Abstract
Rationale and objectives
Major depressive disorder (MDD) is associated with an increased risk for cardiovascular disease (CVD). Apart from biological and life style factors, the use of antidepressants and their potentially adverse effects might contribute to the increased CVD risk. Therefore, we compared cardiovascular risk profiles between relatively young depressed patients without CVD with and without antidepressant medication and healthy participants.
Methods
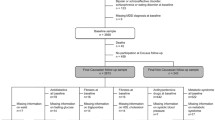
We investigated 44 depressed patients (with antidepressants N = 20 (13 women), mean age 43.2 years; without antidepressants N = 24 (15 women), mean age 40.0) and 41 healthy participants (matched for sex, age, education). As markers of CVD risk, blood pressure, body mass index (BMI), and plasma levels of fasting glucose, cholesterol, low density lipoprotein (LDL), high density lipoprotein (HDL), and high sensitivity C-reactive protein (h-CRP) were measured.
Results
We found significant differences between groups for BMI (p < .01), systolic (p = .02) and diastolic blood pressure (p < .01), and glucose (p < .001). Post hoc analyses indicated differences between both patient groups compared to the healthy control group, but not between patients groups. Further controlling for BMI diminished the effect of diagnosis on blood pressure; however, this was not the case for glucose level. There were no between-group differences in cholesterol, LDL, HDL, and h-CRP.
Conclusions
We found a clearly increased CVD risk in this group of rather young depressed patients. Importantly, there was no significant difference in CVD risk between patients with vs. without antidepressants. This suggests that major depression per se and not antidepressant medication is associated with increased CVD risk.


Similar content being viewed by others
References
Baumeister H, Hutter N, Bengel J (2011) Psychological and pharmacological interventions for depression in patients with coronary artery disease. Cochrane Database Syst Rev 9:CD008012. doi:10.1002/14651858.CD008012.pub3
Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J (1961) An inventory for measuring depression. Arch Gen Psychiatry 4:561–571
Bogers RP, Bemelmans WJ, Hoogenveen RT, Boshuizen HC, Woodward M, Knekt P, Shipley MJ (2007) Association of overweight with increased risk of coronary heart disease partly independent of blood pressure and cholesterol levels: a meta-analysis of 21 cohort studies including more than 300 000 persons. Arch Intern Med 167(16):1720–1728. doi:10.1001/archinte.167.16.1720
Bonnet F, Irving K, Terra JL, Nony P, Berthezene F, Moulin P (2005) Anxiety and depression are associated with unhealthy lifestyle in patients at risk of cardiovascular disease. Atherosclerosis 178(2):339–344
Cohen HW, Gibson G, Alderman MH (2000) Excess risk of myocardial infarction in patients treated with antidepressant medications: association with use of tricyclic agents. Am J Med 108(1):2–8
de Wit LM, Fokkema M, van Straten A, Lamers F, Cuijpers P, Penninx BW (2010) Depressive and anxiety disorders and the association with obesity, physical, and social activities. Depress Anxiety 27(11):1057–1065. doi:10.1002/da.20738
Fan H, Yu W, Zhang Q, Cao H, Li J, Wang J, Hu X (2014) Depression after heart failure and risk of cardiovascular and all-cause mortality: a meta-analysis. Prev Med 63:36–42. doi:10.1016/j.ypmed.2014.03.007
Frasure-Smith N, Lesperance F, Talajic M (1993) Depression following myocardial infarction. Impact on 6-month survival. JAMA 270(15):1819–1825
Glassman AH, O’Connor CM, Califf RM, Swedberg K, Schwartz P, Bigger JT Jr, McLvor M (2002) Sertraline treatment of major depression in patients with acute MI or unstable angina. Jama 288(6):701–709
Hamer M, Batty GD, Seldenrijk A, Kivimaki M (2011) Antidepressant medication use and future risk of cardiovascular disease: the Scottish Health Survey. Eur Heart J 32(4):437–442. doi:10.1093/eurheartj/ehq438
Hamilton M (1960) A rating scale for depression. J Neurol Neurosurg Psychiatry 23:56–62
Hare DL, Toukhsati SR, Johansson P, Jaarsma T (2014) Depression and cardiovascular disease: a clinical review. Eur Heart J 35(21):1365–1372. doi:10.1093/eurheartj/eht462
Ho JM, Gomes T, Straus SE, Austin PC, Mamdani M, Juurlink DN (2014) Adverse cardiac events in older patients receiving venlafaxine: a population-based study. J Clin Psychiatry 75(6):e552–e558. doi:10.4088/JCP.13m08508
Jiang W, Davidson JR (2005) Antidepressant therapy in patients with ischemic heart disease. Am Heart J 150(5):871–881. doi:10.1016/j.ahj.2005.01.041
Kaestner F, Hettich M, Peters M, Sibrowski W, Hetzel G, Ponath G, Rothermundt M (2005) Different activation patterns of proinflammatory cytokines in melancholic and non-melancholic major depression are associated with HPA axis activity. J Affect Disord 87(2–3):305–311. doi:10.1016/j.jad.2005.03.012
Karlovic D, Serretti A, Vrkic N, Martinac M, Marcinko D (2012) Serum concentrations of CRP, IL-6, TNF-alpha and cortisol in major depressive disorder with melancholic or atypical features. Psychiatry Res 198(1):74–80. doi:10.1016/j.psychres.2011.12.007
Kemp AH, Brunoni AR, Santos IS, Nunes MA, Dantas EM, Carvalho de Figueiredo R, Lotufo PA (2014) Effects of depression, anxiety, comorbidity, and antidepressants on resting-state heart rate and its variability: an ELSA-Brasil cohort baseline study. Am J Psychiatry. doi:10.1176/appi.ajp.2014.13121605
Lamers F, de Jonge P, Nolen WA, Smit JH, Zitman FG, Beekman AT, Penninx BW (2010) Identifying depressive subtypes in a large cohort study: results from the Netherlands Study of Depression and Anxiety (NESDA). J Clin Psychiatry 71(12):1582–1589. doi:10.4088/JCP.09m05398blu
Lamers F, Vogelzangs N, Merikangas KR, de Jonge P, Beekman AT, Penninx BW (2013) Evidence for a differential role of HPA-axis function, inflammation and metabolic syndrome in melancholic versus atypical depression. Mol Psychiatry 18(6):692–699. doi:10.1038/mp.2012.144
Lesperance F, Frasure-Smith N, Koszycki D, Laliberte MA, van Zyl LT, Baker B, Guertin MC (2007) Effects of citalopram and interpersonal psychotherapy on depression in patients with coronary artery disease: the Canadian Cardiac Randomized Evaluation of Antidepressant and Psychotherapy Efficacy (CREATE) trial. JAMA 297(4):367–379
Licht CM, de Geus EJ, Seldenrijk A, van Hout HP, Zitman FG, van Dyck R, Penninx BW (2009) Depression is associated with decreased blood pressure, but antidepressant use increases the risk for hypertension. Hypertension 53(4):631–638. doi:10.1161/hypertensionaha.108.126698
Licht CM, de Geus EJ, van Dyck R, Penninx BW (2010) Longitudinal evidence for unfavorable effects of antidepressants on heart rate variability. Biol Psychiatry 68(9):861–868
Licht CM, Naarding P, Penninx BW, van der Mast RC, de Geus EJ, Comijs H (2015) The association between depressive disorder and cardiac autonomic control in adults 60 years and older. Psychosom Med 77(3):279–291. doi:10.1097/psy.0000000000000165
Lippi G, Montagnana M, Favaloro EJ, Franchini M (2009) Mental depression and cardiovascular disease: a multifaceted, bidirectional association. Semin Thromb Hemost 35(3):325–336
Luppino FS, van Reedt Dortland AK, Wardenaar KJ, Bouvy PF, Giltay EJ, Zitman FG, Penninx BW (2011) Symptom dimensions of depression and anxiety and the metabolic syndrome. Psychosom Med 73(3):257–264. doi:10.1097/PSY.0b013e31820a59c0
Meng L, Chen D, Yang Y, Zheng Y, Hui R (2012) Depression increases the risk of hypertension incidence: a meta-analysis of prospective cohort studies. J Hypertens 30(5):842–851. doi:10.1097/HJH.0b013e32835080b7
Mezuk B, Eaton WW, Albrecht S, Golden SH (2008) Depression and type 2 diabetes over the lifespan: a meta-analysis. Diabetes Care 31(12):2383–2390. doi:10.2337/dc08-0985
Montgomery SA, Asberg M (1979) A new depression scale designed to be sensitive to change. Br J Psychiatry 134:382–389
Mottillo S, Filion KB, Genest J, Joseph L, Pilote L, Poirier P, Eisenberg MJ (2010) The metabolic syndrome and cardiovascular risk a systematic review and meta-analysis. J Am Coll Cardiol 56(14):1113–1132. doi:10.1016/j.jacc.2010.05.034
Nicholson A, Kuper H, Hemingway H (2006) Depression as an aetiologic and prognostic factor in coronary heart disease: a meta-analysis of 6362 events among 146 538 participants in 54 observational studies. Eur Heart J 27(23):2763–2774
O’Connor CM, Jiang W, Kuchibhatla M, Silva SG, Cuffe MS, Callwood DD, Krishnan R (2010) Safety and efficacy of sertraline for depression in patients with heart failure: results of the SADHART-CHF (Sertraline Against Depression and Heart Disease in Chronic Heart Failure) trial. J Am Coll Cardiol 56(9):692–699. doi:10.1016/j.jacc.2010.03.068
O’Donnell MJ, Xavier D, Liu L, Zhang H, Chin SL, Rao-Melacini P, Yusuf S (2010) Risk factors for ischaemic and intracerebral haemorrhagic stroke in 22 countries (the INTERSTROKE study): a case–control study. Lancet 376(9735):112–123. doi:10.1016/s0140-6736(10)60834-3
Pan A, Sun Q, Okereke OI, Rexrode KM, Hu FB (2011) Depression and risk of stroke morbidity and mortality: a meta-analysis and systematic review. JAMA 306(11):1241–1249. doi:10.1001/jama.2011.1282
Penninx BW, Milaneschi Y, Lamers F, Vogelzangs N (2013) Understanding the somatic consequences of depression: biological mechanisms and the role of depression symptom profile. BMC Med 11:129. doi:10.1186/1741-7015-11-129
Pratt LA, Ford DE, Crum RM, Armenian HK, Gallo JJ, Eaton WW (1996) Depression, psychotropic medication, and risk of myocardial infarction. Prospective data from the Baltimore ECA follow-up. Circulation 94(12):3123–3129
Rahman I, Humphreys K, Bennet AM, Ingelsson E, Pedersen NL, Magnusson PK (2013) Clinical depression, antidepressant use and risk of future cardiovascular disease. Eur J Epidemiol 28(7):589–595. doi:10.1007/s10654-013-9821-z
Rieckmann N, Kronish IM, Shapiro PA, Whang W, Davidson KW (2013) Serotonin reuptake inhibitor use, depression, and long-term outcomes after an acute coronary syndrome: a prospective cohort study. JAMA Intern Med 173(12):1150–1151. doi:10.1001/jamainternmed.2013.910
Schramm PJ, Poland RE, Rao U (2014) Bupropion response on sleep quality in patients with depression: implications for increased cardiovascular disease risk. Eur Neuropsychopharmacol 24(2):207–214. doi:10.1016/j.euroneuro.2013.09.007
Seldenrijk A, Vogelzangs N, Batelaan NM, Wieman I, van Schaik DJ, Penninx BJ (2015) Depression, anxiety and 6-year risk of cardiovascular disease. J Psychosom Res 78(2):123–129. doi:10.1016/j.jpsychores.2014.10.007
Seppala J, Vanhala M, Kautiainen H, Eriksson J, Kampman O, Mantyselka P, Koponen H (2012) Prevalence of metabolic syndrome in subjects with melancholic and non-melancholic depressive symptoms. A Finnish population-based study. J Affect Disord 136(3):543–549. doi:10.1016/j.jad.2011.10.032
Serodio KJ, Ardern CI, Rotondi MA, Kuk JL (2014) Tricyclic and SSRI usage influences the association between BMI and health risk factors. Clin Obes 4(6):296–302. doi:10.1111/cob.12067
Smoller JW, Allison M, Cochrane BB, Curb JD, Perlis RH, Robinson JG, Wassertheil-Smoller S (2009) Antidepressant use and risk of incident cardiovascular morbidity and mortality among postmenopausal women in the Women’s Health Initiative study. Arch Intern Med 169(22):2128–2139. doi:10.1001/archinternmed.2009.436
van Reedt Dortland AK, Giltay EJ, van Veen T, Zitman FG, Penninx BW (2010) Metabolic syndrome abnormalities are associated with severity of anxiety and depression and with tricyclic antidepressant use. Acta Psychiatr Scand 122(1):30–39. doi:10.1111/j.1600-0447.2010.01565.x
Weeke P, Jensen A, Folke F, Gislason GH, Olesen JB, Andersson C, Torp-Pedersen C (2012) Antidepressant use and risk of out-of-hospital cardiac arrest: a nationwide case-time-control study. Clin Pharmacol Ther 92(1):72–79. doi:10.1038/clpt.2011.368
Whooley MA, Wong JM (2013) Depression and cardiovascular disorders. Annu Rev Clin Psychol 9:327–354. doi:10.1146/annurev-clinpsy-050212-185526
Whooley MA, de Jonge P, Vittinghoff E, Otte C, Moos R, Carney RM, Browner WS (2008) Depressive symptoms, health behaviors, and risk of cardiovascular events in patients with coronary heart disease. JAMA 300(20):2379–2388. doi:10.1001/jama.2008.711
Xiong GL, Jiang W, Clare R, Shaw LK, Smith PK, Mahaffey KW, Newby LK (2006) Prognosis of patients taking selective serotonin reuptake inhibitors before coronary artery bypass grafting. Am J Cardiol 98(1):42–47. doi:10.1016/j.amjcard.2006.01.051
Yoon HK, Kim YK, Lee HJ, Kwon DY, Kim L (2012) Role of cytokines in atypical depression. Nord J Psychiatry 66(3):183–188. doi:10.3109/08039488.2011.611894
Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, Lanas F, Lisheng L (2004) Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case–control study. Lancet 364(9438):937–952. doi:10.1016/s0140-6736(04)17018-9
Ziegelstein RC, Fauerbach JA, Stevens SS, Romanelli J, Richter DP, Bush DE (2000) Patients with depression are less likely to follow recommendations to reduce cardiac risk during recovery from a myocardial infarction. Arch Intern Med 160(12):1818–1823
Zimmermann-Viehoff F, Kuehl LK, Danker-Hopfe H, Whooley MA, Otte C (2014) Antidepressants, autonomic function and mortality in patients with coronary heart disease: data from the Heart and Soul Study. Psychol Med 44(14):2975–2984. doi:10.1017/s003329171400066x
Acknowledgments
The authors received no funding. Dr. LK, Dr. CM, Dr. KH, Dr. LD, Dr. KW, and Dr. CS report no conflict of interest. Dr. CO has received honoria fees for lectures from Lundbeck and Servier.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was carried out in accordance with the latest version of the Declaration of Helsinki and approved by the responsible local ethics committee (ethics committee of the Medical Association of Hamburg). Informed consent of the participants was obtained after the nature of the procedures had been fully explained.
Additional information
Linn K. Kuehl and Christoph Muhtz contributed equally to this work.
Rights and permissions
About this article
Cite this article
Kuehl, L.K., Muhtz, C., Hinkelmann, K. et al. Association between major depression and cardiovascular risk: the role of antidepressant medication. Psychopharmacology 233, 3289–3295 (2016). https://doi.org/10.1007/s00213-016-4361-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-016-4361-3