Abstract
Background
As life expectancy increases, more elderly patients fit into the criteria for bariatric procedures. The aim of our study is to evaluate and compare the safety and efficacy of Roux-en-Y gastric bypass (RYGB), laparoscopic sleeve gastrectomy (LSG), and laparoscopic adjustable gastric banding (LAGB) in patients older than 60.
Material and Methods
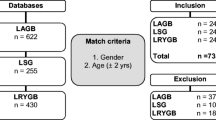
Between January 2005 and December 2013, 68 LAGB, 73 LSG, and 212 RYGB patients were 60 years or older at the time of primary procedure. A retrospective review was performed in these patients.
Results
Mean age and body mass index (BMI) was 62.7 ± 2.2, 64.1 ± 2.9, and 62.6 ± 2.3 years and 42.7 ± 5.6, 44.0 ± 7.0, and 45.2 ± 6.7 kg/m2 for LAGB, LSG, and RYGB at the time of procedure, respectively.
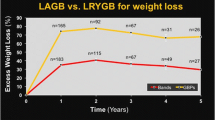
Seven (10.3 %) patients from the LAGB, 3 (4.1 %) from the LSG, and 29 (13.8 %) from the RYGB group required readmissions. Reoperation rate was 10.3, 1.4, and 9.5 % in LAGB, LSG, and RYGB, respectively. The difference in reoperation rates was statistically significant (p < 0.03) while that in readmission rates was not (p > 0.58). Procedure-related mortality rate was 1.4 % in the RYGB group, while no mortality was observed in LSG and LAGB groups. At 6, 12, and 18 months postoperatively, mean percentage of excess weight loss were highest in the RYGB group, followed by LSG and LAGB group (p < 0.01). Mean number of comorbidities at the last follow-up significantly decreased in LSG and RYGB patients.
Conclusions
LSG showed the lowest readmission and reoperation rate, and RYGB patients had the highest mortality rate. Weight loss and comorbidity resolution were effectively achieved in RYGB and LSG patients.

Similar content being viewed by others
References
Arias E. United States life tables, 2010. Natl Vital Stat Rep. 2014;63:1–63.
Kuehn BM. US longevity falls short vs that of peer countries. JAMA. 2013;309:534.
Solomon CG, Manson JE. Obesity and mortality: a review of the epidemiologic data. Am J Clin Nutr. 1997;66:1044S–50S.
Nelson LG, Lopez PP, Haines K, et al. Outcomes of bariatric surgery in patients > or = 65 years. Surg Obes Relat Dis. 2006;2:384–8.
Livingston EH, Langert J. The impact of age and medicare status on bariatric surgical outcomes. Arch Surg. 2006;141:1115–20.
Trieu HT, Gonzalvo JP, Szomstein S, et al. Safety and outcomes of laparoscopic gastric bypass surgery in patients 60 years of age and older. Surg Obes Relat Dis. 2007;3:383–6.
Papasavas PK, Gagne DJ, Kelly J, et al. Laparoscopic Roux-en-Y gastric bypass is a safe and effective operation for the treatment of morbid obesity in patients older than 55 years. Obes Surg. 2004;14:1056–61.
Mizrahi I, Alkurd A, Ghanem M, et al. Outcomes of laparoscopic sleeve gastrectomy in patients older than 60 years. Obes Surg. 2014;24:855–60.
Spaniolas K, Trus TL, Adrales GL, et al. Early morbidity and mortality of laparoscopic sleeve gastrectomy and gastric bypass in the elderly: a NSQIP analysis. Surg Obes Relat Dis. 2014;10:584–8.
DuCoin C, Moon RC, Teixeira AF, et al. Laparoscopic choledochoduodenostomy as an alternate treatment for common bile duct stones after Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2014;10:647–52.
Flum DR, Salem L, Elrod JA, et al. Early mortality among medicare beneficiaries undergoing bariatric surgical procedures. JAMA. 2005;294:1903–8.
Silecchia G, Greco F, Bacci V, et al. Results after laparoscopic adjustable gastric banding in patients over 55 years of age. Obes Surg. 2005;15:351–6.
Giordano S, Victorzon M. Laparoscopic Roux-en-Y gastric bypass is effective and safe in over 55-year-old patients: a comparative analysis. World J Surg. 2014;38:1121–6.
Clough A, Layani L, Shah A, et al. Laparoscopic gastric banding in over 60s. Obes Surg. 2011;21:10–7.
Willkomm CM, Fisher TL, Barnes GS, Kennedy CI, Kuhn JA. Surgical weight loss > 65 years old: is it worth the risk? Surg Obes Relat Dis 2010;491–7.
Luppi CR, Balague C, Targarona EM, et al. Laparoscopic sleeve gastrectomy in patients over 60 years: impact of age on weight loss and co-morbidity improvement. Surg Obes Relat Dis. 2015;11:296–301.
Busetto L, Angrisani L, Basso N, et al. Safety and efficacy of laparoscopic adjustable gastric banding in the elderly. Obesity (Silver Spring). 2008;16:334–8.
Lynch J, Belgaumkar A. Bariatric surgery is effective and safe in patients over 55: a systemic review and meta-analysis. Obes Surg. 2012;22:1507–16.
Taylor CJ, Layani L. Laparoscopic adjustable gastric banding in patients ≥60 years old: is it worthwhile? Obes Surg. 2006;16:1579–83.
Qin C, Luo B, Aggarwal A, et al. Advanced age as an independent predictor of perioperative risk after laparoscopic sleeve gastrectomy (LSG). Obes Surg. 2015;25:406–12.
Wittgrove AC, Martinez T. Laparoscopic gastric bypass in patients 60 years and older: early postoperative morbidity and resolution of comorbidities. Obes Surg. 2009;19:1472–6.
Musella M, Milone M, Maietta P, et al. Bariatric surgery in elderly patients. A comparison between gastric banding and sleeve gastrectomy with five years of follow up. Int J Surg. 2014;12:S69–72.
Quebbemann B, Engstrom D, Siegfried T, et al. Bariatric surgery in patients older than 65 years is safe and effective. Surg Obes Relat Dis. 2005;1:389–93.
O’Keefe KL, Kemmeter PR, Kemmeter KD. Bariatric surgery outcomes in patients aged 65 years and older at an American Society for Metabolic and Bariatric Surgery Center of Excellence. Obes Surg. 2010;20:1199–205.
Ramirez A, Roy M, Hidalgo JE, et al. Outcomes of bariatric surgery in patients >70 years old. Surg Obes Relat Dis. 2012;8:458–62.
Conflict of Interest
The authors declare that they have no competing interests.
Ethical Approval
For this type of study, formal consent is not required.
Informed Consent
Informed consent was waived by the local IRB as this is a retrospective study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Moon, R.C., Kreimer, F., Teixeira, A.F. et al. Morbidity Rates and Weight Loss After Roux-en-Y Gastric Bypass, Sleeve Gastrectomy, and Adjustable Gastric Banding in Patients Older Than 60 Years old: Which Procedure to Choose?. OBES SURG 26, 730–736 (2016). https://doi.org/10.1007/s11695-015-1824-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-015-1824-2