Abstract
Objective
To evaluate clinical and treatment factors for patients recorded in the Extracorporeal Life Support Organization (ELSO) registry and survival of adult extracorporeal membrane oxygenation (ECMO) respiratory failure patients.
Design and patients
Retrospective case review of the ELSO registry from 1986–2006. Data were analyzed separately for the entire time period and the most recent years (2002–2006).
Results
Of 1,473 patients, 50% survived to discharge. Median age was 34 years. Most patients (78%) were supported with venovenous ECMO. In a multi-variate logistic regression model, pre-ECMO factors including increasing age, decreased weight, days on mechanical ventilation before ECMO, arterial blood pH ≤ 7.18, and Hispanic and Asian race compared to white race were associated with increased odds of death. For the most recent years (n = 600), age and PaCO2 ≥ 70 compared to PaCO2 ≤ 44 were also associated with increased odds of death. The two diagnostic categories acute respiratory failure and asthma compared to ARDS were associated with decreased odds of mortality as was venovenous compared to venoarterial mode. CPR and complications while on ECMO including circuit rupture, central nervous system infarction or hemorrhage, gastrointestinal or pulmonary hemorrhage, and arterial blood pH < 7.2 or >7.6 were associated with increased odds of death.
Conclusions
Survival among this cohort of adults with severe respiratory failure supported with ECMO was 50%. Advanced patient age, increased pre-ECMO ventilation duration, diagnosis category and complications while on ECMO were associated with mortality. Prospective studies are needed to evaluate the role of this complex support mode.
Similar content being viewed by others
Introduction
Extracorporeal membrane oxygenation (ECMO) was first used in adults with respiratory failure in the 1970s [1]. A multi-center randomized trial failed to identify any benefit from ECMO—with mortality greater than 90% in both study and control groups—which discouraged widespread application of ECMO in adults [2]. The study was closed prematurely and later criticized for shortcomings including exclusive use of venoarterial (VA) ECMO, lack of established ECMO experience in many centers, extensive blood loss among ECMO patients, prolonged mechanical ventilation preceding ECMO and lack of “lung rest” ventilator settings among the ECMO patients [3]. In an uncontrolled study in 1986, Gatttioni et al. reported improved outcome with extracorporeal CO2 (ECCO2R) removal (49% survival) [4]. A randomized trial of ECCO2R reported no survival benefit for ECCO2 (33 vs. 41% for controls) [5]. These results and successful application of ECMO support in neonates [6–8] and children [9] encouraged cautious reapplication in adults in the 1990s [10].
The modern era of ECMO for adults with respiratory failure was pioneered by Bartlett et al. [10, 11]. Their results and those at other institutions showed that ECMO could be applied with encouraging survival, exceeding 50% [12–19]. In a recently completed, multi-center randomized controlled trial, the conventional ventilation or ECMO for severe respiratory failure (CESAR trial), ECMO demonstrated a survival benefit at 6 months [20, 21]. These results must, however, be interpreted in light of an unusual randomization strategy in which all ECMO patients were treated at one center and control patients remained at the referring center.
The Extracorporeal Life Support Organization (ELSO) has collected data on ECMO patients from international centers since 1986 and thus represents a cross section of ECMO practice. Submission of cases to ELSO is voluntary. We analyzed the ELSO data registry for adult patients with respiratory failure to describe the population and determine factors associated with hospital survival. We hypothesized that older patients and prolonged duration of mechanical ventilation prior to ECMO would be associated with increased odds of death.
Materials and methods
We queried the ELSO registry for adult patients (age ≥16 years) with respiratory failure from 1986 through 2006. Currently, data from 116 US and 14 international centers are submitted on standardized ELSO forms. Each institution approves data reported to the registry through their local institutional review board (IRB). Data are limited to the hospitalization that includes the ECMO run. The decision to employ ECMO is made at each center without standardization. Studies of the ELSO database are approved as analyses of de-identified data by the Registry Committee of ELSO and the University of Michigan IRB.
Only data from the initial ECMO run were included. Variables analyzed included demographic information, ICD-09 diagnosis codes (reviewed by two authors independently and disagreement resolved after review by a third author), ECMO mode, duration and complications. Patients were also classified as having a primary (e.g., pneumonia) or secondary (e.g., sepsis) lung injury. Survival was to hospital discharge. Patient race was categorized as African American, Asian, Hispanic, white and “other.” ECMO mode was categorized as VA, venovenous (VV), VV to VA and miscellaneous. VA mode with additional venous drainage (VA + V) and VA to VV modes were included in the VA category, while VV + V mode was coded as VV. Mechanical ventilation was classified as high frequency (HFV) for high frequency oscillatory or jet ventilation, while all other ventilation modes were grouped as conventional mechanical ventilation.
Other pre-ECMO variables included cardiopulmonary resuscitation (CPR), documented infections, mechanical ventilation parameters, arterial blood gas data and hemodynamic data (including systolic, diastolic and mean blood pressure). PaO2/FiO2 and AaDO2 were calculated from the data provided.
Complications occurring only during ECMO support were evaluated. Mechanical complications included malfunction of any component of the circuit. Circuit clots and tubing rupture were analyzed separately. Patient complications were evaluated by organ system. Radiographic evidence of neurologic injury included infarction or CNS hemorrhage. Renal insufficiency (serum creatinine from 1.5 to 3.0 mg/dl) and renal failure (serum creatinine >3.0 mg/dl) were combined in the multivariable model as “renal dysfunction.” Renal replacement therapy included dialysis or continuous hemofiltration. Hypo- and hyperglycemia were defined as serum glucose <40 and >240 mg/dl, respectively. Complications were analyzed based on survival to discharge and also upon initial mode of ECMO. Patients were divided into time quartiles to assess trends over the course of the study. Summary data for the most recent years (2002–2006) were reported in addition to those for the entire study.
Statistical analysis
Demographic, pre-ECMO and ECMO support details and ECMO complications were compared for patients who survived to hospital discharge with those who died. The Mann–Whitney U test was used to compare continuous data and the Pearson’s chi-square test for categorical data. The Fisher exact test was employed when expected counts in >20% of cells were <5. Trends in ECMO use over time were compared using the Mantel–Haenszel chi-square for linear association. Continuous variables when analyzed by quartiles of the study period were analyzed by analysis of variance (ANOVA) using Tukey’s b post hoc test for changes over time.
Candidate variables for inclusion in a multivariable logistic regression model to predict death were chosen from the bivariate analysis. Variables missing data in excess of 30% of cases were excluded. Criteria for variable selection were set at a p value of 0.1. A forward selection process was used for entry of variables into the model. The variable pH was divided into the lowest quartile (pH < 7.18), middle two quartiles (pH 7.18–7.36) and highest quartiles (pH > 7.36). Data were received in Excel (Microsoft Inc., Redmond, WA) then transferred to a SPSS file version 14.0 software (SPSS Inc, Chicago, IL). Data were reported as frequency (n) with proportion (%), or median values with inter-quartile range (25th, 75th percentile). Statistical significance was defined as a p value < 0.05. The authors had full access to the data and take responsibility for its integrity.
Results
Study population
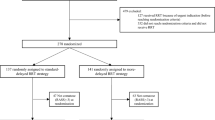
A total of 1,473 patients (1,519 ECMO runs) were supported with ECMO for respiratory failure from 1986–2006. Forty-three patients (3%) had a second run, and three patients (0.2%) had a third run. Survival for the index ECMO run was 50% (Table 1). The patient median age was 34 years (range: 16.0–84.2 years), and median weight was 75 kg (range: 46–168 kg). The majority of patients were initially supported with VV ECMO (78%), and the median time of support was 154 h [interquartile range (IQR): 75, 284 h]. From 2002–2006, 600 patients were supported with ECMO with 50% survival. Survival did not improve with time, although the number of patients increased each year (data not shown).
Survivors were significantly younger and weighed more than non-survivors (Table 1). No survival difference existed by gender. Survival varied significantly by race and by diagnostic category. Patients with primary lung injury (n = 819) had 53% survival, while those with secondary lung injury (n = 654) demonstrated 48% survival (p = 0.06). In the most recent years, patients with primary lung disease (n = 255) again had a non-significant trend for increased survival (53% vs. 48%, p = 0.32).
Differences in pre-ECMO and ECMO support variables between survivors and non-survivors
For evaluated pre-ECMO therapies, no differences existed between survivors and non-survivors except in the use of neuromuscular blockade (NMB) (Table 2). For the most recent years no significant difference in pre-ECMO therapies was present. Survivors had significantly shorter time on mechanical ventilation before ECMO. No differences in pre-ECMO ventilator settings, cardiopulmonary arrests or infections existed. When pre-ECMO blood gas data were evaluated, survivors had a significantly higher pH and lower arterial PCO2 than non-survivors. No statistical differences existed in pre-ECMO vital signs (data not shown).
Duration of ECMO support did not differ between non-survivors and survivors (Table 2). However, patients supported with VV ECMO had significantly greater odds of survival compared to VA patients. After 24 h on ECMO, survivors had a significantly lower PIP and FiO2. In the most recent years, only FiO2 was significantly lower in the survivors. Few patients required bridge to lung transplantation with no difference between groups.
ECMO complications and survival
Non-survivors had a higher rate of ECMO complications including circuit mechanical complications and rupture (Table 3). The incidence of circuit clots did not differ between groups. Brain death occurred in 5% of all patients (6% in 2002–2006). Radiographic evidence of CNS injury occurred more commonly among non-survivors, but seizures did not; however, both complications were more common in the most recent years. Non-survivors showed significantly higher rates of all renal complications. These differences were similar in the most recent years except for renal failure. Surgical, GI and pulmonary hemorrhages were more frequent in non-survivors, but in the most recent years surgical bleeding was no longer significant. Hyperglycemia and arterial pH < 7.20 or pH > 7.60, receipt of CPR or inotropic infusions, infections, arrythmias and pneumothorax occurred more frequently while on ECMO in non-survivors.
The rates of complications occurring on ECMO were compared according to initial mode of ECMO deployed. Complications occurred more commonly among patients started on VA ECMO including circuit rupture, brain death, renal insufficiency, renal failure, surgical and pulmonary hemorrhage, hyperglycemia, arterial alkalosis (pH > 7.60) and the receipt of inotropic infusions. However, patients who originally received VV ECMO had higher rates of pneumothorax, leukopenia and CPR. Of the 95 patients in the VV group who received CPR, 7 (7%) were converted to VA ECMO.
Differences in pre-ECMO and ECMO variables analyzed over the duration of the study
When the period of data acquisition was divided into quartiles, patient age, weight, male gender, rate of pre-ECMO cardiac arrest and infections increased significantly over time (Table 4). Adjunctive therapies including cardioactive medications, inhaled NO, NMB and bicarbonate became more common throughout the data acquisition period. Patients had decreasing time on the ventilator, arterial pH and increasing PaCO2 prior to ECMO.
When complications on ECMO were analyzed over time (Table 5), circuit rupture and pneumothorax became less frequent, but circuit clots, renal insufficiency, renal replacement therapies, pulmonary hemorrhage, inotropic medications, hyperglycemia, extremes of pH, arrhythmias and hypertension became more common.
Factors associated with mortality in patients supported with ECMO
Two separate models were developed to evaluate factors associated with death, one to determine pre-ECMO variables and another to evaluate parameters while on ECMO (Table 6). Advancing patient age, days on mechanical ventilation prior to ECMO and decreasing patient weight were associated with increased odds of death, but only advancing age was significant in the most recent years. In all patients pre-ECMO arterial pH < 7.18 and, in the most recent years, PaCO2 ≥ 70 torr were associated with increased odds of death. Asian race had greater odds of death when compared to white race, a difference not found in the most recent years. Patients with a diagnosis of acute respiratory failure or asthma had decreased odds of mortality compared to patients with ARDS. Compared to VA ECMO, the use of VV ECMO was associated with decreased odds of mortality, while change from VV to VA mode was associated with increased odds of death, but not in the most recent time period. However, only 24 patients were treated with initial VV and changed to VA from 2002 to 2006.
Factors while on ECMO that were associated with increased odds of death included circuit rupture, receipt of CPR, CNS injury, GI or pulmonary hemorrhage, extremes of arterial pH (<7.20 and >7.60), inotropic infusions and renal dysfunction. Inotropic infusions and renal dysfunction were no longer significant in the most recent years, while renal insufficiency significantly increased odds of death.
Discussion
In this cohort of adults supported with ECMO for respiratory failure, survival was 50%. Increasing age, decreasing weight and pre-ECMO arterial blood pH ≤ 7.18 were associated with increased odds of mortality. Patients with either “acute respiratory failure” or asthma demonstrated decreased odds of mortality compared to those with ARDS. Increased duration of pre-ECMO mechanical ventilation decreased survival for all patients, but not in the most recent years. VV ECMO mode had increased survival compared to VA ECMO. The change from VV to VA ECMO was associated with increased odds of death. As expected, complications during ECMO were associated with increased odds of death. The frequency of pre-ECMO special therapies and ECMO complications were more common in the most recent treatment years, suggesting ECMO was used in more complex patients; however, survival did not vary with treatment years.
The 50% survival of this cohort of patients with severe respiratory failure confirmed the increased survival rates of recent ECMO studies [11–19]. Some of these studies were small case series [12, 15, 16], and control groups were difficult to define as the criteria for institution of ECMO was often either acute respiratory collapse or respiratory failure “unresponsive” to conventional therapy. However, ECMO was applied in a diverse group of patients with severe lung disease including trauma and sepsis patients despite the absence of its standardization. The key strategy is that ECMO is used to aid adequate oxygen delivery with acceptable ventilator settings to limit ventilator-associated lung injury (VALI). Unfortunately, the absence of ECMO standardization and clearly defined control groups are important limitations for this and other ECMO studies. A recently completed, multi-center, randomized, controlled study, the CESAR trial, had as the primary outcome survival at 6 months without severe disability [20, 21]. Although ECMO provided a survival benefit, an important design flaw was that all patients in the ECMO arm were treated at a single center while the control group remained at referring tertiary hospitals, rendering the two groups potentially unequal. Unfortunately, this shortcoming severely limits conclusions regarding survival benefit attributable to ECMO.
Several independent factors were associated with outcome in this cohort. Increasing duration of pre-ECMO mechanical ventilation increased the odds of mortality. This relationship did not hold in the most recent cohort, but there was a significant decrease in duration of pre-ECMO ventilation over the years of data acquisition. No other ventilator parameter was associated with mortality, but tidal volume and plateau pressure were not recorded. So, it remains unclear how much pre-ECMO duration of ventilation versus the precise ventilation strategy contributes to outcome [11, 14–16].
Another independent factor associated with improved survival was VV ECMO mode. VV ECMO patients suffered fewer complications, many of which were associated with mortality [22]. However, the modes are employed to somewhat different patient populations because of their inherent differences. Unlike VA ECMO, VV ECMO does not provide direct cardiac support, although by increasing mixed venous oxygenation and permitting lower ventilator settings, it may improve heart function [23, 24]. Consequently, the apparent benefit of VV ECMO may be attributable to some extent to differences in patient population. Still, VV ECMO appears to be the first choice for respiratory failure without severe hemodynamic instability if extracorporeal support is to be provided.
ECMO cases have increased in recent years, but mortality has not changed despite improvements in intensive care and mechanical ventilation. However, during the period of data acquisition there has been an increase in apparent patient complexity, including those previously considered to have contraindications [10] (immunosuppression, sepsis, etc.). Furthermore, the database also includes the use of ECMO as a “rescue” and the “learning curve” periods for newer centers [14, 24]. Comparison of patient characteristics and ECMO complications support the conclusion that older, more complex patients were placed on ECMO in recent years. Selection criteria for ECMO patients have remained difficult to define and are, largely, based on local experience. Because of limited generalizability of these data and the frequent use of ECMO as a “rescue” therapy, definitive conclusions regarding the efficacy of ECMO in promoting survival for patients with respiratory failure compared to conventional therapy cannot be drawn from these data. However, we can say that at least 50% of patients with respiratory failure who received ECMO survived to hospital discharge.
The primary deficiencies of this study arise from its retrospective, uncontrolled nature and the lack of standardized criteria for the application of ECMO. Many variables including patient selection, indication for ECMO institution and ECMO mode are neither included in the ELSO database nor standardized, but rather are center specific. Data coding and entry are performed at each institution, and many fields remain empty at the time of data submission. Also, the ELSO database lacks key variables such as tidal volume, plateau pressures, and delineation of modes of conventional ventilation both before and during the ECMO run. Diagnoses are recorded as the ICD-9 codes, which have well-described shortcomings [25]. These limitations are compounded by the fact that ELSO does not release information on ECMO centers, so no conclusions can be made about the influence of center trends. The concatenation of these limitations underscores the need for controlled, prospective studies. Important questions raised by these data include whether ECMO is superior to low tidal volume ventilation, optimal timing of ECMO application and the limits of its use as a rescue therapy.
In conclusion, in this large multi-center database, adults with respiratory failure supported with ECMO, achieved a 50% survival. ECMO complications appear important contributors to mortality. The data from the ELSO registry indicates that ECMO works best when applied earlier in the course of lung disease. But a great need exists for prospective studies to define more clearly the role of optimal timing for application of this expensive support modality and for the limits of the possibility for “rescue” of moribund patients.
References
Hill JD, O’Brien TG, Murray JJ, Dontigny L, Bramson ML, Osborn JJ, Gerbode F (1972) Prolonged extracorporeal oxygenation for acute post-traumatic respiratory failure (shock-lung syndrome): use of Bramson membrane lung. N Engl J Med 286:629–634
Zapol WM, Snider MT, Hill JD, Fallat RJ, Bartlett RH, Edmunds LH, Morris AH, Peirce EC 2nd, Thomas AN, Proctor HJ, Drinker PA, Pratt PC, Bagniewski A, Miller RG Jr (1979) Extracorporeal membrane oxygenation in severe acute respiratory failure. A randomized prospective study. JAMA 242:2193–2196
Peek GJ, Tirouvopaiti R, Firmin RK (2005) ECLS for adult respiratory failure: etiology and indications. In: Van Meurs K, Lally KP, Peek G, Zwischenberger JB (eds) ECMO Extracorporeal Cardiopulmonary Support in Critical Care, 3rd edn. Extracorporeal Life Support Organization, Ann Arbor, pp 393–402
Gattinoni L, Pesenti A, Mascheroni D, Marcolin R, Fumagalli R, Rossi F, Iapichino G, Romagnoli G, Uziel L, Agostoni A, Koblow T, Damia G (1986) Low-frequency positive-pressure ventilation with extracorporeal CO2 removal in severe acute respiratory failure. JAMA 256:881–886
Morris AH, Wallace CJ, Menlove RL, Clemmer TP, Orme JF Jr, Weaver LK, Dean NC, Thomas F, East TD, Pace NL, Suchyta MR, Beck E, Bombino M, Sittig DF, Bohm S, Hoffman B, Becks H, Butler S, Pearl J, Rasmusson B (1994) Randomized clinical trial of pressure-controlled inverse ratio ventilation and extracorporeal CO2 removal for adult respiratory distress syndrome. Am J Respir Crit Care Med 149:295–305
Bartlett RH, Roloff DW, Cornell RG, Andrews AF, Dillon PW, Zwischenberger JB (1985) Extracorporeal circulation in neonatal respiratory failure: a prospective randomized study. Pediatrics 76:479–487
O’Rourke PP, Crone RK, Vacanti JP, Ware JH, Lillehei CW, Parad RB, Epstein MF (1989) Extracorporeal membrane oxygenation and conventional medical therapy in neonates with persistent pulmonary hypertension of the newborn: a prospective randomized study. Pediatrics 84:957–963
UK Collaborative ECMO Trial Group (1996) UK Collaborative randomised trial of neonatal extracorporeal membrane oxygenation. Lancet 348:75–82
Green TP, Timmons OD, Fackler JC, Moler FW, Thompson AE, Sweeney MF (1996) The impact of extracorporeal membrane oxygenation on survival in pediatric patients with acute respiratory failure. Pediatric Critical Care Study Group. Crit Care Med 24:323–332
Anderson HL 3rd, Delius RE, Sinard JM, McCurry KR, Shanley CJ, Chapman RA, Shapiro MB, Rodriquez JL, Bartlett RH (1992) Early experience with adult extracorporeal membrane oxygenation in the modern era. Ann Thorac Surg 53:553–563
Kolla S, Awad SS, Rich PB, Schreiner RJ, Hirschl RB, Bartlett RH (1997) Extracorporeal life support for 100 adult patients with severe respiratory failure. Ann Surg 226:544–564
Linden V, Palmer K, Reinhard J, Westman R, Ehren H, Granholm T, Freckner B (2000) High Survival in adult patients with acute respiratory distress syndrome treated by extracorporeal membrane oxygenation, minimal sedation, and pressure supported ventilation. Intensive Care Med 26:1630–1637
Bartlett RH, Roloff DW, Custer JR, Younger JG, Hirschl RB (2000) Extracorporeal life support. The University of Michigan experience. JAMA 283:904–908
Hemmila MR, Rowe SA, Boules TN, Miskulin J, McGillicuddy JW, Schuerer DJ, Haft JW, Swaniker F, Arbabi S, Hirschl RB, Bartlett RH (2004) Extracorporeal life support for severe acute respiratory distress syndrome in adults. Ann Surg 240:595–607
Beiderlinden M, Eikermann M, Boes T, Breitfeld C, Peters J (2006) Treatment of severe acute respiratory distress syndrome: role of extracorporeal gas exchange. Intensive Care Med 32:1627–1631
Peek GJ, Moore HM, Moore N, Sosnowski AW, Firmin RK (1997) Extracorporeal membrane oxygenation for adult respiratory failure. Chest 112:759–764
Pranikoff T, Hirschl RB, Steimle CN, Anderson HL 3rd, Bartlett RH (1997) Mortality is directly related to the duration of mechanical ventilation before the initiation of extracorporeal life support for severe respiratory failure. Crit Care Med 25:28–32
Lewandowski K, Rossaint R, Pappert D, Gerlach H, Slama KJ, Weidermann H, Frey DJ, Hoffmann O, Keske U, Falke KJ (1997) High survival rate in 122 ARDS patients managed according to a clinical algorithm including extracorporeal membrane oxygenation. Intensive Care Med 23:803–805
Frenckner B, Palmer P, Linden V (2002) Extracorporeal respiratory support and minimally invasive ventilation in severe ARDS. Minerva Anestesiol 68:381–386
Peek GJ, Clemens F, Elbourne D, Firmin R, Hardy P, Hibbert C, Killer H, Mugford M, Thalanany M, Tiruvoipati R, Truesdale A, Wilson A (2006) CESAR: conventional ventilatory support vs extracorporeal membrane oxygenation for severe adult respiratory failure. BMC Health Serv Res 6:163
Peek G (2008) The CESAR Trial: conventional ventilatory support versus extracorporeal membrane oxygenation for severe adult respiratory failure. Society of critical care medicine 37th critical care congress. Honolulu Hawaii. Society of critical care medicine. February 2, 2008
Cengiz P, Seidel K, Rycus PT, Brogan TV, Roberts JS (2005) Central nervous system complications during pediatric extracorporeal life support: incidence and risk factors. Crit Care Med 33:2817–2824
Jardin F, Vieillard-Baron A (2007) Is there a safe plateau pressure in ARDS? The right heart knows. Intensive Care Med 33:444–447
Toomasian JM, Snedecor SM, Cornell RG, Cilley RE, Bartlett RH (1988) National experience with extracorporeal membrane oxygenation for newborn respiratory failure. Data from 715 cases. ASAIO Trans 34:140–147
O’Malley KJ, Cook KF, Price MD, Wildes KR, Hurdle JF, Ashton CM (2005) Measuring diagnoses: ICD code accuracy. Health Serv Res 40:1620–1639
Acknowledgments
Peter Rycus is employed by The Extracorporeal Life Support Organization. There are no other disclosures
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Brogan, T.V., Thiagarajan, R.R., Rycus, P.T. et al. Extracorporeal membrane oxygenation in adults with severe respiratory failure: a multi-center database. Intensive Care Med 35, 2105–2114 (2009). https://doi.org/10.1007/s00134-009-1661-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-009-1661-7