Abstract
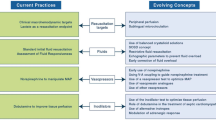
While guidelines provide important information on how to approach a patient in septic shock, “many challenges remain” for the management of these patients. In this narrative review, the panel discusses the challenges in identifying the right hemodynamic target, optimization of fluid therapy, selection of vasopressor agents, identification of patients who may benefit from inotropic agents or on the contrary beta-blockade, and use of steroids. The place for microcirculation-targeted therapy is debated as well as the use of alternative techniques (blood purification) and therapies (vitamin C). The implications of hemodynamic alterations on antibiotic doses is discussed. Finally, the specific challenges in low- and middle-income countries are addressed. Ongoing trials address some of these challenges, but many uncertainties will remain, and individualized therapies based on careful clinical assessment will continue to be essential to optimizing the care of patients with septic shock.


Similar content being viewed by others
References
Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M et al (2016) The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 315:801–810
Rhodes A, Evans LE, Alhazzani W, Levy MM, Antonelli M, Ferrer R et al (2017) Surviving Sepsis Campaign: international guidelines for management of sepsis and septic shock: 2016. Intensive Care Med 43:304–377
De Backer D, Bakker J, Cecconi M, Hajjar L, Liu DW, Lobo S et al (2018) Alternatives to the Swan-Ganz catheter. Intensive Care Med 44:730–741
Alegria L, Vera M, Dreyse J, Castro R, Carpio D, Henriquez C et al (2017) A hypoperfusion context may aid to interpret hyperlactatemia in sepsis-3 septic shock patients: a proof-of-concept study. Ann Intensive Care 7:29
Vincent JL, De Backer D (2018) From early goal-directed therapy to late(r) ScvO2 checks. Chest 154:1267–1269
Ospina-Tascon GA, Umana M, Bermudez W, Bautista-Rincon DF, Hernandez G, Bruhn A et al (2015) Combination of arterial lactate levels and venous-arterial CO to arterial-venous O content difference ratio as markers of resuscitation in patients with septic shock. Intensive Care Med 41:796–805
De Backer D (2003) Lactic acidosis. Intensive Care Med 29:699–702
Vincent JL, De Backer D (2013) Circulatory shock. N Engl J Med 369:1726–1734
Cecconi M, Hofer C, Teboul JL, Pettila V, Wilkman E, Molnar Z et al (2015) Fluid challenges in intensive care: the FENICE study: a global inception cohort study. Intensive Care Med 41:1529–1537
Sakr Y, Rubatto Birri PN, Kotfis K, Nanchal R, Shah B, Kluge S et al (2017) Higher Fluid Balance Increases the Risk of Death From Sepsis: results From a Large International Audit. Crit Care Med 45:386–394
Hjortrup PB, Haase N, Bundgaard H, Thomsen SL, Winding R, Pettila V et al (2016) Restricting volumes of resuscitation fluid in adults with septic shock after initial management: the CLASSIC randomised, parallel-group, multicentre feasibility trial. Intensive Care Med 42:1695–1705
Cecconi M, De Backer D, Antonelli M, Beale RJ, Bakker J, Hofer C et al (2014) Consensus on Circulatory Shock and hemodynamic monitoring. Task Force of the European Society of Intensive Care Medicine. Intensive Care Med 40:1795–1815
Monnet X, Julien F, Ait-Hamou N, Lequoy M, Gosset C, Jozwiak M et al (2013) Lactate and venoarterial carbon dioxide difference/arterial-venous oxygen difference ratio, but not central venous oxygen saturation, predict increase in oxygen consumption in fluid responders. Crit Care Med 41:1412–1420
Aya HD, Rhodes A, Chis SI, Fletcher N, Grounds RM, Cecconi M (2017) Hemodynamic Effect of Different doses of fluids for a fluid challenge: a quasi-randomized controlled study. Crit Care Med 45:e161–e168
Aya HD, Ster IC, Fletcher N, Grounds RM, Rhodes A, Cecconi M (2016) Pharmacodynamic analysis of a fluid challenge. Crit Care Med 44:880–891
Perner A, Haase N, Guttormsen AB, Tenhunen J, Klemenzson G, Aneman A et al (2012) Hydroxyethyl starch 130/0.42 versus Ringer’s acetate in severe sepsis. N Engl J Med 367:124–134
Avni T, Lador A, Lev S, Leibovici L, Paul M, Grossman A (2015) Vasopressors for the treatment of septic shock: systematic review and meta-analysis. PLoS One 10:e0129305
De Backer D, Biston P, Devriendt J, Madl C, Chochrad D, Aldecoa C et al (2010) Comparison of dopamine and norepinephrine in the treatment of shock. N Engl J Med 362:779–789
Myburgh JA, Higgins A, Jovanovska A, Lipman J, Ramakrishnan N, Santamaria J (2008) A comparison of epinephrine and norepinephrine in critically ill patients. Intensive Care Med 34:2226–2234
Russell JA, Walley KR, Singer J, Gordon AC, Hebert PC, Cooper DJ et al (2008) Vasopressin versus norepinephrine infusion in patients with septic shock. N Engl J Med 358:877–887
Khanna A, English SW, Wang XS, Ham K, Tumlin J, Szerlip H et al (2017) Angiotensin II for the Treatment of Vasodilatory Shock. N Engl J Med 377:419–430
Annane D, Ouanes-Besbes L, De BD, Du B, Gordon AC, Hernandez G et al (2018) A global perspective on vasoactive agents in shock. Intensive Care Med 44:833–846
Gordon AC, Perkins GD, Singer M, McAuley DF, Orme RM, Santhakumaran S et al (2016) Levosimendan for the Prevention of Acute Organ Dysfunction in Sepsis. N Engl J Med 375:1638–1648
Ackland GL, Yao ST, Rudiger A, Dyson A, Stidwill R, Poputnikov D et al (2010) Cardioprotection, attenuated systemic inflammation, and survival benefit of beta1-adrenoceptor blockade in severe sepsis in rats. Crit Care Med 38:388–394
Kimmoun A, Louis H, Al KN, Delemazure J, Dessales N, Wei C et al (2015) beta1-Adrenergic inhibition improves cardiac and vascular function in experimental septic shock. Crit Care Med 43:e332–e340
Morelli A, Ertmer C, Westphal M, Rehberg S, Kampmeier T, Ligges S et al (2013) Effect of heart rate control with esmolol on hemodynamic and clinical outcomes in patients with septic shock: a randomized clinical trial. JAMA 310:1683–1691
Du W, Wang XT, Long Y, Liu DW (2016) Efficacy and safety of esmolol in treatment of patients with septic shock. Chin Med J (Engl) 129:1658–1665
De Backer D, Creteur J, Preiser JC, Dubois MJ, Vincent JL (2002) Microvascular blood flow is altered in patients with sepsis. Am J Respir Crit Care Med 166:98–104
De Backer D, Donadello K, Sakr Y, Ospina-Tascon GA, Salgado DR, Scolletta S et al (2013) Microcirculatory alterations in patients with severe sepsis: impact of time of assessment and relationship with outcome. Crit Care Med 41:791–799
De Backer D, Donadello K, Taccone FS, Ospina-Tascon G, Salgado D, Vincent JL (2011) Microcirculatory alterations: potential mechanisms and implications for therapy. Ann Intensive Care 1:27
Ince C, Boerma EC, Cecconi M, De Backer D, Shapiro NI, Duranteau J et al (2018) Second consensus on the assessment of sublingual microcirculation in critically ill patients: results from a task force of the European Society of Intensive Care Medicine. Intensive Care Med 44:281–299
Ospina-Tascon GA, Umana M, Bermudez WF, Bautista-Rincon DF, Valencia JD, Madrinan HJ et al (2016) Can venous-to-arterial carbon dioxide differences reflect microcirculatory alterations in patients with septic shock? Intensive Care Med 42:211–221
Ospina-Tascon G, Neves AP, Occhipinti G, Donadello K, Buchele G, Simion D et al (2010) Effects of fluids on microvascular perfusion in patients with severe sepsis. Intensive Care Med 36:949–955
Hoffmann JN, Vollmar B, Laschke MW, Inthorn D, Schildberg FW, Menger MD (2002) Hydroxyethyl starch (130 kD), but not crystalloid volume support, improves microcirculation during normotensive endotoxemia. Anesthesiology 97:460–470
Dubin A, Pozo MO, Casabella CA, Palizas F Jr, Murias G, Moseinco MC et al (2009) Increasing arterial blood pressure with norepinephrine does not improve microcirculatory blood flow: a prospective study. Crit Care 13:R92
De Backer D, Creteur J, Dubois MJ, Sakr Y, Koch M, Verdant C et al (2006) The effects of dobutamine on microcirculatory alterations in patients with septic shock are independent of its systemic effects. Crit Care Med 34:403–408
Hernandez G, Bruhn A, Luengo C, Regueira T, Kattan E, Fuentealba A et al (2013) Effects of dobutamine on systemic, regional and microcirculatory perfusion parameters in septic shock: a randomized, placebo-controlled, double-blind, crossover study. Intensive Care Med 39:1435–1443
Bone RC, Fisher CJ, Clemmer TP, Slotman GJ, Metz CA, Balk RA (1987) A controlled clinical trial of high-dose methylprednisolone in the treatment of severe sepsis and septic shock. N Engl J Med 317:653–658
Annane D, Sebille V, Charpentier C, Bollaert PE, Francois B, Korach JM et al (2002) Effect of treatment with low doses of hydrocortisone and fludrocortisone on mortality in patients with septic shock. JAMA 288:862–871
Sprung CL, Annane D, Keh D, Moreno R, Singer M, Freivogel K et al (2008) Hydrocortisone therapy for patients with septic shock. N Engl J Med 358:111–124
Venkatesh B, Finfer S, Cohen J, Rajbhandari D, Arabi Y, Bellomo R et al (2018) Adjunctive glucocorticoid therapy in patients with septic shock. N Engl J Med 378:797–808
Venkatesh B, Finfer S, Myburgh J, Cohen J, Billot L (2018) Long-Term Outcomes of the ADRENAL trial. N Engl J Med 378:1744–1745
Annane D, Renault A, Brun-Buisson C, Megarbane B, Quenot JP, Siami S et al (2018) Hydrocortisone plus fludrocortisone for adults with septic shock. N Engl J Med 378:809–818
Rygard SL, Butler E, Granholm A, Moller MH, Cohen J, Finfer S et al (2018) Low-dose corticosteroids for adult patients with septic shock: a systematic review with meta-analysis and trial sequential analysis. Intensive Care Med 44:1003–1016
Marik PE, Khangoora V, Rivera R, Hooper MH, Catravas J (2017) Hydrocortisone, vitamin C, and thiamine for the treatment of severe sepsis and septic shock: a retrospective before-after study. Chest 151:1229–1238
Russell JA, Walley KR, Gordon AC, Cooper DJ, Hebert PC, Singer J et al (2009) Interaction of vasopressin infusion, corticosteroid treatment, and mortality of septic shock. Crit Care Med 37:811–818
Cruz DN, Antonelli M, Fumagalli R, Foltran F, Brienza N, Donati A et al (2009) Early use of polymyxin B hemoperfusion in abdominal septic shock: the EUPHAS randomized controlled trial. JAMA 301:2445–2452
Dellinger RP, Bagshaw SM, Antonelli M, Foster DM, Klein DJ, Marshall JC et al (2018) Effect of targeted polymyxin B hemoperfusion on 28-day mortality in patients with septic shock and elevated endotoxin level: the EUPHRATES randomized clinical trial. JAMA 320:1455–1463
Schadler D, Pausch C, Heise D, Meier-Hellmann A, Brederlau J, Weiler N et al (2017) The effect of a novel extracorporeal cytokine hemoadsorption device on IL-6 elimination in septic patients: a randomized controlled trial. PLoS One 12:e0187015
Ala-Kokko TI, Laurila J, Koskenkari J (2011) A new endotoxin adsorber in septic shock: observational case series. Blood Purif 32:303–309
Livigni S, Bertolini G, Rossi C, Ferrari F, Giardino M, Pozzato M et al (2014) Efficacy of coupled plasma filtration adsorption (CPFA) in patients with septic shock: a multicenter randomised controlled clinical trial. BMJ Open 4:e003536
Schorah CJ, Downing C, Piripitsi A, Gallivan L, Al-Hazaa AH, Sanderson MJ et al (1996) Total vitamin C, ascorbic acid, and dehydroascorbic acid concentrations in plasma of critically ill patients. Am J Clin Nutr 63:760–765
Wilson JX (2013) Evaluation of vitamin C for adjuvant sepsis therapy. Antioxid Redox Signal 19:2129–2140
Fowler AA III, Syed AA, Knowlson S, Sculthorpe R, Farthing D, DeWilde C et al (2014) Phase I safety trial of intravenous ascorbic acid in patients with severe sepsis. J Transl Med 12:32
Zabet MH, Mohammadi M, Ramezani M, Khalili H (2016) Effect of high-dose Ascorbic acid on vasopressor’s requirement in septic shock. J Res Pharm Pract 5:94–100
Taccone FS, Laterre PF, Spapen H, Dugernier T, Delattre I, Layeux B et al (2010) Revisiting the loading dose of amikacin for patients with severe sepsis and septic shock. Crit Care 14:R53
Roberts JA, Taccone FS, Lipman J (2016) Understanding PK/PD. Intensive Care Med 42:1797–1800
Blot S, Lipman J, Roberts DM, Roberts JA (2014) The influence of acute kidney injury on antimicrobial dosing in critically ill patients: are dose reductions always necessary? Diagn Microbiol Infect Dis 79:77–84
Udy AA, Roberts JA, Shorr AF, Boots RJ, Lipman J (2013) Augmented renal clearance in septic and traumatized patients with normal plasma creatinine concentrations: identifying at-risk patients. Crit Care 17:R35
Baptista JP, Udy AA, Sousa E, Pimentel J, Wang L, Roberts JA et al (2011) A comparison of estimates of glomerular filtration in critically ill patients with augmented renal clearance. Crit Care 15:R139
De Waele JJ, Lipman J, Akova M, Bassetti M, Dimopoulos G, Kaukonen M et al (2014) Risk factors for target non-attainment during empirical treatment with beta-lactam antibiotics in critically ill patients. Intensive Care Med 40:1340–1351
Abdul-Aziz MH, Lipman J, Akova M, Bassetti M, De Waele JJ, Dimopoulos G et al (2016) Is prolonged infusion of piperacillin/tazobactam and meropenem in critically ill patients associated with improved pharmacokinetic/pharmacodynamic and patient outcomes? An observation from the Defining Antibiotic Levels in Intensive care unit patients (DALI) cohort. J Antimicrob Chemother 71:196–207
Dulhunty JM, Roberts JA, Davis JS, Webb SA, Bellomo R, Gomersall C et al (2015) A Multicenter Randomized Trial of Continuous versus Intermittent beta-Lactam Infusion in Severe Sepsis. Am J Respir Crit Care Med 192:1298–1305
Machado FR, Cavalcanti AB, Bozza FA, Ferreira EM, Angotti Carrara FS, Sousa JL et al (2017) The epidemiology of sepsis in Brazilian intensive care units (the Sepsis PREvalence Assessment Database, SPREAD): an observational study. Lancet Infect Dis 17:1180–1189
Maitland K, Kiguli S, Opoka RO, Engoru C, Olupot-Olupot P, Akech SO et al (2011) Mortality after fluid bolus in African children with severe infection. N Engl J Med 364:2483–2495
Andrews B, Semler MW, Muchemwa L, Kelly P, Lakhi S, Heimburger DC et al (2017) Effect of an early resuscitation protocol on in-hospital mortality among adults with sepsis and hypotension: a randomized clinical trial. JAMA 318:1233–1240
Machado FR, Angus DC (2017) Trying to improve sepsis care in low-resource settings. JAMA 318:1225–1227
Cavalcanti AB, Bozza FA, Machado FR, Salluh JI, Campagnucci VP, Vendramim P et al (2016) Effect of a quality improvement intervention with daily round checklists, goal setting, and clinician prompting on mortality of critically ill patients: a randomized clinical trial. JAMA 315:1480–1490
Singhi S, Rungta N, Nallasamy K, Bhalla A, Peter JV, Chaudhary D et al (2017) Tropical fevers in Indian intensive care units: a prospective multicenter study. Indian J Crit Care Med 21:811–818
Gordon AC, Russell JA, Walley KR, Singer J, Ayers D, Storms MM et al (2010) The effects of vasopressin on acute kidney injury in septic shock. Intensive Care Med 36:83–91
Morelli A, Ertmer C, Rehberg S, Lange M, Orecchioni A, Cecchini V et al (2009) Continuous terlipressin versus vasopressin infusion in septic shock (TERLIVAP): a randomized, controlled pilot study. Crit Care 13:R130
Liu ZM, Chen J, Kou Q, Lin Q, Huang X, Tang Z et al (2018) Terlipressin versus norepinephrine as infusion in patients with septic shock: a multicentre, randomised, double-blinded trial. Intensive Care Med
Tumlin JA, Murugan R, Deane AM, Ostermann M, Busse LW, Ham KR et al (2018) Outcomes in patients with vasodilatory shock and renal replacement therapy treated with intravenous angiotensin II. Crit Care Med 46:949–957
Russell JA, Vincent JL, Kjolbye AL, Olsson H, Blemings A, Spapen H et al (2017) Selepressin, a novel selective vasopressin V1A agonist, is an effective substitute for norepinephrine in a phase IIa randomized, placebo-controlled trial in septic shock patients. Crit Care 21:213
Kirov MY, Evgenov OV, Evgenov NV, Egorina EM, Sovershaev MA, Sveinbjornsson B et al (2001) Infusion of methylene blue in human septic shock: a pilot, randomized, controlled study. Crit Care Med 29:1860–1867
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Daniel De Backer: consultant to and material for studies by Edwards Lifesciences. Maurizio Cecconi: consultancy for Edwards Lifesciences, LiDCO, Cheetah, Masimo. Jeffrey Lipman: MSD (Australia)—Antibacterials Advisory Board; honoraria for lectures—Pfizer South Africa, MSD South Africa; committee—Pfizer International 2018 Anti-Infectives. Flavia Machado: member of steering committee for BASIC study, for which drug was supplied by Baxter. Sheila Nainan Myatra: no conflict of interest. Marlies Ostermann: research funding from Ja Jolla Pharma. Anders Perner: Dept. of Intensive Care at Rigshospitalet has received support for research from CSL Behring, Fresenius Kabi, and Ferring Pharmaceutical. Jean-Louis Teboul: member of the medical advisory board of Pulsion/Getinge (Germany). Jean Louis Vincent: no conflict of interest. Keith Walley: no conflict of interest.
Ethics approval
An approval by an ethics committee was not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
De Backer, D., Cecconi, M., Lipman, J. et al. Challenges in the management of septic shock: a narrative review. Intensive Care Med 45, 420–433 (2019). https://doi.org/10.1007/s00134-019-05544-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-019-05544-x