Abstract
Infection with Leishmania causes diseases with variable presentation. The most severe form is visceral leishmaniasis (VL), caused by either L. donovani or L. infantum. Despite efforts to eliminate VL, to date, molecular detection in resource-poor settings have lacked the accuracy and rapidity that would enable widespread field use and the need for accurate, sensitive assays to detect asymptomatic Leishmania infection has become apparent. The domestic dog serves as the primary reservoir host of L. infantum. Study of this reservoir population provides an opportunity to evaluate the sensitivity and specificity of diagnostics for well-defined, symptomatic, canine visceral leishmaniasis (CVL) and asymptomatic L. infantum infection. Blood samples from an L. infantum-endemic population of US hunting dogs were evaluated with Dual-Path Platform (DPP®) CVL compared to those obtained via direct detection methods (culture- and Leishmania-specific quantitative polymerase chain reaction, qPCR) and immunofluorescence anti-Leishmania antibody test (IFAT). Statistically significant correlations were found between DPP® CVL development time and clinical status, culture status, circulating DNA levels, and IFAT titer. DPP® CVL results correlated with both clinical severity of disease and serological evidence of asymptomatic L. infantum infection. By precisely documenting the minimum time required for the development of a clear positive result in DPP® CVL, this test could be used in a rapid, semi-quantitative manner for the evaluation of asymptomatic and symptomatic CVL. Our results also indicate that a similar test could be used to improve our understanding of human VL.
Similar content being viewed by others
Introduction
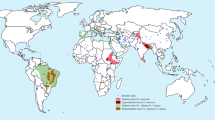
Leishmaniasis is a parasitic disease endemic to 98 countries and territories (Alvar et al. 2012) Transmission of Leishmania spp. has been demonstrated classically via sand fly, but can also occur through vertical, sexual, or blood-borne transmission (Boehme et al. 2006; Drahota et al. 2014; Dye et al. 1992; Karkamo et al. 2014; Maroli et al. 2008; Meinecke et al. 1999; Naucke and Lorentz 2012; Osorio et al. 2012; Otero et al. 2000; Owens et al. 2001; Papageorgiou et al. 2010; Parrot et al. 1930; Rosypal et al. 2005; Silva et al. 2009; Solano-Gallego et al. 2009; Symmers 1960; Travi et al. 1990; Zinchuk and Nadraga 2010) Leishmania donovani causes visceral leishmaniasis (VL; also known as Kala-Azar) in South Asia and Africa, while Leishmania infantum causes VL in the Mediterranean, the Middle East, Latin America, and parts of Asia (Coura-Vital et al. 2014). While there are multiple tests available for the diagnosis of VL, few of them can be used rapidly, without sophisticated laboratory equipment, or by individuals lacking technical training (Baneth and Aroch 2008; Grimaldi et al. 2012; Mukhtar et al. 2015). Traditionally, direct diagnosis achieved through microscopy has been the predominant means of Leishmania evaluation in field settings, but accurate microscopic diagnosis requires training and sensitivity is limited (Ertabaklar et al. 2015; Santos et al. 2014). Molecular assays, including direct detection of parasites by quantitative polymerase chain reaction (qPCR) or indirect methods such as immunofluorescence anti-Leishmania antibody test (IFAT) have been used at regional health centers but are not amenable to use in primary care clinics or true field settings (Ejazi and Ali 2013; Srividya et al. 2011). Indeed, quantitative molecular diagnosis in resource-poor settings, where the majority of VL cases occur, has been challenging (Boelaert et al. 2014; Chappuis et al. 2007).
Over the last decade, several recombinant Leishmania proteins have been identified and developed for the diagnosis of VL via detection of parasite-specific antibodies. A recombinant fusion protein, rK28, was used to produce an immunochromatographic test that was adapted to a Dual-Path Platform (DPP®) format that is suitable for use outside the laboratory setting (Pattabhi et al. 2010). Comparing the sensitivity and specificity of this test to more traditional diagnostic assays, as well as evaluating the distinct quantitative abilities of different assays to distinguish asymptomatic and symptomatic infection, is important for understanding the merits and limits of such tests.
In addition to humans, L. infantum can also infect dogs, and infected dogs serve as the major reservoir of these parasites in endemic regions. L. infantum is endemic within the US hunting hound population (Boggiatto et al. 2010; Esch et al. 2013; Gaskin et al. 2002; Gibson-Corley et al. 2008; Petersen 2009b; Petersen and Barr 2009; Schantz et al. 2005; Song et al. 2010) where we have shown it to be maintained primarily through vertical transmission (Boggiatto et al. 2011; Schaut et al. 2015). Infected dogs can maintain asymptomatic (subclinical) L. infantum infection for years before progression to canine visceral leishmaniasis (CVL), an important veterinary concern in its own right (Alvar et al. 2004; Courtenay et al. 2014; Foglia Manzillo et al. 2013; Schaut et al. 2015). Infection progresses to the chronic severe visceralizing form, which is often fatal, in approximately 40 % of L. infantum-infected dogs. Both asymptomatic and symptomatic dogs can be infectious to competent vectors, and naturally infected US hunting hounds have been shown to be infectious to vectors present in the USA (Courtenay et al. 2014; Schaut et al. 2015). These dogs could potentially serve as domestic reservoirs for emergent human infection (Drahota et al. 2014; Petersen 2009a; Schaut et al. 2015). Most US-trained health professionals do not have VL on their list of differential diagnoses, and even in endemic countries, discrimination of early symptoms of VL can be difficult (Ergen et al. 2015; Herwaldt et al. 1993).
Lateral flow-based tests typically develop for 15–20 min before results are obtained by interpretation of test band intensity on a subjective scale of 0–4. These semi-quantitative interpretations are helpful, but more objective, fully quantitative assessments would allow more accurate therapeutic decision making and permit monitoring of disease progression or response to treatment (de Vries et al. 2006; Francino et al. 2006; Rodriguez-Cortes et al. 2013; Srividya et al. 2011; Verma et al. 2010). While some researchers are now developing digital readers to enhance the differentiation/quantification of the test band, we hypothesized that a simple semi-quantitative result could be obtained by timed examination for the appearance of the test band. To test our hypothesis, we compared the performance of DPP® CVL against three assays that are frequently used for VL diagnosis: culture, qPCR, and IFAT. We found that DPP® CVL results correlate with both severity of disease and IFAT titers. By documenting the minimum time required to develop a clear positive result, we propose that DPP® CVL could be used in nonlaboratory settings for VL diagnosis and to provide more informed management of L. infantum infection.
Materials and methods
Samples
Whole blood samples were collected from hunting hounds in three US locations (n = 130). A physical exam was performed at the time of blood collection, and hounds were categorized as (a) uninfected; (b) asymptomatic, with qPCR evidence of infection; or (c) polysymptomatic, based on having two or more of the following clinical signs of CVL: alopecia, dermatitis, conjunctivitis, and lymphadenopathy, as determined in previous studies (Ciaramella et al. 1997; Reis et al. 2009). Animals were enrolled with the informed consent of the caretaker, and evaluations followed protocols as approved by the Iowa State University and University of Iowa Animal Control and Use Committees (IACUC).
Sample demographics
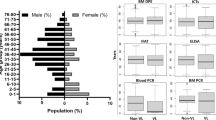
Of 130 samples, 90 had complete demographic information available (69.2 %). Of these 90, 48 were female and 42 were male. The average age of the study population was 4.1 years, the biologic equivalent of 30–40-year-old people.
Culture
Blood (3 mL) collected for parasite culture was spun at 1430 rcf for 10 min to separate buffy coat. Buffy coat (100 μL) was transferred into 800 μL of both Schneider’s and HOMEM media and incubated overnight at 26 °C. Buffy coat in media was placed onto blood agar slants and incubated for a further 3 to 4 weeks with daily observation for parasite growth.
DPP® canine visceral leishmaniasis
DPP® CVL are disposable plastic cassettes that detect Leishmania-specific antibodies using the recombinant diagnostic antigen, rK28, and colloidal gold particles coupled to protein A (Pattabhi et al. 2010). The test is developed by the addition of blood drops, then running buffer, to a sample portal. After addition of the buffer, a timer was started. Within the cassette test window, a positive test line can be visualized next to the control line (Fig. 1) (Grimaldi et al. 2012). Test result was visually read and the time required to develop a positive test band recorded. If the positive sample band did not appear within 7 min, it was considered an outlier. Presence of a control line after 15 min confirmed the validity of DPP® CVL developed with negative test samples (Fig. 1).
qPCR
QIAamp DNA Blood Mini Kit (Qiagen, Valencia, CA) was used for DNA isolation per manufacturer’s specifications for 1 mL blood. The quality and quantity of isolated DNA from whole blood samples were assessed using NanoDrop 2000 (Thermo Scientific, Waltham, MA). Isolated DNA (neat and 10-fold dilution) was analyzed in duplicate via qPCR in a 96-well plate via Super MasterMix (Rox) (Quanta Biosciences, Gaithersburg, MD). Each qPCR plate contained negative control nuclease-free water and samples of whole blood-extracted DNA from negative dogs. Positive control samples of DNA from 106 parasites spiked into canine blood were tested at full-strength, 1:10, and 1:20 dilutions. Ribosomal primer sequences used are as follows: F 5′-AAGCCACCCCAGAGGTAAAAA, R 5′ GACGGGTCTGACCCTTGGTT (Invitrogen, Life Technologies, Grand Island, NY), probe 5′ 6FAM-CGGTTCGGTGTGTGGCGCC-MGBNFQ (Applied Biosystems, Life Technologies, Grand Island, NY). Primers and probe were used at a concentration of 10 nM. The assay was run on an ABI 7000 system machine. Cycling protocol was as follows: 95 °C for 2 min, 95 °C for 1 min, and 50 cycles of 95 °C for 15 s and 60 °C for 1 min. Results were analyzed using ABI 7000 System SDS Software (Applied Biosystems, Life Technologies, Grand Island, NY).
Immunofluorescence anti-Leishmania antibody test titers
IFAT was performed on samples submitted to the Division of Parasitic Diseases, Centers for Disease Control and Prevention (CDC). The assay was considered positive at dilutions equal to or above 1/64.
Statistical analysis
Sample use was blinded through coding of sample identifiers. A post hoc power analysis was conducted using GraphPad StatMate version 2.00 (Graph Pad Software Inc., La Jolla, CA) and was found to be adequate (>99 %) for a sample size of 130 to detect a difference in sensitivity of 22.9 % between qPCR and DPP® CVL, the difference shown between a similar immunochromatographic kinetic test and qPCR (Cota et al. 2013). The time-to-positive-band for each sample was compared to the known anti-Leishmania antibody titer, qPCR cycle threshold (Ct) value, and clinical status assessed at the time of sample collection. Time-to-positive band was treated as an event, and survival analysis techniques were used to compare diagnostics. Kaplan-Meier estimator was used as a nonparametric survival estimate to compare differences in overall survival rates between clinical statuses. Cox proportional hazards regression models and subsequent hazard ratios were used to compare the predictive ability of PCR, PCR and clinical status, IFAT, and IFATand clinical status to predict time-to-positive band. AIC and SBC were used to assess model fit. Pearson correlations (r) coefficients of determination (r 2) and 95 % confidence intervals were utilized to preliminarily assess the relationship between diagnostics. Due to the fact that Pearson’s correlation only explains correlative and not predictive effects, subsequent nonlinear and linear regressions were performed to determine whether time-to-positive-band was able to predict comparative diagnostic results. All statistical analyses were performed at the 0.05 significance level. Statistical analyses were completed using Microsoft Excel (Microsoft, Redmond, WA), GraphPad Prism version 6.05 (GraphPad Software Inc., La Jolla, CA), SAS version 9.4 (SAS Institute Inc., Cary, NC), and R version 3.2.1 (R Foundation for Statistical Computing, Vienna, Austria) (Stevenson et al. 2015).
Results
Agreement of DPP® CVL results with parasite culture
Although constrained by prolonged propagation times, direct observation of parasites provides the most definitive diagnosis of VL and asymptomatic L. infantum infection. To assess the performance of DPP® CVL, we therefore established the infection status of various dogs and evaluated DPP® CVL performance on matched blood samples. Following culture of blood samples from hounds with known clinical status, samples from polysymptomatic (black) or asymptomatic infected (gray) animals had visible Leishmania parasites within 3 to 4 weeks of culture (5/6 samples; Fig. 2). As expected, the samples from uninfected dogs were culture negative. The DPP® CVL developed a positive band before 7 min in 83.3 % of known Leishmania-infected samples, providing a concordance of 87.5 % between DPP and culture. This also showed that there was a good correlation between parasite culture and DPP® CVL development time (Fig. 2; r = −0.78, 95 % CI = −0.9580, −0.1667, p value = 0.023). Linear regression analysis indicated that the variation of DPP® CVL development time explained 60.81 % of the variation in culture status results (goodness of fit r 2 = 0.6081). These data indicate that DPP® CVL is well suited for the detection of animals with clear L. infantum infection.
DPP® CVL results correlate with Leishmania culture. Comparison of culture results from eight hunting hounds with known clinical status (scored as 1 if parasites were observed, as 0 if not) against DPP® CVL development time. The plot represents a linear regression fit to the data. Black, polysymptomatic; gray, infected asymptomatic; white, uninfected
Samples from CVL have short DPP® CVL development times
To further explore the potential of DPP® CVL to detect infected animals, we next compared DPP® CVL development times against clinical status (asymptomatic vs. >2 clinical signs of disease). As expected, more than three quarters of symptomatic dogs (11/14, 78.6 %) had a DPP® CVL development time of <3 min (Fig. 3). Similarly, nearly three quarters (15/21, 71.4 %) of infected but asymptomatic dogs tested positive on DPP® CVL in <3 min. All uninfected dog samples were negative. While the correlation between clinical status and development time was still statistically significant (Fig. 3; r = −0.6357, r 2 = 0.4041, 95 % CI = −0.7791,−0.4291, p value ≤0.0001), DPP® CVL was only able to explain 40 % of the variation in symptomatic and asymptomatic infected dogs (goodness-of-fit r 2 = 0.4041). The log rank test using a Kaplan-Meier curve showed that there was a statistically significant difference between 1 or more conditions, although further analysis showed that there was no difference between asymptomatic and symptomatic infection. Thus, while DPP® CVL was able to detect L. infantum infection in a majority of dogs, the test could not discriminate between asymptomatic and symptomatic infection.
DPP® CVL provides better sensitivity than qPCR in identifying clinical status when utilizing blood samples
Several other methods have been proposed to detect L. infantum infection, including direct detection of circulating parasite DNA by PCR-based strategies. We therefore generated DPP® CVL results from 91 samples that had previously been defined by qPCR, using a Pearson correlation plot to filter different test outcomes. A good Pearson’s correlation between qPCR and DPP® CVL development times of 0.7162 was obtained (95 % CI = −0.5985–0.8036, p value = 0.0001). DPP® CVL was able to explain more than 50 % of the variation in qPCR Ct values (Fig. 4; goodness-of-fit r 2 = 0.5129). In addition, a Cox proportional regression model was created using PCR and clinical status to determine whether these variables were related to the DPP® CVL time-to-positive band. The model found with statistical significance that as qPCR ct values increase by 1, the hazard rate (risk of having a faster time-to-positive band) decreases by 12.4 % (hazard ratio 0.883). There was a subset with clearly positive DPP® CVL but lacking evidence of parasite DNA in the blood (x-axis black dots).
Faster DPP® CVL development time correlates with circulating parasite DNA levels. Whole blood from 91 hunting hounds was tested with DPP® CVL and parasite DNA quantified by qPCR. DPP® CVL development time is plotted against qPCR Ct value. Black, polysymptomatic; gray, infected asymptomatic; white, uninfected control. The solid line indicates the linear fit, with the hatched lines representing the 95 % confidence intervals
To validate the correlation of the qPCR and the DPP® CVL, we next calculated the sensitivity and specificity of these assays using 32 samples with known clinical status. In samples from polysymptomatic dogs, sensitivity of the DPP® CVL was 85 % with a specificity of 100 %, markedly improved over the 55 % sensitivity, 100 % specificity achieved by qPCR (Table 1). In samples from asymptomatic L. infantum-infected dogs, DPP® CVL sensitivity was 100 % and specificity was 86 % (Table 2). These results indicate that the DPP® CVL performed better than qPCR in matching test outcome with clinical disease.
DPP® CVL development times correlate with IFAT titer
Although it appears to be a less reliable means to assess Leishmania infection than many other diagnostic tests, IFAT is a widely used and reported assay (Rodríguez-Cortés et al. 2010). Therefore, we compared the performance of the DPP® CVL and IFAT. DPP® CVL results from samples with known clinical status samples were contrasted with previously determined IFAT titers. Dogs with higher serological IFAT titers (>1:256) had an average DPP® CVL development time of <3 min. An increasing IFAT titer correlated strongly with a shorter development time in DPP® CVL (Fig. 5a), yielding a Pearson’s correlation of −0.7983 (r = −0.7983 95 % CI = −0.9619, −0.2139, p value = 0.0175). Linear regression analysis revealed that DPP® CVL explained 63.72 % of the variation among IFAT titers (goodness-of-fit r 2 = 0.6372). Using Cox proportional regression model, it was also seen that as IFAT titers increased by 1 unit (dilution), the hazard rate increased by a statistically significant 0.8 % (hazard ratio 1.008). These data are consistent with relative antibody levels in these samples determining these diagnostic results.
DPP® CVL development time correlates with IFAT titer. A panel of a known and b previously unknown canine whole blood samples were subjected to a timed DPP® CVL evaluation. In a, comparison between IFAT result and time to positive DPP® CVL was made using preselected samples from eight dogs with known progression histories across the clinical and IFAT diagnostic continuum. The plot represents linear regression fit to the data. In b, sera from 36 previously unknown status dog samples were analyzed via IFAT and DPP® CVL. The plot represents exponential growth curve fit for the resulting data. IFAT positive cutoff value of 1:64 is designated by the horizontal line. IFAT results stratified to c below the positive threshold (<64) or d above the threshold; comparison was made with DPP® CVL development time. Each plot represents a linear regression fit to the data. Black, polysymptomatic; gray, infected asymptomatic; white, uninfected. The solid line indicates the linear fit, with the hatched lines representing the 95 % confidence intervals
To further explore the robustness of the correlation between IFAT and DPP® CVL, we determined IFAT titers for 36 previously undefined samples and compared these to DPP® CVL development time for the same samples. As observed for the archived samples, there was a strong and significant correlation between IFAT titer and DPP® CVL development time (Fig. 5b; Pearson’s correlation of −0.5853, r = −0.5853, 95 % CI = −0.7413, 0.3693, p value = <0.0001). Nonlinear regression analysis indicated that DPP® CVL development time explained only 32.33 % of variations in IFAT titers (goodness-of-fit r 2 = 0.3233). Utilizing cox proportional regression, it was found that there was a statistically significant increase, of 0.5 %, in the hazard rate (hazard ratio 1.005) as IFAT titer increased by 1 unit (dilution), when both IFAT titers and clinical status were included in the model.
Discrepancy in DPP® CVL and IFAT results from samples of asymptomatic infected animals
Previous research has indicated that serological tests such as IFAT cannot reliably detect asymptomatic L. infantum infection (Mettler et al. 2005). To determine if DPP® CVL could complement IFAT in detecting infected dogs, we analyzed samples that were below the threshold for positive results in IFAT. Analyses of samples that were scored as negative by IFAT (IFAT <64)) versus DPP® CVL development time indicated a moderate correlation of results (Fig. 5c; r = −0.0066, 95 % CI = −0.4007, 0.3895, p value = ns). Further analysis using linear regressions showed that variations in DPP® CVL development time explained 16.90 % (goodness-of-fit r 2 = 0.1690). These data contrast with the comparison of serum with positive IFAT titers (IFAT ≥64) versus DPP® CVL development time, which had a fair correlation (Fig. 5d; r = −0.6077, 95 % CI = −0.8850, −0.0123, p value = 0.0474) and 38.03 % goodness of fit (r 2 = 0.3803). Thus, although samples from asymptomatic infected dogs were frequently scored as negative by IFAT, many were positive in DPP® CVL.
IFAT and DPP® CVL had a superior agreement IFAT had with qPCR
As a result of this high sensitivity and good specificity, we wondered whether the DPP® CVL test identified asymptomatic infection better than other serological tests, such as IFAT. We compared the sensitivity and specificity of DPP® CVL and qPCR using IFAT as the comparator. Against IFAT results, the DPP® CVL test had a sensitivity of 73 % and a specificity of 80 % (Table 3). When calculating sensitivity and specificity for qPCR against IFAT results, it was found that qPCR had a sensitivity of 45 % and a specificity of 90 %.
Discussion
A test that has the ability to rapidly detect and quantify both symptomatic VL and asymptomatic L. infantum infection could provide earlier diagnosis of the disease and identify those at greatest risk of developing symptoms. In this study, as expected, DPP® CVL was able to detect the majority of dogs displaying symptoms of CVL. By assessing the time required for positive bands to develop in DPP® CVL, we found that results correlated with both circulating parasite DNA levels, as determined by qPCR, and anti-Leishmania antibody titers, as determined by IFAT. We also observed a correlation of DPP® CVL results with asymptomatic L. infantum infection (as determined by qPCR) but a lack of correlation with IFAT as observed by the larger change in hazard rate when using PCR to predict time-to-positive band versus IFAT determined by cox proportional regression. Together, our data indicate that in the absence of a truly objective reader, recording the time for a positive band to appear in DPP® CVL represents a practical strategy with which to detect and semi-quantify L. infantum infection.
Patients may be positive at different stages of infection due to the varying availability of parasite targets or antibodies within samples used for detection (Rodríguez-Cortés et al. 2007). While qPCR is a sensitive test for directly detecting parasite nucleic acids and is believed to have a greater ability to detect infection earlier during the development of disease, the presence of nucleic acids in the blood can be transient. Unlike direct detection methods such as culture or qPCR, DPP® CVL can provide results rapidly at the site of sample collection. This attribute lends itself to use within surveillance programs that could be implemented on a community-wide scale to screen dogs (or humans) for L. infantum infection. Such assessments will be required to truly evaluate the impact of any control measures that are implemented for VL. Dogs that test positive by DPP® CVL but have no evidence of parasite DNA in the blood will, however, continue to confound diagnosis (Rodríguez-Cortés et al. 2007). Instead, guidelines regarding the use of both antibody detection and DNA methods are likely needed. In addition, long-term surveillance studies are required to generate the clinical data that will allow an accurate assessment of the rate of conversion of infection to disease.
IFAT and DPP® CVL are both antibody-detection tests, and it is not therefore surprising that IFAT and DPP® CVL had a higher correlation than that observed between DPP® CVL and qPCR. The improved performance of the DPP® CVL over IFAT may be due to the use of defined recombinant Leishmania proteins incorporated into DPP® CVL rather than the wide array of antigenic components present in the whole parasite preparation used in IFAT. In addition, the DPP® CVL test platform itself might also provide additional sensitivity that allows more reproducible detection of asymptomatic L. infantum infection. Similar to our data, several studies have shown that serological and immunochromatographic tests commonly correlate (da Silva et al. 2013; KoÇOĞLu et al. 2014; Laurenti et al. 2014; Monno et al. 2009). Higher IFAT titers correlated with the time required to reveal positive results in DPP® CVL development tests. Samples from animals that were culture positive or positive by IFAT were likely to develop positive bands in DPP® CVL in less than 3 min, but this correlation decreased dramatically for samples from asymptomatic L. infantum-infected animals. This conundrum of accurate detection of asymptomatic infection occurs within both dog and human populations. By definition, asymptomatic L. infantum-infected individuals do not show signs or symptoms of disease, which in many instances can be mediated through increased systemic antibodies and resultant antibody-antigen complexes, e.g., renal failure, wasting, and splenic and hepatic congestion (Esch et al. 2015; Grimaldi and Tesh 1993; Grimaldi et al. 2012; Moreno and Alvar 2002). If antibodies are not in high enough abundance to contribute to clinical disease, they are also unlikely to be detectable by IFAT.
To help monitor the progression of VL and evaluate asymptomatic infection, it is important to have a diagnostic test that quantifies the levels of infection and pathologic severity, as both of these correlate to transmissibility. A test that has the ability to cheaply and quantitatively detect both symptomatic VL and asymptomatic L. infantum infection could provide earlier diagnosis and better therapeutic decision making. This is of particular importance at this time because the WHO limits certain therapies only to the most severe VL cases (Alvar et al. 2012; Chappuis et al. 2007). When used in the semi-quantitative manner described here, DPP® CVL represents a simple and inexpensive tool to both confirm VL and detect L. infantum infection. Our data support the quantitative use of this test as a cost- and time-effective tool that could permit active surveillance within VL control programs.
References
Alvar J, Canavate C, Molina R, Moreno J, Nieto J (2004) Canine leishmaniasis. Adv Parasitol 57:1–88. doi:10.1016/s0065-308x(04)57001-x
Alvar J, Vélez ID, Bern C, Herrero M, Desjeux P, Cano J, Jannin J, Boer M (2012) Leishmaniasis worldwide and global estimates of its incidence. PLoS One 7(5):e35671. doi:10.1371/journal.pone.0035671
Baneth G, Aroch I (2008) Canine leishmaniasis: a diagnostic and clinical challenge. Vet J 175(1):14–15. doi:10.1016/j.tvjl.2006.11.011
Boehme CC, Hain U, Novosel A, Eichenlaub S, Fleischmann E, Loscher T (2006) Congenital visceral leishmaniasis. Emerg Infect Dis 12(2):359–360. doi:10.3201/eid1202.050449
Boelaert M, Verdonck K, Menten J, Sunyoto T, van Griensven J, Chappuis F, Rijal S (2014) Rapid tests for the diagnosis of visceral leishmaniasis in patients with suspected disease. The Cochrane database of systematic reviews 6:Cd009135. doi:10.1002/14651858.CD009135.pub2
Boggiatto PM, Gibson-Corley KN, Metz K, Gallup JM, Hostetter JM, Mullin K, Petersen CA (2011) Transplacental transmission of Leishmania infantum as a means for continued disease incidence in North America. PLoS Negl Trop Dis 5(4):e1019. doi:10.1371/journal.pntd.0001019
Boggiatto PM, Ramer-Tait AE, Metz K, Kramer EE, Gibson-Corley K, Mullin K, Hostetter JM, Gallup JM, Jones DE, Petersen CA (2010) Immunologic indicators of clinical progression during canine Leishmania infantum infection. Clin Vaccine Immunol 17(2):267–273. doi:10.1128/CVI.00456-09
Chappuis F, Sundar S, Hailu A, Ghalib H, Rijal S, Peeling RW, Alvar J, Boelaert M (2007) Visceral leishmaniasis: what are the needs for diagnosis, treatment and control? Nat Rev Microbiol 5(11):873–882. doi:10.1038/nrmicro1748
Ciaramella P, Oliva G, Luna RD, Gradoni L, Ambrosio R, Cortese L, Scalone A, Persechino A (1997) A retrospective clinical study of canine leishmaniasis in 150 dogs naturally infected by Leishmania infantum. Vet Rec 141(21):539–543
Cota GF, de Sousa MR, de Freitas Nogueira BM, Gomes LI, Oliveira E, Assis TSM, de Mendonça ALP, Pinto BF, Saliba JW, Rabello A (2013) Comparison of parasitological, serological, and molecular tests for visceral leishmaniasis in HIV-infected patients: a cross-sectional delayed-type study. AmJTrop Med Hyg 89(3):570–577. doi:10.4269/ajtmh.13-0239
Coura-Vital W, Ker HG, Roatt BM, Aguiar-Soares RDO, Leal GGA, Moreira ND, Oliveira LAM, de Menezes Machado EM, Morais MHF, Corrêa-Oliveira R, Carneiro M, Reis AB (2014) Evaluation of change in canine diagnosis protocol adopted by the visceral leishmaniasis control program in Brazil and a new proposal for diagnosis. PLoS One 9(3):e91009. doi:10.1371/journal.pone.0091009
Courtenay O, Carson C, Calvo-Bado L, Garcez LM, Quinnell RJ (2014) Heterogeneities in Leishmania infantum infection: using skin parasite burdens to identify highly infectious dogs. PLoS Negl Trop Dis 8(1):e2583. doi:10.1371/journal.pntd.0002583
da Silva DA, Madeira Mde F, Abrantes TR, Filho CJ, Figueiredo FB (2013) Assessment of serological tests for the diagnosis of canine visceral leishmaniasis. Vet J 195(2):252–253. doi:10.1016/j.tvjl.2012.06.010
de Vries PJ, van der Meide WF, Godfried MH, Schallig HDFH, Dinant HJ, Faber WR (2006) Quantification of the response to miltefosine treatment for visceral leishmaniasis by QT-NASBA. Trans R Soc Trop Med Hyg 100(12):1183–1186. doi:10.1016/j.trstmh.2006.01.002
Drahota J, Martin-Martin I, Sumova P, Rohousova I, Jimenez M, Molina R, Volf P (2014) Recombinant antigens from Phlebotomus perniciosus saliva as markers of canine exposure to visceral leishmaniases vector. PLoS Negl Trop Dis 8(1):e2597. doi:10.1371/journal.pntd.0002597
Dye C, Killick-Kendrick R, Vitutia MM, Walton R, Killick-Kendrick M, Harith AE, Guy MW, Canavate MC, Hasibeder G (1992) Epidemiology of canine leishmaniasis: prevalence, incidence and basic reproduction number calculated from a cross-sectional serological survey on the island of Gozo, Malta. Parasitology 105(Pt 1):35–41
Ejazi SA, Ali N (2013) Developments in diagnosis and treatment of visceral leishmaniasis during the last decade and future prospects. Expert Rev Anti-Infect Ther 11(1):79–98. doi:10.1586/eri.12.148
Ergen EN, King AH, Tuli M (2015) Cutaneous leishmaniasis: an emerging infectious disease in travelers. Cutis 96(4):E22–E26
Ertabaklar H, Ozlem Caliskan S, Boduc E, Ertug S (2015) Comparison of direct microscopy, culture and polymerase chain reaction methods for the diagnosis of cutaneous leishmaniasis. Mikrobiyoloji bulteni 49(1):77–84
Esch KJ, Juelsgaard R, Martinez PA, Jones DE, Petersen CA (2013) Programmed death 1-mediated T cell exhaustion during visceral leishmaniasis impairs phagocyte function. Journal of immunology (Baltimore, Md : 1950) 191(11):5542–5550. doi:10.4049/jimmunol.1301810
Esch KJ, Schaut RG, Lamb IM, Clay G, Morais Lima AL, do Nascimento PR, Whitley EM, Jeronimo SM, Sutterwala FS, Haynes JS, Petersen CA (2015) Activation of autophagy and nucleotide-binding domain Leucine-rich repeat-containing-like receptor family, pyrin domain-containing 3 Inflammasome during Leishmania infantum-associated glomerulonephritis. Am J Pathol 185(8):2105–2117. doi:10.1016/j.ajpath.2015.04.017
Foglia Manzillo V, Di Muccio T, Cappiello S, Scalone A, Paparcone R, Fiorentino E, Gizzarelli M, Gramiccia M, Gradoni L, Oliva G (2013) Prospective study on the incidence and progression of clinical signs in naive dogs naturally infected by Leishmania infantum. PLoS Negl Trop Dis 7(5):e2225. doi:10.1371/journal.pntd.0002225
Francino O, Altet L, Sanchez-Robert E, Rodriguez A, Solano-Gallego L, Alberola J, Ferrer L, Sanchez A, Roura X (2006) Advantages of real-time PCR assay for diagnosis and monitoring of canine leishmaniosis. Vet Parasitol 137(3–4):214–221. doi:10.1016/j.vetpar.2006.01.011
Gaskin AA, Schantz P, Jackson J, Birkenheuer A, Tomlinson L, Gramiccia M, Levy M, Steurer F, Kollmar E, Hegarty BC, Ahn A, Breitschwerdt EB (2002) Visceral Leishmaniasis in a New York foxhound kennel. J Vet Intern Med 16(1):34. doi:10.1892/0891-6640(2002)016<0034:vliany>2.3.co;2
Gibson-Corley KN, Hostetter JM, Hostetter SJ, Mullin K, Ramer-Tait AE, Boggiatto PM, Petersen CA (2008) Disseminated Leishmania infantum infection in two sibling foxhounds due to possible vertical transmission. Can Vet J 49(10):1005–1008
Grimaldi G Jr, Tesh RB (1993) Leishmaniases of the New World: current concepts and implications for future research. Clin Microbiol Rev 6(3):230–250
Grimaldi G Jr, Teva A, Ferreira AL, dos Santos CB, Pinto I, de-Azevedo CT, Falqueto A (2012) Evaluation of a novel chromatographic immunoassay based on Dual-Path Platform technology (DPP(R) CVL rapid test) for the serodiagnosis of canine visceral leishmaniasis. Trans R Soc Trop Med Hyg 106(1):54–59. doi:10.1016/j.trstmh.2011.10.001
Herwaldt BL, Stokes SL, Juranek DD (1993) American cutaneous leishmaniasis in U.S. travelers. Ann Intern Med 118(10):779–784
Karkamo V, Kaistinen A, Nareaho A, Dillard K, Vainio-Siukola K, Vidgren G, Tuoresmaki N, Anttila M (2014) The first report of autochthonous non-vector-borne transmission of canine leishmaniosis in the Nordic countries. Acta Vet Scand 56(1):84. doi:10.1186/s13028-014-0084-9
KoÇOĞLu ME, TaŞ T, MengeloĞLu FZ, ÖZsoy Ş, Bucak Ö (2014) Evaluation of 4 methods for the serological diagnosis of Epstein–Barr virus infection using an immunofluorescence assay as the reference method. TURKISH JOURNAL OF MEDICAL SCIENCES 44:914–919. doi:10.3906/sag-1308-38
Laurenti MD, de Santana Leandro MV, Tomokane TY, De Lucca HRL, Aschar M, Souza CSF, Silva RM, Marcondes M, da Matta VLR (2014) Comparative evaluation of the DPP® CVL rapid test for canine serodiagnosis in area of visceral leishmaniasis. Vet Parasitol 205(3–4):444–450. doi:10.1016/j.vetpar.2014.09.002
Maroli M, Rossi L, Baldelli R, Capelli G, Ferroglio E, Genchi C, Gramiccia M, Mortarino M, Pietrobelli M, Gradoni L (2008) The northward spread of leishmaniasis in Italy: evidence from retrospective and ongoing studies on the canine reservoir and phlebotomine vectors. Tropical Med Int Health 13(2):256–264. doi:10.1111/j.1365-3156.2007.01998.x
Meinecke CK, Schottelius J, Oskam L, Fleischer B (1999) Congenital transmission of visceral leishmaniasis (Kala Azar) from an asymptomatic mother to her child. Pediatrics 104(5):e65
Mettler M, Grimm F, Capelli G, Camp H, Deplazes P (2005) Evaluation of enzyme-linked immunosorbent assays, an immunofluorescent-antibody test, and two rapid tests (immunochromatographic-dipstick and gel tests) for serological diagnosis of symptomatic and asymptomatic Leishmania infections in dogs. J Clin Microbiol 43(11):5515–5519. doi:10.1128/JCM.43.11.5515-5519.2005
Monno R, Giannelli G, Rizzo C, De Vito D, Fumarola L (2009) Recombinant K39 immunochromatographic test for diagnosis of human leishmaniasis. Future Microbiol 4(2):159–170. doi:10.2217/17460913.4.2.159
Moreno J, Alvar J (2002) Canine leishmaniasis: epidemiological risk and the experimental model. Trends Parasitol 18(9):399–405
Mukhtar M, Abdoun A, Ahmed AE, Ghalib H, Reed SG, Boelaert M, Menten J, Khair MM, Howard RF (2015) Diagnostic accuracy of rK28-based immunochromatographic rapid diagnostic tests for visceral leishmaniasis: a prospective clinical cohort study in Sudan. Trans R Soc Trop Med Hyg 109(9):594–600. doi:10.1093/trstmh/trv060
Naucke TJ, Lorentz S (2012) First report of venereal and vertical transmission of canine leishmaniosis from naturally infected dogs in Germany. Parasit Vectors 5:67. doi:10.1186/1756-3305-5-67
Osorio Y, Rodriguez LD, Bonilla DL, Peniche AG, Henao H, Saldarriaga O, Travi BL (2012) Congenital transmission of experimental leishmaniasis in a hamster model. AmJTrop Med Hyg 86(5):812–820. doi:10.4269/ajtmh.2012.11-0458
Otero AC, da Silva VO, Luz KG, Palatnik M, Pirmez C, Fernandes O, Palatnik de Sousa CB (2000) Short report: occurrence of Leishmania donovani DNA in donated blood from seroreactive Brazilian blood donors. AmJTrop Med Hyg 62(1):128–131
Owens SD, Oakley DA, Marryott K, Hatchett W, Walton R, Nolan TJ, Newton A, Steurer F, Schantz P, Giger U (2001) Transmission of visceral leishmaniasis through blood transfusions from infected English foxhounds to anemic dogs. J Am Vet Med Assoc 219(8):1076–1083
Papageorgiou T, Pana Z, Tragiannidis A, Tsotoulidou V, Pratsiou E, Tzouvelekis G, Athanassiadou F (2010) Letter to the editor. J Paediatr Child Health 46(10):611–612. doi:10.1111/j.1440-1754.2010.01862.x
Parrot L, Donatien A, Lestoquard F (1930) On the development of the parasite of canine visceral leishmaniasis in Phlebotomus major var perniciosus Newstead. Bull Soc Pathol Exot 23(7):724–726
Pattabhi S, Whittle J, Mohamath R, El-Safi S, Moulton GG, Guderian JA, Colombara D, Abdoon AO, Mukhtar MM, Mondal D, Esfandiari J, Kumar S, Chun P, Reed SG, Bhatia A (2010) Design, development and evaluation of rK28-based point-of-care tests for improving rapid diagnosis of visceral leishmaniasis. PLoS Negl Trop Dis 4(9) doi:10.1371/journal.pntd.0000822
Petersen CA (2009a) Leishmaniasis, an emerging disease found in companion animals in the United States. Top Companion Anim Med 24(4):182–188. doi:10.1053/j.tcam.2009.06.006
Petersen CA (2009b) New means of canine leishmaniasis transmission in North America: the possibility of transmission to humans still unknown. Interdisciplinary Perspectives on Infectious Diseases 2009:1–5. doi:10.1155/2009/802712
Petersen CA, Barr SC (2009) Canine leishmaniasis in North America: emerging or newly recognized? Vet Clin North Am Small Anim Pract 39(6):1065–1074 . doi:10.1016/j.cvsm.2009.06.008vi
Reis AB, Martins-Filho OA, Teixeira-Carvalho A, Giunchetti RC, Carneiro CM, Mayrink W, Tafuri WL, Correa-Oliveira R (2009) Systemic and compartmentalized immune response in canine visceral leishmaniasis. Vet Immunol Immunopathol 128(1–3):87–95. doi:10.1016/j.vetimm.2008.10.307
Rodríguez-Cortés A, Ojeda A, Francino O, López-Fuertes L, Timón M, Alberola J (2010) Leishmania infection: laboratory diagnosing in the absence of a “gold standard”. AmJTrop Med Hyg 82(2):251–256. doi:10.4269/ajtmh.2010.09-0366
Rodríguez-Cortés A, Ojeda A, López-Fuertes L, Timón M, Altet L, Solano-Gallego L, Sánchez-Robert E, Francino O, Alberola J (2007) A long term experimental study of canine visceral leishmaniasis. Int J Parasitol 37(6):683–693. doi:10.1016/j.ijpara.2006.11.007
Rodriguez-Cortes A, Ojeda A, Todoli F, Alberola J (2013) Performance of commercially available serological diagnostic tests to detect Leishmania infantum infection on experimentally infected dogs. Vet Parasitol 191(3–4):363–366. doi:10.1016/j.vetpar.2012.09.009
Rosypal AC, Troy GC, Zajac AM, Frank G, Lindsay DS (2005) Transplacental transmission of a North American isolate of Leishmania infantum in an experimentally infected beagle. J Parasitol 91(4):970–972. doi:10.1645/ge-483r.1
Santos TR, Carreira VS, Ferrari HF, Moreira MA, Luvizotto MC (2014) Comparison of PCR with stained slides of bone marrow and lymph nodes aspirates with suspect diagnosis for leishmaniasis. Acta Trop 140:137–140. doi:10.1016/j.actatropica.2014.08.016
Schantz PM, Steurer FJ, Duprey ZH, Kurpel KP, Barr SC, Jackson JE, Breitschwerdt EB, Levy MG, Fox JC (2005) Autochthonous visceral leishmaniasis in dogs in North America. J Am Vet Med Assoc 226(8):1316–1322
Schaut RG, Robles-Murguia M, Juelsgaard R, Esch KJ, Bartholomay LC, Ramalho-Ortigao M, Petersen CA (2015) Vectorborne transmission of Leishmania infantum from hounds, United States. Emerg Infect Dis 21(12):2209–2212. doi:10.3201/eid2112.141167
Silva FL, Oliveira RG, Silva TM, Xavier MN, Nascimento EF, Santos RL (2009) Venereal transmission of canine visceral leishmaniasis. Vet Parasitol 160(1–2):55–59. doi:10.1016/j.vetpar.2008.10.079
Solano-Gallego L, Koutinas A, Miro G, Cardoso L, Pennisi MG, Ferrer L, Bourdeau P, Oliva G, Baneth G (2009) Directions for the diagnosis, clinical staging, treatment and prevention of canine leishmaniosis. Vet Parasitol 165(1–2):1–18. doi:10.1016/j.vetpar.2009.05.022
Song EH, Osanya AO, Petersen CA, Pohl NL (2010) Synthesis of multivalent tuberculosis and Leishmania-associated capping carbohydrates reveals structure-dependent responses allowing immune evasion. J Am Chem Soc 132(33):11428–11430. doi:10.1021/ja103351m
Srividya G, Kulshrestha A, Singh R, Salotra P (2011) Diagnosis of visceral leishmaniasis: developments over the last decade. Parasitol Res 110(3):1065–1078. doi:10.1007/s00436-011-2680-1
Stevenson M, Nunes T, Heuer C, Marshall J, Sanchez J, Thornton R, Reiczigel J, Robison-Cox J, Sebastiani P, Solymos P, Yoshida K, Firestone S (2015) epiR: Tools for the analysis of epidemiological data. vol R package version 0.9–62. R
Symmers WS (1960) Leishmaniasis acquired by contagion: a case of marital infection in Britain. Lancet 1(7116):127–132
Travi BL, Velez ID, Brutus L, Segura I, Jaramillo C, Montoya J (1990) Lutzomyia evansi, an alternate vector of Leishmania chagasi in a Colombian focus of visceral leishmaniasis. Trans R Soc Trop Med Hyg 84(5):676–677
Verma S, Kumar R, Katara GK, Singh LC, Negi NS, Ramesh V, Salotra P (2010) Quantification of parasite load in clinical samples of leishmaniasis patients: IL-10 level correlates with parasite load in visceral leishmaniasis. PLoS One 5(4):e10107. doi:10.1371/journal.pone.0010107
Zinchuk A, Nadraga A (2010) Congenital visceral leishmaniasis in Ukraine: case report. Ann Trop Paediatr 30(2):161–164. doi:10.1179/146532810x12703902516400
Acknowledgments
We would like to thank our collaborating hunting dog kennels for assistance with their priceless dogs. We would also like to thank members of the Mary Wilson lab and Louis Palen for their assistance with performing the cultures and the DPP® CVL tests. We recognize the contributions provided by students in EPID:158:001 University of Iowa College of Public Health Public Health Lab Techniques Course: Albertson, J., Brown, A., Chang, N., Granseth, G., Johnson, C., Lueck, C., Oltman, S., and Ritter, R.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Funding
This work was funded by grant D13CA-501 from the Morris Animal Foundation.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Animals were enrolled with the informed consent of the caretaker, and evaluations followed protocols as approved by the Iowa State University and University of Iowa Animal Control and Use Committees (IACUC).
Informed consent
There were no human subjects involved in this study.
Authors’ contributions
ML performed physical examinations, DPP® CVL diagnostic tests, statistical analyses, and writing the manuscript. AT performed DPP® CVL and qPCR diagnostic tests, statistical analyses, and manuscript figure development. BS performed DPP® CVL and qPCR diagnostic tests and figure/table development. EPID:158:001 performed DPP® CVL diagnostic tests. MK performed the cultures. HF carried out cultures and DPP® CVL tests. JE, RFH, and ACV provided feedback during analysis of results and editorial assistance with the manuscript. MSD provided feedback during analysis of results, writing, and editing of the manuscript. CP provided study design, physical examinations, writing, and editing of the manuscript. All authors read and approved the final version of the manuscript.
Rights and permissions
About this article
Cite this article
Larson, M., Toepp, A., Scott, B. et al. Semi-quantitative measurement of asymptomatic L. infantum infection and symptomatic visceral leishmaniasis in dogs using Dual-Path Platform® CVL. Appl Microbiol Biotechnol 101, 381–390 (2017). https://doi.org/10.1007/s00253-016-7925-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00253-016-7925-6