ABSTRACT
BACKGROUND
Prescription opioid analgesic use has quintupled recently. Evidence linking opioid use with depression emanates from animal models and studies of persons with co-occurring substance use and major depression. Little is known about depressogenic effects of opioid use in other populations.
OBJECTIVE
The purpose of this study was to determine whether prescription opioids are associated with increased risk of diagnosed depression.
DESIGN
Retrospective cohort study, new user design.
PATIENTS
Medical record data from 49,770 US Department of Veterans Affairs (VA) health care system patients with no recent (24-month) history of opioid use or a diagnosis of depression in 1999 and 2000.
MAIN MEASURES
Propensity scores were used to control for bias by indication, and the data were weighted to balance the distribution of covariates by duration of incident opioid exposure. Cox proportional hazard models with adjustment for painful conditions were used to estimate the association between duration of prescription opioid use and the subsequent risk of development of depression between 2001 and 2007.
KEY RESULTS
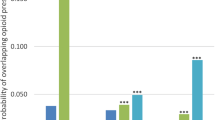
Of 49,770 patients who were prescribed an opioid analgesic, 91 % had a prescription for < 90 days, 4 % for 90–180 days, and 5 % for > 180 days. Compared to patients whose prescription was for < 90 days, the risk of depression increased significantly as the duration of opioid prescription increased (HR = 1.25; 95 % CI: 1.05–1.46 for 90–180 days, and HR = 1.51; 95 % CI:1.31–1.74 for > 180 days).
CONCLUSIONS
In this sample of veterans with no recent (24-month) history of depression or opioid analgesic use, the risk of development of depression increased as the duration of opioid analgesic exposure increased. The potential for depressogenic effect should be considered in risk-benefit discussions, and patients initiating opioid treatment should be monitored for development of depression.




Similar content being viewed by others
REFERENCES
Hall AJ, Logan JE, Toblin RL, et al. Patterns of abuse among unintentional pharmaceutical overdose fatalities. JAMA. 2008;300:2613–2620.
Caudill-Slosberg MA, Schwartz LM, Woloshin S. Office visits and analgesic prescriptions for musculoskeletal pain in US: 1980 vs 2000. Pain. 2004;109:514–9.
Ballantyne JC, Mao J. Opioid therapy for chronic pain. N Engl J Med. 2003;349:1943–53.
Cicero T, Inciardi JA, Munoz A. Trends in abuse of Oxycontin and other opioid analgesics in the United States 2002–2004. J Pain. 2005;6:662–72.
Kluger J. The new drug crisis: addiction by prescription. Time 2010:46–9.
Cole BE. The need for chronic opioids to treat persistent noncancer pain. Gen Hosp Psychiatry. 2011;33:419–22.
Morrison RS, Magaziner J, Gilbert M, Koval KJ, McLaughlin MA, Orosz G, Strauss E, Siu AL. Relationship between pain and opioid analgesics on the development of delirium following hip fracture. J Gerontol A Biol Sci Med Sci. 2003;58:76–81.
Results from the 2010 National Survey on Drug Use and Health. In: Administration SAMHSA, ed. Rockville, MD: Substance Abuse and Mental Health Services Administration; 2011.
Dodrill CL, Helmer DA, Kosten TR. Prescription pain medication dependence. Am J Psychiatry. 2011;168:466–71.
Department of Health & Human Services CfDCaP. Unintentional Drug Poisoning in the United States; 2010.
Jackson SW. Melancholia and depression: from hippocratic times to modern times. New Haven, CT: Yale University Press; 1986.
Pfeiffer A, Brantl V, Herz A, Emrich HM. Psychotomimesis mediated by kappa opiate recepters. Science. 1986;233:774–6.
Grattan A, Sullivan M, Saunders K, Campbell C, Von Korff M. Depression and prescription opioid misuse among chronic opioid therapy recipients with no history of substance abuse. Ann Fam Med. 2012;10:304–11.
Reid MC, Engles-Horton LL, Weber MB, Kerns RD, Rogers EL, O’Connor PG. Use of opioid medications for chronic noncancer pain syndromes in primary care. J Gen Intern Med. 2002;17:173–9.
Sullivan MD, Edlund MJ, Zhang L, Unutzer J, Wells KB. Association between mental health disorders, problem drug use, and regular prescription opioid use. Arch Intern Med. 2006;166:2087–93.
Braden JB, Sullivan MD, Ray GT, et al. Trends in long-term opioid therapy for noncancer pain among persons with a history of depression. Gen Hosp Psych. 2009;31:564–70.
Volkow ND. Drug abuse and mental illness: progress in understanding comorbidity. Am J Psychiatry. 2001;158:1181–3.
Edlund M, Martine BC, Fan MY, Brennan Braden J, Deveries A, Sullivan MD. An analysis of heavy utilizers of opioids for chronic noncancer pain in the TROUP study. J Pain Symptom Manage. 2010;40:279–89.
Volkow ND. The reality of comorbidity: depression and drug abuse. Biol Psychiatry. 2004;56:714–7.
Oxycodone and acetaminophen: drug information. In: Lexicomp, Inc; 2012.
Diagnostic and Statistical Manual of Mental Disorders, Text Revision (DSM-IV-TR). Fourth Edition. Washington DC: American Psychiatric Association; 2000.
Fishbain D, Cutler R, Rosomoff H, Rosomoff RS. Chronic pain-associated depression: antecedent or consequence of chronic pain? A review. Clin J Pain. 1997;13:116–37.
Heinze G, Juni P. An overview of the objectives and the approaches to propensity score analysis. Eur Heart J. 2011;32:1704–8.
Frayne SM, Miller DR, Sharkansky EJ, Jackson VW, Wang F, Halanych JH, Berlowitz DR, Kader B, Rosen CS, Keane TM. Using administrative data to identify mental illness: what approach is best? American Journal of Medical Quality 2010;25[1]:42–50.
Solberg LI, Engebretson KI, Sperl-Hillen JM, Hroscikoski MC, O'Connor PJ. Are claims data accurate enough to identify patients for performance measures or quality improvement? The case of diabetes, heart disease, and depression. American Journal of Medical Quality 2006;21[4]:238-245.
Rosenbaum PR, Rubin DB. The central role of the propensity score in observational studies for causal effects. Biometrika. 1983;70:41–55.
Williamson E, Morley R, Lucas A, Carpenter J. Propensity scores: From naive enthusiasm to inituitive understanding. Stat Methods Med Res. 2012;21:273–93.
Cole SR, Hernan MA. Constructing inverse probability weights for marginal structural models. Am J Epidemiol. 2008;168:656–64.
Curtis LH, Hammill BG, Eisenstein EL, Kramer JM, Anstrom KJ. Using inverse probability-weighted estimators in comparative effectiveness analysis with observational databases. Med Care. 2007;45:S103–7.
Kilpatrick RD, Gilberston D, Brookhart MA, Polley E, Rothman KJ, Bradbury BD. Exploring large weight deletion and the ability to balance confounders when using inverse probability of treatment weighting in the presence of rate treatment decisions. Pharmacoepidemiol Drug Saf. 2013;22:111–21.
Seal KH, Shi Y, Cohen G, et al. Association of mental health disorders with prescription opioids and high-risk opioid use in US Veterans of Iraq and Afghanistan. JAMA. 2012;307:940–7.
Healy D. Pharmageddon. Berkley and Los Angeles: University of California Press; 2010.
Hyman SE, Malenka RC, Nestler EJ. Neural mechanisms of addiction: the role of reward-related learning and memory. Annu Rev Neurosci. 2006;29:565–98.
Robinson TE, Kolb B. Structural plasticity associated with exposure to drugs of abuse. Neuropharmacology. 2004;47:33–46.
Spanagel R, Shipenberg TS. Modulation of morphine-induced sensitization by endogenous kappa opioid systems in the rat. Neurosci Lett. 1993;153:232–6.
George S, Murali V, Pullickal R. Review of neuroendocrine correlates of chronic opiate misuse: dysfunctions and pathophysiological mechanisms. Addic Dis Treat. 2005;4:99–109.
Schaffer CB, Nordahl TE, Schaffer LC, Howe J. Mood-elevating effects of opioid analgesics in patients with bipolar disorder. J Neuropsychiatry Clin Neurosci. 2007;19:449–52.
Schneeweiss S. Sensitivity analysis and external adjustment for unmeasured confounders in epidemiologic database studies of therapeutics. Pharmacoepidemiol Drug Saf. 2006;15:291–303.
Psaty BM, Koepsell TD, Lin D, et al. Assessment and control for confounding by indication in obsrvational studies. J Am Geriatr Soc. 1999;47:749–54.
Acknowledgements
This work was supported by a VA HSR&D Career Development Award-2 granted to Jeffrey F. Scherrer, Ph.D. The funding agency had no role in the design or conduct of the study, data analysis and interpretation, preparation of the manuscript, and review or approval of the manuscript. Dr. Scherrer had full access to all the data in the study and takes responsibility for data integrity and the accuracy of the data analysis.
Conflict of Interest
The authors declare that they do not have a conflict of interest.
Funding Source
Veteran’s Administration Career Development Award to Dr. Scherrer
Statement of Authorship
All authors had access to aggregate data and contributed to writing the manuscript.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
e-Table 1
ICD-9-CM codes used to define diagnoses (DOCX 16 kb)
Rights and permissions
About this article
Cite this article
Scherrer, J.F., Svrakic, D.M., Freedland, K.E. et al. Prescription Opioid Analgesics Increase the Risk of Depression. J GEN INTERN MED 29, 491–499 (2014). https://doi.org/10.1007/s11606-013-2648-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-013-2648-1