Abstract
Purpose
The HemiCAP® implant for femoral resurfacing treatment of cartilage lesions was introduced in 2003. We present outcome from a prospective cohort study of 61 patients with both trochleal and condylar lesions treated with the HemiCAP® implant.
Methods
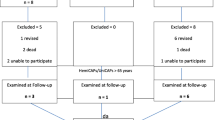
From 2007 to 2012, 61 patients were treated with femoral resurfacing using the HemiCAP implant. There were 36 femoral condyle implants and 25 trochleal implants. Indication for treatment with HemiCAP implant was symptomatic cartilage lesion at the femoral condyle demonstrated by MRI or arthroscopy, which was ICRS grade 3–4 and size less than 4 cm2. There were 24 males and 37 females with a median age of 49 (range 35–65) years. Patients were followed for 2 years with Knee Society subjective outcome scores (KSS), pain scores and radiographic evaluations and for 7 years with complications and reoperations.
Results
At 2-year follow-up, mean KSS was improved from 52 (6.2) to 90 (7.9), mean KSS function score was improved from 45 (7.5) to 92 (8.3), and mean Pain score improved from 7.1 (0.7) to 1.8 (1.7). Twenty-three per cent of implants were revised within 7 years to arthroplasty due to progression of cartilage lesions, progression of osteoarthritis, or increased knee pain. No difference between females and males was found for reoperation rate.
Conclusion
The present study demonstrated improved subjective outcome and reduced pain after femoral resurfacing using the HemiCAP implant in a relatively large cohort of patients with symptomatic cartilage lesions. A concerning 23 % reoperation rate with conversion to arthroplasty was found. Femoral resurfacing implantation treatment can be a temporary treatment for cartilage lesions expected to develop into osteoarthritis and for younger patients not eligible for arthroplasty treatment.
Level of evidence
IV.


Similar content being viewed by others
References
Australian Orthopaedic Association National Joint Replacement Registry (2013) Annual report
Becher C, Huber R, Thermann H, Ezechieli L, Ostermeier S, Wellmann M, von Skrbensky G (2011) Effects of a surface matching articular resurfacing device on tibiofemoral contact pressure: results from continuous dynamic flexion-extension cycles. Arch Orthop Trauma Surg 131(3):413–419
Becher C, Kalbe C, Thermann H, Paessler HH, Laprell H, Kaiser T, Fechner A, Bartsch S, Windhagen H, Ostermeier S (2011) Minimum 5-year results of focal articular prosthetic resurfacing for the treatment of full-thickness articular cartilage defects in the knee. Arch Orthop Trauma Surg 131(8):1135–1143
Biant LC, Bentley G, Vijayan S, Skinner JA, Carrington RW (2014) Long-term results of autologous chondrocyte implantation in the knee for chronic chondral and osteochondral defects. Am J Sports Med 42(9):2178–2183
Bollars P, Bousquet M, Vandekerckhove B, Hardeman F, Bellemans J (2012) Prosthetic inlay resurfacing for the treatment of focal, full thickness cartilage defects of the femoral condyle: a bridge between biologics and conventional arthroplasty. Knee Surg Sports Traumatol Arthrosc 20(9):1753–1759
Brennan SA, Devitt BM, O’Neill CJ, Nicholson P (2013) Focal femoral condyle resurfacing. Bone Joint J 95(3):301–304
Davies-Tuck ML, Wluka AE, Wang Y, Teichtahl AJ, Jones G, Ding C, Cicuttini FM (2008) The natural history of cartilage defects in people with knee osteoarthritis. Osteoarthr Cartil 16(3):337–342
Dhollander AA, Almqvist KF, Moens K, Vandekerckhove PJ, Verdonk R, Verdonk P, Victor J (2014) The use of a prosthetic inlay resurfacing as a salvage procedure for a failed cartilage repair. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-014-2999-0
Flecher X, Parratte S, Aubaniac JM, Argenson JN (2006) A 12–28-year followup study of closing wedge high tibial osteotomy. Clin Orthop Relat Res 452:91–96
Foran JR, Brown NM, Della Valle CJ, Berger RA, Galante JO (2013) Long-term survivorship and failure modes of unicompartmental knee arthroplasty. Clin Orthop Relat Res 471(1):102–108
Furnes O, Espehaug B, Lie SA, Vollset SE, Engesaeter LB, Havelin LI (2007) Failure mechanisms after unicompartmental and tricompartmental primary knee replacement with cement. J Bone Joint Surg Am 89(3):519–525
Gomoll AH, Farr J, Gillogly SD, Kercher J, Minas T (2010) Surgical management of articular cartilage defects of the knee. J Bone Joint Surg Am 92(14):2470–2490
Gross AE, Kim W, Las Heras F, Backstein D, Safir O, Pritzker KP (2008) Fresh osteochondral allografts for posttraumatic knee defects: long-term followup. Clin Orthop Relat Res 466(8):1863–1870
Harrysson OL, Robertsson O, Nayfeh JF (2004) Higher cumulative revision rate of knee arthroplasties in younger patients with osteoarthritis. Clin Orthop Relat Res 421:162–168
Heir S, Nerhus TK, Rotterud JH, Loken S, Ekeland A, Engebretsen L, Aroen A (2010) Focal cartilage defects in the knee impair quality of life as much as severe osteoarthritis: a comparison of knee injury and osteoarthritis outcome score in 4 patient categories scheduled for knee surgery. Am J Sports Med 38(2):231–237
Imhoff AB, Feucht MJ, Meidinger G, Schottle PB, Cotic M (2015) Prospective evaluation of anatomic patellofemoral inlay resurfacing: clinical, radiographic, and sports-related results after 24 months. Knee Surg Sports Traumatol Arthrosc 23(5):1299–1307
Insall JN, Dorr LD, Scott RD, Scott WN (1989) Rationale of the Knee Society clinical rating system. Clin Orthop Relat Res 248:13–14
Kellgren JH, Lawrence JS (1957) Radiological assessment of osteo-arthrosis. Ann Rheum Dis 16(4):494–502
Kirker-Head CA, Van Sickle DC, Ek SW, McCool JC (2006) Safety of, and biological and functional response to, a novel metallic implant for the management of focal full-thickness cartilage defects: preliminary assessment in an animal model out to 1 year. J Orthop Res 24(5):1095–1108
Kreuz PC, Erggelet C, Steinwachs MR, Krause SJ, Lahm A, Niemeyer P, Ghanem N, Uhl M, Sudkamp N (2006) Is microfracture of chondral defects in the knee associated with different results in patients aged 40 years or younger? Arthroscopy 22(11):1180–1186
Vanlauwe J, Saris DB, Victor J, Almqvist KF, Bellemans J, Luyten FP (2011) Five-year outcome of characterized chondrocyte implantation versus microfracture for symptomatic cartilage defects of the knee: early treatment matters. Am J Sports Med 39(12):2566–2574
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Laursen, J.O., Lind, M. Treatment of full-thickness femoral cartilage lesions using condyle resurfacing prosthesis. Knee Surg Sports Traumatol Arthrosc 25, 746–751 (2017). https://doi.org/10.1007/s00167-015-3726-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-015-3726-1