Abstract
Introduction
Enzalutamide is a novel antiandrogen which is approved for the treatment of metastatic, castration-resistant prostate cancer (mCRPC) after taxane-based chemotherapy. The efficacy of enzalutamide after the sequence docetaxel and abiraterone is not proven.
Methods
Thirty-five mCRPC patients in the German compassionate use program, who received enzalutamide after progression with taxane-based chemotherapy and abiraterone were prospectively evaluated. The endpoints of the study were overall survival, radiologic progression-free survival and safety.
Results
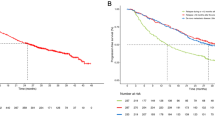
The median treatment duration on enzalutamide was 2.8 months. The median overall survival was 7.5 months [95% confidence interval (CI) 4.7–10.3] while median progression-free survival assessed by imaging was 3.1 months (95% CI 1.4–4.8). The most common toxicities of all grades were anemia and weight loss.
Conclusion
Although the results are limited by a small patient number, the consecutive use of enzalutamide and abiraterone after taxane-based chemotherapy shows a modest clinical activity. Thus, sequence therapy alternating between chemotherapy and antihormonal drugs might be a more promising approach in mCRPC treatment.



Similar content being viewed by others
References
Berthold DR, Pond GR, Soban F, de Wit R, Eisenberger M, Tannock IF. Docetaxel plus prednisone or mitoxantrone plus prednisone for advanced prostate cancer: updated survival in the TAX 327 study. J Clin Oncol. 2008;26(2):242–5. doi:10.1200/jco.2007.12.4008.
Fizazi K, Scher HI, Molina A, Logothetis CJ, Chi KN, Jones RJ, Staffurth JN, North S, Vogelzang NJ, Saad F, Mainwaring P, Harland S, Goodman OB Jr, Sternberg CN, Li JH, Kheoh T, Haqq CM, de Bono JS, C-A- Investigators. Abiraterone acetate for treatment of metastatic castration-resistant prostate cancer: final overall survival analysis of the COU-AA-301 randomised, double-blind, placebo-controlled phase 3 study. Lancet Oncol. 2012;13(10):983–92. doi:10.1016/S1470-2045(12)70379-0.
Ryan CJ, Smith MR, de Bono JS, Molina A, Logothetis CJ, de Souza P, Fizazi K, Mainwaring P, Piulats JM, Ng S, Carles J, Mulders PF, Basch E, Small EJ, Saad F, Schrijvers D, Van Poppel H, Mukherjee SD, Suttmann H, Gerritsen WR, Flaig TW, George DJ, Yu EY, Efstathiou E, Pantuck A, Winquist E, Higano CS, Taplin ME, Park Y, Kheoh T, Griffin T, Scher HI, Rathkopf DE, C-A- Investigators. Abiraterone in metastatic prostate cancer without previous chemotherapy. N Engl J Med. 2013;368(2):138–48. doi:10.1056/NEJMoa1209096.
de Bono JS, Oudard S, Ozguroglu M, Hansen S, Machiels JP, Kocak I, Gravis G, Bodrogi I, Mackenzie MJ, Shen L, Roessner M, Gupta S, Sartor AO. Prednisone plus cabazitaxel or mitoxantrone for metastatic castration-resistant prostate cancer progressing after docetaxel treatment: a randomised open-label trial. Lancet. 2010;376(9747):1147–54. doi:10.1016/s0140-6736(10)61389-x.
Jung ME, Ouk S, Yoo D, Sawyers CL, Chen C, Tran C, Wongvipat J. Structure-activity relationship for thiohydantoin androgen receptor antagonists for castration-resistant prostate cancer (CRPC). J Med Chem. 2010;53(7):2779–96. doi:10.1021/jm901488g.
Tran C, Ouk S, Clegg NJ, Chen Y, Watson PA, Arora V, Wongvipat J, Smith-Jones PM, Yoo D, Kwon A, Wasielewska T, Welsbie D, Chen CD, Higano CS, Beer TM, Hung DT, Scher HI, Jung ME, Sawyers CL. Development of a second-generation antiandrogen for treatment of advanced prostate cancer. Science (New York, NY). 2009;324(5928):787–90. doi:10.1126/science.1168175.
Scher HI, Fizazi K, Saad F, Taplin ME, Sternberg CN, Miller K, de Wit R, Mulders P, Chi KN, Shore ND, Armstrong AJ, Flaig TW, Flechon A, Mainwaring P, Fleming M, Hainsworth JD, Hirmand M, Selby B, Seely L, de Bono JS. Increased survival with enzalutamide in prostate cancer after chemotherapy. N Engl J Med. 2012;367(13):1187–97. doi:10.1056/NEJMoa1207506.
Therasse P, Arbuck SG, Eisenhauer EA, Wanders J, Kaplan RS, Rubinstein L, Verweij J, Van Glabbeke M, van Oosterom AT, Christian MC, Gwyther SG. New guidelines to evaluate the response to treatment in solid tumors. European Organization for Research and Treatment of Cancer, National Cancer Institute of the United States, National Cancer Institute of Canada. J Natl Cancer Inst. 2000;92(3):205–16.
Institute NC. Common Terminology Criteria for Adverse Events v4.0 NIH publication # 09-7473 (2009).
Schrader AJ, Boegemann M, Ohlmann CH, Schnoeller TJ, Krabbe LM, Hajili T, Jentzmik F, Stoeckle M, Schrader M, Herrmann E, Cronauer MV. Enzalutamide in castration-resistant prostate cancer patients progressing after docetaxel and abiraterone. Eur Urol. 2013;. doi:10.1016/j.eururo.2013.06.042.
Loriot Y, Bianchini D, Ileana E, Sandhu S, Patrikidou A, Pezaro C, Albiges L, Attard G, Fizazi K, De Bono JS, Massard C. Antitumour activity of abiraterone acetate against metastatic castration-resistant prostate cancer progressing after docetaxel and enzalutamide (MDV3100). Ann Oncol. 2013;24(7):1807–12. doi:10.1093/annonc/mdt136.
Noonan KL, North S, Bitting RL, Armstrong AJ, Ellard SL, Chi KN. Clinical activity of abiraterone acetate in patients with metastatic castration-resistant prostate cancer progressing after enzalutamide. Ann Oncol. 2013;24(7):1802–7. doi:10.1093/annonc/mdt138.
Mostaghel EA, Marck BT, Plymate SR, Vessella RL, Balk S, Matsumoto AM, Nelson PS, Montgomery RB. Resistance to CYP17A1 inhibition with abiraterone in castration-resistant prostate cancer: induction of steroidogenesis and androgen receptor splice variants. Clin Cancer Res. 2011;17(18):5913–25. doi:10.1158/1078-0432.CCR-11-0728.
Li Y, Chan SC, Brand LJ, Hwang TH, Silverstein KA, Dehm SM. Androgen receptor splice variants mediate enzalutamide resistance in castration-resistant prostate cancer cell lines. Cancer Res. 2013;73(2):483–9. doi:10.1158/0008-5472.CAN-12-3630.
Albiges L, Le Moulec S, Loriot Y, Gross Goupil M, De La Motte Rouge T, Guillot A, Fizazi K, Massard C. Response to cabazitaxel in the postchemotherapy setting in CRPC patients previously treated with docetaxel and abiraterone acetate. Ann Oncol. 2012;23(Suppl 9):S294–S318.
Fitzpatrick JM, de Wit R. Taxane mechanisms of action: potential implications for treatment sequencing in metastatic castration-resistant prostate cancer. Eur Urol. 2013;. doi:10.1016/j.eururo.2013.07.022.
Acknowledgments
We thank Brigitta Grau, Tanja Gröber and Manel Stiasny for their support and of course the patients with their families.
Conflict of interest
No funding or sponsorship was received for this study or publication of this article. Dr. Schmid received lecture fees from Astellas Pharma GmbH and travel grants from GlaxoSmithKline GmbH & Co. KG.
Dr. von Klot received lecture fees from Janssen-Cilag GmbH. Prof. Gschwend received lecture fees and honoraria from Astellas Pharma GmbH, Janssen-Cilag GmbH, Pfizer GmbH, Bayer AG, Amgen GmbH, Novartis AG, Roche GmbH, and GlaxoSmithKline GmbH & Co. KG.
Prof. Kuczyk received lecture fees and honoraria from Astellas Pharma GmbH, Janssen-Cilag GmbH, Novartis Pharma, Pfizer GmbH, Bayer AG and GlaxoSmithKline GmbH & Co. KG.
Prof. Merseburger received lecture fees and honoraria from Astellas Pharma GmbH, Janssen-Cilag GmbH, Novartis Pharma, Pfizer GmbH, Bayer AG and GlaxoSmithKline GmbH & Co. KG.
Prof. Retz received lecture fees and honoraria from Astellas Pharma GmbH, Janssen-Cilag GmbH, Pfizer GmbH, Bayer AG and GlaxoSmithKline GmbH & Co. KG. Mr. Geith, Mrs. Boker, Dr. Tauber and Dr. Seitz declare no conflict of interest.
Compliance with ethics guidelines
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000 and 2008. Informed consent was obtained from all patients for being included in the study.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Schmid, S.C., Geith, A., Böker, A. et al. Enzalutamide After Docetaxel and Abiraterone Therapy in Metastatic Castration-Resistant Prostate Cancer. Adv Ther 31, 234–241 (2014). https://doi.org/10.1007/s12325-014-0092-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-014-0092-1