Abstract
Purpose
This study aimed to retrospectively analyze a series of patients with complex posterior circulation stenosis who underwent stent-assisted angioplasty to evaluate the feasibility of the procedure and summarize the experience with regard to complications.
Methods
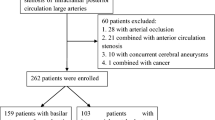
A total of 16 consecutive patients with 27 complex posterior circulation artery stenoses refractory to medical therapy were enrolled. Technical success rate, periprocedural complication, and long-term follow-up result were evaluated.
Results
The study population included 16 patients with 27 lesions. A total of 36 stents were successfully implanted. The technical success rate was 100%, and the overall periprocedural complication rate was 12.5% (2/16). During a median of 25.5 months of follow-up, three patients presented recurrent transient ischemic attacks, which were confirmed had restenosis more than 50% by control angiography or transcranial Doppler.
Conclusions
Stent-assisted angioplasty is a feasible treatment method for complex posterior circulation artery stenosis. However, it appears to be associated with a relatively high periprocedural complication rate. Therefore, strict periprocedural management to reduce mortality and morbidity is needed.



Similar content being viewed by others
References
The Warfarin-Aspirin Symptomatic Intracranial Disease (WASID) Study Group (1998) Prognosis of patients with symptomatic vertebral or basilar artery stenosis. Stroke 29:1389–1392
Qureshi AI, Ziai WC, Yahia AM et al (2003) Stroke-free survival and its determinants in patients with symptomatic vertebrobasilar stenosis: a multicenter study. Neurosurgery 52:1033–1039. doi:10.1227/01.NEU.0000057744.96295.9F
Mori T, Kazita K, Mori K (1999) Cerebral angioplasty and stenting for intracranial vertebral atherosclerotic stenosis. AJNR Am J Neuroradiol 20:787–789
Mori T, Kazita K, Chokyu K, Mima T, Mori K (2000) Short-term arteriographic and clinical outcome after cerebral angioplasty and stenting for intracranial vertebrobasilar and carotid atherosclerotic occlusive disease. AJNR Am J Neuroradiol 21:249–254
Gomez CR, Misra VK, Liu MW et al (2000) Elective stenting of symptomatic basilar artery stenosis. Stroke 31:95–99
SSYLVIA Study Investigators (2004) Stenting of symptomatic atherosclerotic lesions in the vertebral or intracranial arteries (SSYLVIA): study results. Stroke 35:1388–1392. doi:10.1161/01.STR.0000128708.86762.d6
Levy EI, Horowitz MB, Koebbe CJ et al (2001) Transluminal stent-assisted angioplasty of the intracranial vertebrobasilar system for medically refractory, posterior circulation ischemia: early results. Neurosurgery 48:1215–1221. doi:10.1097/00006123-200106000-00002
Levy EI, Hanel RA, Bendok BR et al (2002) Staged stent-assisted angioplasty for symptomatic intracranial vertebrobasilar artery stenosis. J Neurosurg 97:1294–1301
Levy EI, Turk AS, Albuquerque FC et al (2007) Wingspan in-stent restenosis and thrombosis: incidence, clinical presentation, and management. Neurosurgery 61:644–651
Chimowitz MI, Lynn MJ, Howlett-Smith H, Stern BJ (2005) Comparison of warfarin and aspirin for symptomatic intracranial arterial stenosis. N Engl J Med 352:1305–1316. doi:10.1056/NEJMoa043033
Thijs VN, Albers GW (2000) Symptomatic intracranial atherosclerosis: outcome of patients who fail antithrombotic therapy. Neurology 55:490–497
Mori T, Mori K, Fukuoka M et al (1997) Percutaneous transluminal cerebral angioplasty for total occlusion of middle cerebral arteries. Neuroradiology 39:71–74. doi:10.1007/s002340050370
Mori T, Mori K, Fukuoka M et al (1997) Percutaneous transluminal cerebral angioplasty: serial angiographic follow-up after successful dilatation. Neuroradiology 39:111–116. doi:10.1007/s002340050376
Coutts SB, Hill MD, Hu WY (2003) Hyperperfusion syndrome: toward a stricter definition. Neurosurgery 53:1053–1058. doi:10.1227/01.NEU.0000088738.80838.74
Marco TR, Laurent S, Charbel M et al (2006) Hyperperfusion syndrome after stenting for intracranial vertebral stenosis. Stroke 37:e12–e14
Yu W, Smith WS, Singh V et al (2005) Long-term outcome of endovascular stenting for symptomatic basilar artery stenosis. Neurology 64:1055–1057
Jiang WJ, Srivastava T, Gao F et al (2006) Perforator stroke after elective stenting of symptomatic intracranial stenosis. Neurology 66:1868–1872. doi:10.1212/01.wnl.0000219744.06992.bb
Leung TW, Mak H, Yu SCH et al (2007) Perforator stroke after elective stenting of symptomatic intracranial stenosis. Neurology 68:1237. doi:10.1212/01.wnl.0000261903.62909.0d
Kim DJ, Lee BH, Kim DI et al (2005) Stent-assisted angioplasty of symptomatic intracranial vertebrobasilar artery stenosis: feasibility and follow-up results. AJNR Am J Neuroradiol 26:1381–1388
Jiang WJ, Xu XT, Du B et al (2007) Long-term outcome of elective stenting for symptomatic intracranial vertebrobasilar stenosis. Neurology 68:856–858. doi:10.1212/01.wnl.0000256713.23864.be
Fiorella D, Chow MM, Anderson M et al (2007) A 7-year experience with balloon-mounted coronary stents for the treatment of symptomatic vertebrobasilar intracranial atheromatous disease. Neurosurgery 61:236–243. doi:10.1227/01.NEU.0000255521.42579.31
Kallmes DF, Do HM (2007) Wherefore wingspan? AJNR Am J Neuroradiol 28:997–998. doi:10.3174/ajnr.A0614
Turk AS, Ahmed A, Niemann DB et al (2007) Utilization of self-expanding stents in the treatment of intracranial atherosclerotic disease in the distal small cerebral vessels. Neuroradiology 49:659–663. doi:10.1007/s00234-007-0229-x
Gomez CR, Misra VK, Campbell MS et al (2000) Elective stenting of symptomatic middle cerebral artery stenosis. AJNR Am J Neuroradiol 21:971–973
Acknowledgement
This study was sponsored by the Beijing Medical Development and Research Fund.
Conflict of interest statement
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wang, B., Miao, Zr., Li, Gl. et al. Treatment of symptomatic complex posterior circulation cerebral artery stenosis with balloon-mounted stents: technique feasibility and outcome. Neuroradiology 51, 319–326 (2009). https://doi.org/10.1007/s00234-009-0503-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-009-0503-1