Abstract
Purpose
Women who face pregnancy complications may require hospitalization in a high-risk pregnancy unit (HRPU), and this may have a negative impact on the pregnant woman’s mental health. The purpose of this study was to screen for depressive symptoms in pregnant women admitted in a high-risk pregnancy unit and also to investigate associated risk factors.
Methods
This was a cross-sectional study that enrolled pregnant women admitted at ≥24 gestational weeks in a university hospital HRPU, between September 2014 and November 2015. The Edinburgh Postnatal Depression Scale was used to assess depressive symptoms on admission. A cutoff score ≥13 was considered as indicative of depression. Test results were then correlated with the reasons that led to the women’s admission as well as socio-demographic characteristics.
Results
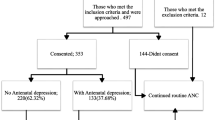
Overall, 157 of the women admitted in the HRPU during the study period were eligible for the study and agreed to complete the questionnaire. The mean age of the pregnant women was 30 ± 6 years, and the mean gestational week at admission was 32 ± 3 weeks. The prevalence of antenatal depression (score ≥13) was 28 % (44/157). In the multivariate analysis, antenatal depression was significantly correlated with smoking (OR = 2.681, 95 % CI 1.089–6.601) and the existence of thoughts for pregnancy termination (OR = 3.624, 95 % CI 1.149–11.427).
Conclusions
Approximately one quarter of pregnant women hospitalized in the HRPU may show signs of depression at the time of admission. Smoking and an unwanted pregnancy were found to be independently associated with antenatal depression, whereas no association was found with any obstetric parameters.
Similar content being viewed by others
References
Bennett HA, Einarson A, Taddio A, Koren G, Einarson TR (2004) Prevalence of depression during pregnancy: systematic review. Obstet Gynecol 103:698–709. doi:10.1097/01.AOG.0000116689.75396.5f
Evans J, Heron J, Francomb H, Oke S, Golding J (2001) Cohort study of depressed mood during pregnancy and after childbirth. BMJ 323:257–260
Adouard F, Glangeaud-Freudenthal NM, Golse B (2005) Validation of the Edinburgh postnatal depression scale (EPDS) in a sample of women with high-risk pregnancies in France. Arch Womens Ment Health 8:89–95. doi:10.1007/s00737-005-0077-9
Brandon AR, Trivedi MH, Hynan LS, Miltenberger PD, Labat DB, Rifkin JB, Stringer CA (2008) Prenatal depression in women hospitalized for obstetric risk. J Clin Psychiatry 69:635–643
Powers PS, Johnson T, Knuppel R, Cupoli JM, Achenbach KE (1986) Psychiatric disorders in high-risk pregnancy. Compr Psychiatry 27:159–164
King NM, Chambers J, O’Donnell K, Jayaweera SR, Williamson C, Glover VA (2010) Anxiety, depression and saliva cortisol in women with a medical disorder during pregnancy. Arch Womens Ment Health 13:339–345. doi:10.1007/s00737-009-0139-5
Zuckerman B, Amaro H, Bauchner H, Cabral H (1989) Depressive symptoms during pregnancy: relationship to poor health behaviors. Am J Obstet Gynecol 160:1107–1111
Alder J, Fink N, Bitzer J, Hosli I, Holzgreve W (2007) Depression and anxiety during pregnancy: a risk factor for obstetric, fetal and neonatal outcome? A critical review of the literature. J Matern Fetal Neonatal Med 20:189–209. doi:10.1080/14767050701209560
Grote NK, Bridge JA, Gavin AR, Melville JL, Iyengar S, Katon WJ (2010) A meta-analysis of depression during pregnancy and the risk of preterm birth, low birth weight, and intrauterine growth restriction. Arch Gen Psychiatry 67:1012–1024. doi:10.1001/archgenpsychiatry.2010.111
Van den Bergh BR, Mulder EJ, Mennes M, Glover V (2005) Antenatal maternal anxiety and stress and the neurobehavioural development of the fetus and child: links and possible mechanisms. A review. Neurosci Biobehav Rev 29:237–258. doi:10.1016/j.neubiorev.2004.10.007
Pearson RM, Bornstein MH, Cordero M, Scerif G, Mahedy L, Evans J, Abioye A, Stein A (2015) Maternal perinatal mental health and offspring academic achievement at age 16: the mediating role of childhood executive function. J Child Psychol Psychiatry. doi:10.1111/jcpp.12483
Logsdon MC, Wisner KL, Pinto-Foltz MD (2006) The impact of postpartum depression on mothering. J Obstet Gynecol Neonatal Nurs 35:652–658. doi:10.1111/j.1552-6909.2006.00087.x
Austin MP (2004) Antenatal screening and early intervention for “perinatal” distress, depression and anxiety: where to from here? Arch Womens Ment Health 7:1–6. doi:10.1007/s00737-003-0034-4
Gotlib IH, Whiffen VE, Mount JH, Milne K, Cordy NI (1989) Prevalence rates and demographic characteristics associated with depression in pregnancy and the postpartum. J Consult Clin Psychol 57:269–274
Koutra K, Vassilaki M, Georgiou V, Koutis A, Bitsios P, Chatzi L, Kogevinas M (2014) Antenatal maternal mental health as determinant of postpartum depression in a population based mother-child cohort (Rhea Study) in Crete, Greece. Soc Psychiatry Psychiatr Epidemiol 49:711–721. doi:10.1007/s00127-013-0758-z
Field T, Diego M, Hernandez-Reif M, Figueiredo B, Deeds O, Ascencio A, Schanberg S, Kuhn C (2010) Comorbid depression and anxiety effects on pregnancy and neonatal outcome. Infant Behav Dev 33:23–29. doi:10.1016/j.infbeh.2009.10.004
The American College of Obstetricians and Gynecologists (2015) Screening for Perinatal Depression. Committee Opinion Number 630
Littleton HL, Breitkopf CR, Berenson AB (2007) Correlates of anxiety symptoms during pregnancy and association with perinatal outcomes: a meta-analysis. Am J Obstet Gynecol 196:424–432. doi:10.1016/j.ajog.2007.03.042
Heaman M (1992) Stressful life events, social support, and mood disturbance in hospitalized and non-hospitalized women with pregnancy-induced hypertension. Can J Nurs Res 24:23–37
Tsai SJ, Lee YC, Yang CH, Sim CB (1996) Psychiatric consultations in obstetric inpatients. J Obstet Gynaecol Res 22:603–607
Cox JL, Holden JM, Sagovsky R (1987) Detection of postnatal depression. Development of the 10-item Edinburgh postnatal depression scale. Br J Psychiatry 150:782–786
Murray L, Carothers AD (1990) The validation of the Edinburgh post-natal depression scale on a community sample. Br J Psychiatry 157:288–290
Leonardou AAZY, Papageorgiou CC, Marks MN, Tsartsara EC, Antsaklis A, Christodoulou GN, Soldatos CR (2009) Validation of the Edinburgh postnatal depression scale and prevalence of postnatal depression at 2 months postpartum in a sample of Greek mothers. J Reprod Infant Psyc 27(1):28–39
Vivilaki VG, Dafermos V, Kogevinas M, Bitsios P, Lionis C (2009) The Edinburgh postnatal depression scale: translation and validation for a Greek sample. BMC Public Health 9:329. doi:10.1186/1471-2458-9-329
Brouwers EP, van Baar AL, Pop VJ (2001) Does the Edinburgh postnatal depression scale measure anxiety? J Psychosom Res 51:659–663
Gibson J, McKenzie-McHarg K, Shakespeare J, Price J, Gray R (2009) A systematic review of studies validating the Edinburgh postnatal depression scale in antepartum and postpartum women. Acta Psychiatr Scand 119:350–364. doi:10.1111/j.1600-0447.2009.01363.x
Thiagayson P, Krishnaswamy G, Lim ML, Sung SC, Haley CL, Fung DS, Allen JC Jr, Chen H (2013) Depression and anxiety in Singaporean high-risk pregnancies–prevalence and screening. Gen Hosp Psychiatry 35:112–116. doi:10.1016/j.genhosppsych.2012.11.006
Fishell A (2010) Depression and anxiety in pregnancy. J Popul Ther Clin Pharmacol 17:e363–e369
Pearlstein T (2008) Perinatal depression: treatment options and dilemmas. J Psychiatry Neurosci 33:302–318
Redshaw M, Henderson J (2013) From antenatal to postnatal depression: associated factors and mitigating influences. J Womens Health (Larchmt) 22:518–525. doi:10.1089/jwh.2012.4152
Hickey CA, Cliver SP, Goldenberg RL, McNeal SF, Hoffman HJ (1995) Relationship of psychosocial status to low prenatal weight gain among nonobese black and white women delivering at term. Obstet Gynecol 86:177–183
Silva RA, Jansen K, Souza LD, Moraes IG, Tomasi E, Silva Gdel G, Dias Mde S, Pinheiro RT (2010) Depression during pregnancy in the Brazilian public health care system. Rev Bras Psiquiatr 32:139–144
Kitamura T, Yoshida K, Okano T, Kinoshita K, Hayashi M, Toyoda N, Ito M, Kudo N, Tada K, Kanazawa K, Sakumoto K, Satoh S, Furukawa T, Nakano H (2006) Multicentre prospective study of perinatal depression in Japan: incidence and correlates of antenatal and postnatal depression. Arch Womens Ment Health 9:121–130. doi:10.1007/s00737-006-0122-3
Abajobir AA, Maravilla JC, Alati R, Najman JM (2016) A systematic review and meta-analysis of the association between unintended pregnancy and perinatal depression. J Affect Disord 192:56–63. doi:10.1016/j.jad.2015.12.008
Moraes IG, Pinheiro RT, Silva RA, Horta BL, Sousa PL, Faria AD (2006) Prevalence of postpartum depression and associated factors. Rev Saude Publica 40:65–70
Luger TM, Suls J, Vander Weg MW (2014) How robust is the association between smoking and depression in adults? A meta-analysis using linear mixed-effects models. Addict Behav 39:1418–1429. doi:10.1016/j.addbeh.2014.05.01
Smedberg J, Lupattelli A, Mardby AC, Overland S, Nordeng H (2015) The relationship between maternal depression and smoking cessation during pregnancy–a cross-sectional study of pregnant women from 15 European countries. Arch Womens Ment Health 18:73–84. doi:10.1007/s00737-014-0470-3
Goodwin RD, Keyes K, Simuro N (2007) Mental disorders and nicotine dependence among pregnant women in the United States. Obstet Gynecol 109:875–883
Orr ST, Blazer DG, Orr CA (2012) Maternal prenatal depressive symptoms, nicotine addiction, and smoking-related knowledge, attitudes, beliefs, and behaviors. Matern Child Health J 16:973–978. doi:10.1007/s10995-011-0822-9
Linares Scott TJ, Heil SH, Higgins ST, Badger GJ, Bernstein IM (2009) Depressive symptoms predict smoking status among pregnant women. Addict Behav 34:705–708. doi:10.1016/j.addbeh.2009.04.003
Dayan J, Creveuil C, Dreyfus M, Herlicoviez M, Baleyte JM, O’Keane V (2010) Developmental model of depression applied to prenatal depression: role of present and past life events, past emotional disorders and pregnancy stress. PLoS One 5:e12942. doi:10.1371/journal.pone.0012942
Johanson R, Chapman G, Murray D, Johnson I, Cox J (2000) The North Staffordshire Maternity Hospital prospective study of pregnancy-associated depression. J Psychosom Obstet Gynaecol 21:93–97
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Dagklis, T., Papazisis, G., Tsakiridis, I. et al. Prevalence of antenatal depression and associated factors among pregnant women hospitalized in a high-risk pregnancy unit in Greece. Soc Psychiatry Psychiatr Epidemiol 51, 1025–1031 (2016). https://doi.org/10.1007/s00127-016-1230-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-016-1230-7