Abstract
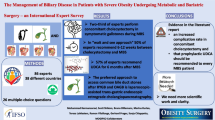
Background
The surgical management of complex or morbid obesity is increasing exponentially. Laparoscopic procedures are being increasingly utilized due to their similar efficacy but shorter hospital stay and faster convalescence when compared with open surgery. Despite this, many patients remain in hospital for a number of days after laparoscopic obesity surgery due to concerns about potential sequelae. We present the results of our simplified fast-track service, designed to enable discharge of all patients on postoperative day one following laparoscopic Roux-en-Y gastric bypass (LRYGB).
Methods
All patients operated on by a single surgeon during a 3-year period underwent fast-track management and were included. Our simplified fast-track service has three components; it is applicable to all patients, patients are counselled regarding fast-track discharge and the only routine postoperative investigations are full blood count and serum C-reactive protein (CRP). CRP was investigated as a prognosticator for complications following LRYGB.
Results
One hundred twelve patients underwent a LRYGB during the study period (35 male, median age 44 [18–73], median BMI 49.4 [36.5–75.0]). Ninety-eight patients (87.5 %) were discharged the day after LRYGB. Five patients developed postoperative complications (three major, two minor). One patient required readmission following discharge on postoperative day 1. A CRP greater than 100 mg/L on postoperative day 1 was found to predict major complications with 100 % sensitivity and 95 % specificity with a diagnostic accuracy of 0.98.
Conclusion
Our simplified fast-track LRYGB service allows the vast majority of patients to be safely and successfully discharged on postoperative day 1.




Similar content being viewed by others
References
Burns EM, Naseem H, Bottle A, et al. Introduction of laparoscopic bariatric surgery in England: observational population cohort study. BMJ. 2010;341:c4296.
Colquitt JL, Clegg AJ, Loveman E, et al. Surgery for morbid obesity. Chichester: Wiley; 2010.
Bamgbade OA, Adeogun BO, Abbas K. Fast-track laparoscopic gastric bypass surgery: outcomes and lessons from a bariatric surgery service in the United Kingdom. Obes Surg. 2012;22:398–402.
Fazylov R, Soto E, Merola S. Laparoscopic Roux-en-Y gastric bypass in morbidly obese patients > or = 55 years old. Obes Surg. 2008;18:656–9.
Collins J, Mattar S, Qureshi F, et al. Initial outcomes of laparoscopic Roux-en-Y gastric bypass in morbidly obese adolescents. Surg Obes Relat Dis. 2007;3:147–52.
Papasavas PK, Hayetian FD, Caushaj PF, et al. Outcome analysis of laparoscopic Roux-en-Y gastric bypass for morbid obesity. The first 116 cases. Surg Endosc. 2002;16:1653–7.
Nguyen NT, Ho HS, Palmer LS, et al. A comparison study of laparoscopic versus open gastric bypass for morbid obesity. J Am Chem Soc. 2000;191:149–55.
Nguyen NT, Goldman C, Rosenquist CJ, et al. Laparoscopic versus open gastric bypass: a randomized study of outcomes, quality of life, and costs. Ann Surg. 2001;234:279–91.
Nguyen NT, Lee SL, Goldman C, et al. Comparison of pulmonary function and postoperative pain after laparoscopic versus open gastric bypass: a randomized trial. J Am Chem Soc. 2001;192:469–76.
Luján JA, Frutos MD, Hernández Q, et al. Laparoscopic versus open gastric bypass in the treatment of morbid obesity: a randomized prospective study. Ann Surg. 2004;239:433–7.
Serafini F, Anderson W, Ghassemi P, et al. The utility of contrast studies and drains in the management of patients after Roux-en-Y gastric bypass. Obes Surg. 2002;12:34–8.
Shah S, Shah V, Ahmed AR, et al. Imaging in bariatric surgery: service set-up, post-operative anatomy and complications. Br J Radiol. 2011;84:101–11.
Sims TL, Mullican MA, Hamilton EC, et al. Routine upper gastrointestinal Gastrografin swallow after laparoscopic Roux-en-Y gastric bypass. Obes Surg. 2003;13:66–72.
Singh R, Fisher BL. Sensitivity and specificity of postoperative upper GI series following gastric bypass. Obes Surg. 2003;13:73–5.
Doraiswamy A, Rasmussen JJ, Pierce J, et al. The utility of routine postoperative upper GI series following laparoscopic gastric bypass. Surg Endosc. 2007;21:2159–62.
Carter JT, Tafreshian S, Campos GM, et al. Routine upper GI series after gastric bypass does not reliably identify anastomotic leaks or predict stricture formation. Surg Endosc. 2007;21:2172–7.
Hamilton EC, Sims TL, Hamilton TT, et al. Clinical predictors of leak after laparoscopic Roux-en-Y gastric bypass for morbid obesity. Surg Endosc. 2003;17:679–84.
Lyass S, Khalili TM, Cunneen S, et al. Radiological studies after laparoscopic Roux-en-Y gastric bypass: routine or selective? Am Surg. 2004;70:918–21.
McCarty TM, Arnold DT, Lamont JP, et al. Optimizing outcomes in bariatric surgery: outpatient laparoscopic gastric bypass. Ann Surg. 2005;242:494–501.
Elliott JA, Patel VM, Kirresh A, et al. Fast-track laparoscopic bariatric surgery: a systematic review. Updat Surg. 2013;65:85–94.
Zevin B, Aggarwal R, Grantcharov TP. Simulation-based training and learning curves in laparoscopic Roux-en-Y gastric bypass. Br J Surg. 2012;99:887–95.
National Institute of Health and Care Excellence. Obesity: guidance on the prevention, identification, assessment and management of overweight and obesity in adults and children. [CG43]. London: National Institute for Health and Care Excellence; 2006.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240:205–13.
Ballesta C, Berindoague R, Cabrera M, et al. Management of anastomotic leaks after laparoscopic Roux-en-Y gastric bypass. Obes Surg. 2008;18:623–30.
Fobi MAL, Lee H, Holness R, et al. Gastric bypass operation for obesity. World J Surg. 1998;22:925–35.
Madan AK, Speck KE, Ternovits CA, et al. Outcome of a clinical pathway for discharge within 48 hours after laparoscopic gastric bypass. Am J Surg. 2006;192:399–402.
Spanjersberg WR, Reurings J, Keus F, et al. Fast track surgery versus conventional recovery strategies for colorectal surgery. Cochrane Database Syst Rev. 2011;2:CD007635.
Wind J, Polle SW, Fung Kon Jin PHP, et al. Systematic review of enhanced recovery programmes in colonic surgery. Br J Surg. 2006;93:800–9.
Varadhan KK, Neal KR, Dejong CHC, et al. The enhanced recovery after surgery (ERAS) pathway for patients undergoing major elective open colorectal surgery: a meta-analysis of randomized controlled trials. Clin Nutr. 2010;29:434–40.
Adamina, Kehlet, Tomlinson, et al. Enhanced recovery pathways optimize health outcomes and resource utilization: a meta-analysis of randomized controlled trials in colorectal surgery. Surgery. 2011;149:830–40.
Warschkow R, Tarantino I, Folie P, et al. C-reactive protein 2 days after laparoscopic gastric bypass surgery reliably indicates leaks and moderately predicts morbidity. J Gastrointest Surg. 2012;16:1128–35.
Csendes A. Clinical predictors of leak after laparoscopic Roux-en-Y gastric bypass for morbid obesity. Surg Endosc. 2004;18:559.
Acknowledgments
The authors would like the acknowledge the invaluable help and assistance that has been provided by Ann Horsfall, Lyndsay Keeley, Maureen Sugden, Carol Thornton, Maria Fowler, Wendy Bartle, Anna Tchaikosky and Suzanne Wynne-Jones at Spire Leeds Hospital during the development of the surgery programme and care protocols. The senior author would particularly like to thank Mikael Stokel, Goran Lundergaardh and Claus Riber for providing bariatric surgical training at Hamlet Hospital in Copenhagen, Denmark.
Conflicts of Interest
All authors declare no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pike, T.W., White, A.D., Snook, N.J. et al. Simplified Fast-Track Laparoscopic Roux-en-Y Gastric Bypass. OBES SURG 25, 413–417 (2015). https://doi.org/10.1007/s11695-014-1408-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-014-1408-6