Abstract
Introduction and hypothesis
Cervical cancer complicated by complete uterine prolapse is a rare clinical entity and uniform management recommendations have yet to be determined. The aim of the current review was to examine the effects of management patterns on survival outcomes in cervical cancer patients with complete uterine prolapse.
Methods
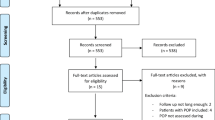
A systematic review of the literature was conducted using three public search engines. This included case reports with detailed descriptions of tumor characteristics, cancer management, and survival outcomes. Treatment patterns and tumor characteristics were correlated to survival outcomes.
Results
There were 78 patients with cervical cancer with complete uterine prolapse. Their mean age was 63.7 years. The median duration of prolapse was 147.9 months and 22.2 % of the patients experienced persistent/recurrent prolapse after cancer treatment. The mean tumor size was 8.9 cm and squamous cell carcinoma (83.9 %) was the most common histologic type. The majority of patients (56.2 %) had stage I cancer. Tumor characteristics were similar across the treatment patterns. Survival outcomes were more favorable with surgery-based treatment (48 patients) than with radiation-based treatment (30 patients): 5-year recurrence-free survival rate 72.0 % vs. 62.9 % (p = 0.057), and 5-year disease-specific overall survival rate 77.0 % vs. 68.2 % (p = 0.017). After controlling for age and stage, surgery-based therapy remained an independent prognostic factor for better disease-specific overall survival outcome (hazard ratio 0.32, 95 % confidence interval 0.11 – 0.94, adjusted p = 0.039).
Conclusions
Although limited in study size, our results at least suggest that surgery-based treatment may have a positive effect on survival outcome in cervical cancer patients with complete uterine prolapse.


Similar content being viewed by others
References
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D (2011) Global cancer statistics. CA Cancer J Clin 61:69–90
Maher C, Feiner B, Baessler K, Schmid C (2013) Surgical management of pelvic organ prolapse in women. Cochrane Database Syst Rev 4, CD004014
Richter HE, Varner ER (2007) Pelvic organ prolapse. In: Berek JS (ed) Berek and Novak's gynecology, vol 24. Lippincott Williams and Wilkins, Philadelphia, pp 897–934
Swift S, Woodman P, O'Boyle A, Kahn M, Valley M, Bland D et al (2005) Pelvic Organ Support Study (POSST): the distribution, clinical definition, and epidemiologic condition of pelvic organ support defects. Am J Obstet Gynecol 192:795–806
Edwards EA, Beebe RA (1950) Carcinoma of the cervix in association with procidentia. Q Bull Northwest Univ Med Sch 24:12
Mehboob R, Ahmad N (2002) Unexpected pathology at vaginal hysterectomy for genital prolapse. Pak J Med Res 41:1–5
Loizzi V, Cormio G, Selvaggi L, Carriero C, Putignano G (2010) Locally advanced cervical cancer associated with complete uterine prolapse. Eur J Cancer Care (Engl) 19:548–550
da Silva BB, da Costa AR, Filho CP, Melo JA (2002) Carcinoma of the cervix in association with uterine prolapse. Gynecol Oncol 84:349–350
Cabrera S, Franco-Camps S, Garcia A, Verges R, Diaz-Feijoo B, Perez-Benavente MA et al (2010) Total laparoscopic radical hysterectomy for cervical cancer in prolapsed uterus. Arch Gynecol Obstet 282:63–67
de Lima OA (1952) Cervical cancer and prolapse of the uterus. Obstet Gynecol Surv 7:849–850
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283:2008–2012
Bump RC, Mattiasson A, Bo K, Brubaker LP, DeLancey JO et al (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175:10–17
Beecham CT (1980) Classification of vaginal relaxation. Am J Obstet Gynecol 136:957–958
Baden WF, Walker TA (1972) Genesis of the vaginal profile: a correlated classification of vaginal relaxation. Clin Obstet Gynecol 15:1048–1054
Chen GD, Ng CS (2007) Updated definition of female pelvic organ prolapse. Incont Pelvic Floor Dysfunct 1:121–124
Ashton DL (1948) Carcinoma of the cervix complicating procidentia uteri. Am J Obstet Gynecol 55:299–302
Cabaniss CM, Crocker CL (1963) Carcinoma of the prolapsed cervical stump. Report of a case. Obstet Gynecol 22:606–9
Calame RJ, Perticucci S, de Fazio L (1970) Multiple primary carcinoma of the uterus: a review. Obstet Gynecol Surv 25:191–206
Chambers CB (1975) Uterine prolapse with incarceration. Am J Obstet Gynecol 122:459–462
Dane B, Dane C, Erginbas M, Baran S, Cetin A (2009) Verrucous carcinoma of the cervix in a case with uterine prolapse. Ann Diagn Pathol 13:344–346
Daw E (1972) Carcinoma of cervix in association with procidentia. Br J Clin Pract 26:197–200
Diaz-Bazan N (1964) Cervical carcinoma with procidentia in El Salvador: report of 10 cases with review of the literature. Obstet Gynecol 23:281–288
Guthrie D, Bache W (1932) The Infrequency of carcinoma of the cervix with complete procidentia. Ann Surg 96:796–800
Hesselberg E (1963) Cancer of the cervix associated with procidentia. S Afr Med J 37:589–592
Kistner RW (1957) Cervical carcinoma complicating procidentia; report of a case. Obstet Gynecol 10:482–6
Kriplani A, Relan S, Kumar L, Biswal BM, Rath GK (1995) Incarcerated procidentia: a rare complication of carcinoma cervix. Aust N Z J Obstet Gynaecol 35:463–464
Reimer D, Sztankay A, Steppan I, Abfalter E, Lunzer H, Marth C et al (2008) Cervical cancer associated with genital prolapse – a brief review of the literature and long-term results of successful treatment with radiochemotherapy and surgery in a very frail patient. Eur J Gynaecol Oncol 29:272–275
Rocker I (1958) Malignant changes in procidentia; the incidence during the years 1949-54 at Addenbrooke's Hospital, Cambridge. J Obstet Gynaecol Br Emp 65:89–91
Sholes DM Jr (1959) Carcinoma of the cervix and uterine prolapse. Obstet Gynecol 13:223–225
Stone BH, Mansell H (1955) Procidentia and cervical cancer. Obstet Gynecol 5:198–200
Todd TF (1937) Two cases of carcinoma of the cervix complicating procidentia uteri. Proc R Soc Med (Section of Obstetrics and Gynaecology) 30:1343–1344
Wong WS, Ng CS, Lee CK (1990) Verrucous carcinoma of the cervix. Arch Gynecol Obstet 247:47–51
Graham JB, Sotto LSJ, Paloucek FP (1962) Carcinoma of the cervix, vol 12. WB Saunders Company, Philadelphia, pp 231–239
Du XL, Tao J, Sheng XG, Lu CH, Yu H, Wang C et al (2012) Intensity-modulated radiation therapy for advanced cervical cancer: a comparison of dosimetric and clinical outcomes with conventional radiotherapy. Gynecol Oncol 125:151–7
Quinn MA, Benedet JL, Odicino F, Maisonneuve P, Beller U, Creasman WT et al (2006) Carcinoma of the cervix uteri. FIGO 26th Annual Report on the Results of Treatment in Gynecological Cancer. Int J Gynaecol Obstet 95 (Suppl 1):S43–S103
Harvey RA, Ritchie RN (1943) Carcinoma of the cervix complicated by complete procidentia: radiation therapy. Radiology 41:48–51
Way S (1958) Perineal anterior exenteration. Br J Obstet Gynaecol 65:24–27
Acknowledgments
The authors thank Drs. Katherine E. Tierney, MD, Kodama Michiko, MD, PhD, and Mikio Mikami, MD, PhD, for scientific input and technical support for this study.
Conflicts of interest
None.
Funding support
None.
Authors’ contributions
K. Matsuo: study concept, data collection and analysis, manuscript writing
M.E. Fullerton: data collection, manuscript writing
A. Moeini: data interpretation, manuscript writing
All authors significantly contributed to the study and approved the final version of manuscript.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 222 kb)
Rights and permissions
About this article
Cite this article
Matsuo, K., Fullerton, M.E. & Moeini, A. Treatment patterns and survival outcomes in patients with cervical cancer complicated by complete uterine prolapse: a systematic review of literature. Int Urogynecol J 27, 29–38 (2016). https://doi.org/10.1007/s00192-015-2731-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-015-2731-8