Abstract
Introduction
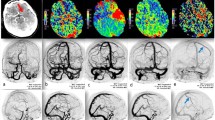
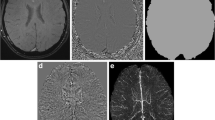
Peri-ischemic early venous filling (PEVD) has been reported to occur at certain stages of brain infarction and has previously been termed as "luxury perfusion". We report on the significance of PEVD after a successful endovascular recanalization.
Methods
We retrospectively evaluated all patients who underwent endovascular stroke treatment from February 2006 to April 2010 in two centers. PEVD was rated as present or absent. Infarction was evaluated on computed tomography (CT) ≥18 h post-treatment. Localization of the PEVD and the infarction was noted for the anterior and posterior circulation; for the anterior circulation, also deep and superficial veins/brain regions were defined.
Results
A total of 151 of the 175 patients developed an infarct. Of these 151 patients, 118 had PEVD (sensitivity 78.1%); meanwhile, 20 of 24 patients without an infarction had no PEVD (specificity 83.3%). Consistent localization of the PEVD and the infarct was seen in 107/151 patients (70.9%); in 28 of these 107 cases, the territory of PEVD was smaller than the infarct (26.2%) and exceeded it in 7/107 patients (5.6%). Territorial congruency of the PEVD and the final infarct was 57.6–75% for deep/superficial brain regions of the anterior, but only 16.7% for the posterior circulation. Separate evaluation for the anterior circulation resulted in a 94.9% sensitivity and an 81.0% specificity.
Conclusion
PEVD is a potential angiographic predictor for irreversible regional tissue damage and subsequent infarction despite successful recanalization. This finding deserves further studies and may influence therapeutic decisions such as post-treatment anticoagulative medication. It may also be considered in potential refined classifications of angiographic reperfusion success in the future.




Similar content being viewed by others
References
Donnan G, Fisher M, Macleod M, Davis S (2008) Stroke. Lancet 371(9624):1612–1623
The World Health Report (2004) Annex table 2: Deaths by cause, sex and mortality stratum in WHO regions, estimates for 2002. World Health Organization, Geneva, 2004 Contract No.: Document Number
Castaño C, Dorado L, Guerrero C, Millán M, Gomis M, Perez de la Ossa N et al (2010) Mechanical thrombectomy with the Solitaire AB device in large artery occlusions of the anterior circulation: a pilot study. Stroke 41(8):1836–1840
Roth C, Papanagiotou P, Behnke S, Walter S, Haass A, Becker C et al (2010) Stent-assisted mechanical recanalization for treatment of acute intracerebral artery occlusions. Stroke
Menon BK, Kochar P, Ah-Seng A, Almekhlafi MA, Modi J, Wong JH, Hudon ME, Morrish W, Demchuk AM, Goyal M (2011) Initial experience with a self-expanding retrievable stent for recanalization of large vessel occlusions in acute ischemic stroke. Neuroradiology, 2011 Jan 12
Kim SM, Lee DH, Kwon SU, Choi CG, Kim SJ, Suh DC (2011) Treatment of acute ischemic stroke: feasibility of primary or secondary use of a self-expanding stent (Neuroform) during local intra-arterial thrombolysis. Neuroradiology, 2011 Jan 1
Liebeskind D (2010) Reperfusion for acute ischemic stroke: arterial revascularization and collateral therapeutics. Curr Opin Neurol 23(1):36–45
De Silva D, Fink J, Christensen S, Ebinger M, Bladin C, Levi C et al (2009) Assessing reperfusion and recanalization as markers of clinical outcomes after intravenous thrombolysis in the echoplanar imaging thrombolytic evaluation trial (EPITHET). Stroke 40(8):2872–2874
Tomsick T, Broderick J, Carrozella J, Khatri P, Hill M, Palesch Y et al (2008) Revascularization results in the Interventional Management of Stroke II trial. AJNR Am J Neuroradiol 29(3):582–587
Woringer E, Baumgartner J, Braun J (1958) Sign of early local-regional venous opacification during rapid carotid serio-angiography. Acta Radiol 50(1–2):125–131
Cronqvist S, Laroche F (1967) Transitory hyperaemia in focal cerebral vascular lesions studied by angiography and regional cerebral blood flow measurements. Br J Radiol 40(472):270–274
Taveras J, Gilson J, Davis D, Kilgore B, Rumbaugh C (1969) Angiography in cerebral infarction. Radiology 93(3):549–558
Olsen TS, Skriver EB, Herning M (1991) Radiologic manifestations of focal cerebral hyperemia in acute stroke. Acta Radiol 32(2):100–104
Ohta H, Nakano S et al (2004) Appearance of early venous filling during intra-arterial reperfusion therapy for acute middle cerebral artery occlusion: a predictive sign for hemorrhagic complications. Stroke 35(4):893–898
Lassen N (1966) The luxury-perfusion syndrome and its possible relation to acute metabolic acidosis localised within the brain. Lancet 2(7473):1113–1115
Marchal G, Furlan M, Beaudouin V, Rioux P, Hauttement J, Serrati C et al (1996) Early spontaneous hyperperfusion after stroke. A marker of favourable tissue outcome? Brain 119(Pt 2):409–419
Fink GR, Herholz K, Pietrzyk U, Huber M, Heiss WD (1993) Peri-infarct perfusion in human ischemia: its relation to tissue metabolism, morphology, and clinical outcome. J Stroke Cerebrovasc Dis (3):123–131
Ackerman R, Subramanyam R, Correia J, Alpert N, Taveras J (1980) Positron imaging of cerebral blood flow during continuous inhalation of C15O2. Stroke 11(1):45–49
Ackerman R, Correia J, Alpert N, Baron J, Gouliamos A, Grotta J et al (1981) Positron imaging in ischemic stroke disease using compounds labeled with oxygen 15. Initial results of clinicophysiologic correlations. Arch Neurol 38(9):537–543
Baron J, Bousser M, Rey A, Guillard A, Comar D, Castaigne P (1981) Reversal of focal "misery-perfusion syndrome" by extra-intracranial arterial bypass in hemodynamic cerebral ischemia. A case study with 15O positron emission tomography. Stroke 12(4):454–459
Sugiyama H, Christensen J, Skyhøj Olsen T, Lassen N (1986) Monitoring CBF in clinical routine by dynamic single photon emission tomography (SPECT) of inhaled xenon-133. Stroke 17(6):1179–1182
Lenzi G, Frackowiak R, Jones T (1982) Cerebral oxygen metabolism and blood flow in human cerebral ischemic infarction. J Cereb Blood Flow Metab 2(3):321–335
Tran Dinh Y, Ille O, Guichard J, Haguenau M, Seylaz J (1997) Cerebral postischemic hyperperfusion assessed by Xenon-133 SPECT. J Nucl Med 38(4):602–607
Yonas H, Gur D, Claassen D, Wolfson SJ, Moossy J (1990) Stable xenon-enhanced CT measurement of cerebral blood flow in reversible focal ischemia in baboons. J Neurosurg 73(2):266–273
Heiss W, Graf R, Löttgen J, Ohta K, Fujita T, Wagner R et al (1997) Repeat positron emission tomographic studies in transient middle cerebral artery occlusion in cats: residual perfusion and efficacy of postischemic reperfusion. J Cereb Blood Flow Metab 17(4):388–400
Graf R, Lottgen J, Ohta K, Wagner R, Rosner G, Pietrzyk U (1997) Dynamics of postischemic perfusion following transient MCA occlusion in cats determined by sequential PET. J Cereb Blood Flow Metab, S323
Rowed D, Stark V, Hoffer P, Mullan S (1972) Cerebral arteriovenous shunts re-examined. Stroke 3(5):592–600
Benda P, Brownell G (1960) The fate of radioactive emboli injected into the cerebral circulation, the brain as a filter. J Neuropathol Exp Neurol 19:383–406
del Zoppo G, Higashida R, Furlan A, Pessin M, Rowley H, Gent M (1998) PROACT: a phase II randomized trial of recombinant pro-urokinase by direct arterial delivery in acute middle cerebral artery stroke. PROACT Investigators. Prolyse in Acute Cerebral Thromboembolism. Stroke 29(1):4–11
Furlan A, Abou-Chebl A (2002) The role of recombinant pro-urokinase (r-pro-UK) and intra-arterial thrombolysis in acute ischaemic stroke: the PROACT trials. Prolyse in Acute Cerebral Thromboembolism. Curr Med Res Opin 18(Suppl 2):s44–s47
Kase C, Furlan A, Wechsler L, Higashida R, Rowley H, Hart R et al (2001) Cerebral hemorrhage after intra-arterial thrombolysis for ischemic stroke: the PROACT II trial. Neurology 57(9):1603–1610
Roberts H, Dillon W, Furlan A, Wechsler L, Rowley H, Fischbein N et al (2002) Computed tomographic findings in patients undergoing intra-arterial thrombolysis for acute ischemic stroke due to middle cerebral artery occlusion: results from the PROACT II trial. Stroke 33(6):1557–1565
Mazighi M, Serfaty J, Labreuche J, Laissy J, Meseguer E, Lavallée P et al (2009) Comparison of intravenous alteplase with a combined intravenous-endovascular approach in patients with stroke and confirmed arterial occlusion (RECANALISE study): a prospective cohort study. Lancet Neurol 8(9):802–809
Smith W, Sung G, Saver J, Budzik R, Duckwiler G, Liebeskind D et al (2008) Mechanical thrombectomy for acute ischemic stroke: final results of the Multi MERCI trial. Stroke 39(4):1205–1212
Flint A, Duckwiler G, Budzik R, Liebeskind D, Smith W, MaMMW C (2007) Mechanical thrombectomy of intracranial internal carotid occlusion: pooled results of the MERCI and Multi MERCI Part I trials. Stroke 38(4):1274–1280
Investigators PPST (2009) The penumbra pivotal stroke trial: safety and effectiveness of a new generation of mechanical devices for clot removal in intracranial large vessel occlusive disease. Stroke 40(8):2761–2768
Eckert B, Küsel T, Leppien A, Michels P, Müller-Jensen A, Fiehler J (2011) Clinical outcome and imaging follow-up in acute stroke patients with normal perfusion CT and normal CT angiography. Neuroradiology 53(2):79–88, Epub 2010 Apr 27
Acknowledgments
The authors acknowledge the contribution of Sascha Prothmann and Annette Förschler, as well as of Michael Söderman and Staffan Holmin, who were involved in the endovascular treatment of the patients in Munich and Stockholm.
Conflict of interest
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dorn, F., Kuntze-Soderqvist, A., Popp, S. et al. Early venous drainage after successful endovascular recanalization in ischemic stroke — a predictor for final infarct volume?. Neuroradiology 54, 745–751 (2012). https://doi.org/10.1007/s00234-011-0966-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-011-0966-8