Abstract
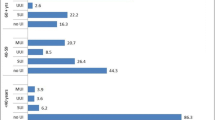
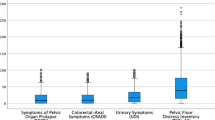
We aimed to determine the prevalence and bother from pelvic floor disorders (PFD) by obesity severity, hypothesizing that both would increase with higher degrees of obesity. We performed a secondary analysis of 1,155 females enrolled in an epidemiologic study that used a validated questionnaire to identify PFD. Prevalence and degree of bother were compared across three obesity groups. Logistic regression assessed the contribution of degree of obesity to the odds of having PFD. Prevalence of any PFD was highest in morbidly (57%) and severely (53%) obese compared to obese women (44%). Regression models demonstrated higher prevalence of pelvic organ prolapse, overactive bladder, stress urinary incontinence, and any PFD in morbidly compared to obese women and higher prevalence of stress urinary incontinence in severely obese compared to obese women. Degree of bother did not vary by degree of obesity. Prevalence of PFD increases with higher degrees of obesity.
Similar content being viewed by others
Abbreviations
- POP:
-
pelvic organ prolapse
- SUI:
-
stress urinary incontinence
- OAB:
-
overactive bladder
- AI:
-
anal incontinence
- PFD:
-
pelvic floor disorders
- BMI:
-
body mass index
- KP CARES:
-
Kaiser Permanente Continence-Associated Risk Epidemiology Study
- EPIQ:
-
Epidemiology of Prolapse and Incontinence Questionnaire
- VAS:
-
visual analog scale
References
Subak LL, Brown JS, Kraus SR, Brubaker L, Lin F, Richter HE et al (2006) The “costs” of urinary incontinence for women. Obstet Gynecol 107:908–916
Grimby A, Milsom I, Molander U, Wiklund I, Ekelund P (1993) The influence of urinary incontinence on the quality of life of elderly women. Age Ageing 22:82–89
Norton PA, MacDonald LD, Sedgwick PM, Stanton SL (1988) Distress and delay associated with urinary incontinence, frequency, and urgency in women. BMJ 297:1187–1189
Varma MG, Brown JS, Creasman JM, Thom DH, Van Den Eeden SK, Beattie MS et al (2006) Fecal incontinence in females older than aged 40 years: who is at risk? Dis Colon Rectum 49:841–851
Ogden CL, Carroll MD, Curtin LR, McDowell MA, Tabak CJ, Flegal KM (2006) Prevalence of overweight and obesity in the United States, 1999–2004. Jama 295:1549–1555
Lawrence JM, Lukacz ES, Nager CW, Hsu JW, Luber KM (2008) Prevalence and co-occurrence of pelvic floor disorders in community-dwelling women. Obstet Gynecol 111:678–685
Ogden CL, Carroll MD, McDowell MA, Flegal KM (2007) Obesity among adults in the United States-no change since 2003–2004. NCHS data brief no 1. National Center for Health Statistics, Hyattsville
Richter HE, Burgio KL, Brubaker L, Moalli P, Markland AD, Mallet V et al (2005) Factors associated with incontinence frequency in a surgical cohort of stress incontinent women. Am J Obstet Gynecol 193:2088–2093
Kapoor DS, Davila GW, Rosenthal RJ, Ghoniem GM (2004) Pelvic floor dysfunction in morbidly obese women: pilot study. Obes Res 12:1104–1107
Uustal Fornell E, Wingren G, Kjolhede P (2004) Factors associated with pelvic floor dysfunction with emphasis on urinary and fecal incontinence and genital prolapse: an epidemiological study. Acta Obstet Gynecol Scand 83:383–389
Dwyer PL, Lee ET, Hay DM (1988) Obesity and urinary incontinence in women. Br J Obstet Gynaecol 95:91–96
Roe B, Doll H (1999) Lifestyle factors and continence status: comparison of self-report data from a postal survey in England. J Wound Ostomy Continence Nurs 26:312–313 315–319
Yarnell JW, Voyle GJ, Sweetnam PM, Milbank J, Richards CJ, Stephenson TP (1982) Factors associated with urinary incontinence in women. J Epidemiol Community Health 36:58–63
Richter HE, Burgio KL, Clements RH, Goode PS, Redden DT, Varner RE (2005) Urinary and anal incontinence in morbidly obese women considering weight loss surgery. Obstet Gynecol 106:1272–1277
Lawrence JM, Lukacz ES, Liu IL, Nager CW, Luber KM (2007) Pelvic floor disorders, diabetes, and obesity in women: findings from the Kaiser Permanente Continence Associated Risk Epidemiology Study. Diabetes Care 30:2536–2541
Subak LL, Johnson C, Whitcomb E, Boban D, Saxton J, Brown JS (2002) Does weight loss improve incontinence in moderately obese women? Int Urogynecol J Pelvic Floor Dysfunct 13:40–43
Subak LL, Whitcomb E, Shen H, Saxton J, Vittinghoff E, Brown JS (2005) Weight loss: a novel and effective treatment for urinary incontinence. J Urol 174:190–195
Kuruba R, Almahmeed T, Martinez F, Torrella TA, Haines K, Nelson LG et al (2007) Bariatric surgery improves urinary incontinence in morbidly obese individuals. Surg Obes Relat Dis 3:586–590 discussion 590–591
Burgio KL, Richter HE, Clements RH, Redden DT, Goode PS (2007) Changes in urinary and fecal incontinence symptoms with weight loss surgery in morbidly obese women. Obstet Gynecol 110:1034–1040
Bump RC, Sugerman HJ, Fantl JA, McClish DK (1992) Obesity and lower urinary tract function in women: effect of surgically induced weight loss. Am J Obstet Gynecol 167:392–397 discussion 397–9
Lukacz ES, Lawrence JM, Contreras R, Nager CW, Luber KM (2006) Parity, mode of delivery, and pelvic floor disorders. Obstet Gynecol 107:1253–1260
Lukacz ES, Lawrence JM, Buckwalter JM, Burchette RJ, Nager CW, Luber KM (2005) Epidemiology of prolapse and incontinence questionnaire: validation of a new epidemiologic survey. Int Urogynecol J Pelvic Floor Dysfunct 16(4):272–284
Lukacz ES, Lawrence JM, Burchette RJ, Luber KM, Nager CW, Buckwalter JM (2004) The use of visual analog scale in urogynecologic research: a psychometric evaluation. Am J Obstet Gynecol 191(1):165–170
Foldspang A, Mommsen S (1995) Overweight and urinary incontinence in women. Ugeskr Laeger 157:5848–5851
Moller LM, Lose G, Jorgensen T (2001) Risk factors of lower urinary tract symptoms in women aged 40–60 years. Ugeskr Laeger 163:6598–6601
Wasserberg N, Haney M, Petrone P, Crookes P, Rosca J, Ritter M et al (2008) Fecal incontinence among morbid obese women seeking for weight loss surgery: an underappreciated association with adverse impact on quality of life. Int J Colorectal Dis 23:493–497
Gerten KA, Richter HE, Burgio KL, Wheeler TL, Goode PS, Redden DT (2007) Impact of urinary incontinence in morbidly obese women versus women seeking urogynecologic care. Urology 70:1082–1085
Wasserberg N, Haney M, Petrone P, Ritter M, Emami C, Rosca J et al (2007) Morbid obesity adversely impacts pelvic floor function in females seeking attention for weight loss surgery. Dis Colon Rectum 50:2096–2103
McAdams MA, Van Dam RM, Hu FB (2007) Comparison of self-reported and measured BMI as correlates of disease markers in US adults. Obesity (Silver Spring) 15:188–196
Noblett KL, Jensen JK, Ostergard DR (1997) The relationship of body mass index to intra-abdominal pressure as measured by multichannel cystometry. Int Urogynecol J Pelvic Floor Dysfunct 8:323–326
Funding
NICHD #R01 HD4113-01A1
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Whitcomb, E.L., Lukacz, E.S., Lawrence, J.M. et al. Prevalence and degree of bother from pelvic floor disorders in obese women. Int Urogynecol J 20, 289–294 (2009). https://doi.org/10.1007/s00192-008-0765-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-008-0765-x