Abstract
Objectives
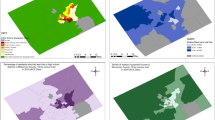
The purpose of this study was to examine the importance of urban–rural context as a determinant of call rates to smoking cessation lines.
Methods
This study used individual level New Zealand Quitline call data from 2005 to 2009, and 2006 New Zealand Census data on smoking to calculate Quitline call rates for smokers. Negative binomial regression examined the relationship between call rates and a sevenfold urban–rural classification, controlling for age, sex, ethnicity and deprivation.
Results
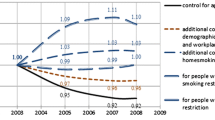
We found a significant urban–rural gradient in the rate of smokers calling Quitline. Rates were highest among smokers in main-urban areas [0.09 (95 % confidence interval (CI) = 0.089, 0.091)] decreasing with successive urban–rural classifications to the lowest rate in rural/remote areas [0.036 (95 % CI = 0.03, 0.04)]. This association was not confounded by age, sex, ethnicity or deprivation.
Conclusions
Smokers in rural areas are less likely to use the New Zealand Quitline, even after controlling for confounding factors. This suggests that the national quitline is less effective in reaching rural smokers and more attention to the promotion of smoking cessation in rural communities is needed.
Similar content being viewed by others
References
Anderson CM, Zhu SH (2007) Tobacco quitlines: looking back and looking ahead. Tob Control 16(Suppl 1):i81–i86. doi:10.1136/tc.2007.020701
Borland R, Segan CJ (2006) The potential of quitlines to increase smoking cessation. Drug Alcohol Rev 25(1):73–78. doi:10.1080/09595230500459537
Campbell SL, Lee L, Haugland C, Helgerson SD, Harwell TS (2008) Tobacco quitline use: enhancing benefit and increasing abstinence. Am J Prev Med 35(4):386–388. doi:10.1016/j.amepre.2008.06.032
Cosh S, Maksimovic L, Ettridge K, Copley D, Bowden JA (2013) Aboriginal and Torres Strait Islander utilisation of the Quitline service for smoking cessation in South Australia. Aust J Prim Health 19(2):113–118
Delnevo C, Foulds J, Vorbach U, Kazimir E (2006) Seasonal variations in stage of change among Quitline clients. Tob Control 15(1):70–71. doi:10.1136/tc.2005.013847
Farrelly MC, Hussin A, Bauer UE (2007) Effectiveness and cost effectiveness of television, radio and print advertisements in promoting the New York smokers’ quitline. Tob Control 16(Suppl 1):i21–i23. doi:10.1136/tc.2007.019984
Harris R, Tobias M, Jeffreys M, Waldegrave K, Karlsen S, Nazroo J (2006) Racism and health: the relationship between experience of racial discrimination and health in New Zealand. Soc Sci Med 63(6):1428–1441. doi:10.1016/j.socscimed.2006.04.009
Harwell TS, Lee L, Haugland C, Wilson SM, Campbell SL, Holzman GS, Gohdes D, Helgerson SD (2007) Utilization of a tobacco quit line prior to and after a tobacco tax increase. J Public Health Manag Pract 13(6):637–641. doi:10.1097/01.PHH.0000296141.02295.16
Hutcheson TD, Greiner KA, Ellerbeck EF, Jeffries SK, Mussulman LM, Casey GN (2008) Understanding smoking cessation in rural communities. J Rural Health 24(2):116–124. doi:10.1111/j.1748-0361.2008.00147.x
Li J, Chen N (2008) Trends and seasonal variations on where new Quitline clients obtained the Quitline number, 2003–2007. The Quit Group, Wellington. http://www.quit.org.nz/file/research/factsAndFigures/obtain_Quitline_number_2003-2007_20080721.pdf
Li J, Grigg M (2007) Evidence of declining nicotine dependency in new callers to a national quitline. J Smoking Cessation 2:8–11. doi:10.1375/jsc.2.1.8
Lichtenstein E, Zhu SH, Tedeschi GJ (2010) Smoking cessation quitlines: an underrecognized intervention success story. Am Psychol 65(4):252–261. doi:10.1037/a0018598
McAfee TA (2007) Quitlines a tool for research and dissemination of evidence-based cessation practices. Am J Prev Med 33(6 Suppl):S357–367. doi:10.1016/j.amepre.2007.09.011
Ortiz AP, Diaz-Toro EC, Calo WA, Correa-Fernandez V, Cases A, Santos-Ortiz MC, Mejía L, Wetter DW (2008) Characteristics of smokers accessing the Puerto Rico Quitline. Puerto Rico Health Sci J 27(3):213–219
Ossip-Klein DJ, McIntosh S (2003) Quitlines in North America: evidence base and applications. Am J Med Sci 326(4):201–205
Pearce J, Barnett R, Moon G (2012) Sociospatial inequalities in health-related behaviours. Pathways linking place and smoking. Prog Hum Geogr 36(1):3–24. doi:10.1177/0309132511402710
Salmond C, Crampton P, Atkinson J (2007) NZDep2006 index of deprivation. Department of Public Health, University of Otago Wellington, New Zealand. http://www.health.govt.nz/system/files/documents/publications/nzdep2006-report.pdf
Sheffer MA, Redmond LA, Kobinsky KH, Keller PA, McAfee T, Fiore MC (2010) Creating a perfect storm to increase consumer demand for Wisconsin’s Tobacco Quitline. Am J Prev Med 38(3 Suppl):S343–S346. doi:10.1016/j.amepre.2009.11.014
Sood A, Andoh J, Rajoli N, Hopkins-Price P, Verhulst SJ (2008) Characteristics of smokers calling a national reactive telephone helpline. Am J Health Promot 22(3):176–179. doi:10.4278/ajhp.22.3.176
Statistics New Zealand (2008) Housing Indicators 2008. Indicator 18: access to telecommunications. http://www.stats.govt.nz/browse_for_stats/people_and_communities/housing/housing-indicators/18-access-to-telecommunications.aspx
Statistics New Zealand (2009) New Zealand: an urban/rural profile update. http://www.stats.govt.nz/browse_for_stats/people_and_communities/Geographic-areas/urban-rural-profile-update.aspx
Twigg L, Moon G, Szatkowski L, Iggulden P (2009) Smoking cessation in England: intentionality, anticipated ease of quitting and advice provision. Soc Sci Med 68(4):610–619. doi:10.1016/j.socscimed.2008.11.032
Wilson N, Grigg M, Graham L, Cameron G (2005) The effectiveness of television advertising campaigns on generating calls to a national Quitline by Maori. Tob Control 14(4):284–286. doi:10.1136/tc.2004.010009
Wilson N, Sertsou G, Edwards R, Thomson G, Grigg M, Li J (2007) A new national smokefree law increased calls to a national quitline. BMC Public Health 7(1):75. doi:10.1186/1471-2458-7-75
Wilson N, Weerasekera D, Borland R, Edwards R, Bullen C, Li J (2010) Use of a national quitline and variation in use by smoker characteristics: ITC Project New Zealand. Nicotine Tob Res 12(suppl 1):S78–S84. doi:10.1093/ntr/ntq111
Zhu S-H, Rosbrook B, Anderson C, Gilpin E, Sadler G, Pierce JP (1995) The demographics of help-seeking for smoking cessation in California and the role of the California Smokers’ Helpline. Tob Control 9:S9–S15
Zhu SH, Anderson CM, Tedeschi GJ, Rosbrook B, Johnson CE, Byrd M, Gutiérrez-Terrell E (2002) Evidence of real-world effectiveness of a telephone quitline for smokers. N Engl J Med 347(14):1087–1093
Zhu SH, Gardiner P, Cummins S, Anderson C, Wong S, Cowling D, Gamst A (2011) Quitline utilization rates of African-American and white smokers: the California experience. Am J Health Promot 25(5 Suppl):S51–58. doi:10.4278/ajhp.100611-QUAN-185
Acknowledgments
This study was supported by the GeoHealth Laboratory, University of Canterbury, New Zealand.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Griffin, E., Moon, G. & Barnet, R. Examining the significance of urban–rural context in tobacco quitline use: does rurality matter?. Int J Public Health 60, 327–333 (2015). https://doi.org/10.1007/s00038-014-0634-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00038-014-0634-y