Abstract
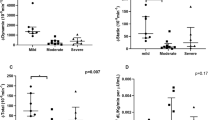
Sleep Apnea is highly prevalent and may contribute to insulin resistance in patients with acromegaly. The primary aim of this study was to assess the impact of sleep apnea treatment with a continuous positive air pressure (CPAP) device on insulin resistance evaluated by hyperinsulinemic euglycemic clamp (HEC). A prospective, randomized, open label, placebo-controlled, crossover study was performed at a tertiary outpatient pituitary center. Twelve acromegalic subjects on somatostatin analogs (SA) with a recent diagnosis of moderate to severe sleep apnea were randomized to CPAP therapy or to nasal dilator adhesive (NDA) with placebo effect for 3 months and then crossed over for another 3 months period without washout. Assessment of HEC, mathematical insulin resistance indexes (HOMA, HOMA2 and QUICKI), GH, IGF-1, HbA1c and free fat acids were performed. A significant reduction on insulin resistance was demonstrated by HEC at the end of the study in patients on CPAP (HEC, pre- and post-CPAP: 4.27 vs. 6.10 mg/Kg/min, P = 0.032). This reduction was not observed in NDA group (HEC, pre- and post-adhesive: 5.53 vs. 5.19 mg/Kg/min, P = 0.455). There was no significant difference on HbA1c or on peripheral insulin resistance indexes in both treatments. CPAP promoted a significant increase on peripheral insulin sensitivity in acromegalic patients with moderate to severe sleep apnea on SA use. Our results support the concept that sleep apnea plays an important role on glucose metabolism. Insulin resistance indexes were unable to detect this finding.


Similar content being viewed by others
References
Alexander L, Appleton D, Hall R, Ross WM, Wilkinson R (1980) Epidemiology of acromegaly in the Newcastle region. Clin Endocrinol (Oxf) 12(1):71–79
Bengtsson BA, Eden S, Ernest I, Oden A, Sjogren B (1988) Epidemiology and long-term survival in acromegaly. A study of 166 cases diagnosed between 1955 and 1984. Acta Med Scand 223(4):327–335
Davi MV, Dalle Carbonare L, Giustina A, Ferrari M, Frigo A, Lo Cascio V, Francia G (2008) Sleep apnoea syndrome is highly prevalent in acromegaly and only partially reversible after biochemical control of the disease. Eur J Endocrinol 159(5):533–540. doi:10.1530/EJE-08-0442
Pelttari L, Polo O, Rauhala E, Vuoriluoto J, Aitasalo K, Hyyppa MT, Kronholm E, Irjala K, Viikari J (1995) Nocturnal breathing abnormalities in acromegaly after adenomectomy. Clin Endocrinol (Oxf) 43(2):175–182
Berg C, Wessendorf TE, Mortsch F, Forsting M, Teschler H, Weischer T, Mann K, Saller B, Herrmann BL (2009) Influence of disease control with pegvisomant on sleep apnoea and tongue volume in patients with active acromegaly. Eur J Endocrinol 161(6):829–835. doi:10.1530/EJE-09-0694
Sze L, Schmid C, Bloch KE, Bernays R, Brandle M (2007) Effect of transsphenoidal surgery on sleep apnoea in acromegaly. Eur J Endocrinol 156(3):321–329. doi:10.1530/eje.1.02340
Tolis G, Angelopoulos NG, Katounda E, Rombopoulos G, Kaltzidou V, Kaltsas D, Protonotariou A, Lytras A (2006) Medical treatment of acromegaly: comorbidities and their reversibility by somatostatin analogs. Neuroendocrinology 83(3–4):249–257. doi:10.1159/000095535
Colao A, Ferone D, Marzullo P, Lombardi G (2004) Systemic complications of acromegaly: epidemiology, pathogenesis, and management. Endocr Rev 25(1):102–152
Attal P, Chanson P (2010) Endocrine aspects of obstructive sleep apnea. J Clin Endocrinol Metab 95(2):483–495. doi:10.1210/jc.2009-1912
Punjabi NM, Ahmed MM, Polotsky VY, Beamer BA, O’Donnell CP (2003) Sleep-disordered breathing, glucose intolerance, and insulin resistance. Respir Physiol Neurobiol 136(2–3):167–178. doi:10.1016/S1569-9048(03)00079-X
Stoohs RA, Facchini F, Guilleminault C (1996) Insulin resistance and sleep-disordered breathing in healthy humans. Am J Respir Crit Care Med 154(1):170–174
Ip MS, Lam B, Ng MM, Lam WK, Tsang KW, Lam KS (2002) Obstructive sleep apnea is independently associated with insulin resistance. Am J Respir Crit Care Med 165(5):670–676
Coughlin SR, Mawdsley L, Mugarza JA, Calverley PM, Wilding JP (2004) Obstructive sleep apnoea is independently associated with an increased prevalence of metabolic syndrome. Eur Heart J 25(9):735–741. doi:10.1016/j.ehj.2004.02.021
Henley DE, Russell GM, Douthwaite JA, Wood SA, Buchanan F, Gibson R, Woltersdorf WW, Catterall JR, Lightman SL (2009) Hypothalamic-pituitary-adrenal axis activation in obstructive sleep apnea: the effect of continuous positive airway pressure therapy. J Clin Endocrinol Metab 94(11):4234–4242. doi:10.1210/jc.2009-1174
Prabhakar NR, Kumar GK (2010) Mechanisms of sympathetic activation and blood pressure elevation by intermittent hypoxia. Respir Physiol Neurobiol 174(1–2):156–161. doi:10.1016/j.resp.2010.08.021
Netzer NC, Stoohs RA, Netzer CM, Clark K, Strohl KP (1999) Using the Berlin Questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med 131(7):485–491
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14(6):540–545
Drager LF, Bortolotto LA, Lorenzi MC, Figueiredo AC, Krieger EM, Lorenzi-Filho G (2005) Early signs of atherosclerosis in obstructive sleep apnea. Am J Respir Crit Care Med 172(5):613–618. doi:10.1164/rccm.200503-340OC
DeFronzo RA, Tobin JD, Andres R (1979) Glucose clamp technique: a method for quantifying insulin secretion and resistance. Am J Physiol 237(3):E214–E223
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28(7):412–419
Wallace TM, Levy JC, Matthews DR (2004) Use and abuse of HOMA modeling. Diabetes Care 27(6):1487–1495
Katz A, Nambi SS, Mather K, Baron AD, Follmann DA, Sullivan G, Quon MJ (2000) Quantitative insulin sensitivity check index: a simple, accurate method for assessing insulin sensitivity in humans. J Clin Endocrinol Metab 85(7):2402–2410
Giustina A, Chanson P, Bronstein MD, Klibanski A, Lamberts S, Casanueva FF, Trainer P, Ghigo E, Ho K, Melmed S (2010) A consensus on criteria for cure of acromegaly. J Clin Endocrinol Metab. doi:10.1210/jc.2009-2670
American Diabetes Association (2010) Diagnosis and classification of diabetes mellitus. Diabetes Care 33(1):S62S–S69. doi:10.2337/dc10-S062
De Menis E, Giustina A, Colao A, Degli Uberti E, Ghigo E, Minuto F, Bogazzi F, Drigo R, Cattaneo A, Aimaretti G (2011) Assessment of the awareness and management of sleep apnea syndrome in acromegaly. The COM.E.TA (Comorbidities Evaluation and Treatment in Acromegaly) Italian Study Group. J Endocrinol Invest 34(1):60–64
Bopparaju S, Surani S (2010) Sleep and diabetes. Int J Endocrinol 2010:759509. doi:10.1155/2010/759509
Harsch IA, Schahin SP, Radespiel-Troger M, Weintz O, Jahreiss H, Fuchs FS, Wiest GH, Hahn EG, Lohmann T, Konturek PC, Ficker JH (2004) Continuous positive airway pressure treatment rapidly improves insulin sensitivity in patients with obstructive sleep apnea syndrome. Am J Respir Crit Care Med 169(2):156–162. doi:10.1164/rccm.200302-206OC
Moller N, Butler PC, Antsiferov MA, Alberti KG (1989) Effects of growth hormone on insulin sensitivity and forearm metabolism in normal man. Diabetologia 32(2):105–110
Baldelli R, Battista C, Leonetti F, Ghiggi MR, Ribaudo MC, Paoloni A, D’Amico E, Ferretti E, Baratta R, Liuzzi A, Trischitta V, Tamburrano G (2003) Glucose homeostasis in acromegaly: effects of long-acting somatostatin analogues treatment. Clin Endocrinol (Oxf) 59(4):492–499. doi:10.1046/j.1365-2265.2003.01876.x
Ferone D, Colao A, van der Lely AJ, Lamberts SW (2000) Pharmacotherapy or surgery as primary treatment for acromegaly? Drugs Aging 17(2):81–92
Ezzat S, Snyder PJ, Young WF, Boyajy LD, Newman C, Klibanski A, Molitch ME, Boyd AE, Sheeler L, Cook DM et al (1992) Octreotide treatment of acromegaly. A randomized, multicenter study. Ann Intern Med 117(9):711–718
Ayuk J, Stewart SE, Stewart PM, Sheppard MC (2002) Long-term safety and efficacy of depot long-acting somatostatin analogs for the treatment of acromegaly. J Clin Endocrinol Metab 87(9):4142–4146
Tzanela M, Vassiliadi DA, Gavalas N, Szabo A, Margelou E, Valatsou A, Vassilopoulos C (2011) Glucose homeostasis in patients with acromegaly treated with surgery or somatostatin analogues. Clin Endocrinol (Oxf). doi:10.1111/j.1365-2265.2011.03996.x
Mazziotti G, Floriani I, Bonadonna S, Torri V, Chanson P, Giustina A (2009) Effects of somatostatin analogs on glucose homeostasis: a metaanalysis of acromegaly studies. J Clin Endocrinol Metab 94(5):1500–1508. doi:10.1210/jc.2008-2332
Brooks B, Cistulli PA, Borkman M, Ross G, McGhee S, Grunstein RR, Sullivan CE, Yue DK (1994) Obstructive sleep apnea in obese noninsulin-dependent diabetic patients: effect of continuous positive airway pressure treatment on insulin responsiveness. J Clin Endocrinol Metab 79(6):1681–1685
Harsch IA, Schahin SP, Bruckner K, Radespiel-Troger M, Fuchs FS, Hahn EG, Konturek PC, Lohmann T, Ficker JH (2004) The effect of continuous positive airway pressure treatment on insulin sensitivity in patients with obstructive sleep apnoea syndrome and type 2 diabetes. Respiration 71(3):252–259. doi:10.1159/000077423
Lam JC, Lam B, Yao TJ, Lai AY, Ooi CG, Tam S, Lam KS, Ip MS (2010) A randomised controlled trial of nasal continuous positive airway pressure on insulin sensitivity in obstructive sleep apnoea. Eur Respir J 35(1):138–145. doi:10.1183/09031936.00047709
Babu AR, Herdegen J, Fogelfeld L, Shott S, Mazzone T (2005) Type 2 diabetes, glycemic control, and continuous positive airway pressure in obstructive sleep apnea. Arch Intern Med 165(4):447–452. doi:10.1001/archinte.165.4.447
Smurra M, Philip P, Taillard J, Guilleminault C, Bioulac B, Gin H (2001) CPAP treatment does not affect glucose-insulin metabolism in sleep apneic patients. Sleep Med 2(3):207–213. doi:10.1016/S1389-9457(00)00079-4
West SD, Nicoll DJ, Wallace TM, Matthews DR, Stradling JR (2007) Effect of CPAP on insulin resistance and HbA1c in men with obstructive sleep apnoea and type 2 diabetes. Thorax 62(11):969–974. doi:10.1136/thx.2006.074351
Coughlin SR, Mawdsley L, Mugarza JA, Wilding JP, Calverley PM (2007) Cardiovascular and metabolic effects of CPAP in obese males with OSA. Eur Respir J 29(4):720–727. doi:10.1183/09031936.00043306
Weaver TE, Maislin G, Dinges DF, Bloxham T, George CF, Greenberg H, Kader G, Mahowald M, Younger J, Pack AI (2007) Relationship between hours of CPAP use and achieving normal levels of sleepiness and daily functioning. Sleep 30(6):711–719
Sharma SK, Agrawal S, Damodaran D, Sreenivas V, Kadhiravan T, Lakshmy R, Jagia P, Kumar A (2011) CPAP for the metabolic syndrome in patients with obstructive sleep apnea. N Engl J Med 365(24):2277–2286. doi:10.1056/NEJMoa1103944
Acknowledgments
We thank Dr. Ana Tereza Santomauro for her expertise and intellectual contributions in the clamp procedure. We thank the staff of the hormonal test room and the sleep laboratory for the help in the execution of the clamps and the polysomnographies. We thank Valéria Sutti Nunnes for performing the FFA assays, and we also thank the patients for participating in this demanding study. This research was supported by Supported by Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP) (protocol number: 2008/10045-3).
Ethical standards
The local ethics committee approved the protocol and all participants gave written, informed consent.
Conflict of interest
Authors declare to have no conflict of interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Duarte, F.H.G., Jallad, R.S., Amaro, A.C.S. et al. The impact of sleep apnea treatment on carbohydrate metabolism in patients with acromegaly. Pituitary 16, 341–350 (2013). https://doi.org/10.1007/s11102-012-0430-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-012-0430-8