Abstract
Background
Safety concerns are increasingly raised regarding the use of gadolinium-based contrast media for MR imaging.
Objective
To determine the accuracy of pre-contrast abdominal MR imaging for lesion detection and characterization in pediatric oncology patients.
Materials and methods
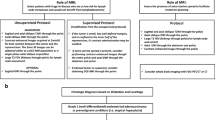
We included 120 children (37 boys and 83 girls; mean age 8.94 years) referred by oncology services. Twenty-five had MRI for the first time and 95 were follow-up scans. Two authors independently reviewed pre-contrast MR images to note the following information about the lesions: location, number, solid vs. cystic and likely nature. Pre- and post-contrast imaging reviewed together served as the reference standard.
Results
The overall sensitivity was 88% for the first reader and 90% for the second; specificity was 94% and 91%; positive predictive value was 96% and 94%; negative predictive value was 82% and 84%; accuracy of pre-contrast imaging for lesion detection as compared to the reference standard was 90% for both readers. The difference between mean number of lesions detected on pre-contrast imaging and reference standard was not significant for either reader (reader 1, P = 0.072; reader 2, P = 0.071). There was substantial agreement (kappa values of 0.76 and 0.72 for readers 1 and 2) between pre-contrast imaging and reference standard for determining solid vs. cystic lesion and likely nature of the lesion. The addition of post-contrast imaging increased confidence of both readers significantly (P < 0.0001), but the interobserver agreement for the change in confidence was poor (kappa 0.12).
Conclusion
Pre-contrast abdominal MR imaging has high accuracy in lesion detection in pediatric oncology patients and shows substantial agreement with the reference standard for characterization of lesions. Gadolinium-based contrast media administration cannot be completely eliminated but can be avoided in many cases, with the decision made on a case-by-case basis, taking into consideration location and type of tumor.




Similar content being viewed by others
References
Michael R (2008) Potential of MR-imaging in the paediatric abdomen. Eur J Radiol 68:235–244
Kaste SC, McCarville MB (2008) Imaging pediatric abdominal tumors. Semin Roentgenol 43:50–59
McHugh K, Roebuck DJ (2014) Pediatric oncology surveillance imaging: two recommendations. Abandon CT scanning, and randomize to imaging or solely clinical follow-up. Pediatr Blood Cancer 61:3–6
Olsen OE (2013) Advances in pediatric oncology MRI. Acta Radiol 54:1030–1036
American College of Radiology (2015) ACR-SAR-SPR practice parameter for the performance of magnetic resonance imaging (MRI) of the abdomen (excluding the liver). http://www.acr.org/~/media/6B520D299C0B4B018A90BE21A79D4F72.pdf.. Accessed 24 May 2016
Petrou M, Foerster B, Maly PV et al (2007) Added utility of gadolinium in the magnetic resonance imaging (MRI) workup of seizures in children younger than 2 years. J Child Neurol 22:200–203
Sundgren PC, Leander P (2011) Is administration of gadolinium-based contrast media to pregnant women and small children justified? J Magn Reson Imaging 34:750–757
Mendichovszky IA, Marks SD, Simcock CM et al (2008) Gadolinium and nephrogenic systemic fibrosis: time to tighten practice. Pediatr Radiol 38:489–496, quiz 602–603
Kanda T, Ishii K, Kawaguchi H et al (2014) High signal intensity in the dentate nucleus and globus pallidus on unenhanced T1-weighted MR images: relationship with increasing cumulative dose of a gadolinium-based contrast material. Radiology 270:834–841
McDonald RJ, McDonald JS, Kallmes DF et al (2015) Intracranial gadolinium deposition after contrast-enhanced MR imaging. Radiology 275:772–782
Diana Afonso P, Kosinski AS, Spritzer CE (2013) Following unenhanced MRI assessment for local recurrence after surgical resection of mesenchymal soft tissue tumors, do additional gadolinium-enhanced images change reader confidence or diagnosis? Eur J Radiol 82:806–813
Macari M, Lee T, Kim S et al (2009) Is gadolinium necessary for MRI follow-up of cystic lesions in the pancreas? Preliminary results. AJR Am J Roentgenol 192:159–164
Gollub MJ, Lakhman Y, McGinty K et al (2015) Does gadolinium-based contrast material improve diagnostic accuracy of local invasion in rectal cancer MRI? A multireader study. AJR Am J Roentgenol 204:W160–W167
Averill LW, Hernandez A, Gonzalez L (2009) Diagnosis of osteomyelitis in children: utility of fat-suppressed contrast-enhanced MRI. AJR Am J Roentgenol 192:1232–1238
Kan JH, Young RS, Yu C et al (2010) Clinical impact of gadolinium in the MRI diagnosis of musculoskeletal infection in children. Pediatr Radiol 40:1197–1205
Weiss PF, Xiao R, Biko DM et al (2015) Detection of inflammatory sacroiliitis in children with magnetic resonance imaging: is gadolinium-contrast enhancement necessary? Arthritis Rheum 67:2250–2256
Klenk C, Gawande R, Tran VT et al (2016) Progressing toward a cohesive pediatric 18 F-FDG PET/MR protocol: is administration of gadolinium chelates necessary? J Nucl Med 57:70–77
Viera AJ, Garrett JM (2005) Understanding interobserver agreement: the kappa statistic. Fam Med 37:360–363
Rosner B (1995) Fundamentals of biostatistics. Duxbury Press, Toronto
Osman S, Lehnert BE, Elojeimy S et al (2013) A comprehensive review of the retroperitoneal anatomy, neoplasms, and pattern of disease spread. Curr Probl Diagn Radiol 42:191–208
Eberhardt SC, Johnson JA, Parsons RB (2013) Oncology imaging in the abdomen and pelvis: where cancer hides. Abdom Imaging 38:647–671
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Mohd Zaki, F., Moineddin, R., Grant, R. et al. Accuracy of pre-contrast imaging in abdominal magnetic resonance imaging of pediatric oncology patients. Pediatr Radiol 46, 1684–1693 (2016). https://doi.org/10.1007/s00247-016-3664-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-016-3664-1