Abstract
Purpose
The high prevalence of alcohol use disorder among individuals with a history of trauma and posttraumatic stress disorder is well documented. The current study applied network analysis to map the structure of symptom associations between these disorders.
Methods
Data come from a community sample of 449 Australian adults with a history of trauma and alcohol consumption during the last 12 months. Data analysis consisted of the construction of the comorbidity network of PTSD/AUD symptoms, identification of the bridging symptoms, computation of the centrality measures, and evaluation of the robustness of the results.
Results
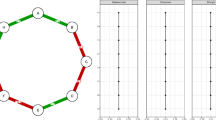
Results highlighted two main symptom clusters, corresponding to two disorders, and that only nine edges connected the two clusters. Bridging symptoms connecting the two clusters were: alcohol use in dangerous situations, physical or mental health problems as a result of alcohol use, loss of interest or reduced social activities, and reckless/self-destructive behaviour.
Conclusions
Identification of both central symptoms, because of their key role in the constellation and strong associations with majority of symptoms, and bridge symptoms, because of their mediating role between two disorders, has some implications in terms of self-medication and risk-taking/self-regulation theories of comorbidity and provides a number of clinical implications, which warrants further exploration within clinical samples.



Similar content being viewed by others
References
Kessler RC, Chiu WT, Demler O et al (2005) Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the National Comorbidity Survey replication. Arch Gen Psychiatry 62:617–627. doi:10.1001/archpsyc.62.6.617
Reynolds M, Mezey G, Chapman M et al (2005) Co-morbid post-traumatic stress disorder in a substance misusing clinical population. Drug Alcohol Depend 77:251–258. doi:10.1016/j.drugalcdep.2004.08.017
Danielson CK, Amstadter AB, Dangelmaier RE et al (2009) Trauma-related risk factors for substance abuse among male versus female young adults. Addict Behav 34:395–399. doi:10.1016/j.addbeh.2008.11.009
Santiago PO, Wilk JE, Milliken CS et al (2010) Screening for alcohol misuse and alcohol- related behaviors among combat veterans. Psychiatr Serv 61:575–581
Breslau N, Davis GC, Schultz LR (2003) Posttraumatic stress disorder and the incidence of nicotine, alcohol, and other drug disorders in persons who have experienced trauma. Arch Gen Psychiatry 60:289–294. doi:10.1001/archpsyc.60.3.289
Mills KL, Teesson M, Ross J, Peters L (2006) Trauma, PTSD, and substance use disorders: findings from the Australian National Survey of Mental Health and Well-Being. Am J Psychiatry 163:652–658. doi:10.1176/appi.ajp.163.4.652
Pietrzak RH, Goldstein RB, Southwick SM, Grant BF (2011) Prevalence and axis I comorbidity of full and partial posttraumatic stress disorder in the United States: results from Wave 2 of the National Epidemiologic Survey on alcohol and related conditions. J Anxiety Disord 25:456–465. doi:10.1016/j.janxdis.2010.11.010
McCauley JL, Killeen T, Gros DF et al (2012) Posttraumatic stress disorder and co-occurring substance use disorders: advances in assessment and treatment. Clin Psychol Sci Pract 19:283–304. doi:10.1111/cpsp.12006
Ouimette P, Moos RH, Finney JW (2003) PTSD treatment and 5-year remission among patients with substance use and posttraumatic stress disorders. J Consult Clin Psychol 71:410–414. doi:10.1037/0022-006x.71.2.410
Riggs DS, Rukstalis M, Volpicelli JR et al (2003) Demographic and social adjustment characteristics of patients with comorbid posttraumatic stress disorder and alcohol dependence: potential pitfalls to PTSD treatment. Addict Behav 28:1717–1730. doi:10.1016/j.addbeh.2003.08.044
Evren C, Sar V, Dalbudak E et al (2011) Lifetime PTSD and quality of life among alcohol-dependent men: impact of childhood emotional abuse and dissociation. Psychiatry Res 186:85–90. doi:10.1016/j.psychres.2010.07.004
Evren C, Dalbudak E, Evren B et al (2011) Self-mutilative behaviours in male alcohol-dependent inpatients and relationship with posttraumatic stress disorder. Psychiatry Res 186:91–96. doi:10.1016/j.psychres.2010.07.045
Reed PL, Anthony JC, Breslau N (2007) Incidence of drug problems in young adults exposed to trauma and posttraumatic stress disorder: do early life experiences and predispositions matter? Arch Gen Psychiatry 64:1435–1442. doi:10.1001/archpsyc.64.12.1435
Saladin ME, Brady KT, Dansky BS, Kilpatrick DG (1995) Understanding comorbidity between PTSD and substance use disorders: two preliminary investigations. Addict Behav 20:643–655. doi:10.1016/0306-4603(95)00024-7
Jacobsen LK, Southwick SM, Kosten TR (2001) Substance use disorders in patients with posttraumatic stress disorder: a review of the literature. Am J Psychiatry 158:1184–1190. doi:10.1176/appi.ajp.158.8.1184
Back SE, Sonne SC, Killeen T et al (2003) Comparative profiles of women with Ptsd and comorbid cocaine or alcohol dependence. Am J Drug Alcohol Abuse 29:169–189. doi:10.1081/ADA-120018845
Stewart SH, Conrod PJ, Pihl RO, Dongier M (1999) Relations between posttraumatic stress symptom dimensions and substance dependence in a community-recruited sample of substance-abusing women. Psychol Addict Behav 13:78–88. doi:10.1037/0893-164X.13.2.78
Stewart SH, Pihl RO, Conrod PJ, Dongier M (1998) Functional associations among trauma, PTSD, and substance-related disorders. Addict Behav 23:797–812. doi:10.1016/S0306-4603(98)00070-7
Chilcoat HD, Breslau N (1998) Investigations of causal pathways between PTSD and drug use disorders. Addict Behav 23:827–840. doi:10.1016/S0306-4603(98)00069-0
Stewart SH, Conrod PJ, Samoluk SB et al (2000) Posttraumatic stress disorder symptoms and situation-specific drinking in women substance abusers. Alcohol Treat Q 18:31–47. doi:10.1300/J020v18n03_04
Borsboom D, Cramer AOJ (2013) Network analysis: an integrative approach to the structure of psychopathology. Annu Rev Clin Psychol 9:91–121. doi:10.1146/annurev-clinpsy-050212-185608
Fried EI, van Borkulo CD, Cramer AOJ et al (2016) Mental disorders as networks of problems: a review of recent insights. Soc Psychiatry Psychiatr Epidemiol. doi:10.1007/s00127-016-1319-z (in press)
Boschloo L, van Borkulo CD, Rhemtulla M et al (2015) The network structure of symptoms of the diagnostic and statistical manual of mental disorders. PLoS One 10:e0137621. doi:10.1371/journal.pone.0137621
Tio P, Epskamp S, Noordhof A, Borsboom D (2016) Mapping the manuals of madness: comparing the ICD-10 and DSM-IV-TR using a network approach. Int J Methods Psychiatr Res 25:267–276. doi:10.1002/mpr.1503
Fried EI, Epskamp S, Nesse RM et al (2016) What are “good” depression symptoms? Comparing the centrality of DSM and non-DSM symptoms of depression in a network analysis. J Affect Disord 189:314–320. doi:10.1016/j.jad.2015.09.005
Bringmann LF, Vissers N, Wichers M et al (2013) A network approach to psychopathology: new insights into clinical longitudinal data. PLoS One. doi:10.1371/journal.pone.0060188
McNally RJ, Robinaugh DJ, Wu GWY et al (2015) Mental disorders as causal systems: a network approach to posttraumatic stress disorder. Clin Psychol Sci 3:836–849. doi:10.1177/2167702614553230
Ruzzano L, Borsboom D, Geurts HM (2015) Repetitive behaviors in autism and obsessive-compulsive disorder: new perspectives from a network analysis. J Autism Dev Disord 45:192–202. doi:10.1007/s10803-014-2204-9
Afzali MH, Sunderland M, Teesson M et al (2016) A network approach to the comorbidity between posttraumatic stress disorder and major depressive disorder: the role of overlapping symptoms. J Affect Disord. doi:10.1016/j.jad.2016.10.037
Cramer AOJ, Waldorp LJ, van der Maas HLJ, Borsboom D (2010) Comorbidity: a network perspective. Behav Brain Sci 33:137-50-93. doi:10.1017/S0140525X09991567
Borsboom D, Epskamp S, Kievit RA et al (2011) Transdiagnostic Networks: commentary on Nolen-Hoeksema and Watkins. Perspect Psychol Sci 6:610–614. doi:10.1177/1745691611425012
Beard C, Millner AJ, Forgeard MJC et al (2016) Network analysis of depression and anxiety symptoms. Psychol Med 46:3359–3369. doi:10.1017/S0033291716002300
Calear AL, Ph D, Mackinnon AJ et al (2015) The Distress Questionnaire-5: population screener for psychological distress was more accurate than the K6/K10. J Clin Epidemiol 71:35–42. doi:10.1016/j.jclinepi.2015.10.005
Thornton L, Batterham PJ, Fassnacht DB et al (2016) Recruiting for health, medical or psychosocial research using Facebook: systematic review. Internet Interv 4:72–81. doi:10.1016/j.invent.2016.02.001
Epskamp S, Maris G, Waldorp LJ, Borsboom D (2016) Network Psychometrics. In: Irwing P, Hughes D, Booth T (eds) Handbook of psychometrics. Wiley, New York (in press)
van Borkulo CD, Borsboom D, Epskamp S et al (2014) A new method for constructing networks from binary data. Sci Rep 4:5918. doi:10.1038/srep05918
Epskamp S, Cramer AOJ, Waldorp LJ et al (2012) qgraph: network visualizations of relationships in psychometric data. J Stat Softw 48:1–18. doi:10.18637/jss.v048.i04
Fruchterman TMJ, Reingold EM (1991) Graph drawing by force-directed placement. Softw-Pract Exp 21:1129–1164. doi:10.1002/spe.4380211102
Costantini G, Epskamp S, Borsboom D et al (2015) State of the aRt personality research: a tutorial on network analysis of personality data in R. J Res Pers 54:13–29. doi:10.1016/j.jrp.2014.07.003
Epskamp S, Borsboom D, Fried EI (2016) Estimating psychological networks and their accuracy: a tutorial paper. 1–14 (arXiv:1604.08462)
Hawthorne G, Osborne R (2005) Population norms and meaningful differences for the assessment of quality of life (AQoL) measure. Aust N Z J Public Health 29:136–142
Hawthorne G, Korn S, Richardson J (2013) Population norms for the AQoL derived from the 2007 Australian National Survey of Mental Health and Wellbeing. Aust N Z J Public Health 37:7–16. doi:10.1111/1753-6405.12004
Slade T, Johnston A, Oakley Browne MA et al (2009) 2007 National Survey of Mental Health and Wellbeing: methods and key findings. Aust N Z J Psychiatry 43:594–605. doi:10.1080/00048670902970882
Kaysen D, Simpson T, Dillworth T et al (2006) Alcohol problems and posttraumatic stress disorder in female crime victims. J Trauma Stress 19:399–403. doi:10.1002/jts.20122
Rosen GM, Spitzer RL, McHugh PR (2008) Problems with the post-traumatic stress disorder diagnosis and its future in DSM V. Br J Psychiatry 192:3–4. doi:10.1192/bjp.bp.107.043083
Gros DF, Price M, Magruder KM, Frueh BC (2012) Symptom overlap in posttraumatic stress disorder and major depression. Psychiatry Res 196:267–270. doi:10.1016/j.psychres.2011.10.022
Elhai JD, de Francisco Carvalho L, Miguel FK et al (2011) Testing whether posttraumatic stress disorder and major depressive disorder are similar or unique constructs. J Anxiety Disord 25:404–410. doi:10.1016/j.janxdis.2010.11.003
Blanco C, Xu Y, Brady KT et al (2013) Comorbidity of posttraumatic stress disorder with alcohol dependence among US adults: results from national epidemiological survey on alcohol and related conditions. Drug Alcohol Depend 132:630–638. doi:10.1016/j.drugalcdep.2013.04.016
Chilcoat HD, Breslau N (1998) Posttraumatic stress disorder and drug disorders: testing causal pathways. Arch Gen Psychiatry 55:913–917. doi:10.1001/archpsyc.55.10.913
Acierno R, Resnick H, Kilpatrick DG et al (1999) Risk factors for rape, physical assault, and posttraumatic stress disorder in women: examination of differential multivariate relationships. J Anxiety Disord 13:541–563. doi:10.1016/S0887-6185(99)00030-4
Yuan NP, Koss MP, Polacca M, Goldman D (2006) Risk factors for physical assault and rape among six native american tribes. J Interpers Violence 21:1566–1590. doi:10.1177/0886260506294239
Amstadter AB, Elwood LS, Begle AM et al (2011) Predictors of physical assault victimization: findings from the National Survey of Adolescents. Addict Behav 36:814–820. doi:10.1016/j.addbeh.2011.03.008
McNally RJ (2016) Can network analysis transform psychopathology? Behav Res Ther. doi:10.1016/j.brat.2016.06.006
Carragher N, Sunderland M, Batterham PJ et al (2016) Discriminant validity and gender differences in DSM-5 posttraumatic stress disorder symptoms. J Affect Disord 190:56–67. doi:10.1016/j.jad.2015.09.071
Rhemtulla M, Fried EI, Aggen SH et al (2016) Network analysis of substance abuse and dependence symptoms. Drug Alcohol Depend 161:230–237. doi:10.1016/j.drugalcdep.2016.02.005
Bringmann LF, Lemmens LHJM, Huibers MJH et al (2015) Revealing the dynamic network structure of the Beck Depression Inventory-II. Psychol Med 45:747–757. doi:10.1017/S0033291714001809
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics statement
Data were collected using a computerized testing; the statutory body responsible for conducting such surveys provided ethical protocols that include written informed consent.
Conflict of interest
The authors have not transmitted any conflict of interest.
Role of funding source
This project was funded by the Endeavour research fellowship granted by department of education and training—Australian Government. The sponsor had no role in study design, data collection, analysis, interpretation of results, report writing, or manuscript submission.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Afzali, M.H., Sunderland, M., Batterham, P.J. et al. Network approach to the symptom-level association between alcohol use disorder and posttraumatic stress disorder. Soc Psychiatry Psychiatr Epidemiol 52, 329–339 (2017). https://doi.org/10.1007/s00127-016-1331-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-016-1331-3