Abstract
Objectives and design
Microglia play an important role in immune and inflammatory responses in the central nervous system. Astragalus polysaccharide (APS) has been reported as an immune stimulant for various inflammation-associated diseases in vivo. The present study investigated the effects of APS on lipopolysaccharide-stimulated inflammatory responses in microglial cells.
Materials and methods
Cultured BV2 microglial cells were pre-treated with APS (0–200 μg/ml) prior to lipopolysaccharide (50 ng/ml) stimulation. The production of proinflammatory mediators including inducible nitric oxide synthase (iNOS)/nitric oxide (NO), cyclooxygenase-2 (COX-2)/prostaglandin E (PGE2), tumor necrosis factor-α (TNF-α) and interleukin-1β (IL-1β) were evaluated.
Results
APS dose-dependently reduced lipopolysaccharide stimulated nitric oxide and PGE2 production, as well as iNOS and cyclooxygenase-2 gene expression. It also attenuated proinflammatory cytokines IL-1β and TNF-α generation. In addition, APS inhibited nuclear factor-κB translocation by blockade of IκB degradation and suppressed protein kinase B phosphorylation in lipopolysaccharide-stimulated cells.
Conclusions
The inhibitory effects of APS on lipopolysaccharide-stimulated inflammatory mediator production in microglia are associated with suppression of nuclear factor-κB and protein kinase B signaling pathways. APS may offer therapeutic potential for treating inflammatory and neurodegenerative diseases accompanied with microglial activation.
Similar content being viewed by others
Introduction
Microglia are the resident macrophage-like cells in the central nervous system (CNS) and play an important role in the brain’s innate immunity [1]. Microglial cells respond to neuronal injury or damage with microglial activation, which typically prevent the pathophysiological process. However, over activated microglia can produce large amounts of harmful neurotoxic factors including nitric oxide (NO), prostaglandin E2 (PGE2), pro-inflammatory cytokines [interleukin-1 (IL-1), IL-6 and tumor necrosis factor-α (TNF-α)], reactive oxygen species and complement factors, etc. [2–5]. These neurotoxic and pro-inflammatory mediators are thought to contribute to the pathological processes associated with neurodegenerative diseases, such as Alzheimer’s disease, Parkinson’s disease and Amyotrophic lateral sclerosis [6–8]. In that regard, controlling microglial activation has been suggested as an important therapeutic target for treating various neurodegenerative diseases.
Astragalus polysaccharide (APS) is a water-soluble heteropolysaccharide extracted from the dried root of Astragalus membranaceus (Huangqi) [9, 10]. Huangqi has about 2,000 years of history in traditional Chinese medicine, with diverse pharmacologic activities including antioxidant, antitumor, anti-diabetes, antiviral, hepatoprotection, anti-atherosclerosis, hematopoiesis and neuroprotection [11–16]. Some of the previously observed beneficial effects of APS are associated with its anti-inflammatory activity in peripheral organs [13, 17]. Whether APS exhibits direct immunomodulatory effect on brain immune cell microglia, however, remains to be determined. Moreover, the bioactive principles and molecular mechanisms responsible for the anti-inflammatory activities of the APS in the microglia remain to be elucidated.
Lipopolysaccharide (LPS) is a bacterial endotoxin which can elicit a variety of inflammatory responses in cells, mammals and humans. LPS stimulation of the microglia has been employed as a useful model for the study of mechanisms underlying neuronal injury by various pro-inflammatory and neurotoxic factors released from activated microglia. The BV2 cells are derived from raf/myc-immortalized murine neonatal microglia and are the most frequently used substitute for primary microglia. The objective of the present study was to investigate the effect of APS on the inflammatory response induced by LPS in cultured BV2 microglial cells in vitro. The results demonstrated that APS attenuated the LPS-stimulated gene expression of iNOS, COX-2, TNF-α and IL-1β and subsequent production of NO, PGE2, TNF-α and IL-1β in BV2 cells. To elucidate the underlying mechanisms, the involvement of mitogen-activated protein kinases (MAPKs), protein kinase B (PKB) and nuclear factor-κB (NF-κB) was also examined. Our findings may provide critical information that will contribute to the therapeutic use of APS in the prevention of microglial activation.
Materials and methods
BV2 microglial cell culture
The murine BV2 cell line was obtained from China Center for Type Culture Collection, Wuhan, China. Cells were maintained in Dulbecco’s Modified Eagle’s Medium supplemented with 10 % Fetal Bovine Serum, 100 U/ml penicillin and 100 mg/ml streptomycin at 37 °C in a humidified incubator with 5 % CO2. For the experiments, confluent cultures were passaged by trypsinization and treated in culture medium overnight before treatments.
Nitrite quantification
BV2 microglial cells (2 × 105 cells/well) were plated onto 96-well plates and pre-treated with different concentrations of APS (Shanghai Medicinal Materials, China) (0, 50, 100, or 200 μg/ml) for 1 h prior to stimulation with 50 ng/ml of LPS (Sigma, USA) for 24 h. The cell supernatants were collected and assayed for NO production using Griess reagent (Invitrogen, USA). The samples were mixed with Griess reagent according to the manufacture’s instruction and then incubated at room temperature for 30 min. The absorbance was measured at 540 nm on a microplate reader (PerkinElmer Inc, USA). Nitrite concentration was determined from a sodium nitrite standard curve.
Analysis of cell viability
Cell viability was measured by CCK-8 assay (Dojindo, Japan). BV2 microglial cells (2 × 105 cells/well) were plated onto 96-well plates and pre-treated with different concentrations of APS (0, 50, 100, or 200 μg/ml) for 1 h prior to stimulation with 50 ng/ml of LPS. After incubation for 24 h, 20 µl of the ready-to-use kit reagent was added to cell cultures in each cell culture well according to the manufacturer’s instruction. Following an additional 2-h incubation at 37 °C, 5 % CO2, the absorbance at 460 nm was determined using a microplate reader (PerkinElmer Inc, USA).
ELISA assay for TNF-α, IL-1β and PGE2
BV2 cells were plated at a density of 2 × 105 cells/well in a 96-well plate. Cells were then pretreated with APS (0, 50, 100, or 200 μg/ml) for 1 h prior to stimulation with 50 ng/ml of LPS. The cell-free supernatant was collected at 24 h stimulation with LPS. TNF-α (R&D Systems, Inc., USA), IL-1β (R&D Systems, Inc., USA) and PGE2 (Cayman, USA) were measured by ELISA kits according to the manufacturer’s instructions. The absorbance at 450 nm was determined using a microplate reader (PerkinElmer Inc, USA).
Isolation of total RNA and reverse transcription polymerase chain reaction
BV2 cells were pretreated with APS (0, 50, 100, or 200 μg/ml) for 1 h and stimulated with LPS for 24 h. Total RNA was isolated using TRIzol reagent (Life Technologies, USA). The total RNA (1.0 mg) obtained from cells was using RevertAid First Strand cDNA Synthesis Kit (Thermo Scientific, USA) to produce cDNAs. The inducible nitric oxide synthase (iNOS), cyclooxygenase-2 (COX-2), TNF-α and IL-1β genes were amplified from the cDNA by PCR. PCR primers were as follows: mouse iNOS (5′-ATCTTGAAGCCCCGCTACT-3′ and 5′-TCCTTTGAGCCCTTTGTGCT-3′), COX-2 (5′-CCTGCTGCCCGAC ACCTT CAACAT-3′ and 5′-CAGCAACCC GGCCAGCAATCT-3′), IL-1β (5′-GACGGACCCCAAAAGATGAA-3′ and 5′-CA GCACGAGGCTTTTTTGTT-3′), TNF-a (5′-CAAAAGATGGGGGGCTTC-3′ and 5′-TGTGGGTGAGGAGCACGTAGT-3′) and β-actin (5′-AAGGCGAC AGCAGTTGGTT-3′ and 5′-ACCTGGGCCATTCAGAAATT-3′). After amplification, PCR reactions were separated electrophoretically on 1 % agarose gels and visualized by ethidium bromide staining. β-Actin was used as an internal control.
Western blot analysis
BV2 cells were pretreated with APS (0 or 200 μg/ml) for 1 h and stimulated with LPS for 24 h. The treated cells were washed with ice-cold PBS followed by homogenization in 0.2 ml ice-cold lysis buffer (50 mM Tris–HCl, pH 7.4, 1 % NP-40, 0.25 % sodium deoxycholate, 150 mM NaCl, 1 mM EGTA) containing protease inhibitor cocktail (1 mM phenylmethylsulfonyl fluoride, 1 μg/ml aprotinin, 5 μg/ml leupeptin, 1 mM Na3VO4, and 1 mM NaF). Cell lysates were centrifuged at 12,000×g for 15 min at 4 °C. The supernatant was collected and stored at −70 °C as total protein samples. Protein concentration was determined using BCA protein assay kit. Samples of the lysates were separated by 10 % SDS-PAGE and then transferred onto PVDF membranes. After being placed in blocking buffer, the membranes were incubated with the following primary antibodies (1:1,000 dilutions): anti-phosphorylated-NFκBp65, anti-IκBα, anti-p-P38, anti-P38, anti-p-ERK (extracellular signal-regulated protein kinase), anti-ERK, anti-p-SARP/JNK (c-Jun NH(2)-terminal kinase), anti-SARP/JNK, anti-p-PKB, anti-PKB (Signaling Technology, USA) and GAPDH (R&D Systems, Inc., USA). Then, secondary antibodies (LI-COR Biosciences, USA) were conjugated to a fluorescent entity: IRDye 800-conjugated goat anti-rabbit IgG and/or Alexa Fluor 680-conjugated goat anti-mouse IgG (dilution 1:10,000) in 10 ml LI-COR blocking buffer with gentle agitation for 1 h at room temperature. The membrane was scanned and analyzed on the Odyssey infrared imaging system (LI-COR Biosciences, USA).
Statistical analyses
Data are expressed as mean ± SEM of six independent determinations. Statistical significance was determined using analysis of variance (ANOVA) followed by Newman–Keuls’s test. AP value of <0.05 was considered statistically significant.
Results
APS suppresses LPS-stimulated iNOS and NO production in BV2 cells
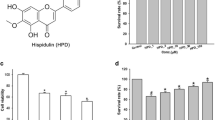
We first examined whether APS could regulate LPS-induced NO production in BV2 microglia. The cells were pretreated with 0, 50, 100, or 200 μg/ml of APS for 1 h prior to LPS (50 ng/ml) stimulation for 24 h, and NO levels in the cell culture medium were measured by the Griess assay. As shown in Fig. 1a, LPS alone markedly increased NO production compared to control. BV2 cells treated with LPS accumulated 31.25 ± 0.76 μM nitrite at 24 h (p < 0.001, compared to 1.98 ± 0.09 μM nitrite from untreated control cells). Cultures treated with 100 μg/ml APS and LPS accumulated 20.03 ± 1 μM nitrite, a significant 35 % decrease compared to cells treated with LPS alone (p < 0.001). Cultures treated with 200 μg/ml APS and LPS accumulated 9.73 ± 0.73 μM nitrite, a significant 69 % decrease compared to cells treated with LPS alone (p < 0.001). Thus, APS counteracts the effects of LPS on nitrite production.
Astragalus polysaccharide (APS) attenuates LPS-stimulated NO production and iNOS gene expression in BV2 microglial cells. BV2 cells were pretreated with APS (0–200 μg/ml) 1 h prior to incubation with LPS (50 ng/ml). The total RNA and the supernatants were isolated at 24 h after LPS treatment a The levels of NO in the culture medium were determined using the Griess reaction. b Levels of iNOS mRNA were determined by RT-PCR. The relative mRNA levels were quantified by scanning densitometry and normalized to β-actin mRNA. Bars represent the mean ± SEM from six independent measures: ###, p < 0.001 versus control; *, p < 0.05, ***, p < 0.001 versus LPS
We further examined whether APS’s inhibitory effect on NO production was associated with decreased iNOS expressions in LPS-stimulated BV2 microglia. The RT-PCR analysis showed that iNOS mRNA transcription levels were undetectable in unstimulated BV2 microglia. LPS treatment significantly increased iNOS mRNA levels (p < 0.001, versus control); however, these expressions were markedly attenuated in BV2 microglia pretreated with APS at concentrations of 100 μg/ml and 200 μg/ml (p < 0.05 and p < 0.001, respectively, versus LPS; Fig. 1b). The results suggest that APS-induced reductions in the transcriptional expression of iNOS were the cause of the inhibition of NO production.
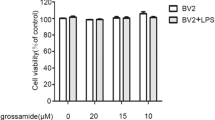
Cytotoxic effects of APS were evaluated by measurement of the viability of BV2 cells incubated with LPS (50 ng/ml) in the presence or absence of APS (50, 100, or 200 μg/ml) using the CCK-8 assay. Cell viability was not significantly altered by APS at the concentrations used (data not shown).
APS inhibits LPS-induced COX-2 mRNA and PGE2 in BV2 cells
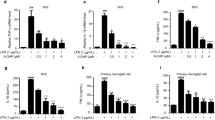
Treatment of BV2 microglia with LPS resulted in increased another pro-inflammatory enzyme, COX-2 mRNA expression (p < 0.001 versus control; Fig. 2a). Pre-treatment with APS significantly inhibited COX-2 mRNA expression, compared with LPS-treated cells (p < 0.001). Levels of PGE2 production were measured in BV2 cells by ELISA assay. LPS stimulation increased the PGE2 production tenfold as compared with control (p < 0.001; Fig. 2b). Consistent with the results of COX-2 mRNA expression, LPS-induced PGE2 up-regulation was significantly decreased by APS in a concentration-dependent manner (p < 0.001 versus LPS).
Effect of astragalus polysaccharide (APS) on LPS-stimulated expression of COX-2 gene expression and PGE2 production in BV2 microglia. BV2 cells were pretreated with APS (0–200 μg/ml) 1 h prior to incubation with LPS (50 ng/ml). The total RNA and the supernatants were isolated at 24 h after LPS treatment. a The levels of COX-2 mRNA were determined by RT-PCR. The relative mRNA levels were quantified by scanning densitometry and normalized to β-actin mRNA. b Levels of PGE2 in the culture medium were determined by ELISA. Bars represent the mean ± SEM from six independent measures: ###, p < 0.001 versus control; ***, p < 0.001 versus LPS
APS suppresses production of inflammatory cytokines in LPS-stimulated BV2 microglia
We next analyzed whether APS regulated the production of proinflammatory cytokines, such as TNF-α and IL-1β and their mRNA levels in LPS-stimulated BV2 cells. For this study, BV2 cells were incubated with various concentrations of APS in the presence or absence of LPS (50 ng/ml) for 24 h, and cytokine levels in the culture supernatant were measured by ELISA assay. As shown in Fig. 3a, b, TNF-α and IL-1β levels were significantly increased in the culture media of LPS-stimulated BV2 microglia (p < 0.001, versus control). However, pretreatment with APS resulted in a significantly decreased release of pro-inflammatory cytokines in a concentration-dependent manner (p < 0.05 or p < 0.001 versus LPS). In a parallel experiment, using BV2 cell line, the expressions of LPS stimulated TNF-α and IL-1β mRNA were also dose-dependently decreased by APS treatment (p < 0.01 or p < 0.001 versus LPS; Fig. 3c, d).
Astragalus polysaccharide (APS) attenuates LPS-stimulated proinflammatory cytokines in BV2 microglia. Cells were pretreated with APS (0–200 μg/ml) for 1 h before LPS treatment (50 ng/ml), and total RNA and the supernatants were isolated at 24 h after LPS treatment. a The levels of TNF-α and b interleukin-1β (IL-1β) present in the supernatants were measured by ELISA. c The levels of TNF-α and d IL-1β mRNA were determined by RT-PCR. The relative mRNA levels were quantified by scanning densitometry and normalized to β-actin mRNA. Bars represent the mean ± SEM from six independent measures: ###, p < 0.001 versus control; *, p < 0.05, **, p < 0.01, ***, p < 0.001 versus LPS
APS inhibits NFκB activation in LPS-stimulated BV2 microglia
Since NFκB is a key transcriptional regulator of genes involved in inflammatory responses, the effect of APS on LPS-induced NFκB activation was examined. LPS treatment resulted in 2.5-fold increase in phosphorylated NFκBp65 protein (p < 0.001 versus control), whereas this activation was prevented in cells pre-incubated with 200 μg/ml of APS (p < 0.001 versus LPS; Fig. 4a). NFκB is located in the cytosol bound to the inhibitor IκB, and IκB protein degradation is an essential step for NFκB activation. We next assessed whether LPS stimulation resulted in changes in the content of IκB. LPS addition to cells caused a 70 % decrease in the abundance of IκB (p < 0.001 versus control), whereas APS significantly blocked the LPS-induced IκB degradation (p < 0.01 versus LPS; Fig. 4b), thereby inhibiting activation and translocation of NF-κB.
Effect of astragalus polysaccharide (APS) on LPS-induced NFκB activation and IκB degradation in BV2 microglia. Cells were treated with APS (0 or 200 μg/ml) for 1 h before LPS treatment (50 ng/ml) for 24 h. Cell extracts were then prepared and subjected to Western blotting using a anti-phosphorylated-NFκB p65 and b anti-IκB antibodies. The relative protein expression were quantified by scanning densitometry and normalized to GAPDH. Bars represent the mean ± SEM from six independent measures: ###, p < 0.001 versus control; **, p < 0.01, ***, p < 0.001 versus LPS
Effects of APS on MAPKs and PKB signaling pathway
Recent findings have indicated that the MAPKs and PKB signaling pathways prompt NFκB activation through the IκB degradation. Therefore, the effects of APS on phosphorylation level of MAPKs and PKB pathway were analyzed by Western blot assay in BV2 cells activated with LPS. As shown in Fig. 5, LPS-induced phosphorylation of MAPKs (ERK, JNK, p38) and PKB (p < 0.001 versus control). APS at 200 μg/ml inhibited PKB phosphorylation (p < 0.001 versus LPS; Fig. 5d), but did not affect ERK, JNK, or p38 phosphorylation (p > 0.05 versus LPS; Fig. 5a–c). These findings suggest that inhibition of PKB phosphorylation by APS treatment may result in decreased expression of LPS-induced inflammatory transcription factors in BV2 cells.
Effect of astragalus polysaccharide (APS) on LPS-induced phosphorylation of ERK, JNK, p38 and PKB in BV-2 microglia. BV-2 cells were APS (0 or 200 μg/ml) for 1 h before being incubated with LPS (50 ng/ml) for 24 h. Cell extracts were then prepared and subjected to Western blotting with antibodies specific for phosphorylated forms of a JNK, b ERK, c p38 and d PKB. The relative protein expression was quantified by scanning densitometry and normalized to GAPDH. Bars represent the mean ± SEM from six independent measures: ###, p < 0.001 versus control; ***, p < 0.001 versus LPS
Discussion
Microglia activation produces a variety of pro-inflammatory mediators, including NO and PGE2, and pro-inflammatory cytokines, such as TNF-α and IL-1β, which play critical roles in several neurodegenerative conditions [18–20]. The significant finding of this study is that pretreatment with APS, an extract from the herb Huangqi that frequently used in traditional medicine, prominently attenuates the LPS-upregulated pro-inflammatory mediator production in cultured BV2 microglial cells. The APS concentrations (0–200 µg/ml) were chosen based on preliminary experiments and previous studies demonstrating that APS at concentrations up to 200 μg/ml exerts protective effects in vitro [21, 22]. Our data showed that APS dose-dependently inhibits the production of NO and PGE2 in LPS-stimulated BV2 microglia. These inhibitory effects of APS are accompanied by decreased expression of iNOS and COX-2 at the transcriptional levels. TNF-α and IL-1β are also important pro-inflammatory cytokines, which are secreted by activated microglia. We identified that APS reduced the synthesis of TNF-α and IL-1β mRNA and inhibited the subsequent release of TNF-α and IL-1β. This is the first report demonstrating that APS is capable of regulating LPS-stimulated inflammatory mediator production in BV2 microglia.
There is evidence supporting the anti-inflammatory effect of APS in various experimental models in vivo and in vitro. APS treatment has been reported to attenuate hyperglycemia and pancreatic beta-cell apoptosis in type 1 diabetic mice, with possible mechanism of immunoregulatory action on Th1/Th2 cytokine ratio [23]. APS can also reduce serum concentrations of TNF-α and IL1-β and the indices of arthritis in animal model of adjuvant-induced arthritis in rats [24]. In palmitate-treated RAW264.7 cells in vitro, APS administration inhibits the expression of pro-inflammatory genes, such as IL-1β, iNOS, monocyte chemoattractant protein-1, IL-6 and CD11c, but not TNF-α [25]. APS also induces the differentiation of splenic dendritic cells to CD11c (high) CD45RB (low) dendritic cells followed by shifting of Th2 to Th1 with enhancement of T lymphocyte immune function in vitro [26]. Our study demonstrated that APS is able to prevent the microglia activation-associated production of inflammatory mediators. It is becoming increasingly evident that microglia are central to mediating the effects of neuroinflammation and play a crucial role in the development and progression of many neurodegenerative diseases [27]. The findings of the current study may provide a new attractive therapeutic in traditional medicine in the treatment and prevention of neuroinflammation.
NFκB is a transcriptional regulator of various genes involved in the production of many proinflammatory cytokines and enzymes related to the inflammatory process. Inactivated NFκB is normally located in the cytoplasm where it is complexed with its inhibitory protein IκB. In response to pro-inflammatory stimuli, IκB is phosphorylated and subsequently degraded, leading to the release and nuclear translocation of NFκB [28]. Once in the nucleus, activated NFκB then regulates expression of a range of the pro-inflammatory genes, including iNOS, COX-2, TNF-α and IL-1β [29–32]. Therefore, NFκB–IκB complexes are an effective target for decreasing pro-inflammatory mediator production. Astragalus membranaceus has been shown to inhibit mRNA expressions of NFκB and IκB in renal cortex of streptozotoxin-induced diabetic rats [33]. In order to investigate the mechanism involved in anti-inflammatory effect of APS, we analyzed the NFκB signaling in activated microglia. Exposure of BV2 cells to LPS resulted in degradation of IκB and the subsequent release and translocation of NFκB. APS administration, however, suppressed degradation of IκB, thereby preventing the phosphorylation of NFκB. These results suggested that the anti-inflammatory effect of APS in activated microglia is associated with inhibition of the NFκB signaling activation.
Mitogen-activated protein kinases, including p38, JNK and ERK have been suggested to be involved in oxidative stress and proinflammatory signaling cascades [34]. In addition, PI3K/PKB regulates cellular activation, inflammatory responses and apoptosis [35]. Previous investigations by us and other researchers have discovered that the PI3K/PKB and MAPKs pathways are essential targets of APS [21, 36]. We, therefore, questioned whether the anti-inflammatory mechanisms of APS are associated with modulation of PI3K/PKB and MAPKs in activated BV2 microglia. Our results showed that each of the tested kinases including ERK, JNK, p38 and PKB was phosphorylated upon LPS stimulation, consistent with their crucial role in mediating inflammation. However, only pPKB was selectively suppressed by APS treatment. The inhibitory effect of APS on PKB expression in BV2 cells is in contrast to our previous finding that APS inhibited palmitate-induced insulin resistance by restoring phosphorylation of PKB in C2C12 cells [21]. The reason for this discrepancy could mainly due to variation in individual PKB gene expression with cell types and stimulators. In another study reported by Ye et al., APS was found to inhibit proliferation of basal-like breast cancer cell line MDA-MB-468 and down-regulate the expression of PKB phosphorylation [37].
Taken together, the results of our study demonstrate that APS prevents LPS-induced activation of PKB and NFκB, which leads to down-regulation of iNOS, COX-2, TNF-α and IL-1β in BV2 microglial cells (summarized in Fig. 6), suggesting the possibility of strong anti-inflammatory actions of this compound. Further investigations will identify whether the anti-inflammatory effects of APS on microglial cells might be correlated with its protective effects against neurodegenerative diseases.
Schematic of how astragalus polysaccharide (APS) impacts LPS-induced inflammatory responses in BV2 microglia cells. LPS stimulation activates TLR4 which acts on MAPKs, PI3K/PKB and sends signals to NFκB–IκB complex to release NFκB into the nucleus. NFκB while in the nucleus induces the transcription of genes that involved in inflammatory responses. APS administration selectively prevents LPS-induced PKB phosphorylation, which in turn, suppresses degradation of IκB, and inhibits the phosphorylation of NFκB, leading to decreased production of NO, PGE2, TNF-α and IL-1β in BV2 microglia cells
References
Kettenmann H, Hanisch UK, Noda M, Verkhratsky A. Physiology of microglia. Physiol Rev. 2011;91:461–553.
Cunningham C. Microglia and neurodegeneration: the role of systemic inflammation. Glia. 2013;61:71–90.
Graeber MB, Li W, Rodriguez ML. Role of microglia in CNS inflammation. FEBS Lett. 2011;585:3798–805.
Zhang Y, Chen WA. Biochanin A inhibits lipopolysaccharide-induced inflammatory cytokines and mediators production in BV2 microglia. Neurochem Res. 2015;40:165–71.
Lee HJ, Kim KW. Anti-inflammatory effects of arbutin in lipopolysaccharide-stimulated BV2 microglial cells. Inflamm Res. 2012;61:817–25.
Depboylu C, Stricker S, Ghobril JP, Oertel WH, Priller J, Hoglinger GU. Brain-resident microglia predominate over infiltrating myeloid cells in activation, phagocytosis and interaction with T-lymphocytes in the MPTP mouse model of Parkinson disease. Exp Neurol. 2012;238:183–91.
Lee M, McGeer E, McGeer PL. Activated human microglia stimulate neuroblastoma cells to upregulate production of beta amyloid protein and tau: implications for Alzheimer’s disease pathogenesis. Neurobiol Aging. 2015;36:42–52.
Sanagi T, Nakamura Y, Suzuki E, Uchino S, Aoki M, Warita H, et al. Involvement of activated microglia in increased vulnerability of motoneurons after facial nerve avulsion in presymptomatic amyotrophic lateral sclerosis model rats. Glia. 2012;60:782–93.
Fu J, Wang Z, Huang L, Zheng S, Wang D, Chen S, et al. Review of the botanical characteristics, phytochemistry, and pharmacology of Astragalus membranaceus (Huangqi). Phytother Res. 2014;28:1275–83.
Ma XQ, Shi Q, Duan JA, Dong TT, Tsim KW. Chemical analysis of Radix astragali (Huangqi) in China: a comparison with its adulterants and seasonal variations. J Agric Food Chem. 2002;50:4861–6.
Yuan W, Wang J, Wu T. Chinese herbal medicine Huangqi type formulations for nephrotic syndrome. Cochrane Database Syst Rev 2008:CD006335.
Sang Z, Zhou L, Fan X, McCrimmon RJ. Radix astragali (Huangqi) as a treatment for defective hypoglycemia counter regulation in diabetes. Am J Chin Med. 2010;38:1027–38.
Liu C, Wang G, Chen G, Mu Y, Zhang L, Hu X, et al. Huangqi decoction inhibits apoptosis and fibrosis, but promotes Kupffer cell activation in dimethylnitrosamine-induced rat liver fibrosis. BMC Complement Altern Med. 2012;12:51.
Fu S, Zhang J, Menniti-Ippolito F, Gao X, Galeotti F, Massari M, et al. Huangqi injection (a traditional Chinese patent medicine) for chronic heart failure: a systematic review. PLoS One. 2011;6:e19604.
Cheng XD, Hou CH, Zhang XJ, Xie HY, Zhou WY, Yang L, et al. Effects of Huangqi (Hex) on inducing cell differentiation and cell death in K562 and HEL cells. Acta Biochim Biophys Sin (Shanghai). 2004;36:211–7.
Cao J, Chen Z, Zhu Y, Li Y, Guo C, Gao K, et al. Huangqi–Honghua combination and its main components ameliorate cerebral infarction with Qi deficiency and blood stasis syndrome by antioxidant action in rats. J Ethnopharmacol. 2014;155:1053–60.
Wang XH, Jia HL, Deng L, Huang WM. Astragalus polysaccharides mediated preventive effects on bronchopulmonary dysplasia in rats. Pediatr Res. 2014;76:347–54.
Orre M, Kamphuis W, Dooves S, Kooijman L, Chan ET, Kirk CJ, et al. Reactive glia show increased immunoproteasome activity in Alzheimer’s disease. Brain. 2013;136:1415–31.
Luo T, Wu J, Kabadi SV, Sabirzhanov B, Guanciale K, Hanscom M, et al. Propofol limits microglial activation after experimental brain trauma through inhibition of nicotinamide adenine dinucleotide phosphate oxidase. Anesthesiology. 2013;119:1370–88.
Harms AS, Cao S, Rowse AL, Thome AD, Li X, Mangieri LR, et al. MHCII is required for alpha-synuclein-induced activation of microglia, CD4 T cell proliferation, and dopaminergic neurodegeneration. J Neurosci. 2013;33:9592–600.
Liu M, Qin J, Hao Y, Liu M, Luo J, Luo T, et al. Astragalus polysaccharide suppresses skeletal muscle myostatin expression in diabetes: involvement of ROS-ERK and NF-kappa B pathways. Oxid Med Cell Longev. 2013;2013:782497.
Zhang CL, Ren HJ, Liu MM, Li XG, de Sun L, Li N, et al. Modulation of intestinal epithelial cell proliferation, migration, and differentiation in vitro by Astragalus polysaccharides. PLoS One. 2014;9:e106674.
Li RJ, Qiu SD, Chen HX, Tian H, Wang HX. The immunotherapeutic effects of Astragalus polysaccharide in type 1 diabetic mice. Biol Pharm Bull. 2007;30:470–6.
Jiang JB, Qiu JD, Yang LH, He JP, Smith GW, Li HQ. Therapeutic effects of astragalus polysaccharides on inflammation and synovial apoptosis in rats with adjuvant-induced arthritis. Int J Rheum Dis. 2010;13:396–405.
Lu J, Chen X, Zhang Y, Xu J, Zhang L, Li Z, et al. Astragalus polysaccharide induces anti-inflammatory effects dependent on AMPK activity in palmitate-treated RAW264.7 cells. Int J Mol Med. 2013;31:1463–70.
Liu QY, Yao YM, Zhang SW, Sheng ZY. Astragalus polysaccharides regulate T cell-mediated immunity via CD11c (high) CD45RB (low) DCs in vitro. J Ethnopharmacol. 2011;136:457–64.
Frank-Cannon TC, Alto LT, McAlpine FE, Tansey MG. Does neuroinflammation fan the flame in neurodegenerative diseases? Mol Neurodegener. 2009;4:47.
Bourke E, Kennedy EJ, Moynagh PN. Loss of I kappa B-beta is associated with prolonged NF-kappa B activity in human glial cells. J Biol Chem. 2000;275:39996–40002.
Yao ZA, Xu L, Wu HG. Immunomodulatory function of kappa-carrageenan oligosaccharides acting on LPS-activated microglial cells. Neurochem Res. 2014;39:333–43.
Vo TS, Ngo DH, Ta QV, Wijesekara I, Kong CS, Kim SK. Protective effect of chitin oligosaccharides against lipopolysaccharide-induced inflammatory response in BV-2 microglia. Cell Immunol. 2012;277:14–21.
Dilshara MG, Lee KT, Kim HJ, Lee HJ, Choi YH, Lee CM, et al. Anti-inflammatory mechanism of alpha-viniferin regulates lipopolysaccharide-induced release of proinflammatory mediators in BV2 microglial cells. Cell Immunol. 2014;290:21–9.
Kaushik DK, Thounaojam MC, Mitra A, Basu A. Vespa tropica venom suppresses lipopolysaccharide-mediated secretion of pro-inflammatory cyto-chemokines by abrogating nuclear factor-kappa B activation in microglia. Inflamm Res. 2014;63:657–65.
Zhang YW, Wu CY, Cheng JT. Merit of Astragalus polysaccharide in the improvement of early diabetic nephropathy with an effect on mRNA expressions of NF-kappa B and I kappa B in renal cortex of streptozotoxin-induced diabetic rats. J Ethnopharmacol. 2007;114:387–92.
Kim EK, Choi EJ. Pathological roles of MAPK signaling pathways in human diseases. Biochim Biophys Acta. 2010;1802:396–405.
Manukyan MC, Weil BR, Wang Y, Abarbanell AM, Herrmann JL, Poynter JA, et al. The phosphoinositide-3 kinase survival signaling mechanism in sepsis. Shock. 2010;34:442–9.
Liu M, Wu K, Mao X, Wu Y, Ouyang J. Astragalus polysaccharide improves insulin sensitivity in KKAy mice: regulation of PKB/GLUT4 signaling in skeletal muscle. J Ethnopharmacol. 2010;127:32–7.
Ye MN, Chen HF, Zhou RJ, Liao MJ. Effects of Astragalus polysaccharide on proliferation and Akt phosphorylation of the basal-like breast cancer cell line. Zhong Xi Yi Jie He Xue Bao. 2011;9:1339–46.
Acknowledgments
This study was supported by Nature Science Foundation of China, Grant number 81102863, 81271205; and Nature Science Foundation of Hubei Province, Grant number 2012FFB04437, 2013CFB252.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Responsible Editor: John Di Battista.
J. Qin is a co-first author.
Rights and permissions
About this article
Cite this article
Luo, T., Qin, J., Liu, M. et al. Astragalus polysaccharide attenuates lipopolysaccharide-induced inflammatory responses in microglial cells: regulation of protein kinase B and nuclear factor-κB signaling. Inflamm. Res. 64, 205–212 (2015). https://doi.org/10.1007/s00011-015-0798-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-015-0798-9