Abstract
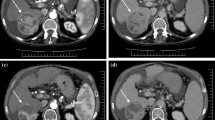
Stereotactic body radiation therapy (SBRT) is a noninvasive treatment technique for selected patients with primary liver tumors and liver-confined oligometastatic disease. Recently, SBRT has emerged as an alternative treatment option in non-surgical candidates and in whom percutaneous treatment methods are not possible or contraindicated. The experience with SBRT continues to grow. There are currently no imaging guidelines for assessment of tumor response and follow-up schedule following SBRT. SBRT produces characteristic radiation-induced changes in the treated tumor and surrounding liver parenchyma. Knowledge of these changes is essential in the interpretation of follow-up imaging and assessment of treatment response. In this review, we will describe the CT, MRI, and PET imaging findings following SBRT of both the targeted liver tumor and surrounding hepatic parenchyma.



















Similar content being viewed by others
References
Kirkpatrick JP, Kelsey CR, Palta M, et al. (2014) Stereotactic body radiotherapy: a critical review for nonradiation oncologists. Cancer 120:942–954
Sanuki N, Takeda A, Kunieda E (2014) Role of stereotactic body radiation therapy for hepatocellular carcinoma. World J Gastroenterol 20:3100–3111
Price TR, Perkins SM, Sandrasegaran K, et al. (2012) Evaluation of response after stereotactic body radiotherapy for hepatocellular carcinoma. Cancer 118:3191–3198
Olsen CC, Welsh J, Kavanagh BD, et al. (2009) Microscopic and macroscopic tumor and parenchymal effects of liver stereotactic body radiotherapy. Int J Radiat Oncol Biol Phys 73:1414–1424
Rusthoven KE, Kavanagh BD, Cardenes H, et al. (2009) Multi-institutional phase I/II trial of stereotactic body radiation therapy for liver metastases. J Clin Oncol 27:1572–1578
Swaminath A, Massey C, Brierley JD, et al. (2015) Accumulated delivered dose response of stereotactic body radiation therapy for liver metastases. Int J Radiat Oncol Biol Phys 93:639–648
Sanuki N, Takeda A, Oku Y, et al. (2015) Influence of liver toxicities on prognosis after stereotactic body radiation therapy for hepatocellular carcinoma. Hepatol Res 45:540–547
Scorsetti M, Clerici E, Navarria P, et al. (2015) The role of stereotactic body radiation therapy (SBRT) in the treatment of oligometastatic disease in the elderly. Br J Radiol 88:20150111
Scorsetti M, Comito T, Cozzi L, et al. (2015) The challenge of inoperable hepatocellular carcinoma (HCC): results of a single-institutional experience on stereotactic body radiation therapy (SBRT). J Cancer Res Clin Oncol 141:1301–1309
Huertas A, Baumann AS, Saunier-Kubs F, et al. (2015) Stereotactic body radiation therapy as an ablative treatment for inoperable hepatocellular carcinoma. Radiother Oncol 115:211–216
Bujold A, Massey CA, Kim JJ, et al. (2013) Sequential phase I and II trials of stereotactic body radiotherapy for locally advanced hepatocellular carcinoma. J Clin Oncol 31:1631–1639
Maturen KE, Feng MU, Wasnik AP, et al. (2013) Imaging effects of radiation therapy in the abdomen and pelvis: evaluating “innocent bystander” tissues. Radiographics 33:599–619
Shaffer JL, Osmundson EC, Visser BC, et al. (2015) Stereotactic body radiation therapy and central liver toxicity: a case report. Pract Radiat Oncol 5:282–285
Fajardo LF (1989) The unique physiology of endothelial cells and its implications in radiobiology. Front Radiat Ther Oncol 23:96–112
Fajardo LF, Colby TV (1980) Pathogenesis of veno-occlusive liver disease after radiation. Arch Pathol Lab Med 104:584–588
Shulman HM, McDonald GB, Matthews D, et al. (1980) An analysis of hepatic venocclusive disease and centrilobular hepatic degeneration following bone marrow transplantation. Gastroenterology 79:1178–1191
Sanuki N, Takeda A, Oku Y, et al. (2014) Stereotactic body radiotherapy for small hepatocellular carcinoma: a retrospective outcome analysis in 185 patients. Acta Oncol 53:399–404
Lall C, Bhargava P, Sandrasegaran K, et al. (2015) Three-dimensional conformal radiation therapy in the liver: MRI findings along a time continuum. J Comput Assist Tomogr 39:356–364
Schmid-Tannwald C, Strobl FF, Theisen D, et al. (2015) Diffusion-weighted MRI before and after robotic radiosurgery (Cyberknife®) in primary and secondary liver malignancies: a pilot study. Technol Cancer Res Treat 14:191–199
Eccles CL, Haider EA, Haider MA, et al. (2009) Change in diffusion weighted MRI during liver cancer radiotherapy: preliminary observations. Acta Oncol 48:1034–1043
Stinauer MA, Diot Q, Westerly DC, et al. (2012) Fluorodeoxyglucose positron emission tomography response and normal tissue regeneration after stereotactic body radiotherapy to liver metastases. Int J Radiat Oncol Biol Phys 83:e613–e618
Solanki AA, Weichselbaum RR, Appelbaum D, et al. (2012) The utility of FDG-PET for assessing outcomes in oligometastatic cancer patients treated with stereotactic body radiotherapy: a cohort study. Radiat Oncol 7:216
Lawrence TS, Robertson JM, Anscher MS, et al. (1995) Hepatic toxicity resulting from cancer treatment. Int J Radiat Oncol Biol Phys 31:1237–1248
Howells CC, Stinauer MA, Diot Q, et al. (2012) Normal liver tissue density dose response in patients treated with stereotactic body radiation therapy for liver metastases. Int J Radiat Oncol Biol Phys 84:e441–e446
Dyk P, Weiner A, Badiyan S, et al. (2015) Effect of high-dose stereotactic body radiation therapy on liver function in the treatment of primary and metastatic liver malignancies using the Child–Pugh score classification system. Pract Radiat Oncol 5:176–182
Yannam GR, Han B, Setoyama K, et al. (2014) A nonhuman primate model of human radiation-induced venocclusive liver disease and hepatocyte injury. Int J Radiat Oncol Biol Phys 88:404–411
Osmundson EC, Wu Y, Luxton G, et al. (2015) Predictors of toxicity associated with stereotactic body radiation therapy to the central hepatobiliary tract. Int J Radiat Oncol Biol Phys 91:986–994
Reed GB, Cox AJ (1966) The human liver after radiation injury. A form of veno-occlusive disease. Am J Pathol 48:597–611
Sanuki N, Takeda A, Oku Y, et al. (2014) Threshold doses for focal liver reaction after stereotactic ablative body radiation therapy for small hepatocellular carcinoma depend on liver function: evaluation on magnetic resonance imaging with Gd-EOB-DTPA. Int J Radiat Oncol Biol Phys 88:306–311
Kimura T, Takahashi S, Takahashi I, et al. (2015) The time course of dynamic computed tomographic appearance of radiation injury to the cirrhotic liver following stereotactic body radiation therapy for hepatocellular carcinoma. PLoS One 10:e0125231
Willemart S, Nicaise N, Struyven J, van Gansbeke D (2000) Acute radiation-induced hepatic injury: evaluation by triphasic contrast enhanced helical CT. Br J Radiol 73:544–546
Farach A, Quesada J, Teh BS (2015) Liver regeneration following repeat SBRT. J Gastrointest Oncol 6:E2–E6
Jarraya H, Borde P, Mirabel X, et al. (2015) Lobulated enhancement evaluation in the follow-up of liver metastases treated by stereotactic body radiation therapy. Int J Radiat Oncol Biol Phys 92:292–298
Lencioni R, Llovet JM (2010) Modified RECIST (mRECIST) assessment for hepatocellular carcinoma. Semin Liver Dis 30:52–60
Chun YS, Vauthey JN, Boonsirikamchai P, et al. (2009) Association of computed tomography morphologic criteria with pathologic response and survival in patients treated with bevacizumab for colorectal liver metastases. JAMA 302:2338–2344
Choi H, Charnsangavej C, de Castro Faria S, et al. (2004) CT evaluation of the response of gastrointestinal stromal tumors after imatinib mesylate treatment: a quantitative analysis correlated with FDG PET findings. AJR Am J Roentgenol 183:1619–1628
Jarraya H, Mirabel X, Taieb S, et al. (2013) Image-based response assessment of liver metastases following stereotactic body radiotherapy with respiratory tracking. Radiat Oncol 8:24
Aitken KL, Hawkins MA (2015) Stereotactic body radiotherapy for liver metastases. Clin Oncol (R Coll Radiol) 27:307–315
Aitken K, Tree A, Thomas K, et al. (2015) Initial UK experience of stereotactic body radiotherapy for extracranial oligometastases: can we change the therapeutic paradigm? Clin Oncol (R Coll Radiol) 27:411–419
Jarraya H, Chalayer C, Tresch E, et al. (2014) Novel technique for hepatic fiducial marker placement for stereotactic body radiation therapy. Int J Radiat Oncol Biol Phys 90:119–125
Oldrini G, Taste-George H, Renard-Oldrini S, et al. (2015) Implantation of fiducial markers in the liver for stereotactic body radiation therapy: feasibility and results. Diagn Interv Imaging 96:589–592
Janoray G (2015) Mornex F [Follow-up after stereotactic body radiation therapy for liver tumours: a review of the literature and recommendations]. Cancer Radiother 19:573–581
Herfarth KK, Hof H, Bahner ML, et al. (2003) Assessment of focal liver reaction by multiphasic CT after stereotactic single-dose radiotherapy of liver tumors. Int J Radiat Oncol Biol Phys 57:444–451
Hajj C, Goodman KA (2015) Role of radiotherapy and newer techniques in the treatment of GI cancers. J Clin Oncol 33:1737–1744
Oldrini G, Vogin G, Renard-Oldrini S, Taste-George H, Grignon B (2015) Henrot P [Post-therapeutics features of hepatocellular carcinoma treated by stereotactic body radiation therapy]. Presse Med 44:951–953
Richter C, Seco J, Hong TS, Duda DG, Bortfeld T (2014) Radiation-induced changes in hepatocyte-specific Gd-EOB-DTPA enhanced MRI: potential mechanism. Med Hypotheses 83:477–481
Kishan AU, Cao M, Wang PC, et al. (2015) Feasibility of magnetic resonance imaging-guided liver stereotactic body radiation therapy: a comparison between modulated tri-cobalt-60 teletherapy and linear accelerator-based intensity modulated radiation therapy. Pract Radiat Oncol 5:330–337
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
This retrospective image review study was approved by the institution review board with a waiver of informed consent for retrospective image analysis.
Additional information
CME activity This article has been selected as the CME activity for the current month. Please visit https://ce.mayo.edu/node/24286 and follow the instructions to complete this CME activity.
Rights and permissions
About this article
Cite this article
Haddad, M.M., Merrell, K.W., Hallemeier, C.L. et al. Stereotactic body radiation therapy of liver tumors: post-treatment appearances and evaluation of treatment response: a pictorial review. Abdom Radiol 41, 2061–2077 (2016). https://doi.org/10.1007/s00261-016-0768-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-016-0768-x