Abstract
Background
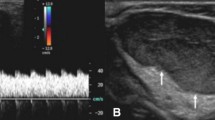
The absence of a discrete mass, surrounding signal abnormality and solid enhancement are imaging features that have traditionally been used to differentiate soft-tissue arteriovenous malformations from vascular tumors on MRI. We have observed that these findings are not uncommon in arteriovenous malformations, which may lead to misdiagnosis or inappropriate treatment.
Objective
To estimate the frequency of atypical MRI features in soft-tissue arteriovenous malformations and assess their relationship to lesion size, location, tissue type involved and vascular architecture.
Materials and methods
Medical records, MRI and histopathology were reviewed in consecutive patients with soft-tissue arteriovenous malformations in a multidisciplinary vascular anomalies clinic. Arteriovenous malformations were divided into those with and without atypical MRI findings (perilesional T2 signal abnormality, enhancement and/or a soft-tissue mass). Lesion location, size, tissue involved and vascular architecture were also compared between groups. Tissue stains were reviewed in available biopsy or resection specimens to assess relationships between MRI findings and histopathology.
Results
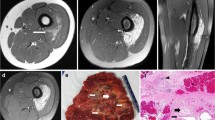
Thirty patients with treatment-naïve arteriovenous malformations were included. Fifteen lesions demonstrated atypical MRI. There was no difference in age, gender, lesion size or involved body part between the groups. However, more than half of the atypical lesions demonstrated multicompartmental involvement, and tiny intralesional flow voids were more common in atypical arteriovenous malformations. Histopathology also differed in atypical cases, showing densely packed endothelial cells with connective tissue architectural distortion and edema.
Conclusion
Arteriovenous malformations may exhibit features of a vascular tumor on MRI, particularly when multicompartmental and/or containing tiny internal vessels. These features are important to consider in suspected fast-flow vascular malformations and may have implications with respect to their treatment.








Similar content being viewed by others
References
Donnelly LF, Adams DM, Bisset GS 3rd (2000) Vascular malformations and hemangiomas: a practical approach in a multidisciplinary clinic. AJR Am J Roentgenol 174:597–608
Dubois J, Alison M (2010) Vascular anomalies: what a radiologist needs to know. Pediatr Radiol 40:895–905
Konez O, Burrows PE (2002) Magnetic resonance of vascular anomalies. Magn Reson Imaging Clin N Am 10:363–388, vii
Enjolras O, Wassef M, Chapot R (2007) Color atlas of vascular tumors and vascular malformations. Cambridge University Press, Cambridge
Hovius SE, Borg DH, Paans PR et al (1996) The diagnostic value of magnetic resonance imaging in combination with angiography in patients with vascular malformations: a prospective study. Ann Plast Surg 37:278–285
Robertson RL, Robson CD, Barnes PD et al (1999) Head and neck vascular anomalies of childhood. Neuroimaging Clin N Am 9:115–132
Yilmaz S, Kozakewich HP, Alomari AI et al (2014) Intramuscular capillary-type hemangioma: radiologic-pathologic correlation. Pediatr Radiol 44:558–5658
Meijer-Jorna LB, van der Loos CM, de Boer OJ et al (2007) Microvascular proliferation in congenital vascular malformations of skin and soft tissue. J Clin Pathol 60:798–803
Meijer-Jorna LB, van der Loos CM, Teeling P et al (2012) Proliferation and maturation of microvessels in arteriovenous malformations—expression patterns of angiogenic and cell cycle-dependent factors. J Cutan Pathol 39:610–620
Saliou G, Krings T, Rutgers DR et al (2011) PWI-MRI and contrast extravasation in brain AVM help to estimate angiogenic activity. Neuroradiology 53:793–800
Conflicts of interest
Dr. Frieden is a consultant for Pierre Fabre. Drs. Patel, Schulman, Ruben, Hoffman, Dowd and Hess have no disclosures.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Patel, A.S., Schulman, J.M., Ruben, B.S. et al. Atypical MRI features in soft-tissue arteriovenous malformation: a novel imaging appearance with radiologic-pathologic correlation. Pediatr Radiol 45, 1515–1521 (2015). https://doi.org/10.1007/s00247-015-3359-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-015-3359-z