Summary
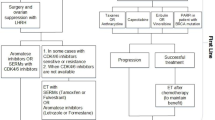
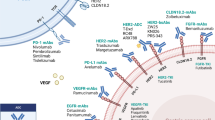
Molecular genetic evidence indicates that endometrial carcinoma likely develops as the result of a multistep process of oncogene activation and tumor suppressor gene inactivation. These molecular alterations appear to be specific for Type I (endometrioid) and Type II (non endometrioid) cancers. Type I cancers are characterized by mutation of PTEN, KRAS2, defects in DNA mismatch repair, as evidenced by the microsatellite instability phenotype, and a near diploid karyotype. Type II cancers often contain mutations of TP53 and Her-2/neu and are usually nondiploid. The clinical value of many of these molecular markers is now being tested and it may help to refine diagnosis and establish an accurate prognosis. Furthermore, some of these tumor biomarkers constitute the targets for emerging therapies. Transtuzumab against Her-2/neu and bevacizumab against VEGF overexpressing carcinomas are among the promising novel treatments. Additional translational research is needed to identify molecular and genetic alterations with potential for therapeutic interventions.
Similar content being viewed by others
References
Potischman N, Hoover RN, Brinton LA, et al. Case-control study of endogenous steroid hormones and endometrial cancer. J Natl Cancer Inst. 1996;88:1127–31.
Lax SF. Molecular genetic pathways in various types of endometrial carcinoma: from a phenotypical to a molecular-based classification. Virchows Arch. 2004;444: 213–23.
Pral J. Prognostic parameters of endometrial carcinoma. Hum Pathol. 2004;35:649–62.
Herrington CS. What we could do now: molecular pathology of gynaecological cancer. J Clin Pathol: Mol Pathol. 2001;54: 222–4.
Ioachin E. Immunohistochemical tumour markers in endometrial ercinoma. Eur J Gyneacol Oncol. 2005;26:563–71.
Creasman WT. Prognostic significance of hormone receptors in endometrial cancer. Cancer. 1993;71:1467–70.
Halperin R, Zehavi S, Habler L, et al. Comparative immunohistochemical study of endometrioid and serous papillary carcinoma of endometrium. Eur J Gynaecol Oncol. 2001;22:122–6.
Mutter GL, Lin MC, Fitzgerald JT, et al. Altered PTEN expression as a diagnostic marker for the earliest endometrial precancers. J Natl Cancer Inst. 2000;92:924–30.
Salvesen HB, Stefansson I, Kretzschmar EI, et al. Significance of PTEN alterations in endometrial carcinoma: A population-based study of mutations, promoter methylation and PTEN protein expression. Int J Oncol. 2004;25:1615–23.
Risinger JL, Berchuck A, Kohler M, et al. Genetic instability of microsatellites in endometrial carcinoma. Cancer Res. 1993; 53:5100–3.
Ichikawa Y, Lemon SJ, Wang S, et al. Microsatellites instability and expression of hMSH2 or hMLH1 in normal and malignant endometrial and ovarian epithelium in hereditary nonpolyposis colorectal cancer family members. Cancer Genet Cytogenet. 1999;112:2–8.
Wijnen JT, Vasen HF, Khan PM, et al. Clinical findings with implications for genetic testing in families with clustering of colorectal cancer. N Engl J Med. 1998;339: 511–518.
Goodfellow PJ, Buttin BM, Herzog TJ, et al. Prevalence of defective DNA mismatch repair and MSH6 mutation in an unselected series of endometrial cancers. PNAS. 2003;100:5908–13.
Broaddus RR, Lynch HT, Chen LM, et al. Pathologic features of endometrial carcinoma associated with HNPCC: a comparison with sporadic endometrial carcinoma. Cancer. 2006;106:87–94.
Miturski R, Bogusiewicz M, Ciotta C, et al. Mismatch repair genes and microsatellite instability as molecular markers for gynaecological cancer detection. Exp Biol Med. 2002;227:579–86.
MacDonald ND, Salvesen HB, Ryan A, et al. Frequency and prognostic impact of microsatellite instability in a large population-based study of endometrial carcinomas. Cancer Res. 2000;60:1750–2.
Pijnenborg JM, Dam-de Veen GC, de Haan J, et al. Defective mismatch repair and the development of recurrent endometrial carcinoma. Gynecol Oncol. 2004; 94:550–9.
Levine RL, Cargile CB, Blazes MS, et al. PTEN mutations and microsatellite instability in complex atypical hyperplasia, a precursor lesion to uterine endometrioid carcinoma. Cancer Res. 1998;58:5254–8.
Vousden KH. Activation of the p53 tumor suppressor protein. Biochim Biophys Acta. 2002;1602:47–59.
Tashiro H, Isacson C, Levine R, et al. p53 gene mutations are common in uterine serous carcinoma and occur early in their pathogenesis. Am J Pathol. 1997;150:177–85.
Lax SF, Kendall B, Tashiro H, Slebos RJ, Hedrick L. The frequency of p53, K-ras mutations, and microsatellite instability differs in uterine endometrioid and serous carcinoma: evidence of distinct molecular genetic pathways. Cancer. 2000; 88:814–24.
Ragni N, Ferrero S, Prefumo F, et al. The association between p53 expression, stage and histological features in endometrial cancer. Eur J Obstet Gynecol Reprod Biol. 2005;125:111–6.
Geisler JP, Geisler HE, Wiermann MC, et al. p53 expression as a prognostic indicator of 5-year survival in endometrial cancer. Gynecol Oncol. 1999;74:468–71.
Pijnenborg JM, van de Broek L, Dam de Veen GC, et al. TP53 overexpression in recurrent endometrial carcinoma. Gynecol Oncol. 2006;100:597–404.
Erdem O, Erdem M, Dursum A, et al. Angiogenesis, p53, and bcl-2 expression as prognostic indicators in endometrial cancer: comparison with tradicional clinicopathologic variables. Int J Gynecol Pathol. 2003;22:254–60.
Ohkouchi T, Sakuragi N, Watari H, et al. Prognostic significance of Bcl-2, p55 overexpression, and lymph node metastasis in surgically staged endometrial carcinoma. Am J Obstet Gynecol. 2002;187:353–9.
Saffari B, Bernstein L, Hong DC, et al. Association of p53 mutations and a codon 72 single nucleotide polymorphism with lower overall survival and responsiveness to adjuvant radiotherapy in endometrioid endometrial carcinomas. Int J Gynecol Cancer. 2005;15:952–63.
Alkushi A, Lim P, Coldman A, et al. Interpretation of p53 immunoreactivity in endometrial carcinoma: establishing a clinically relevant cut-off level. Int J Gynecol Pathol. 2004;25:129–37.
McCluggage WG, Connolly LE, McGregor G, et al. A strategy for defining biologically relevant levels of p53 protein expression in clinical samples with reference to endometrial neoplasia. Int J Gynecol Pathol. 2005;24:507–12.
Ellison DA, Maygarden SJ. Quantitative DNA analysis of fresh solid tumors by flow and image cytometric methods: a comparison using the Roche Pathology Workstation Image Analyzer. Mod Pathol. 1995;8:275–81.
Evans MP, Podratz KC. Endometrial neoplasia: prognostic significance of ploidy status. Clin Obstet Gynecol. 1996;59:696–706.
Silverman MB, Roche PC, Kho RM, et al. Molecular and cytogenetic risk assessment in endometrial cancer. Gynecol Oncol. 2000;77:1–7.
Wimberger P, Hillemanns P, Kapsner T, et al. Evaluation of prognostic factors following flow-cytometric DNA analysis after cytokeratin labelling. II. Cervical and endometrial cancer. Anal Cell Pathol. 2002; 24:147–58.
Mariani A, Sebo TJ, Katzmann JA, et al. Pretreatment assessment of prognostic indicators in endometrial cancer. Am J Obstet Gynecol. 2000, p. 1535–44.
Mariani L, Conti L, Antenucci A, et al. Predictive value of cell kinetics in endometrial adenocarcinoma. Anticancer Res. 2000;20:3569–74.
Konski A, Domenico D, Tyrkus M, et al. Prognostic characteristics of surgical stage I endometrial adenocarcinoma. Int J Radiat Oncol Biol Phys. 1996;35:935–40.
Orbo A, Rydningen M, Straume B, Lysne S. Significance of morphometric, DNA cytometric features, and other prognostic markers on survival of endometrial cancer patients in northern Norway, Int J Gynecol Cancer. 2002;12:49–56.
Lundgren C, Auer G, Frankendal B, et al. Nuclear DNA content, proliferative activity, and p55 expression related to clinical and histopahologic features in endometrial carcinoma. Int J Gynecol Cancer. 2002; 12:110–8.
Baak JP, Suijders W, van Dierman B, et al. Prospective multicenter validation confirms the prognostic superiority of the endometrial carcinoma prognostic index in International Federation of Gynecology and Obstetrics stage 1 and 2 endometrial carcinoma. J Clin Oncol. 2003. p. 4214–21.
Santala M, Talvensaari-Mattila A. DNA ploidy is an independent prognostic indicador of overall survival in stage 1 endometrial endometrioid adenocarcinoma. Anticancer Res. 2005;23:5191–6.
Zaino RJ, Davis ATL, Ohlsson-Wilhelm BM, Brunetto VL. DNA content is an independent prognostic indicator in endometrial adenocarcinoma: a Gynecologic Oncology Group study. Int J Gynecol Pathol. 1998;17:312–9.
Slamon DJ, Clark GM, Wong SG, et al. Human breast cancer: correlation of relapse and survival with amplification of HER-2/neu oncogene. Science. 1987;235: 177–82.
Hellstrom I, Goodman G, Pullman J, et al. Overexpression of HER-2/neu in ovarian carcinomas. Cancer Res. 2001;61:2420–3.
Rolitsky CD, Theil KS, McGaughy VR, et al. HER-2/neu amplification and overexpression in endometrial carcinoma. Int J Gynecol Pathol. 1999;18:138–43.
Santin AD, Bellone S, Van Stedum S, et al. Determination of HER2/neu status in uterine serous papillary carcinoma: Comparative analysis of immunohistochemistry, and fluorescence in situ hybridisation. Gynecol Oncol. 2005;98:24–30.
Saffari B, Jones LA, el-Naggar A, et al. Amplification and overexpression of HER-2/neu (c-erbB2) in endometrial cancers: correlation with overall survival. Cancer Res. 1995;55:5695–8.
Kohlberger P, Loesch A, Koelbl B, et al. Prognostic value of immunohistochemically detected HER-2/neu oncoprotein in endometrial cancer. Cancer Lett. 1996;98: 151–5.
Riben MW, Malfetano JH, Nazeer T, et al. Identification of HER-2/neu oncogene amplification by fluorescence in situ hybridization in stage I endometrial carcinoma. Mod Pathol. 1997;10:823–31.
Rasty G, Murray R, Lu L et al. Expression of HER-2/neu oncogene in normal, hyperplastic, and malignant endometrium. Ann Clin Lab Sci. 1998;28:138–43.
Cianciulli AM, Guadagni F, Marzano R, et al. HER-2/neu oncogene amplification and chromosome 17 aneusomy in endometrial carcinoma: correlation with oncoprotein expression and conventional pathological parameters. J Exp Clin Cancer Res. 2003; 22:265–71.
Santin AD, Bellone S, Gokden M, et al. Overexpression of HER-2/neu in uterine serous papillary cancer. Clin Cancer Res. 2002;8:1271–9.
Slomovitz BM, Broaddus RR, Burke TW et al. Her-2/neu overexpression and 3126 amplification in uterine papillary serous carcinoma. J Clin Oncol. 2004;22:3132.
Mariani A, Sebo TH, Katzmann JA, et al. HER-2/neu overexpression and hormone dependency in endometrial cancer: analysis of cohort and review of literature. Anticancer Res. 2005;25:2921–7.
Backe J, Gassel AM, Krebs S, et al. Immunohistochemically detected HER-2/neu expression and prognosis in endometrial carcinoma. Arch Gynecol Obstet. 1997;259:189–95.
Williams JA, Wang ZR, Parrish RS, et al. Fluorescence in situ hybridization analysis of HER-2/neu, c-myc, and p53 in endometrial cancer. Exp Mol Pathol. 1999;67: 135–43.
Sivridis E. Angiogenesis and endometrial cancer. Anticancer Res. 2001;21:4383–8.
Guidi AJ, Abu-Jawdeh G, Tognazzi K, Dvorak HF, et al. Expression of vascular permeability factor (vascular endothelial growth factor) and its receptors in endometrial carcinoma. Cancer. 1996;78: 454–60.
Fujimoto J, Ichigo S, Hirose R, et al. Expression pression of vascular endothelial growth factor (VEGF) and its mRNA in uterine endometrial cancers. Cancer Lett. 1998; 134:15–22.
Seki N, Kodama J, Hongo A, et al. Vascular endotelial growth factor and platelet-derived endothelial cell growth factor expression are implicated in the angiogenesis of endometrial cancer. Eur J Cancer. 2000;36:68–73.
Mazurek A, Pierzynski P, Kuc P, et al. Evaluation of angiogenesis, p-53 tissue protein expression and serum VEGF in patients with endometrial cancer. Neoplasma. 2004;51:193–7.
Salvesen HB, Iversen OE, Akslen LA, Prognostic significance of angiogenesis and Ki-67, p53, and p21 expression: a population-based endometrial carcinoma study. J Clin Oncol. 1999;17:1382–90.
Ozuysal S, Bilgin T, Ozan H, et al. Angiogenesis in endometrial carcinoma: correlation with survival and clinicopathologic risk factors. Gynecol Onstet Invest. 2005; 55:175–7.
Ozalp S, Yalcin OT, Acikalin M, et al. Microvessel density (MVD) as a prognosticator in endometrial carcinoma. Eur J Gynaecol Oncol. 2003;24:305–8.
Giatromanolaki A, Sivridis E, Koukourakis MI, et al. Intratumoral angiogenesis: a new prognostic indicador for stage 1 endometrial adenocarcinomas? Oncol Res. 1999;11:205–12.
Sanseverino F, Santopietro R, Torricelli M, et al. PRb2/p130 and VEGF expression in endometrial carcinoma in relation to angiogenesis and histopathologic tumor grade. Cancer Biol The. 2006;5:84–8.
Fine BA, Valente PT, Feinstein GI, Dey T. VEGF, fit-1, and KDR/flk-1 as prognostic indicators in endometrial carcinoma. Gynecol Oncol. 2000;76:33–9.
Toyoki H, Fujimoto F, Sato E, et al. Clinical implications of expresion of cyclooxigenase-2 related to angiogenesis in uterine endometrial cancers. Ann Oncol. 2005;16:51–5.
Fujiwaki R, Lida K, Kanasaki H, et al. Cyclooxygenase-2 expression in endometrial cancer: correlation with microvessel count and expression of vascular endothelial growth factor and thymidine phosphorylase. Human Pathol. 2002;35: 213–9.
Ferrandina G, Legge F, Ranelletti FO, et al. Cyclooxygenase-2 expression in endometrial carcinoma: correlation with clinicopathologic parameters and clinical outcome. Cancer. 2002;95:801–7.
Maxwell GL, Risinger JI, Álvarez AA, Barret JC, Berechuck A. Favorable survival associated with microsatellite instability in endometrioid cancerx. Obstet Gynecol. 2001;84:209–17.
Saegusa M, Hashimura M, Yoshida T, et al. Beta-catenin mutations and aberrant nuclear expresión during endometrial tumorigenesis. Br J Cancer. 2001;84:209–17.
Lax SF, Kendaall B, Tashiro H, Slebos RJ, Hedrick L. The frequency of p53, K-ras mutations and microsatellite instability differs in uterine endometrioid and serous carcinoma: evidence o distinct molecular genetic pathways. Cancer. 2000; 88:814–24.
Lax SF, Pizer ES, Ronnett BM, Kurman RJ. Clear cell carcinoma of the endometrium is charactrized by a distinctive profile of p53, Ki-67, estrogen and progesterone receptor expression. Hum Pathol. 1998;29:551–8.
Khalifa MA, Mannel RS, Haraway SD, Walker J, Mi KW. Expression of EGFR, HER-2/neu, P53, and PCNA in endometrioid, serous papillary, and clear cell endometrial adenocarcinomas. Gynecol. Oncol. 1994;53:84–92.
Risinger JI, Maxwell GL, Chandramouli GV, et al. Microarray analysis reveals distinct gene expression profiles among different histologic types of endometrial cancer. Cancer Res. 2003;63:6–11.
Pallarés J, Martinez-Guitarte JL, Dolcet X, et al. Survivin expression in endometrial carcinoma: a tissue microarray study with correlation with PTEN and STAT-3. Int J Gynecol Pathol. 2003;24:247–53.
Santin AD, Zhan F, Cane S, et al. Gene expression fingerprint of uterine serous papillary carcinoma: identification of novel molecular markers for uterine serous cancer diagnosis and therapy. Br J Cancer. 2005;92:1561–73.
Salvesen HB, Akslen LA. Molecular pathogenesis and prognostic factors in endometrial carcinoma. APMIS. 2002;110: 673–89.
Von Minckwitz G, Loibl S, Brunnert K, et al. Adjuvant endocrine treatment with medroxyprogesterone acetate or tamoxifen in stage I and II endometrial cancer-a multi-centre, open, controlled prospectively randomised trial. Eur J Ca. 2002; 38:2265–71.
Ota T, Yoshida M, Kimura M, Kinoshita K. Clinicopathologic study of uterine endometrial carcinoma in young women aged 40 years and younger. Int J Gynecol Cancer 2005;15:657–62.
Barakat RR, Bundy BN, Spirtos NM, Bell J, Mannel RS. Randomized double-blind trial of estrogen replacement therapy versus placebo in stage I or II endometrial cancer: a Gynecologic Oncology Group Study. J Clin Oncol. 2006;24:587–92.
Nygren P, Sorbye H, Osterlund P, Pfeiffer P, Targeted drugs in metastatic colorectal cancer with special emphasis on guidelines for the use of bevacizumab and cetuximab. Acta Oncol. 2005;44:203–17.
Tsujii M, Kawano S, Tsuji S et al. Cyclo-oxygenase regulates angiogenesis induced by colon cancer cells. Cell. 1998;29: 705–16.
Mujoo K, Maneval DC, Anderson SC, Gutterman JU. Adenoviral mediated p53 tumor suppressor gene therapy of human ovarian carcinoma. Oncogene. 1996;12:1617–25.
Ramondetta L, Mills GB, Burke TW, Wolf JK. Adenovirus-mediated expression of p55 or p21 in a papillary serous endometrial carcinoma cell line (SPEC-2) results in both growth inhibition and apoptotic cell death: Potential application of gene therapy to endometrial cancer. Clin Cancer Res. 2000;6:278–84.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by an unrestricted educational grant by Bristol-Myers Squibb.
Rights and permissions
About this article
Cite this article
Cerezo, L., Cárdenes, H. & Michael, H. Molecular alterations in the pathogenesis of endometrial adenocarcinoma. Therapeutic implications. Clin Transl Oncol 8, 231–241 (2006). https://doi.org/10.1007/BF02664933
Issue Date:
DOI: https://doi.org/10.1007/BF02664933