Abstract
Summary
We conducted a Mendelian randomization analysis to assess the effect of serum uric acid on bone-related outcomes using a weighted urate transporter genetic risk score as the instrumental variable. The results showed no significance. Our study identified no evidence of a causal role between uric acid and bone-related outcomes.
Introduction
Observational studies have associated elevated levels of serum uric acid (SUA) with increasing bone mineral density (BMD) and a lowered prevalence of osteoporotic fractures (OFs) in postmenopausal women and elderly men. However, due to unmeasured confounding variables, these observational studies have not provided insight into the causal relationship between SUA and bone-related outcomes. Our aim was to evaluate the effect of SUA on bone-related outcomes using Mendelian randomization.
Methods
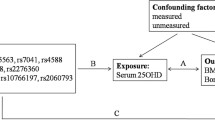
We recruited 1322 Chinese Han individuals (214 elderly men and 1108 postmenopausal women) from the Shanghai area in China. Mendelian randomization using a two-stage least-squares regression method was conducted with SUA as the exposure variable, a weighted urate transporter genetic risk score as the instrumental variable, and all-site BMD, bone turnover markers, and levels of 25-hydroxyvitamin D3 [25(OH)D], serum calcium (Ca), serum phosphorus (P), and parathyroid hormone (PTH) as outcome variables.
Results
Strong associations between SUA and bone-related outcomes were observed in an ordinary observational analysis (lumbar spine: beta = 0.122, p < 0.0001; hip: beta = 0.104, p < 0.0001; femoral neck: beta = 0.108, p < 0.0001). However, the Mendelian randomization analysis showed no evidence for a causal association of SUA with BMD (lumbar spine: beta = 0.385, p = 0.257; hip: beta = 0.191, p = 0.499; femoral neck: beta = 0.194, p = 0.533). Similar results were found between SUA and other bone-related phenotypes.
Conclusions
Our study identified no evidence of a causal role between SUA and bone-related outcomes, although strong associations in an observational analysis were observed in a population of postmenopausal women and elderly men.

Similar content being viewed by others
References
Bai XC, Lu D, Bai J, Zheng H, Ke ZY, Li XM, Luo SQ (2004) Oxidative stress inhibits osteoblastic differentiation of bone cells by ERK and NF-kappaB. Biochem Biophys Res Commun 314:197–207
Ha H, Kwak HB, Lee SW, Jin HM, Kim HM, Kim HH, Lee ZH (2004) Reactive oxygen species mediate RANK signaling in osteoclasts. Exp Cell Res 301:119–127
Ostman B, Michaelsson K, Helmersson J, Byberg L, Gedeborg R, Melhus H, Basu S (2009) Oxidative stress and bone mineral density in elderly men: antioxidant activity of alpha-tocopherol. Free Radic Biol Med 47:668–673
Bruce N, Ames RC, Elizabeth SH, Paul HC (1981) Uric acid provides an antioxidant defense in humans against oxidant- and radical-caused aging and cancer: a hypothesis. Proc Natl Acad Sci U S A 78:6858–6862
Hershfield MS, Roberts LJ, Ganson NJ, Kelly SJ, Santisteban I, Scarlett E, Jaggers D, Sundy JS (2010) Treating gout with pegloticase, a PEGylated urate oxidase, provides insight into the importance of uric acid as an antioxidant in vivo. Proc Natl Acad Sci U S A 107:14351–14356
Nabipour I, Sambrook PN, Blyth FM et al (2011) Serum uric acid is associated with bone health in older men: a cross-sectional population-based study. J Bone Miner Res 26:955–964
Ahn SH, Lee SH, Kim BJ et al (2013) Higher serum uric acid is associated with higher bone mass, lower bone turnover, and lower prevalence of vertebral fracture in healthy postmenopausal women. Osteoporos Int 24:2961–2970
Makovey J, Macara M, Chen JS, Hayward CS, March L, Seibel MJ, Sambrook PN (2013) Serum uric acid plays a protective role for bone loss in peri- and postmenopausal women: a longitudinal study. Bone 52:400–406
Ishii S, Miyao M, Mizuno Y, Tanaka-Ishikawa M, Akishita M, Ouchi Y (2014) Association between serum uric acid and lumbar spine bone mineral density in peri- and postmenopausal Japanese women. Osteoporos Int 25:1099–1105
Lane NE, Parimi N, Lui L-Y, Wise BL, Yao W, Lay Y-AE, Cawthon PM, Orwoll E (2014) Association of serum uric acid and incident nonspine fractures in elderly men: the Osteoporotic Fractures in Men (MrOS) study. J Bone Miner Res 29:1701–1707
Lee YJ, Hong JY, Kim SC, Joo JK, Na YJ, Lee KS (2015) The association between oxidative stress and bone mineral density according to menopausal status of Korean women. Obstet Gynecol Sci 58:46–52
Kim BJ, Baek S, Ahn SH et al (2014) Higher serum uric acid as a protective factor against incident osteoporotic fractures in Korean men: a longitudinal study using the National Claim Registry. Osteoporos Int 25:1837–1844
Zhang D, Bobulescu IA, Maalouf NM et al (2015) Relationship between serum uric Acid and bone mineral density in the general population and in rats with experimental hyperuricemia. J Bone Miner Res 30:992–999
Mehta T, Buzkova P, Sarnak MJ, Chonchol M, Cauley JA, Wallace E, Fink HA, Robbins J, Jalal D (2015) Serum urate levels and the risk of hip fractures: data from the Cardiovascular Health Study. Metabolism 64:438–446
Palmer TM, Lawlor DA, Harbord RM, Sheehan NA, Tobias JH, Timpson NJ, Davey Smith G, Sterne JA (2012) Using multiple genetic variants as instrumental variables for modifiable risk factors. Stat Methods Med Res 21:223–242
Kottgen A, Albrecht E, Teumer A et al (2013) Genome-wide association analyses identify 18 new loci associated with serum urate concentrations. Nat Genet 45:145–154
Sulem P, Gudbjartsson DF, Walters GB et al (2011) Identification of low-frequency variants associated with gout and serum uric acid levels. Nat Genet 43:1127–1130
Yang B, Mo Z, Wu C et al (2014) A genome-wide association study identifies common variants influencing serum uric acid concentrations in a Chinese population. BMC Med Genomics 7:10
Pfister R, Barnes D, Luben R, Forouhi NG, Bochud M, Khaw KT, Wareham NJ, Langenberg C (2011) No evidence for a causal link between uric acid and type 2 diabetes: a Mendelian randomisation approach. Diabetologia 54:2561–2569
Hughes K, Flynn T, de Zoysa J, Dalbeth N, Merriman TR (2014) Mendelian randomization analysis associates increased serum urate, due to genetic variation in uric acid transporters, with improved renal function. Kidney Int 85:344–351
Rasheed H, Hughes K, Flynn TJ, Merriman TR (2014) Mendelian randomization provides no evidence for a causal role of serum urate in increasing serum triglyceride levels. Circ Cardiovasc Genet 7:830–837
Simon KC, Eberly S, Gao X et al (2014) Mendelian randomization of serum urate and Parkinson disease progression. Ann Neurol 76:862–868
Lu HK, Zhang Z, Ke YH, He JW, Fu WZ, Zhang CQ, Zhang ZL (2012) High prevalence of vitamin D insufficiency in China: relationship with the levels of parathyroid hormone and markers of bone turnover. PLoS One 7:e47264
Zhang H, He JW, Gao G et al (2010) Polymorphisms in the HOXD4 gene are not associated with peak bone mineral density in Chinese nuclear families. Acta Pharmacol Sin 31:977–983
Kolz M, Johnson T, Sanna S et al (2009) Meta-analysis of 28,141 individuals identifies common variants within five new loci that influence uric acid concentrations. PLoS Genet 5, e1000504
Son CN, Bang SY, Cho SK, Sung YK, Kim TH, Bae SC, Jun JB (2014) The frequency of single nucleotide polymorphisms and their association with uric acid concentration based on data from genome-wide association studies in the Korean population. Rheumatol Int 34:777–783
Purcell S, Neale B, Todd-Brown K et al (2007) PLINK: a tool set for whole-genome association and population-based linkage analyses. Am J Hum Genet 81:559–575
Glickman ME, Rao SR, Schultz MR (2014) False discovery rate control is a recommended alternative to Bonferroni-type adjustments in health studies. J Clin Epidemiol 67:850–857
Davies NM, von Hinke Kessler Scholder S, Farbmacher H, Burgess S, Windmeijer F, Smith GD (2015) The many weak instruments problem and Mendelian randomization. Stat Med 34:454–468
Ja H (1978) Specification tests in econometrics. Econometrica 46:1251–1271
Burgess S, Daniel RM, Butterworth AS, Thompson SG, E-IC (2015) Network Mendelian randomization: using genetic variants as instrumental variables to investigate mediation in causal pathways. Int J Epidemiol 44:484–495
Freeman G, Cowling BJ, Schooling CM (2013) Power and sample size calculations for Mendelian randomization studies using one genetic instrument. Int J Epidemiol 42:1157–1163
Dalbeth N, Topless R, Flynn T, Cadzow M, Bolland MJ, Merriman TR (2015) Mendelian randomisation analysis to examine for a causal effect of urate on bone mineral density. J Bone Miner Res 30:985–991
Sritara C, Ongphiphadhanakul B, Chailurkit L, Yamwong S, Ratanachaiwong W, Sritara P (2013) Serum uric acid levels in relation to bone-related phenotypes in men and women. J Clin Densitom 16:336–340
Bonora E, Targher G, Zenere MB et al (1996) Relationship of uric acid concentration to cardiovascular risk factors in young men. Role of obesity and central fat distribution. The Verona Young Men Atherosclerosis Risk Factors Study. Int J Obes Relat Metab Disord 20:975–980
McAdams DeMarco MA, Maynard JW, Baer AN, Gelber AC, Young JH, Alonso A, Coresh J (2012) Diuretic use, increased serum urate levels, and risk of incident gout in a population-based study of adults with hypertension: the atherosclerosis risk in communities cohort study. Arthritis Rheum 64:121–129
Sumino H, Ichikawa S, Kanda T, Nakamura T, Sakamaki T (1999) Reduction of serum uric acid by hormone replacement therapy in postmenopausal women with hyperuricaemia. Lancet 354:650
Hui JY, Choi JW, Mount DB, Zhu Y, Zhang Y, Choi HK (2012) The independent association between parathyroid hormone levels and hyperuricemia: a national population study. Arthritis Res Ther 14:R56
Takahashi S, Yamamoto T, Moriwaki Y, Tsutsumi Z, Yamakita J, Higashino K (1998) Decreased serum concentrations of 1,25(OH)2-vitamin D3 in patients with gout. Metabolism 47:336–338
Chen W, Roncal-Jimenez C, Lanaspa M, Gerard S, Chonchol M, Johnson RJ, Jalal D (2014) Uric acid suppresses 1 alpha hydroxylase in vitro and in vivo. Metabolism 63:150–160
Acknowledgments
We thank all participants for their cooperation as well as Yi Wang, PhD (Fudan University, Shanghai China) for statistical support. This study was supported by the National Basic Research Program of China (2014CB942903), the National Natural Science Foundation of China (81170803 and 81370978), the Frontier Technology Joint Research Program of the Shanghai Municipal Hospitals (SHDC 12013115), the Shanghai Leading Talents Award (051), the Science and Technology Commission of Chongqing Municipality (CSTC2013jcyjC00009), the Science and Technology Commission of Shanghai Municipality (14JC1405000), and the Ningbo Science and Technology Plan Projects (2015C50031).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflicts of interest
None.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplemental Table 1
Analysis of association of weighted UA transporter genetic score with tested confounders by linear regression (DOC 31 kb)
Supplemental Table 2
Mendelian randomization analysis conducted in female groups on BMD and SUA levels (DOC 35 kb)
Rights and permissions
About this article
Cite this article
Xiong, A., Yao, Q., He, J. et al. No causal effect of serum urate on bone-related outcomes among a population of postmenopausal women and elderly men of Chinese Han ethnicity—a Mendelian randomization study. Osteoporos Int 27, 1031–1039 (2016). https://doi.org/10.1007/s00198-015-3341-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-015-3341-5