 3D model compared to that with imaging alone in these cases. The 3D printed models helped increase confidence regarding the chosen operative procedure in all cases.
Conclusions
Pre-operative physical 3D models created from MRI data may influence surgical planning for complex kidney cancer.




Similar content being viewed by others
Abbreviations
- MRI:
-
Magnetic resonance imaging
- CT:
-
Computed tomography
- 3D:
-
Three-dimensional
- 2D:
-
Two-dimensional
- RN:
-
Radical nephrectomy
- STL:
-
Stereolithography
- PACS:
-
Picture archiving and communication system
- CAD:
-
Computer-aided design
- ROI:
-
Region of interest
References
Campbell SC, Novick AC, Belldegrun A, et al. (2009) Guideline for management of the clinical T1 renal mass. J Urol. 182(4):1271–1279. doi:10.1016/j.juro.2009.07.004
Zargar H, Allaf ME, Bhayani S, et al. (2015) Trifecta and optimal perioperative outcomes of robotic and laparoscopic partial nephrectomy in surgical treatment of small renal masses: a multi-institutional study. BJU Int. 116(3):407–414. doi:10.1111/bju.12933
Broughton GJ, Clark PE, Barocas DA, et al. (2012) Tumour size, tumour complexity, and surgical approach are associated with nephrectomy type in small renal cortical tumours treated electively. BJU Int 109(11):1607–1613. doi:10.1111/j.1464-410X.2011.10607.x
Funahashi Y, Murotani K, Yoshino Y, et al. (2015) The renal tumor morphological characteristics that affect surgical planning for laparoscopic or open partial nephrectomy. Nagoya J Med Sci. 77(1–2):229–235
Canter D, Kutikov A, Manley B, et al. (2011) Utility of the R.E.N.A.L. nephrometry scoring system in objectifying treatment decision-making of the enhancing renal mass. Urology. 78(5):1089–1094. doi:10.1016/j.urology.2011.04.035
Tomaszewski JJ, Smaldone MC, Mehrazin R, et al. (2014) Anatomic complexity quantitated by nephrometry score is associated with prolonged warm ischemia time during robotic partial nephrectomy. Urology. 84(2):340–344. doi:10.1016/j.urology.2014.04.013
Simmons MN, Hillyer SP, Lee BH, et al. (2012) Nephrometry score is associated with volume loss and functional recovery after partial nephrectomy. J Urol. 188(1):39–44. doi:10.1016/j.juro.2012.02.2574
Poon SA, Silberstein JL, Chen LY, et al. (2013) Trends in partial and radical nephrectomy: an analysis of case logs from certifying urologists. J Urol. 190(2):464–469. doi:10.1016/j.juro.2013.02.094
Mitsouras D, Liacouras P, Imanzadeh A, et al. (2015) Medical 3D printing for the radiologist. Radiographics. 35(7):1965–1988. doi:10.1148/rg.2015140320
Matsumoto JS, Morris JM, Foley TA, et al. (2015) Three-dimensional physical modeling: applications and experience at Mayo Clinic. Radiographics. 35(7):1989–2006. doi:10.1148/rg.2015140260
Silberstein JL, Maddox MM, Dorsey P, et al. (2014) Physical models of renal malignancies using standard cross-sectional imaging and 3-dimensional printers: a pilot study. Urology 84(2):268–272. doi:10.1016/j.urology.2014.03.042
Zhang Y, Ge HW, Li NC, et al. (2015) Evaluation of three-dimensional printing for laparoscopic partial nephrectomy of renal tumors: a preliminary report. World J Urol. 34(4):533–537. doi:10.1007/s00345-015-1530-7
Rengier F, Mehndiratta A, von Tengg-Kobligk H, et al. (2010) 3D printing based on imaging data: review of medical applications. Int J Comput Assist Radiol Surg. 5(4):335–341. doi:10.1007/s11548-010-0476-x
Wake N, Rude T, Huang C, et al. (2015) 3D printed renal cancer models derived from MRI data: application in pre-surgical planning. Proceedings of the ISMRM. Singapore
Esses SJ, Berman P, Bloom AI, Sosna J (2011) Clinical applications of physical 3D models derived from MDCT data and created by rapid prototyping. AJR. 196(6):W683–W688. doi:10.2214/AJR.10.5681
Wake N, Chandarana H, Huang WC, Taneja SS, Rosenkrantz AB (2016) Application of anatomically accurate, patient-specific 3D printed models from MRI data in urological oncology. Clin Radiol. 71:610–614. doi:10.1016/j.crad.2016.02.012
Di Parma M, Coburn J, Hwang D, et al. (2016) Additively manufactured medical products—the FDA perspective. 3D Print Med 2(1):1–6
Ripley B, Kelil T, Cheezum MK, et al. (2016) D printing based on cardiac CT assists anatomic visualization prior to transcatheter aortic valve replacement. JCCT 10:28–36
Kang SK, Huang WC, Pandharipande PV, Chandarana H (2014) Solid renal masses: what the numbers tell us. AJR. 202:1196–1206. doi:10.2214/AJR.14.12502
Heilbrun ME, Casilano DD, Beland MD, et al. (2014) ACR Appropriateness Criteria: indeterminate renal mass. ACR: Reston, p 11
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported by the Center for Advanced Imaging Innovation and Research (www.cai2r.net), an NIBIB Biomedical Technology Resource Center (NIH P41 EB017183).
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Wake, N., Rude, T., Kang, S.K. et al. 3D printed renal cancer models derived from MRI data: application in pre-surgical planning. Abdom Radiol 42, 1501–1509 (2017). https://doi.org/10.1007/s00261-016-1022-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-016-1022-2