Abstract
Early detection is critical to successful treatment of melanoma, and at-risk individuals often are educated about melanoma by showing them examples of symptom-free and highly symptomatic lesions. We explain why, according to principles of stimulus control, this common practice could discourage the detection of newly developed symptoms and present an experiment modeling the predicted effects. Using images depicting a continuum of melanoma symptom severity, we familiarized participants with a symptomatic lesion (S+), and then conducted generalization tests to determine how often they would label other degrees of symptom severity as the same as (unchanged from) S+. During training for a group that was modeled after typical melanoma education efforts, S- was an asymptomatic lesion. For passive and active control groups, respectively, S- was either absent or a more severely symptomatic lesion. In generalization tests, gradient shift occurred such that stimuli similar to S- were especially unlikely to be called “same.” For the target group, this resulted in reduced labeling of mildly symptomatic lesions as symptomatic. We discuss the implications of these findings for melanoma education efforts.





Similar content being viewed by others
Notes
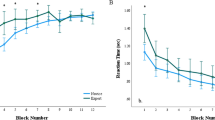
Following the generalization gradients of Fig. 2, it might be objected that using a moderately symptomatic lesion as S+ would result in patients overlooking highly symptomatic lesions (e.g., Fig. 2, right side of middle panel). Here, for two reasons, we suggest that parallels break down between our laboratory model and everyday circumstances. First, our stimuli were presented as abstract shapes, free of any experimentally provided cancer context. In the everyday world, people know about cancer and its potentially deadly consequences. Thus, unusual changes in the skin, once they are noticed, may be alarming. Second, physicians do not generally complain of patients being unable to recognize fairly advanced melanoma as unusual. These factors are likely to leave highly symptomatic lesions as easy to recognize. Of course, this proposition can be experimentally tested, in part by replicating our Standard Education procedures while describing the stimuli as related to skin cancer and modifying the response to explicitly identify possible instances of cancer.
References
Abbasi, N. R., Shaw, H. M., Rigel, D. S., Friedman, R. J., McCarthy, W. H., Osman, I., … Polsky, D. (2004). Early diagnosis of cutaneous melanoma. Journal of the American Medical Association, 292, 2771–2776. doi:10.1001/jama.292.22.2771.
Adams, C. K., Hall, D. C., Pennypacker, H. S., Goldstein, M. K., Hench, L. L., Madden, M. C., … Catania, A. C. (1976). Lump detection in simulated human breasts. Perception & Psychophysics, 20, 163–167. doi:10.3758/bf03198595.
Bizo, L. A., & McMahon, C. V. (2007). Temporal generalization and peak shift in humans. Learning & Behavior, 35, 123–130. doi:10.3758/bf03193047.
Bloom, H. S., Criswell, E. L., Pennypacker, H. S., Catania, A. C., & Adams, C. K. (1982). Major stimulus dimensions determining detection of simulated breast lesions. Perception & Psychophysics, 32, 251–260. doi:10.3758/bf03206229.
Blough, P. M. (1972). Wavelength generalization and discrimination in the pigeon. Perception & Psychophysics, 12, 342–348.
Boniol, M., Autier, P., Boyle, P., & Gandini, S. (2012). Cutaneous melanoma attributable to sunbed use: Systematic review and metaanalysis. British Medical Journal, 345, e4757. doi:10.1136/bmj.e4757.
Brady, M. S., Oliveria, S. A., Christos, P. J., Berwick, M., Coit, D. G., Katz, J., & Halpern, A. C. (2000). Patterns of detection in patients with cutaneous melanoma. Cancer, 89, 342–347. doi:10.1002/1097-0142(20000715)89:2<342::AID-CNCR19>3.0.CO;2-P.
Branstrom, R., Hedblad, M., Krakau, I., & Ullen, H. (2002). Laypersons’ perceptual discrimination of pigmented skin lesions. Journal of American Academy of Dermatology, 46, 667–673. doi:10.1067/mjd.2002.120463.
Dalianis, E. A., Critchfield, T. S., Howard, N. L., Jordan, J. S., & Derenne, A. (2011). Using morphed images to study visual detection of cutaneous melanoma symptom evolution. The Psychological Record, 61, 341–362.
Derenne, A. (2010). Shifts in postdiscrimination gradients within a stimulus dimension based on bilateral facial symmetry. Journal of the Experimental Analysis of Behavior, 93, 485–494. doi:10.1901/jeab. 2010.93-485.
Derenne, A., Breitstein, M., & Cicha, R. J. (2008). Shifts in postdiscrimination gradients within a stimulus dimension based on female waist-to-hip ratios. The Psychological Record, 58, 51–60.
Dinsmoor, J. A. (1995a). Stimulus control: Part I. The Behavior Analyst, 18, 51–68.
Dinsmoor, J. A. (1995b). Stimulus control: Part II. The Behavior Analyst, 18, 253–269.
Epstein, D. S., Lange, J. R., Gruber, S. B., Mofid, M., & Koch, S. E. (1999). Is physician detection associated with thinner melanomas? Journal of the American Medical Association, 281, 640–643. doi:10.1001/jama.281.7.640.
Fletcher, S. W., O’Malley, M. S., Earp, J. L., Morgan, T. W., Lin, S., & Degnan, D. (1990). How best to teach women breast self-examination: A randomized controlled trial. Annals of Internal Medicine, 112, 772–779. doi:10.7326/0003-4819-112-10-772.
Friedman, R. J., Rigel, D. S., & Kopf, A. W. (1985). Early detection of malignant melanoma: The role of physician examination and self-examination of the skin. CA: A Cancer Journal for Clinicians, 35, 130–151. doi:10.3322/canjclin.35.3.130.
Galizio, M. (1985). Human peak shift: Analysis of the effects of three-stimulus discrimination training. Learning & Motivation, 16, 478–494. doi:10.1016/0023-9690(85)90028-1.
Geller, A. C., Swetter, S. M., Oliveria, S., Dusza, S., & Halpern, A. C. (2011). Reducing mortality in individuals at high risk for advanced melanoma through education and screening. Journal of the American Academy of Dermatology, 65, S87.e1–S87.e9. doi:10.1016/j.jaad.2011.05.045.
Ghirlanda, S., & Enquist, M. (2003). A century of generalization. Animal Behaviour, 66, 15–36. doi:10.1006/anbe.2003.2174.
Girardi, S., Gaudy, C., Gouvernet, J., Teston, J., Richard, M. A., & Grob, J. J. (2006). Superiority of a cognitive education with photographs over ABCD criteria in the education of the general population to the early detection of melanoma: A randomized study. International Journal of Cancer, 118, 2276–2280. doi:10.1002/ijc.21351.
Goodson, A. G., & Grossman, D. (2008). Strategies for early melanoma detection: Approaches to the patient with nevi. Journal of the American Academy of Dermatology, 60, 719–735. doi:10.1016/j.jaad.2008.10.065.
Guttman, N., & Kalish, H. I. (1956). Discriminability and stimulus generalization. Journal of Experimental Psychology, 51, 79–88. doi:10.1037/h0046219.
Guy, G. P., Berkowitz, Z., Watson, M., Holman, D. M., & Richardson, L. C. (2013). Indoor tanning among young non-Hispanic white females. JAMA Internal Medicine, 173(20), 1920–1922. doi:10.1001/jamainternmed.2013.10013.
Hamidi, R., Peng, D., & Cockburn, M. (2010). Efficacy of skin self-examination for the early detection of melanoma. International Journal of Dermatology, 49, 126–134. doi:10.1111/j.1365-4632.2009.04268.x.
Hanson, H. M. (1959). Effects of discrimination training on stimulus generalization. Journal of Experimental Psychology, 58, 321–334. doi:10.1037/h0042606.
Honig, W. K., & Urcuioli, P. J. (1981). The legacy of Guttman and Kalish (1956): 25 years of research on stimulus generalization. Journal of the Experimental Analysis of Behavior, 36, 405–445. doi:10.1901/jeab. 1981.36-405.
Howlader, N., Noone, A. M., Krapcho, M., Garshell, J., Miller, D., Altekruse, S. F., ... Cronin, K. A. (eds) (2013). SEER Cancer Statistics Review, 1975–2011. Retrieved from National Cancer Institute website http://seer.cancer.gov/csr/1975_2011/.
Karakousis, G. C., & Czerniecki, B. J. (2011). Diagnosis of melanoma. PET Clinics, 6, 1–8. doi:10.1016/j.cpet.2011.02.001.
Kasparian, N. A., McLoone, J. K., & Meiser, B. (2009). Skin cancer-related prevention and screening behaviors: A review of the literature. Journal of Behavioral Medicine, 32, 406–428. doi:10.1007/s10865-009-9219-2.
Lamerson, C. L., Eaton, K., Sax, J. L., & Kashani-Sabet, M. (2012). Comparing melanoma invasiveness in dermatologist-versus patient-detected lesions: A retrospective chart review. Journal of Skin Cancer, 2012, 1–5. doi:10.1155/2012/187963.
Liu, W., Hill, D., Gibbs, A. F., Tempany, M., Howe, C., Borland, R., … Kelly, J. W. (2005). What features do patients notice that help to distinguish between benign pigmented lesions and melanomas?: The ABCD(E) rule versus the seven-point checklist. Melanoma Research, 15, 549–554. doi:10.1097/00008390-200512000-00011.
McGuire, S. T., Secrest, A. M., Andrulonis, R., & Ferris, L. K. (2011). Surveillance of patients for early detection of melanoma: Patterns in dermatologist vs patient discovery. Archives of Dermatology, 147, 673–678. doi:10.1001/archdermatol.2011.135.
McPherson, M., Elwood, M., English, D. R., Baade, P. D., Youl, P. H., & Aitken, J. F. (2006). Presentation and detection of invasive melanoma in a high-risk population. Journal of the American Academy of Dermatology, 54, 783–792. doi:10.1016/j.jaad.2005.08.065.
McWhirter, J. E., & Hoffman-Goetz, L. (2013). Visual images for skin self-examination and melanoma detection: A review of published studies. Journal of the American Academy of Dermatology, 69, 47–55. doi:10.1016/j.jaad.2013.01.031.
Miles, F., & Meehan, J. W. (1995). Visual discrimination of pigmented skin lesions. Health Psychology, 14, 171–177. doi:10.1037/0278-6133.14.2.171.
Miller, D. R., Geller, A. C., Wyatt, S. W., Halpern, A., Howell, J., Cockerell, C., … Rosenthal, L. (1996). Melanoma awareness and self-examination practices: Results of a United States survey. Journal of the American Academy of Dermatology, 34, 962–970. doi:10.1016/s0190-9622(96)90273-x.
National Cancer Institute (2014). SEER stat fact sheets: Melanoma of the skin. Retrieved from http://seer.cancer.gov/statfacts/html/melan.html. Accessed 1 June 2014.
O’Malley, M. S. (1993). Cost effectiveness of two nurse-led programs to teach breast self-examination. American Journal of Preventive Medicine, 9(3), 139–145.
Pollitt, R. A., Geller, A. C., Brooks, D. R., Johnson, T. M., Park, E. R., & Swetter, S. M. (2009). Efficacy of skin self-examination practices for early melanoma detection. Cancer Epidemiology, Biomarkers & Prevention, 18, 3018–3023. doi:10.1158/1055-9965.EPI-09-0310.
Richard, M. A., Grob, J. J., Avril, M. F., Delaunay, M., Gouvernet, J., Wolkenstein, P., … Dalac, S. (2000). Delays in diagnosis and melanoma prognosis (I): The role of patients. International Journal of Cancer, 89, 271–279. doi:10.1002/1097-0215(20000520)89:3<271::aid-ijc10>3.0.co;2-7.
Rigel, D. S., & Carucci, J. A. (2000). Malignant melanoma: Prevention, early detection, and treatment in the 21st century. CA: A Cancer Journal for Clinicians, 50(4), 215–236. doi:10.3322/canjclin.50.4.215.
Saunders, K. J., Pilgrim, C. A., & Pennypacker, H. S. (1986). Increased proficiency of search in breast self-examination. Cancer, 58, 2531–2537.
Schwartz, J. L., Wang, T. S., Hamilton, T. A., Lowe, L., Sondak, V. K., & Johnson, T. M. (2002). Thin primary cutaneous melanomas. Cancer, 95, 1562–1568. doi:10.1002/cncr.10880.
Spetch, M., Cheng, K., & Clifford, C. (2004). Peak shift but not range effects in recognition of faces. Learning and Motivation, 35, 221–241. doi:10.1016/j.lmot.2003.11.001.
Terrace, H. S. (1963). Discrimination learning with and without “errors”. Journal of the Experimental Analysis of Behavior, 6(1), 1–27. doi:10.1901/jeab.1963.6-1.
Titus, L. J., Clough-Gorr, K., Mackenzie, T. A., Perry, A., Spencer, S. K., Weiss, J., … Ernstoff, M. S. (2012). Recent skin self-examination and doctor visits in relation to melanoma risk and tumour depth. British Journal of Dermatology, 168, 571–576. doi:10.1111/bjd.12003.
U.S. Preventive Services Task Force (2009). Screening for skin cancer. Retrieved from http://www.uspreventiveservicestaskforce.org/uspstf/uspsskca.htm.
Weinstock, M. A., Martin, R. A., Risica, P. M., Berwick, M., Lasater, T., Rakowski, W., … Dubé, C. E. (1999). Thorough skin examination for the early detection of melanoma. American Journal of Preventive Medicine, 17, 169–175. doi:10.1016/S0749-3797(99)00077-X.
Yagerman, S., & Marghoob, A. (2013). Melanoma patient self-detection: A review of the efficacy of skin self-examination and patient directed educational efforts. Review of Anticancer Therapy, 1312, 1423–1431. doi:10.1586/14737140.2013.856272.
Acknowledgments
Portions of this study were completed in partial fulfillment of the first author’s doctoral degree requirements at the University of Kansas. The authors express sincere gratitude to Kathryn Saunders, David Jarmolowicz, Steven Fawcett, and Kimberly Engelman for their comments on the design and analysis of this study.
This investigation was supported by the University of Kansas New Faculty General Research Fund allocation #2302290 and General Research Fund allocation #2301722.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Miller, J.R., Reed, D.D. & Critchfield, T.S. Modeling the Effects of Melanoma Education on Visual Detection: A Gradient Shift Analysis. Psychol Rec 65, 323–335 (2015). https://doi.org/10.1007/s40732-014-0108-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40732-014-0108-x