Abstract
Introduction and hypothesis
Mid-urethral tape procedures brought a paradigm shift in surgery for stress incontinence; little research into the development and maintenance of surgical competence for the procedure exists. The hypothesis behind this study is that the “learning curve” for retropubic mid-urethral sling procedures, judged by the surrogate of bladder perforation, is longer than previously thought.
Methods
This was a retrospective single-centre database and case note review of retropubic mid-urethral tape procedures. Unadjusted rates of bladder perforation, operating time, postoperative voiding difficulty, tape extrusion, and patient reported outcome were calculated; progress was evaluated using the cumulative sum method. Outcomes were assessed for 1 consultant, 2 subspecialty trainees (fellows), 7 advanced training skills module (ATSM) trainees (senior residents) and 6 core specialty trainees (residents) in years 4–7 of training.
Results
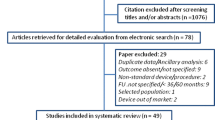
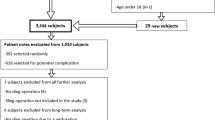
A total of 1,568 women were identified as having mid-urethral tape procedures; 568 (36 %) had additional procedures concurrently; 259 (20 %) were secondary procedures. The overall perforation rate for individual surgeons varied between 0 and 31 % and averaged 10.3 % amongst the core and ATSM trainees (a mean of 11 procedures), 4.5 % amongst the subspecialty trainees (a mean of 66 procedures) and 1.3 % for the consultant (1,284 procedures). The number of perforations for individual surgeons peaked at between 10 and 30 procedures undertaken. The number of cases performed to reach a target level of ≤5 % perforations varied between 20 and 80.
Conclusions
Whilst seductively simple in concept, mid-urethral tape procedures are not without risk; their inherently “blind” nature makes them difficult to teach. The “learning curve” to independent practice may be longer than previously considered.



Similar content being viewed by others
References
Medicines and Healthcare Products Regulatory Agency (2014) A summary of the evidence on the benefits and risks of vaginal mesh implants. Medicines and Healthcare Products Regulatory Agency, London
Keogh B, Calderwood C, Richmond D, Monga A, Joyce A, Morley R (2013) Letter from Prof Sir Bruce Keogh to Medical Directors of NHS and Foundation Trusts re: The surgical management of urinary incontinence and pelvic organ prolapse
Keel A (2014) Letter from Acting CMO Scotland to Chairs, CEO, Medical Directors NHS Boards re: Transvaginal mesh implants
U.S. Food and Drug Administration. Considerations about surgical mesh for SUI (2013). Available from: http://www.fda.gov/MedicalDevices/ProductsandMedicalProcedures/ImplantsandProsthetics/UroGynSurgicalMesh/ucm345219.htm. Accessed 13 May 2015
National Institute for Health & Care Excellence (2013) Urinary incontinence—the management of urinary incontinence in women. CG171. National Institute for Health & Care Excellence, London
Darzi A, Mackay S (2001) Assessment of surgical competence. Qual Health Care 10 [Suppl 2]:ii64–ii69
Kuuva N, Nilsson CG (2002) A nationwide analysis of complications associated with the tension-free vaginal tape (TVT) procedure. Acta Obstet Gynecol Scand 81(1):72–77
Groutz A, Gordon D, Wolman I, Jaffa AJ, David MP, Lessing JB (2002) Tension-free vaginal tape for stress urinary incontinence: is there a learning curve? Neurourol Urodyn 21(5):470–472
Gold RS, Groutz A, Pauzner D, Lessing J, Gordon D (2007) Bladder perforation during tension-free vaginal tape surgery: does it matter? J Reprod Med 52(7):616–618
Ito H, Yamanaka H, Hagiwara M, Furuuchi T, Matsumoto K, Kanai K et al (2011) Efficacy of tension-free vaginal tape compared with transobturator tape in the treatment of stress urinary incontinence in women: analysis of learning curve, perioperative changes of voiding function. BMC Urol 11:13
RCOG (2011) Urogynaecology and vaginal surgery ATSM. Available from: http://www.rcog.org.uk/globalassests/documents/careers-and-training/atsms/atsm_urogynaecologyvaginalsurgery_curriculum.pdf
Maguire T, Mayne CJ, Terry T, Tincello DG (2013) Analysis of the surgical learning curve using the cumulative sum (CUSUM) method. Neurourol Urodyn 32(7):964–967
Hilton P (2012) Urogenital fistula in the UK—a personal case series managed over 25 years.(Includes details of unit surgical database as supporting information). Available from: http://onlinelibrary.wiley.com/store/10.1111/j.1464-410X.2011.10630.x/asset/supinfo/BJU_10630_sm_FigS1.pdf?v=1&s=7dd3c78f7a6d36b202e173aaf0d606458e478b17
Dmochowski RR, Athanasiou S, Reid FM, Kraus S, Nitti V, Gomelsky A et al (2013) Surgery for urinary incontinence in women. In: Abrams P, Cardozo LD, Khoury S, Wein A (eds) Incontinence—ICUD 4th International Consultation on Incontinence, 4th edn. EAU Publications, Geneva, pp 1307–1375
Ogah J, Cody JD, Rogerson L (2009) Minimally invasive synthetic suburethral sling operations for stress urinary incontinence in women. Cochrane Database Syst Rev (4):CD006375
Amid PK (1997) Classification of biomaterials and their related complications in abdominal wall hernia surgery. Hernia 1(1):15–21
Hospital Episode Statistics [database on the Internet]. Department of Health (2015). Available from: http://www.hscic.gov.uk/hes. Accessed 11 May 2015
Ward KL, Hilton P (2002) Prospective multicentre randomised trial of tension-free vaginal tape and colposuspension as primary treatment for stress incontinence. BMJ 325:67–70
Hilton P, Ward K (2002) Tension-free vaginal tape—is there a learning curve? BMJ 325:67 (letter)
Hilton P (2002) Trials of surgery for stress incontinence—thoughts on the “Humpty Dumpty principle”. BJOG 109:1081–1088
Delorme E, Droupy S, de Tayrac R, Delmas V (2004) Transobturator tape (Uratape): a new minimally-invasive procedure to treat female urinary incontinence. Eur Urol 45(2):203–207
Gorlero F, Lijoi D, Glorio M, Mistrangelo E, Nicoletti A, Ferrero S et al (2008) A new technique for surgical treatment of stress urinary incontinence: the TVT-secur. Minerva Ginecol 60(6):459–468
Martan A, Svabik K, Masata J, Koleska T, El-Haddad R, Pavlikova M (2009) Initial experience with a short, tension-free vaginal tape (the tension-free vaginal tape secur system). Eur J Obstet Gynecol Reprod Biol 143(2):121–125
Bernasconi F, Napolitano V, Natale F, Leone V, Lijoi D, Cervigni M (2011) TVT SECUR System: final results of a prospective, observational, multicentric study. Int Urogynecol J 23(1):93–98
Ulmsten U, Henriksson L, Johnson P, Varhos G (1996) An ambulatory surgical procedure under local anesthesia for treatment of female urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 7(2):81–86
Conflicts of interest
PH has no current financial interests. Chief investigator for multi-center randomized trial of TVT TM vs. colposuspension funded by Gynecare 1998-2003.
KR has no conflicts of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hilton, P., Rose, K. The “learning curve” for retropubic mid-urethral sling procedures: a retrospective cohort study. Int Urogynecol J 27, 565–570 (2016). https://doi.org/10.1007/s00192-015-2853-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-015-2853-z