Abstract
Purpose
To identify factors associated with decisions to withdraw life-sustaining therapies in patients with severe traumatic brain injury (TBI).
Materials and Methods
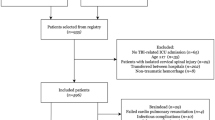
We conducted a 2-year multicenter retrospective cohort study (2005–2006) in mechanically ventilated patients aged 16 years and older admitted to the intensive care units (ICUs) of six Canadian level I trauma centers following severe TBI. One hundred and twenty charts were randomly selected at each center (n = 720). Data on ICU management strategies, patients’ clinical condition, surgical procedures, diagnostic imaging, and decision to withdraw life-sustaining therapies were collected. The association of factors pertaining to the injury, interventions, and management strategies with decisions to withdraw life-sustaining therapies was evaluated among non-survivors.
Results
Among the 228 non-survivors, 160 died following withdrawal of life-sustaining therapies. Patients were predominantly male (69.7 %) with a mean age of 50.7 (±21.7) years old. Brain herniation was more often reported in patients who died following decisions to withdraw life-sustaining therapies (odds ratio [OR] 2.91, 95 % confidence interval [CI] 1.16–7.30, p = 0.02) compared to those who died due to other causes (e.g., cardiac arrest, shock, etc.). Epidural hematomas (OR 0.18, 95 % CI 0.06–0.56, p < 0.01), craniotomies (OR 0.12, 95 % CI 0.02–0.68, p = 0.02), and other non-neurosurgical procedures (OR 0.08, 95 % CI 0.02–0.43, p < 0.01) were less often associated with death following withdrawal of life-sustaining therapies than death from other causes.
Conclusions
Death following decisions to withdraw life-sustaining therapies is associated with specific patient and clinical factors, and the intensity of care.
Similar content being viewed by others
References
National Scientific Advisory Committee. Identifying priorities for research and capacity development in injury as a multi-institute strategic initiative within the Canadian Institutes of Health Research. In: Listening for direction on injury: final report Instituts canadiens de recherche en santé; 2004.
Coronado VG, Xu L, Basavaraju SV, et al. Surveillance for traumatic brain injury-related deaths—United States, 1997–2007. MMWR Surveill Summ. 2011;60:1–32.
Masson F, Thicoipe M, Aye P, et al. Epidemiology of severe brain injuries: a prospective population-based study. J Trauma. 2001;51:481–9.
Murray GD, Teasdale GM, Braakman R, et al. The European Brain Injury Consortium survey of head injuries. Acta Neurochir (Wien). 1999;141:223–36.
Myburgh JA, Cooper DJ, Finfer SR, et al. Epidemiology and 12-month outcomes from traumatic brain injury in Australia and New Zealand. J Trauma. 2008;64:854–62.
Spronk PE, Kuiper AV, Rommes JH, Korevaar JC, Schultz MJ. The practice of and documentation on withholding and withdrawing life support: a retrospective study in two Dutch intensive care units. Anesth Analg. 2009;109:841–6.
Cooper Z, Rivara FP, Wang J, MacKenzie EJ, Jurkovich GJ. Withdrawal of life-sustaining therapy in injured patients: variations between trauma centers and nontrauma centers. J Trauma. 2009;66:1327–35.
Azoulay E, Metnitz B, Sprung CL, et al. End-of-life practices in 282 intensive care units: data from the SAPS 3 database. Intensive Care Med. 2009;35:623–30.
Zahuranec DB, Morgenstern LB, Sanchez BN, Resnicow K, White DB, Hemphill JC III. Do-not-resuscitate orders and predictive models after intracerebral hemorrhage. Neurology. 2010;75:626–33.
Rocker G, Cook D, Sjokvist P, et al. Clinician predictions of intensive care unit mortality. Crit Care Med. 2004;32:1149–54.
Becker KJ, Baxter AB, Cohen WA, et al. Withdrawal of support in intracerebral hemorrhage may lead to self-fulfilling prophecies. Neurology. 2001;56:766–72.
Rocker GM, Cook DJ, Shemie SD. Brief review: practice variation in end of life care in the ICU: implications for patients with severe brain injury. Can J Anaesth. 2006;53:814–9.
O’Callahan JG, Fink C, Pitts LH, Luce JM. Withholding and withdrawing of life support from patients with severe head injury. Crit Care Med. 1995;23:1567–75.
Turgeon AF, Lauzier F, Simard JF, et al. Mortality associated with withdrawal of life-sustaining therapy for patients with severe traumatic brain injury: a Canadian multicentre cohort study. CMAJ. 2011;183:1581–8.
Varelas PN, Abdelhak T, Hacein-Bey L. Withdrawal of life-sustaining therapies and brain death in the intensive care unit. Semin Neurol. 2008;28:726–35.
Cook D, Rocker G, Marshall J, et al. Withdrawal of mechanical ventilation in anticipation of death in the intensive care unit. N Engl J Med. 2003;349:1123–32.
Esteban A, Gordo F, Solsona JF, et al. Withdrawing and withholding life support in the intensive care unit: a Spanish prospective multi-centre observational study. Intensive Care Med. 2001;27:1744–9.
Diringer MN, Edwards DF, Aiyagari V, Hollingsworth H. Factors associated with withdrawal of mechanical ventilation in a neurology/neurosurgery intensive care unit. Crit Care Med. 2001;29:1792–7.
Ferrand E, Robert R, Ingrand P, Lemaire F. Withholding and withdrawal of life support in intensive-care units in France: a prospective survey. French LATAREA Group. Lancet. 2001;357:9–14.
Mayer SA, Kossoff SB. Withdrawal of life support in the neurological intensive care unit. Neurology. 1999;52:1602–9.
Keenan SP, Busche KD, Chen LM, McCarthy L, Inman KJ, Sibbald WJ. A retrospective review of a large cohort of patients undergoing the process of withholding or withdrawal of life support. Crit Care Med. 1997;25:1324–31.
Thompson HJ, Rivara FP, Jurkovich GJ, Wang J, Nathens AB, MacKenzie EJ. Evaluation of the effect of intensity of care on mortality after traumatic brain injury. Crit Care Med. 2008;36:282–90.
Perel P, Arango M, Clayton T, et al. Predicting outcome after traumatic brain injury: practical prognostic models based on large cohort of international patients. BMJ. 2008;336:425–9.
Murray GD, Butcher I, McHugh GS, et al. Multivariable prognostic analysis in traumatic brain injury: results from the IMPACT study. J Neurotrauma. 2007;24:329–37.
Steyerberg EW, Mushkudiani N, Perel P, et al. Predicting outcome after traumatic brain injury: development and international validation of prognostic scores based on admission characteristics. PLoS Med. 2008;5:e165. discussion e165;1251–61.
Harrell FE Jr, Lee KL, Califf RM, Pryor DB, Rosati RA. Regression modelling strategies for improved prognostic prediction. Stat Med. 1984;3:143–52.
Brain Trauma Foundation. Guidelines for the Surgical Management of Traumatic Brain Injury. Neurosurgery. 2006;58:S2-1–3.
Brain Trauma Foundation. Early indicators of prognosis in severe traumatic brain injury. In: Management and prognosis of severe traumatic brain injury. American Association of Neurological Surgeons; 2000.
Brain Trauma Foundation. Guidelines for the Management of Severe Traumatic Brain Injury. 3rd ed. New York: Brain Trauma Foundation; 2007.
Ratnapalan M, Cooper AB, Scales DC, Pinto R. Documentation of best interest by intensivists: a retrospective study in an Ontario Critical Care Unit. BMC Med Ethics. 2010;11:1–7.
Wilkinson D. The self-fulfilling prophecy in intensive care. Theor Med Bioeth. 2009;30:401–10.
Ho KM, Liang J. Withholding and withdrawal of therapy in New Zealand intensive care units (ICUs): a survey of clinical directors. Anaesth Intensive Care. 2004;32:781–6.
Acknowledgments
The authors would like to thank Tran Cong Dung MD, MSc; Mohana Ratnapalan HBSc, Stephanie Todd BSc, MBT, John Harlock MD, Frédéric Morin RN and David Simonyan MD MSc, for their help in data acquisition; Valérie Murat MSc for her participation in the data cleaning process; Mrs. Valérie Boucher for her secretarial assistance. This work was presented in part at the Intensive Care and Emergency Medicine Symposium (Brussels, Belgium, March 2011). The work was supported in part by the Fondation de l’Hôpital de l’Enfant-Jésus (Enfant-Jésus Hospital Foundation) who had no role in any part of conduct of the study or preparation of the manuscript. Drs. Turgeon and Lauzier are recipients of a Research Career Award from the Fonds de Recherche Québec-Santé (FRQ-S). Drs. Moore, Scales, and Fergusson are recipients of New Investigator Awards from the Canadian Institutes for Health Research (CIHR). Dr. Zarychanski is a recipient of a CIHR RCT Mentorship Award. Dr. Burns holds a Clinician Scientist Phase 2 Award from the CIHR.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was performed in six level I trauma centers in Canada: Québec (Centre Hospitalier Affilié Universitaire de Québec—Hôpital de l’Enfant-Jésus, Hôpital du Sacré-Coeur de Montréal), Ontario (Hamilton General Hospital, Sunnybrook Health Science Centre, St-Michael’s Hospital); Alberta (Foothill Medical Centre).
Rights and permissions
About this article
Cite this article
Côte, N., Turgeon, A.F., Lauzier, F. et al. Factors Associated with the Withdrawal of Life-Sustaining Therapies in Patients with Severe Traumatic Brain Injury: A Multicenter Cohort Study. Neurocrit Care 18, 154–160 (2013). https://doi.org/10.1007/s12028-012-9787-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-012-9787-9