Abstract.
Objective: Our aim was to study how different SERMs modulate the inflammatory responses induced by lipopolysaccharide (LPS) or unmethylated CpG-oligonucleotides in mouse and rat microglial cells.
Materials and methods: Inflammatory responses of mouse N9 microglial cells and rat primary hippocampal microglia to lipopolysaccharide (LPS) exposure were recorded by the secretion of nitric oxide (NO) and cytokine IL-6 in two models where SERM was added either 24 h before LPS addition or simultaneously or even after the LPS exposure. The responses of 17β-estradiol, tamoxifen, raloxifene and ICI 182.780 were compared. Responses were recorded by ELISA, Northern and EMSA assays.
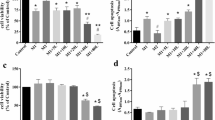
Results: SERMs but not 17β-estradiol induced a significant, concentration-dependent anti-inflammatory response both in rat primary microglial cells and in mouse N9 microglial cells. The response was observed both in NO and IL-6 secretion as well as in total IL-6 mRNA expression. We have recently observed that histone deacetylase (HDAC) inhibitors can potentiate the LPS-induced inflammatory response. Raloxifene and tamoxifen inhibited the potentiation of LPS response induced by trichostatin A, an HDAC inhibitor, in N9 microglia. A SERM-induced anti-inflammatory response was observed in acute models where SERM was added simultaneously or even up to 6 h later than LPS exposure. In contrast, the pretreatment of N9 microglia with tamoxifen or raloxifene for 30 h before LPS exposure did not provide any protection against the LPS response. We also observed that the raloxifene-induced protection in N9 microglia was connected to a decline of LPS-induced DNAbinding activity of AP-1 but not that of NF-κB transcription factors.
Conclusions: Our results show that tamoxifen, raloxifene and ICI 182.780 induce an anti-inflammatory response in acute models of mouse and rat microglial cells. It seems that this response is not estrogen receptor -mediated but, probably, is attributable to some SERM-induced modulation of LPS-activated pro-inflammatory signalling cascades.
Similar content being viewed by others
Author information
Authors and Affiliations
Corresponding author
Additional information
Received 11 September 2004; returned for revision 22 December 2004; accepted by I. Ahnfelt-Rønne 11 January 2005
Rights and permissions
About this article
Cite this article
Suuronen, T., Nuutinen, T., Huuskonen, J. et al. Anti-inflammatory effect of selective estrogen receptor modulators (SERMs) in microglial cells. Inflamm. res. 54, 194–203 (2005). https://doi.org/10.1007/s00011-005-1343-z
Issue Date:
DOI: https://doi.org/10.1007/s00011-005-1343-z