Abstract
Aims/hypothesis
The secretory function of pancreatic beta cells is synergistically stimulated by two signalling pathways which mediate the effects of nutrients and hormones such as glucagon-like peptide 1 (GLP-1), glucose-dependent insulinotropic peptide (GIP) or glucagon. These hormones are known to activate adenylyl cyclase in beta cells. We examined the type of adenylyl cyclase that is associated with this synergistic interaction.
Methods
Insulin release, cAMP production, adenylyl cyclase activity, mRNA and protein expression were measured in fluorescence-activated cell sorter-purified rat beta cells and in the rat beta-cell lines RINm5F, INS-1 832/13 and INS-1 832/2.
Results
In primary beta cells, glucagon and GLP-1 synergistically potentiate the stimulatory effect of 20 mmol/l glucose on insulin release and cAMP production. Both effects are abrogated in the presence of the L-type Ca2+-channel blocker verapamil. The cAMP-producing activity of adenylyl cyclase in membranes from RINm5F cells is synergistically increased by Ca2+-calmodulin and recombinant GTPγS-activated Gsα-protein subunits. This type of regulation is characteristic for type I and type VIII AC isoforms. Consistent with this functional data, AC mRNA analysis shows abundant expression of type VI AC, four splice variants of type VIII AC and low expression level of type I AC in beta cells. Type VIII AC expression at the protein level was observed using immunoblots of RINm5F cell extracts.
Conclusion/interpretation
This study identifies type VIII AC in insulin-secreting cells as one of the potential molecular targets for synergism between GLP-1 receptor mediated and glucose-mediated signalling.
Similar content being viewed by others
We have shown previously that a synergism exists between nutrient signals and cellular cAMP concentrations in the stimulation of insulin release [1]. Stimulation of beta cells with nutrients alone elicits only a partial secretory response that can be potentiated by adding glucagon or other agents which raise intracellular cAMP [2, 3]. In contrast, glucose alone cannot increase cAMP concentration in beta cells, but the sugar has a modest effect on glucagon-induced cAMP production [4]. Subsequent work has shown that glucagon-like peptide 1 (GLP-1) is also a potent stimulus for insulin release that is fully dependent on the presence of glucose [5]. Glucose elicits its best known molecular actions on beta cells via cellular uptake and mitochondrial metabolism, increased ATP to ADP ratios, closure of K+ ATP -channels and calcium influx via L-type Ca2+-channels [6, 7, 8]. A less well characterised pathway occurs independently of the closure of K+ ATP channels [9, 10, 11]. Pharmacological activation of the cAMP signalling pathway can be achieved by various means such as cAMP analogues [2], stimulators of adenylyl cyclase (AC) such as forskolin [12], phosphodiesterase (PDE) inhibitors such as methylxanthines [13], and peptides that stimulate protein kinase A (PKA) [14]. Effects are partially mediated via PKA activation [15], requiring subcellular concentration of the kinase in signalling complexes [16]. Recent evidence suggests that another part of cAMP signalling in beta cells is mediated via the cAMP-binding protein GEFII (Epac2) complexed with Rim2 and Rab3 [17, 18]. Two important physiological stimulators of cAMP production in beta cells are glucose-dependent insulinotropic peptide (GIP) and GLP-1 [19]. Their physiological relevance in the incretin response of the gut on glucose-induced insulin secretion has been underlined by mouse models that have targeted disruption of the corresponding receptor genes [20, 21, 22]. Glucagon also increases cAMP in isolated beta cells [13, 19, 23], and can act as a paracrine stimulator of beta cells. At supraphysiological concentrations, it is able to potentiate glucose-induced insulin release from isolated beta cells [2] as well as in vivo [24]. However, the physiological relevance of glucagon-stimulated cAMP in the beta cell is uncertain, as locally released peptide did not activate beta cell function in the intact perfused rat pancreas [25].
A molecular pathway of synergistic crosstalk between glucose and GLP-1 involves an increase of cytosolic Ca2+, as has recently been illustrated at the transcription factor NFAT (nuclear factor of activated T-cells), which strongly promotes the transcription of the insulin gene [26]. Transcriptional activation increases markedly when the protein is dephosphorylated by calcineurin (PP2B), a Ca2+-calmodulin-dependent protein phosphatase. Both glucose and GLP-1 contributed to the rise in cellular calcium required for transcriptional activation [27]. A second illustration of the concept of synergism is that PP2B and PKA are co-localized in the beta cell in signalling complexes that are anchored by the scaffolding protein AKAP79/150 [16], an organisation proposed to be relevant for exocytosis. We provide another molecular site of interaction between glucose-and GLP-1 signalling by showing that beta cells express type VIII AC, an isoform that is synergistically activated by Ca2+/calmodulin and Gsα.
Materials and methods
Preparation of tissues and cells and culture of beta cells
All studies involving animal cells or tissues were carried out according to the Belgian regulation of animal welfare and after approval by the institution's commission for animal experiments. Control tissues (brain, liver and lung) were dissected from male Wistar rats (±3 months old) washed in phosphate-buffered saline, frozen in liquid nitrogen and stored at −80°C before adenylyl cyclase (AC) expression analysis. Purified rat alpha cells and beta cells were obtained as described [28] from male Wistar rat pancreata. Purity of beta cells (>97%) and alpha cells (>95%) was analysed by immunocytochemistry and electron microscopy. Culture of purified beta cells started by 2-h reaggregation at 37°C in a rotary shaking incubator (95%O2/5%CO2; Braun, Melsungen, Germany), followed by 16-h static incubation in suspension cultured dishes (Nunc, Roskilde, Denmark) in Ham's F10 medium (Gibco BRL, Grand Island, N.Y., USA) supplemented with 2 mmol/l glutamine, 10 mmol/l glucose (Merck, Darmstadt, Germany), 1% charcoal treated type V bovine serum albumin (BSA; Boehringer Mannheim, Germany), 0.075 g/l penicillin (Sigma, St Louis, Mo., USA), and 0.1 g/l streptomycin (Sigma). The rat insulinoma cell line RINm5F was grown as confluent cultures in RPMI-1640 medium with L-glutamax (Gibco BRL) supplemented with 10% (v/v) fetal calf serum (Life Technologies, Paisley, UK), 0.1 mg/ml streptomycin, and 0.075 mg/ml penicillin, using plastic culture flasks (Falcon, Becton Dickinson). The medium was changed every 2 days and the cells were detached by 5-min incubation at 37°C in phosphate-buffered saline, 1 mmol/l EDTA and 0.5% BSA. The clonal cell lines INS-1 832/13 and 832/2 (obtained from C.B. Newgard, Duke University, Durham, N.C., USA) expressing human insulin and being, respectively, strongly and weakly responsive to glucose [29] were cultured as RINm5F cells, except that INS-1 cell growth medium was additionally supplemented with 10 mmol/l HEPES, 50 µmol/l beta-mercaptoethanol, 2 mmol/l glutamine and 1 mmol/l pyruvate, as described previously [29]. The viability of the primary and tumoral beta cells was estimated by neutral red uptake [28] and was routinely above 90%.
Analysis of cAMP production in purified pancreatic beta cells
Cellular cAMP content from pancreatic beta cells was measured during static incubations as described before [13] using 5×104 cells per sample. Unless stated otherwise, the PDE inhibitors 3-isobutyl-1-methylxanthine (IBMX; Aldrich-Janssen Chimica, Beerse, Belgium) or Ro 20-1724 (Roche, Basel, Switzerland) were added to prevent cAMP breakdown. The L-type Ca2+-channel blocker verapamil was purchased from Knoll (Brussels, Belgium). The cellular cAMP content was measured after sonication of the cell pellets in 8% trichloroacetic acid and ether extraction. Samples were lyophilized and acetylated before measurement in duplicate via a commercially available 125I-cAMP radioimmunoassay kit (Amersham, Little Chalfont, UK).
Measurement of insulin release
Flow-sorted rat beta cells that were cultured overnight in Ham's F10 medium were used for measurements of insulin release in static incubations [2] and perifusions [22]. Perifusion experiments were carried out in a multiple microchamber module (Endotronics, Coon Rapids, Minn., USA) using 2.5×105 beta cells. Samples were collected every minute and assayed for immunoreactive insulin with guinea pig anti-insulin serum [2]. Results were expressed as the percentage of the insulin content, measured in each individual batch of rat beta cells by sonicating the Biogel P2-containing beta cells in 2 mmol/l acetic acid with 0.25% BSA. In all experiments, the sum of insulin released in the perifusate was 10% or less of the total insulin content in the cells. Static insulin release experiments on INS-1 cell subclones were carried out essentially as described in [29]. Briefly, the cells were seeded in 24-well plates (Falcon) and grown to confluence. Twenty hours before testing, medium was changed with RPMI-1640 growth medium (including serum and supplements) containing 5 mmol/l glucose. Cells were rinsed twice in Kreb's Ringer bicarbonate HEPES (KRBH) buffer (pH 7.4) with 2 mmol/l glucose, and allowed to pre-incubate for 60 min at 37°C. Insulin release was subsequently measured over 60 min in KRBH with 2 or 20 mmol/l glucose in the presence or absence of 100 µmol/l IBMX.
Analysis of AC activity in RINm5F membranes
The interaction between Ca2+-calmodulin and preactivated Gsα-protein at the level of AC activity was tested in RINm5F membranes prepared from cells that were washed three times with phosphate-buffered saline. The cell pellet was suspended in 100 µl buffer A (20 mmol/l HEPES at pH 7.5, 5 mmol/l EDTA, 1 mmol/l EGTA, 200 mmol/l sucrose, 100 µg/ml phenylmethylsulfonyl fluoride, 100 µg/ml aprotinin, 10 µg/ml leupeptin, 10 µg/ml pepstatin, 22 µg/ml L-1-tosylamido-2-phenylethyl chloromethyl ketone, 22 µg/ml 1-chloro-3-tosylamido-7-amino-2-heptanone and 3.2 µg/ml lima bean trypsin inhibitor) and sonicated on ice for 1 min (Branson sonifier 250, Danbury, Conn., USA). After centrifugation (500×g for 7 min at 4°C) the supernatant was collected while the cell pellet was sonicated and centrifuged a second time. The pooled supernatant fractions were ultracentrifuged at 110 000×g for 1 h at 4°C. Supernatant and pellet fractions containing cellular nonmembrane and membrane compartments, respectively, were homogenized in buffer B (=buffer A with 2 mmol/l EDTA and without EGTA). Samples were taken for protein content using the Micro BCA protein assay Reagent kit (Pierce, Rockford, Ill., USA). The effects of adding 1 µmol/l of the diterpene forskolin [12], 40 nmol/l of the recombinant preactivated GTPγS.rGsα, 120 nmol/l bovine brain calmodulin (Calbiochem, La Jolla, Calif., USA), 100 µmol/l EGTA plus 250 µmol/l CaCl2 (resulting in 17 µmol/l free Ca2+) [30], alone or in combination, were tested on 25 µg protein per reaction. The AC assay mixture and incubation conditions were as described [30] except that 0.25 mmol/l IBMX was used instead of Ro 20-1724. The reaction was stopped by adding 8% ice cold trichloroacetic acid and total cAMP was determined by radioimmunoassay (Amersham). Recombinant Gsα protein was activated for 1 h with GTPγS (Sigma) as described previously [31] and unincorporated GTPγS was removed by gel filtration on a Sephadex G-50 MicroSpin column (Amersham-Pharmacia Biotech, Uppsala, Sweden).
PCR and nucleotide sequence analysis of AC-mRNA in beta cells
Total RNA from cells or tissues was extracted using TRIzol Reagent according to the manufacturer's protocol (Gibco BRL). The RNA quality and quantity was determined in UV-160A spectrophotometer (Shimadzu, Kyoto, Japan). First strand cDNA was generated using GeneAmp RNA PCR Core kit (Perkin Elmer, Branchburg, N.J., USA) using random hexamer primers and the manufacturer's protocol. Controls without template were included in each assay; amplified PCR fragments were absent. Specific cDNA sequences were amplified in a Perkin Elmer GeneAmp thermocycler 9600 (Perkin Elmer) using 2.5 U AmpliTaq Gold (Perkin Elmer), 1.5 mmol/l MgCl2, 20 pmole 5′ primer and 20 pmole 3′ primer (spanning AC cDNA fragments with the following nucleotide (nt) sequences: AC I (nt 2791–3294); AC II (nt 2802–3505); AC III (nt 3211–3665); AC IV (nt 1521–1957); AC V (nt 2802–3651); AC VI (nt 3062–3506); AC VII (nt 2944–3343); AC VIII (nt 3789–4267). Primer pairs for RT-PCR analysis were tested for self-complementarity, dimer formation and melting temperature using the Primer Analysis Software Oligo (National Biosciences, Plymouth, Minn., USA). For all eight AC isoforms, amplification consisted of 35 PCR cycles, including five cycles of [94°C—1 min, between 52°C and 68°C—1 min (optimized for each isoform), 72°C—1 min] and 30 cycles of [94°C—0.5 min, between 51°C and 64°C—1 min (optimized for each isoform), 72°C—1.5 min]. To assess integrity and quantity of reverse transcribed cellular RNA, we amplified the same cDNA samples with beta actin-specific primers (V01217; 5′-primer: codons 249–255 and 3′-primer: codons 338–344, yielding a fragment of 284 bp). The degree of cross-contaminating alpha and beta cells in AC signals amplified from the purified cell preparations was assessed via amplification of preproinsulin-1 (nt 238–1051; 10 cycles of 94°C—1 min, 65°C—1 min,72°C—1 min followed by 10 cycles of 94°C—0.5 min,60°C—1 min,72°C—1 min) and preproglucagon (5′-primer: codons 33–39 and 3'-primer: codons 142–149; five cycles of 94°C—1 min,58°C—1 min,72°C—1 min followed by 20 cycles of 94°C—0.5 min,55°C—1 min,72°C—1 min). Amplified fragments were controlled for length by ethidium bromide after electrophoresis on 1% or 1.5% agarose gels and further characterized via DNA sequencing (ABI-Prism 310, Perkin Elmer, Foster City, Calif., USA). The PCR fragments were photographed using a digital image processor (Kodak DC40 camera, Eastman Kodak, Rochester, N.Y., USA) and signal intensities were determined (Biomax 1D image analysis software, Kodak).
Immunoblotting of type VIII AC protein
Membranes were prepared from cells or tissues as described in "analysis of AC activity". Membrane and non-membrane protein fractions were treated for 5 min at 56°C in 5% SDS, 80 mmol/l TRIS at pH 6.8, 5 mmol/l EDTA, 10% glycerol, 5% beta mercaptoethanol, 1 mmol/l PMSF and bromophenol blue. The samples were further incubated for 10 min at room temperature after adding N-ethylmaleimide (final concentration 50 mmol/l) before loading on 6% polyacrylamide SDS gels. After electrophoresis and blotting, the nitrocellulose membranes (Schleicher and Schuell, Dassel, Germany) were blocked for 1 h at room temperature in TBST/M (5% milk, 10 mmol/l Tris.HCl pH 7.4, 150 mmol/l NaCl, 1% Tween20) and incubated overnight in TBST/M with affinity purified, primary polyclonal antibody (D88AP; dilution 1/250) directed against an oligopeptide corresponding to residues 1229–1248 of type VIII AC [30]. Binding of the primary antibody was detected using Western Blot Chemiluminiscence Reagent Plus (NEN Life Science Products, Boston, Mass., USA) after incubation with donkey anti rabbit F(ab')2 HRP conjugate (diluted1/2500 in TBST/M; Amersham-Pharmacia Biotech) as secondary antibody. As a quality control for the immunoreactivity, the antibody was used for immunodetection of type VIII AC protein in membranes from HEK 293 cells transfected with pCMV5-neo vector in which the full length type VIII AC cDNA was subcloned (HEK 293/AC-VIII-A in Fig. 6) [32]. Furthermore, preincubation of the primary antibody with excess of the respective antigenic peptide completely abolished the immunoreactive signal.
Statistical analysis
Results of functional tests are presented as means ± SEM of at least three independent experiments; in each experiment duplicate samples were incubated in parallel. The statistical significance of differences was assessed by two-tailed unpaired Student's t tests and confirmed by non-parametric Wilcoxon tests when appropriate or by ANOVA as mentioned, accepting p values of 0.05 or less as significant.
Results
Receptor-mediated cAMP accumulation in beta cells is potentiated by glucose in a calcium-dependent manner
During static incubations, cAMP content in rat beta cells was not influenced by glucose alone; however, the sugar enhanced the stimulatory effect of GLP-1 on cAMP accumulation in the cells (Fig. 1). This effect of glucose was not specific for GLP-1-induced cAMP accumulation, since it was also observed with glucagon (Fig. 2, Table 1). The potentiation seems mediated at the stage of cAMP production, rather than cAMP breakdown, because the phenomenon was only observed in the presence of the phosphodiesterase inhibitors such as the potent inhibitor 3-isobutyl-1-methylxanthine (IBMX) and the more selective inhibitor Ro-20-1724 (Fig. 2). The synergism between glucose and GLP-1 on cAMP production in beta cells (Fig. 1) was completely suppressed by co-incubation with 50 µmol/l of the L-type Ca2+-channel blocker verapamil, a well known inhibitor of glucose-induced insulin release [33, 34]. On the contrary, acetylcholine (Table 1), a neurotransmitter that mobilizes calcium ions from intracellular stores in beta cells [35] did not influence cAMP content in beta cells. However, potentiating effects of acetylcholine on insulin release from purified cells were observed (p<0.005; Table 1).
Synergism between glucose and GLP-1 on cAMP accumulation in beta cells is calcium-dependent. FACS-purified rat beta cells were incubated for 15 min at 37°C in Earle's HEPES buffer with 250 µmol/l IBMX and 1.4 mmol/l glucose (white bars) or 20 mmol/l glucose (black bars) either without or with GLP-1 (10 nmol/l) or GLP-1 plus verapamil (50 µmol/l). Data represent mean values ± SEM of five experiments; a p<0.01
Synergism between glucose and glucagon on cAMP accumulation in beta cells is not mediated by interaction at the level of phosphodiesterases. Rat beta cells were preincubated for 5 min in Earle's HEPES buffer containing 1.4 mmol/l glucose alone (A) or 1.4 mmol/l glucose in the presence of 100 µmol/l of the PDE inhibitors Ro-20-1724 (B) or IBMX (C). Subsequent 5 min incubations occurred in 1.4 mmol/l (open bars) or 20 mmol/l glucose (closed bars), either alone or in combination with 10 nmol/l glucagon as indicated. Data represent mean values ± SEM of four experiments; * p<0.01; ** p<0.001
The L-type Ca2+-channel blocker verapamil abrogates the synergism between GLP-1 and glucose upon insulin release
A marked synergism exists in the stimulation of insulin release by glucose on the one hand and hormones that raise cAMP on the other hand [2]. Such synergism can be observed both in static incubations (Table 1) and in dynamic perifusions (Fig. 3). In static incubations and in the presence of Ro-20-1724, the combination of glucagon (10 nmol/l) and glucose (20 mmol/l) increased insulin release 5±1-fold over the calculated sum of insulin released from each individual stimulus (p<0.005). Insulin released from perifused beta cells was higher during combined GLP-1 and glucose stimulation (data above basal rates: 3.2±0.3% of insulin content over 15 min) than the summation of the effects of the two separated stimuli (20 mmol/l glucose alone: 1.2±0.2% of cellular insulin content and GLP-1 at low glucose: 0.2±0.1% of content; p<0.001 vs combined stimulation). This synergism was equally present when the order of stimuli was reversed. It was not the result of a memory effect caused by repetitive beta cell stimulation with GLP-1, since a second stimulation with glucose plus GLP-1 elicited the same insulin release as during the first period of co-stimulation (Fig. 3B). In parallel to its effect on cAMP accumulation in the cells, Fig. 3A shows that verapamil effectively counteracted the combined stimulatory effect of glucose and GLP-1 upon insulin release (1.1±0.2% of content; p<0.001 vs control without verapamil), raising the question as to whether the effects of this drug on insulin release can be attributed solely to a decrease in [Ca2+]i or to both a decrease in [Ca2+]i and in [cAMP].
Synergism between glucose and GLP-1 on insulin release is abrogated by the L-type Ca2+-channel blocker verapamil. Beta cells were perifused with 1.4 mmol/l glucose (basal medium) which alternated with 10 min stimulations with 20 mmol/l glucose, 10 nmol/l GLP-1 (gray box) or both. Second stimulation with 20 mmol/l glucose plus 10 nmol/l GLP-1 occurred in the presence (A) or absence (B) of 50 µmol/l verapamil (black box). Data represent mean values ± SEM of eight (A) or three (B) experiments
AC activity in RINm5F cells is activated by both Gsα and Ca2+-calmodulin
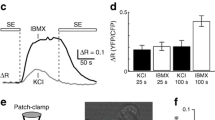
To examine the molecular mechanism underlying the observed synergism between glucose-stimulation and hormone-stimulation of cAMP production in rat beta cells, we measured adenylyl cyclase activity in membranes extracted from the insulinoma cell line RINm5F (Fig. 4). Functional integrity of the membranes was assessed by adding 1 µmol/l forskolin [12] which enhanced AC activity between two- and three-fold (13±3 vs 32±5 pmol cAMP·mg protein−1·min−1 in basal and forskolin-stimulated membranes respectively; p<0.05 vs basal). The measured AC activity in RINm5F membranes was not influenced by raising the free [Ca2+] to17 µmol/l or by adding calmodulin alone up to 600 nmol/l. The combination of 17 µmol/l [Ca2+] and 120 nmol/l calmodulin increased AC activity to similar values as observed upon forskolin stimulation (p<0.05 vs basal). Incubation of RINm5F membranes with 40 nmol/l of the recombinant preactivated G protein GTPγS.rGsα stimulated AC activity about threefold above basal (26±8 pmol cAMP·mg protein−1·min−1 above basal; p<0.01 vs basal; p<0.05 vs Ca2+-calmodulin). Simultaneous addition of GTPγS.rGsα and calmodulin at 17 µmol/l [Ca2+] resulted in a further increase of AC activity (50±8 pmol cAMP mg protein−1·min−1 above basal; p<0.01 vs basal; p<0.01 vs GTPγS.rGsα). The combined stimulatory effect was higher than what could be expected from the sum of adding Ca2+-calmodulin or GTPγS.rGsα separately (39±10 pmol cAMP mg protein−1·min−1 above basal; p<0.05). This indicates that Ca2+-calmodulin and Gsα act synergistically upon adenylyl cyclase(s) present in RINm5F cells, although this effect is much more modest than that described in type VIII AC-transfected HEK293 cells [30].
Regulation of RINm5F adenylyl cyclase activity by calcium-calmodulin and Gsα. Membrane protein (25 µg) was incubated for 10 min at 30°C in AC assay mixture with or without Ca 2+-calmodulin (17 µmol/l and 120 nmol/l, respectively) and recombinant GTPγS.Gsα(40 nmol/l), either alone or in combination, as indicated. Positive control for AC stimulation was forskolin (1 µmol/l). Data represent mean AC activity values above basal AC activity ± SEM of seven experiments. Basal AC activity in RINm5F cell membranes was 13±3 pmol cAMP·mg protein−1·min−1. Statistical significance was calculated by one-way analysis of variance (ANOVA). a p<0.05; b p<0.01
AC type VIII is expressed in insulin-producing cells
Among the cloned and characterized members of the mammalian AC family, two isoforms—i.e. type I AC and type VIII AC—are synergistically activated by Ca2+-calmodulin and Gsα [30, 36, 37]. To assess the mRNA expression of the various AC isoforms in primary beta cells as well as other pancreatic and non-pancreatic cells, we did a RT-PCR analysis on total cellular RNA using isoform-specific primers. This procedure yielded cDNA fragments of the expected length (Figs. 5, 6) and nucleotide sequence. Nonspecific PCR signals were not detected. Type I AC mRNA was abundant in brain but only present at low copy numbers in alpha cells and beta cells (Fig. 5) and very low levels in RINm5F cells. Strong PCR signals for type VI and type VIII AC were obtained from mRNA extracted from brain and flow-sorted beta cells. The other isoforms were either not detectable (type II and type VII AC) or were present at low levels (type III, type IV and type V AC). In addition to the three type VIII AC transcripts which have been described in rat brain [32] we detected a fourth transcript in which both exon 8 and exon 11 were absent (Fig. 6A,B). The same four splice products were present in cDNA prepared from purified rat beta cells and RINm5F cells (Fig. 6B). To assess if mRNA encoding type VIII AC was translated in insulin-producing cells, we examined type VIII AC protein abundance via immunoblots using a polyclonal antiserum that has been validated before [30]. As expected, this antibody detected a 165 kDa protein in the membrane fraction of rat brain, whereas the non-membrane cellular extract was negative (Fig. 6C). Type VIII AC immunoreactive protein was present in the membrane fraction prepared from RINm5F cells (Fig. 6C). Since RINm5F cells are known to be glucose-unresponsive, we compared expression of the type VIII AC splice variants in the INS-1 subclones 832/13 and 832/2 which markedly differ in glucose responsiveness as indicated by the differences in glucose-induced insulin release, being, respectively nine-fold and two-fold above basal secretion (Fig. 7A) [29]. A potent glucose-responsiveness was observed in the two subclones (13- and five-fold basal release, in 832/13- and 832/2-cells respectively) in the presence of the phosphodiesterase inhibitor IBMX (Fig. 7A). In agreement with a role of type VIII AC in beta cell function, the four splice variants were present in both INS-1 subclones (Fig. 7B).
mRNA analysis via RT-PCR of AC isoforms in beta cells with specific primer sets as explained in Materials and methods. Data are representative of four experiments. cDNA fragments amplified from preproinsulin-1 and preproglucagon mRNA's were controls for, respectively, contamination in the purified alpha- and beta-cell preparation
Type VIII AC gene expression in insulin-producing cells. A Schematic representation of exon 7–12 of the murine type VIII AC gene (GenBank accession number U85021) and scheme of the four possible mRNA splice variants observed in rat brain. Boundaries of exon sequences are indicated. Black box (exon 8:198 bp) and gray box (exon 11:90 bp) correspond to deleted regions observed in rat cDNAs [32]. Forward and reverse PCR primers used in panel B are positioned with bold arrows. B Detection of four type VIII AC mRNA splice variants in beta cells via RT PCR as described in Materials and methods. Data are representative of three experiments. C Immunodetection of type VIII AC (~165 kDa) on total protein (50 µg per lane) from the non-membrane and membrane fractions of rat tissues together with membranes prepared from RINm5F cells (100 µg of protein per lane) separated on 6% SDS-PAGE gels. Human HEK 293 cells stably expressing full length protein rat type VIII AC (HEK 293/AC-VIII-A; 2 µg per lane) and the empty expression vector (HEK 293/vector; 2 µg per lane) served as positive and negative controls, respectively
Insulin release and type VIII AC gene expression in clonal insulin-producing INS-1 cells. INS-1 subclones with robust (832/13) and moderate (832/2) responsiveness to glucose [29] were precultured for 20 h in 5 mmol/l glucose prior to 1-h culture in 2 or 20 mmol/l glucose in the absence (open bars) or presence (closed bars) of 100 µmol/l IBMX. The cellular insulin content of the two subclones was not statistically different. Data represent mean values ± SEM of three independent experiments with each time quadruple replicates. Statistical significance was calculated by ANOVA, corrected for multiple comparisons; * p<0.05; ** p<0.01. B RT PCR analysis of type VIII AC isoforms, using the same primerset as in Fig. 6, in both INS-1 subclones precultured for 20 h at 5 mmol/l glucose with rat brain and rat liver as positive and negative controls
Discussion
In vitro studies on rat pancreatic beta cells have shown that the insulinotropic effect of glucose is markedly potentiated by AC activators such as glucagon [2] or GLP-1 [5]. The molecular mechanism that is responsible for this potentiation is still unclear. Proposed sites are K+ ATP -channels [38], L-type Ca2+ channels [39], PKA anchoring site AKAP79/150 allowing crosstalk with PP2B [16] and target proteins involved in exocytosis [15, 18]. Glucose is known to increase cAMP concentrations in isolated islets [40, 41] and in purified beta cells when these are co-incubated with glucagon [13]. It is therefore conceivable that glucose and GLP-1 interact at the level of cAMP production. We propose that synergistic interaction between glucose and GLP-1 signalling pathways also exists for Ca2+-calmodulin-activated type VIII AC, an isotype that is expressed in insulin-producing beta cells. This organization allows beta cells to integrate a variety of signals induced by nutrients and hormones to ensure an appropriate physiological response.
Coincidence detection of simultaneous stimuli is crucial in the central nervous system and requires molecular integrators that allow crosstalk between different signal transduction systems. One example proceeds via voltage-dependent Ca2+-channels and calmodulin-regulated AC isoforms [37]. Type I and type VIII AC isoforms are particularly well adapted to fulfill this role since they are synergistically activated by Ca2+-calmodulin and Gsα [30, 32, 42, 43]. Consistent with their functional importance in the brain is the observation that mice rendered deficient in type I AC by targeted gene disruption present learning defects as a result of impaired long-term potentiation in hippocampal neurons [44] and in the cerebellum [45]. Type VIII AC is particularly abundant in hippocampal neurons [30] which exhibit a large capacity for long-term potentiation and altered synaptic plasticity. Accordingly, type VIII AC knock-out mice show defects in the anxiety response after repetitive exposure to stress [46].
A synergistic regulation by glucose and glucagon was observed at the juncture of cellular cAMP accumulation in flow-sorted beta cells, on condition that inhibitors of cAMP breakdown such as IBMX or Ro-20-1724 were present. This suggests that glucagon- and glucose-induced signalling interact at the level of cAMP production rather than at the point of cAMP breakdown. Glucagon and GLP-1 acutely amplify the glucose-dependent signal to a similar extent, so that their common target of interaction is likely to be distal from the activated receptors. Previous work on whole islets emphasised the importance of calcium for islet adenylyl cyclase activity. Two studies [47, 48] have shown that homogenates of rat isolated islets contain Ca2+-calmodulin-dependent AC activity. We show that the Ca2+-calmodulin effects interact synergistically with that of Gsα. As such, our data provide an explanation for the glucose potentiation on hormone-induced cAMP accumulation in intact beta cells [13]. Our observation that the L-type Ca2+-channel blocker verapamil [33] can abrogate the potentiating effect of glucose on GLP-1-induced intracellular cAMP accumulation supports the idea that the opening of L-type Ca2+-channels is required for the effect of glucose on AC activity in intact beta cells. Already at low glucose concentration, we observe a small, but borderline significant difference between cAMP accumulation in the presence and absence of verapamil subsequent to GLP-1 stimulation. It can be speculated that this effect is mediated by direct GLP-1 action on L-type Ca2+ channels. Activation of the GLP-1 receptor has been observed before to cause opening of L-type voltage-dependent Ca2+ channels under non-stimulatory glucose conditions [49, 50, 51] and to increase electrical activity by slowing Ca2+ channel inactivation [52]. The GLP-1 induced increase in intracellular Ca2+ concentrations may be able to stimulate Ca2+-calmodulin-regulated AC isoforms (type I and VIII AC) resulting in the production of cAMP [37], which can be antagonized by adding the L-type Ca2+-channel blocker verapamil with the preservation of the Gs-protein stimulated cAMP production by ACs. The effect of glucose on glucagon receptor cAMP production was not mimicked or amplified by acetylcholine. This indicates that mobilization of Ca2+ from intracellular stores is not as effective as influx through L-type Ca2+-channels in the activation of AC, consistent with existing literature [53].
Amplification of cDNA using the type VIII AC primer set resulted in strong signals both with primary flow-sorted rat beta cells and the rat beta cell lines RINm5F or INS-1. While it can be argued for FACS-purified beta cells that the PCR signals are derived from the few non-beta cells that are present in these preparations [28], this possibility is highly unlikely. First, the signal intensity of type VIII AC mRNA in FACS-purified alpha cells was around 20% of the signal intensity of flow sorted beta cells. Consequently, the type VIII AC signal in pure beta cells cannot be explained by the 5% or fewer alpha cells present in this cell preparation. Second, type VIII AC expression was observed in three different beta cell lines, with strong (INS-1 832/13), moderate (INS-1 832/2) and no (RINm5F) glucose responsiveness. This indicates that type VIII AC is not directly responsible for conveying glucose-responsiveness to a beta cell, but direct evidence involving gene-overexpression or gene-silencing will be required to further address this issue.
The present observations do not infer that AC type VIII is the only or even the main adenylyl cyclase contributing to overall cellular cAMP accumulation. In fact, our RT-PCR analysis clearly identifies the presence of several isoforms in RNA prepared from purified primary beta cells. It is possible that the rather weak type III, IV, and V AC signals are due to contaminating non-beta cells, because signals were much stronger in FACS-purified alpha cells, respecting the beta to alpha signal intensity ratio that was also observed for glucagon. Amongst the five Ca2+-calmodulin-regulated AC isoforms, only type I and type VIII are synergistically activated by Ca2+-calmodulin and Gsα [37]. Previous expression analyses in isolated islets [54, 55] suggested that the AC isoforms III, V and VI are also present in beta cells. From a regulatory perspective, the possible presence of type III AC in beta cells seems interesting. In isolated membranes, type III AC can be stimulated by Ca2+-calmodulin on condition that other activators, e.g. forskolin or activated Gsα are present at the same time [56]. However, (i) this stimulation is additive rather than synergistic; (ii) in intact cells, type III AC is inhibited by raised cytosolic [Ca2+], possibly as a consequence of the activation of Ca2+-calmodulin-dependent kinases or phosphatases [57]. It was reported that the spontaneously diabetic rat strain Goto-Kakizaki has defects both in the KATP-dependent and -independent pathways of glucose stimulation [58], abnormal glucose activation of exocytosis [59] as well as increased expression of AC type III [54] and type VIII in islets [60] and increased cAMP generation after forskolin stimulation [59]. Congruently, interaction between glucose and glucagon (or related peptides) can be disturbed in other models of Type 2 diabetes [61].
Besides overall cellular expression, subcellular localisation in signalling complexes could be crucial for the integrated response of beta cells to glucose and GLP-1. Co-localisation of Ca2+-sensitive AC and capacitative Ca2+-entry channels was found in embryonic kidney cells [62, 63], as well as in cardiac myocytes [64] and in parotid cells [65]. It will be a challenge for future studies to study such co-localisation in beta cells, since this spatial organization may contribute to foci of cellular cAMP formation when cells are exposed to hormone as observed in other cell types [66, 67]. In RINm5F cells, cAMP signalling complexes with relevance for exocytosis have been observed recently [16]. Important questions that remain to be answered are: (i) whether GLP-1 receptors of primary beta cells in situ are preferentially coupled to type VIII AC isoforms; (ii) if the cAMP that is thus formed preferentially signals to protein complexes involved in regulation of exocytosis.
Is type VIII AC the only site at which cAMP-generating receptors and glucose interact synergistically? As was mentioned above, other molecular targets of interaction have been proposed [16, 27], following crosstalk between cAMP and Ca2+. In isolated mouse islets that were studied under depolarizing conditions in the presence of diazoxide (i.e. under high tonic intracellular [Ca2+]) the synergism between glucose and GLP-1 is still present [68]. We suggest that at least one of the molecuar targets are regulated by other mediators than Ca2+, possibly by signals generated by cataplerosis [11].
In conclusion, our study provides evidence for the expression at RNA and protein level of the type VIII AC gene in pancreatic beta cells, as well as its functional activity in isolated membranes or in intact cells. The regulatory properties of this enzyme make it a well adapted molecular integrator of nutrient and hormonal stimuli that control insulin release.
Abbreviations
- AC:
-
Adenylyl cyclase
- Gsα :
-
alpha subunit of G-protein stimulatory to adenylyl cyclase
- AKAP:
-
A-kinase anchoring protein
- GLP-1:
-
glucagon-like peptide 1
- GIP:
-
glucose-dependent insulinotropic peptide
- IBMX:
-
3-isobutyl-1-methylxanthine
- PDE:
-
phosphodiesterase
- PKA:
-
protein kinase A
- PP2B:
-
protein phosphatase 2B
References
Pipeleers D (1987) The biosociology of pancreatic B cells. Diabetologia 30:277–291
Pipeleers DG, Schuit FC, In't Veld PA et al. (1985) Interplay of nutrients and hormones in the regulation of insulin release. Endocrinology 117:824–833
Huypens P, Ling Z, Pipeleers D, Schuit F (2000) Glucagon receptors on human islet cells contribute to glucose competence of insulin release. Diabetologia 43:1012–1019
Schuit FC, Pipeleers DG (1986) Differences in adrenergic recognition by pancreatic A and B cells. Science 232:875–877
Mojsov S, Weir GC, Habener JF (1987) Insulinotropin: glucagon-like peptide I (7–37) co-encoded in the glucagon gene is a potent stimulator of insulin release in the perfused rat pancreas. J Clin Invest 79:616–619
Newgard CB, McGarry JD (1995) Metabolic coupling factors in pancreatic beta-cell signal transduction. Annu Rev Biochem 64:689–719
Maechler P, Wollheim CB (2001) Mitochondrial function in normal and diabetic beta-cells. Nature 414:807–812
Hellman B, Gylfe E, Bergsten P et al. (1994) Glucose induces oscillatory Ca2+ signalling and insulin release in human pancreatic beta cells. Diabetologia 37:S11–S20
Henquin JC (2000) Triggering and amplifying pathways of regulation of insulin secretion by glucose. Diabetes 49:1751–1760
Prentki M, Tornheim K, Corkey BE (1997) Signal transduction mechanisms in nutrient-induced insulin secretion. Diabetologia 40:S32–S41
Flamez D, Berger V, Kruhoffer M, Orntoft T, Pipeleers D, Schuit FC (2002) Critical role for cataplerosis via citrate in glucose-regulated insulin release. Diabetes 51:2018–2024
Henquin JC, Meissner HP (1984) The ionic, electrical, and secretory effects of endogenous cyclic adenosine monophosphate in mouse pancreatic B cells: studies with forskolin. Endocrinology 115:1125–1134
Schuit FC, Pipeleers DG (1985) Regulation of adenosine 3′,5′-monophosphate levels in the pancreatic B cell. Endocrinology 117:834–840
Lester LB, Langeberg LK, Scott JD (1997) Anchoring of protein kinase A facilitates hormone-mediated insulin secretion. Proc Natl Acad Sci USA 94:14942–14947
Ämmälä C, Eliasson L, Bokvist K et al. (1994) Activation of protein kinases and inhibition of protein phosphatases play a central role in the regulation of exocytosis in mouse pancreatic β cells. Proc Natl Acad Sci USA 91:4343–4347
Lester LB, Faux MC, Nauert JB, Scott JD (2001) Targeted protein kinase A and PP-2B regulate insulin secretion through reversible phosphorylation. Endocrinology 142:1218–1227
Ozaki N, Shibasaki T, Kashima Y et al. (2000) cAMP-GEFII is a direct target of cAMP in regulated exocytosis. Nat Cell Biol 2:805–811
Kashima Y, Miki T, Shibasaki T et al. (2001) Critical role of cAMP-GEFII-Rim2 complex in incretin-potentiated insulin secretion. J Biol Chem 276:46046–46053
Moens K, Heimberg H, Flamez D et al. (1996) Expression and functional activity of glucagon, glucagon-like peptide I, and glucose-dependent insulinotropic peptide receptors in rat pancreatic islet cells. Diabetes 45:257–261
Scrocchi LA, Brown TJ, MaClusky N et al. (1996) Glucose intolerance but normal satiety in mice with a null mutation in the glucagon-like peptide 1 receptor gene. Nat Med 2:1254–1258
Miyawaki K, Yamada Y, Yano H et al. (1999) Glucose intolerance caused by a defect in the entero-insular axis: a study in gastric inhibitory polypeptide receptor knockout mice. Proc Natl Acad Sci USA 96:14843–14847
Flamez D, Van Breusegem A, Scrocchi LA et al. (1998) Mouse pancreatic beta-cells exhibit preserved glucose competence after disruption of the glucagon-like peptide-1 receptor gene. Diabetes 47:646–652
Moens K, Flamez D, Van Schravendijk C, Ling Z, Pipeleers D, Schuit F (1998) Dual recognition by pancreatic β-cells via glucagon and glucagon-like peptide 1 receptors. Diabetes 47:66–72
Scheen AJ, Castillo MJ, Lefebvre PJ (1996) Assessment of residual insulin secretion in diabetic patients using the intravenous glucagon stimulatory test: methodological aspects and clinical applications. Diabetes Metab 22:397–406
Moens K, Berger V, Ahn JM et al. (2002) Assessment of the role of interstitial glucagon in the acute glucose secretory responsiveness of in situ pancreatic beta-cells. Diabetes 51:669–675
Lawrence MC, Bhatt HS, Watterson JM, Easom RA (2001) Regulation of insulin gene transcription by a Ca(2+)-responsive pathway involving calcineurin and nuclear factor of activated T cells. Mol Endocrinol 15:1758–1767
Lawrence MC, Bhatt HS, Easom RA (2002) NFAT regulates insulin gene promoter activity in response to synergistic pathways induced by glucose and glucagon-like peptide-1. Diabetes 51:691–698
Pipeleers DG, In 't Veld PA, Van De Winkel M, Maes E, Schuit F, Gepts W (1985) A new in vitro method for the study of pancreatic A and B cells. Endocrinology 117:806–816
Hohmeier HE, Mulder H, Chen G, Henkel-Rieger R, Prentki M, Newgard CB (2000) Isolation of INS-1-derived cell lines with robust ATP-sensitive K+ channel-dependent and-independent glucose-stimulated insulin secretion. Diabetes 49:424–430
Cali JJ, Zwaagstra JC, Mons N, Cooper DMF, Krupinski J (1994) Type VIII adenylyl cyclase. A Ca2+/calmodulin-stimulated enzyme expressed in discrete regions of rat brain. J Biol Chem 269:12190–12195
Krupinski J, Coussen F, Bakalyar HA et al. (1989) Adenylyl cyclase amino acid sequence: possible channel- or transporter-like structure. Science 244:1558–1564
Cali JJ, Parekh RS, Krupinski J (1996) Splice variants of type VIII adenylyl cyclase: differences in glycosylation and regulation by Ca2+/calmodulin. J Biol Chem 271:1089–1095
Devis G, Somers G, Van Obberghen E, Malaisse WJ (1975) Calcium antagonists and islet function. I. Inhibition of insulin release by verapamil. Diabetes 24:247–251
Lebrun P, Malaisse WJ, Herchuelz A (1982) Evidence for two distinct modalities of Ca2+ influx into pancreatic B cell. Am J Physiol 242:E59–E66
Garcia M-C, Hermans MP, Henquin J-C (1988) Glucose-, calcium- and concentration-dependence of acetylcholine stimulation of insulin release and ionic fluxes in mouse islets. Biochem J 254:211–218
Xia Z, Storm DR (1997) Calmodulin-regulated adenylyl cyclases and neuromodulation. Curr Opin Cell Biol 7:391–396
Cooper DM, Karpen JW, Fagan KA, Mons NE (1998) Ca(2+)-sensitive adenylyl cyclases. Adv Second Messenger Phosphoprotein Res 32:23–51
Beguin P, Nagashima K, Nishimura M, Gonoi T, Seino S (1999) PKA-mediated phosphorylation of the human K(ATP) channel: separate roles of Kir6.2 and SUR1 subunit phosphorylation. EMBO J 18:4722–4732
Rajan AS, Hill RS, Boyd III AE (1989) Effect of rise in cAMP levels on Ca2+influx through voltage-dependent Ca2+ channels in HIT cells. Second-messenger synarchy in β-cells. Diabetes 38:874–880
Charles MA, Fanska R, Schmid FG, Forsham PH, Grodsky GM (1973) Adenosine 3′,5′-monophosphate in pancreatic islets: glucose-induced insulin release. Science 179:569–571
Grill V, Cerasi E (1973) Activation by glucose of adenyl cyclase in pancreatic islets of the rat. FEBS Letters 33:311–314
Krupinski J, Cali JJ (1998) Molecular diversity of the adenylyl cyclases. Adv Second messenger Phosphoprotein Res 32:53–79
Wayman GA, Impey S, Wu Z, Kindsvogel W, Prichard L, Storm DR (1994) Synergistic activation of the type I adenylyl cyclase by Ca2+ and Gs-coupled receptors in vivo. J Biol Chem 269:25400–25405
Wu Z-L, Thomas SA, Villacres EC et al. (1995) Altered behavior and long-term potentiation in type I adenylyl cyclase mutant mice. Proc Natl Acad Sci USA 92:220–224
Storm DR, Hansel C, Hacker B, Parent A, Linden DJ (1998) Impaired cerebellar long-term potentiation in type I adenylyl cyclase mutant mice. Neuron 20:1199–1210
Schaefer ML, Wong ST, Wozniak DF et al. (2000) Altered stress-induced anxiety in adenylyl cyclase type VIII-deficient mice. J Neurosci 20:4809–4820
Valverde I, Vandermeers A, Anjaneyulu R, Malaisse WJ (1979) Calmodulin activation of adenylate cyclase in pancreatic islets. Science 206:225–227
Sharp GWG, Wiedenkeller DE, Kaelin D, Siegel EG, Wollheim CB (1980) Stimulation of adenylyl cyclase by Ca2+ and calmodulin in rat islets of Langerhans: explanation for the glucose-induced increase in cyclic AMP levels. Diabetes 29:74–77
Gromada J, Bokvist K, Ding WG, Holst JJ, Nielsen JH, Rorsman P (1998) Glucagon-like peptide 1 (7–36) amide stimulates exocytosis in human pancreatic beta-cells by both proximal and distal regulatory steps in stimulus-secretion coupling. Diabetes 47:57–65
Kanno T, Suga S, Wu J, Kimura M, Wakui M (1998) Intracellular cAMP potentiates voltage-dependent activation of L-type Ca2+ channels in rat islet beta-cells. Pflugers Arch 435:578–580
Ämmälä C, Ashcroft FM, Rorsman P (1993) Calcium-independent potentiation of insulin release by cyclic AMP in single β-cells. Nature 363:356–358
Britsch S, Krippeit-Drews P, Lang F, Gregor M, Drews G (1995) Glucagon-like peptide-1 modulates Ca2+ current but not K+ATP current in intact mouse pancreatic B-cells. Biochem Biophys Res Commun 207:33–39
Fagan KA, Graft RA, Tolman S, Schaack J, Cooper DMF (2000) Regulation of a Ca2+-sensitive adenylyl cyclase in an excitable cell. Role of voltage-gated versus capacitative Ca2+ entry. J Biol Chem 275:40187–40194
Abdel-Halim SM, Guenifi A, He B et al. (1998) Mutations in the promotor of adenylyl cyclase (AC)-III gene, overexpression of AC-III mRNA, and enhanced cAMP generation in islets from the spontaneosly diabetic GK rat model of type 2 diabates. Diabetes 47:498–504
Leech CA, Castonguay MA, Habener JF (1999) Expression of adenylyl cyclase subtypes in pancreatic β-cells. Biochem Biophys Res Comm 254:703–706
Choi E-J, Xia Z, Storm DR (1992) Stimulation of the type III olfactory adenylyl cyclase by calcium and calmodulin. Biochemistry 31:6492–6498
Wayman GA, Impey S, Storm DR (1995) Ca2+- inhibition of type III adenylyl cyclase in vivo. J Biol Chem 270:21480–21486
Portha B, Serradas P, Bailbé D, Suzuki K-I, Goto Y, Giroix M-H (1991) β-cell insensitivity to glucose in the GK rat, a spontaneous nonobese model for type II diabetes. Diabetes 40:486–491
Abdel-Halim SM, Guenifi A, Khan A et al. (1996) Impaired coupling of glucose signal to the exocytotic machinery in diabetic GK rats. Diabetes 45:934–940
Guenifi A, Portela-Gomes GM, Grimelius L, Efendic S, Abdel-Halim SM (2000) Adenylyl cyclase isoform expression in non-diabetic and diabetic Goto-Kakizaki (GK) rat pancreas. Evidence for distinct overexpression of type-8 adenylyl cyclase in diabetic GK rat islets. Histochem Cell Biol 113:81–89
Cerasi E, Luft R (1970) Diabetes mellitus-A disorder of cellular information transmission? Horm Metab Res 2:246–249
Chiono M, Mahey R, Tate G, Cooper DMF (1995) Capacitative Ca2+ entry exclusively inhibits cAMP synthesis in C6-2B glioma cells. J Biol Chem 270:1149–1155
Fagan KA, Mahey R, Cooper DMF (1996) Functional co-localization of transfected Ca2+-stimulable adenylyl cyclases with capacitative Ca2+ entry sites. J Biol Chem 271:12438–12444
Gao T, Puri TS, Gerhardstein BL, Chien AJ, Green RD, Hosey MM (1997) Identification and subcellular localization of the subunits of L-type calcium channels and adenylyl cyclase in cardiac myocytes. J Biol Chem 272:19401–19407
Watson EL, Jacobson KL, Singh JC et al. (2000) The type 8 adenylyl cyclase is critical for Ca2+ stimulation of cAMP accumulation in mouse parotid acini. J Biol Chem 275:14691–14699
Steinberg SF, Brunton LL (2001) Compartmentation of G protein-coupled signaling pathways in cardiac myocytes. Annu Rev Pharmacol Toxicol 41:751–773
Zaccolo M, Pozzan T (2002) Discrete microdomains with high concentration of cAMP in stimulated rat neonatal cardiac myocytes. Science 295:1711–1715
Sato Y, Nenquin M, Henquin JC (1998) Relative contribution of Ca2+-dependent and Ca2+-independent mechanisms to the regulation of insulin secretion by glucose. FEBS Lett 421:115–119
Acknowledgements
The authors wish to thank E. Quartier, A. Van Breusegem and V. Berger for technical assistance. We are grateful to the personnel of the Department of Metabolism and Endocrinology for providing purified rat islet alpha and beta cells and to L. Kaufman for help with the statistical analysis. The clonal cell lines INS1 832/13 and 832/2 [29] were generously supplied by Dr. C. Newgard, S. Stedman Center for Nutritional and Metabolic Studies, Duke University, Durham, N.C., USA. This study was supported by grant No. 9.0130.99 from the Flemish Fund for Scientific Research (FWO Vlaanderen), the Ministerie van de Vlaamse Gemeenschap, Departement Onderwijs (Geconcerteerde Onderzoeksactie 1807), and the Research Council of the Vrije Universiteit Brussel. S.A. Hinke is Visiting Postdoctoral Fellow at the FWO Vlaanderen.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Delmeire, D., Flamez, D., Hinke, S.A. et al. Type VIII adenylyl cyclase in rat beta cells: coincidence signal detector/generator for glucose and GLP-1. Diabetologia 46, 1383–1393 (2003). https://doi.org/10.1007/s00125-003-1203-8
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-003-1203-8