ABSTRACT
BACKGROUND
In an effort to prevent medical errors, it has been recommended that all healthcare organizations implement a standardized approach to communicating patient information during transitions of care between providers. Most research on these transitions has been conducted in the inpatient setting, with relatively few studies conducted in the outpatient setting.
OBJECTIVES
To develop a structured transfer of care program in an academic outpatient continuity practice and evaluate whether this program improved patient safety as measured by the documented completion of patient care tasks at 3 months post-transition.
DESIGN
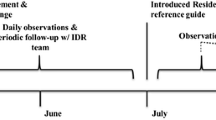
Graduating residents and the corresponding incoming interns inheriting their continuity patient panels were randomized to the pilot structured transfer group or the standard transfer group. The structured transfer group residents were asked to complete written and verbal sign-outs with their interns; the standard transfer group residents continued the current standard of care.
PARTICIPANTS
Thirty-two resident-intern pairs in an academic internal medicine residency program in New York City.
MAIN MEASURES
Three months after the transition, study investigators evaluated whether patient care tasks assigned by the graduating residents had been successfully completed by the interns in both groups. In addition, follow-up appointments, continuity of care and house officer satisfaction with the sign-out process were evaluated.
KEY RESULTS
Among patients seen during the first 3 months, the clinical care tasks were more likely to be completed by interns in the structured group (73 %, n = 49) versus the standard group (46 %, n = 28) (adjusted OR 3.21; 95 % CI 1.55–6.62; p = 0.002). This was further enhanced if the intern who saw the patient was also the assigned primary care provider (adjusted OR 4.26; 95 % CI 1.7–10.63; p = 0.002).
CONCLUSIONS
A structured outpatient sign-out improved the odds of follow-up of important clinical care tasks after the year-end resident clinic transition. Further efforts should be made to improve residents’ competency with regard to sign-outs in the ambulatory setting.

Similar content being viewed by others
REFERENCES
Joint Commission. Improving America’s hospitals: The joint Commission’s annual report on quality and safety [Internet]; 2007. Available from: http://www.jointcommissionreport.org/pdf/JC_2006_Annual_Report.pdf. accessed 8/6/12.
Hand-off Communications Project [Internet]; 2009. Available from: http://www.centerfortransforminghealthcare.org/assets/4/6/CTH_HOC_Fact_Sheet.pdf accessed 8/6/12.
Horwitz LI, Krumholz HM, Green ML, Huot SJ. Transfers of patient care between house staff on internal medicine wards: a national survey. Arch Intern Med. 2006;166(11):1173–7.
Boockvar K, Fishman E, Kyriacou C, Monias A, Gavi S, Cortes T. Adverse events due to discontinuations in drug use and dose changes in patients transferred between acute and long-term care facilities. Arch Intern Med. 2004;164(5):545.
Burton MC, Kashiwagi DT, Kirkland LL, Manning D, Varkey P. Gaining efficiency and satisfaction in the handoff process. J Hosp Med. 2010;5(9):547–52.
Roy MJ, Herbers JE, Seidman A, Kroenke K. Improving patient satisfaction with the transfer of care. A randomized controlled trial. J Gen Intern Med. 2003;18(5):364–9.
Young JQ, Pringle Z, Wachter RM. Improving follow-up of high-risk psychiatry outpatients at resident year-end transfer. Jt Comm J Qual Patient Saf. 2011;37(7):300–8.
Roy MJ, Kroenke K, Herbers JE Jr. When the physician leaves the patient: predictors of satisfaction with the transfer of care in a primary care clinic. J Gen Intern Med. 1995;10(4):206–10.
Young JQ, Eisendrath SJ. Enhancing patient safety and resident education during the academic year-end transfer of outpatients: lessons from the suicide of a psychiatric patient. Acad Psychiatry. 2011;35(1):54–7.
Young JQ, Wachter RM. Academic year-end transfers of outpatients from outgoing to incoming residents: an unaddressed patient safety issue. JAMA. 2009;302(12):1327–9.
Wayne JD, Tyagi R, Reinhardt G, Rooney D, Makoul G, Chopra S, et al. Simple standardized patient handoff system that increases accuracy and completeness. J Surg Educ. 2008;65(6):476–85.
Solet DJ, Norvell JM, Rutan GH, Frankel RM. Lost in translation: challenges and opportunities in physician-to-physician communication during patient handoffs. Acad Med. 2005;80(12):1094–9.
Borowitz SM, Waggoner-Fountain LA, Bass EJ, Sledd RM. Adequacy of information transferred at resident sign-out (in-hospital handover of care): a prospective survey. Qual Saf Health Care. 2008;17(1):6–10.
Arora V, Johnson J, Lovinger D, Humphrey HJ, Meltzer DO. Communication failures in patient sign-out and suggestions for improvement: a critical incident analysis. Qual Saf Health Care. 2005;14(6):401–7.
Horwitz LI, Moin T, Green ML. Development and implementation of an oral sign-out skills curriculum. J Gen Intern Med. 2007;22(10):1470–4.
Caines LC, Brockmeyer DM, Tess AV, Kim H, Kriegel G, Bates CK. The revolving door of resident continuity practice: identifying gaps in transitions of care. J Gen Intern Med. 2011;26(9):995–8.
Pincavage AT, Ratner S, Prochaska ML, Prochaska M, Oyler J, Davis AM, et al. Outcomes for resident-identified high-risk patients and resident perspectives of year-end continuity clinic handoffs. J Gen Intern Med. 2012;23(2):343–7.
Arora VM, Johnson JK, Meltzer DO, Humphrey HJ. A theoretical framework and competency-based approach to improving handoffs. Qual Saf Health Care. 2008;17(1):11–4.
Gottlieb DJ, Parenti CM, Peterson CA, Lofgren RP. Effect of a change in house staff work schedule on resource utilization and patient care. Arch Intern Med. 1991;151(10):2065–70.
Lofgren RP, Gottlieb D, Williams RA, Rich EC. Post-call transfer of resident responsibility: its effect on patient care. J Gen Intern Med. 1990;5(6):501–5.
Laine C, Goldman L, Soukup JR, Hayes JG. The impact of a regulation restricting medical house staff working hours on the quality of patient care. JAMA. 1993;269(3):374–8.
Petersen LA, Brennan TA, O’Neil AC, Cook EF, Lee TH. Does housestaff discontinuity of care increase the risk for preventable adverse events? Ann Intern Med. 1994;121(11):866–72.
ACKNOWLEDGEMENTS
Paul J. Christos, DrPH, MS Division of Biostatistics and Epidemiology and Department of Public Health Joan and Sanford I. Weill Medical College of Cornell University, New York, New York for his statistical consultative services. The consultation services of the Division of Biostatistics and Epidemiology and Department of Public Health are supported by a CTSC grant (UL1 RR 024996)
Conflict of Interest
The authors declare that they do not have a conflict of interest.
Author information
Authors and Affiliations
Corresponding author
ELECTRONIC SUPPLEMENTARY MATERIAL
Below is the link to the electronic supplementary material.
ESM 1
(PDF 190 kb)
Rights and permissions
About this article
Cite this article
Garment, A.R., Lee, W.W., Harris, C. et al. Development of a Structured Year-End Sign-Out Program in an Outpatient Continuity Practice. J GEN INTERN MED 28, 114–120 (2013). https://doi.org/10.1007/s11606-012-2206-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-012-2206-2