Abstract
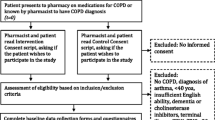
Background Pharmacists can play an important role in identifying and instructing pulmonary patients on their inhalation techniques in their patient contacts when dispensing inhalation medication. Pharmacy dispensing data can be used to identify inappropriate drug use in asthma and chronic obstructive pulmonary disease (COPD) patients. Recent studies found beneficial effects of pharmacy care services in improving drug adherence of pulmonary patients. However, large-scale and rigorous evaluations on pharmacist-led interventions in community care settings to enhance evidence-based drug treatment in patients with asthma and COPD seems to be lacking and results from studies on pharmacist-led interventions for pharmacotherapy improvements are inconsistent. This study evaluated the effectiveness of pharmacist-led interventions on suboptimal drug use patterns with asthma or COPD medication with substantial numbers of pharmacies and patients involved. Setting A prospective cohort study in a group of community pharmacies (intervention group) with a matched control group of Dutch community pharmacies was conducted between May 2011 and February 2012. Algorithms on 19 potential problems with asthma or COPD medication in a national dispensing database were used to signal patients to pharmacists of the intervention group (IG). Methods IG pharmacists selected patients for comprehensive care by a structured program. Changes in problems were measured during 10 months in selected and all users of asthma and COPD medication of IG pharmacies and in compared to a control pharmacies (CG) without the structured program. Primary outcome was reduction of oral high dosage corticosteroids or antibiotics (HDT). Secondary outcomes were changes in the persistence of 19 potential problems in the IG compared to CG. Results In the 107 IG pharmacies, 3,757 patients were selected for comprehensive care from totally 102,497 asthma or COPD patients and compared with 105,507 patients from 105 CG pharmacies. The mean number of HDT decreased in selected IG patients by an additional 0.54 (95 % CI 0.21–0.86) HDT treatments. From the problems with specific COPD and asthma medication, all problems decreased additionally to the CG within the total asthma or COPD population from the IG. Within the selected IG population the following problems decreased additionally for obsolete medication by 35 % (95 % CI 6–54 %), contra-indicated medication by 61 % (95 % CI 38–75 %) and lower use of powder inhalers in elderly patients by 29 % (95 % CI 13–42 %). Conclusion Community pharmacists actively providing comprehensive pharmacy care could improve effective treatment in asthma and COPD patients and thereby decrease the number of prescriptions for exacerbations for these patients.
Similar content being viewed by others
References
Weinberger M, Murray MD, Marrero DG, Brewer N, Lykens M, Harris LE, et al. Effectiveness of pharmacist care for patients with reactive airways disease: a randomized controlled trial. JAMA, J Am Med Assoc. 2002;288(13):1594–602 Epub 2002/09/28.
Braman SS. The global burden of asthma. Chest. 2006;130(1 Suppl):4S–12S Epub 2006/07/15.
Jarab AS, Alqudah SG, Khdour M, Shamssain M, Mukattash TL. Impact of pharmaceutical care on health outcomes in patients with COPD. Int J Clin Pharm. 2012;34(1):53–62 Epub 2011/11/22.
Casas A, Troosters T, Garcia-Aymerich J, Roca J, Hernandez C, Alonso A, et al. Integrated care prevents hospitalisations for exacerbations in COPD patients. Eur Respir J. 2006;28(1):123–30 Epub 2006/04/14.
van Staa TP, Cooper C, Leufkens HG, Lammers JW, Suissa S. The use of inhaled corticosteroids in the United Kingdom and the Netherlands. Respir Med. 2003;97(5):578–85 Epub 2003/05/09.
Pauwels RA, Buist AS, Calverley PM, Jenkins CR, Hurd SS. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease. NHLBI/WHO global initiative for chronic obstructive lung disease (GOLD) workshop summary. Am J Respir Crit Care Med. 2001;163(5):1256–76.
Beney J, Bero LA, Bond C. Expanding the roles of outpatient pharmacists: effects on health services utilisation, costs, and patient outcomes. Cochrane database of systematic reviews (Online). 2000(3):CD000336.
Hesselink AE, Penninx BW, Wijnhoven HA, Kriegsman DM, van Eijk JT. Determinants of an incorrect inhalation technique in patients with asthma or COPD. Scand J Prim Health Care. 2001;19(4):255–60 Epub 2002/02/02.
Mangiapane S, Schulz M, Muhlig S, Ihle P, Schubert I, Waldmann HC. Community pharmacy-based pharmaceutical care for asthma patients. Ann Pharmacother. 2005;39(11):1817–22 Epub 2005/10/13.
Armour C, Bosnic-Anticevich S, Brillant M, Burton D, Emmerton L, Krass I, et al. Pharmacy asthma care program (PACP) improves outcomes for patients in the community. Thorax. 2007;62(6):496–502 Epub 2007/01/26.
Mehuys E, Van Bortel L, De Bolle L, Van Tongelen I, Annemans L, Remon JP, et al. Effectiveness of pharmacist intervention for asthma control improvement. Eur Respir J. 2008;31(4):790–9 Epub 2007/12/21.
Strand LM, Cipolle RJ, Morley PC, Frakes MJ. The impact of pharmaceutical care practice on the practitioner and the patient in the ambulatory practice setting: twenty-five years of experience. Curr Pharm Des. 2004;10(31):3987–4001 Epub 2004/12/08.
Basheti IA, Armour CL, Reddel HK, Bosnic-Anticevich SZ. Long-term maintenance of pharmacists’ inhaler technique demonstration skills. Am J Pharm Educ. 2009;73(2):32.
Kamps AW, van Ewijk B, Roorda RJ, Brand PL. Poor inhalation technique, even after inhalation instructions, in children with asthma. Pediatr Pulmonol. 2000;29(1):39–42 Epub 1999/12/29.
McLean W, Gillis J, Waller R. The BC Community Pharmacy Asthma Study: a study of clinical, economic and holistic outcomes influenced by an asthma care protocol provided by specially trained community pharmacists in British Columbia. Can Respir J. 2003;10(4):195–202 Epub 2003/07/10.
Fischer LR, Scott LM, Boonstra DM, DeFor TA, Cooper S, Elkema MA, et al. Pharmaceutical care for patients with chronic conditions. J Am Pharm Assoc. 2000;40(2):174–80.
Herborg H, Soendergaard B, Froekjaer B, Fonnesbaek L, Jorgensen T, Hepler CD, et al. Improving drug therapy for patients with asthma–part 1: Patient outcomes. J Am Pharm Assoc. 2001;41(4):539–50.
Narhi U, Airaksinen M, Tanskanen P, Enlund H. The effects of a pharmacy-based intervention on the knowledge and attitudes of asthma patients. Patient Educ Couns. 2001;43(2):171–7 Epub 2001/05/23.
Nokela M, Arnlind MH, Ehrs PO, Krakau I, Forslund L, Jonsson EW. The influence of structured information and monitoring on the outcome of asthma treatment in primary care: a cluster randomized study. Respiration. 2010;79(5):388–94 Epub 2009/08/13.
Schulz M, Verheyen F, Muhlig S, Muller JM, Muhlbauer K, Knop-Schneickert E, et al. Pharmaceutical care services for asthma patients: a controlled intervention study. J Clin Pharmacol. 2001;41(6):668–76 Epub 2001/06/14.
Carter BL, Foppe van Mil JW. Comparative effectiveness research: evaluating pharmacist interventions and strategies to improve medication adherence. Am J Hypertens. 2010;23(9):949–55.
Buurma H, de Smet PA, van den Hoff OP, Egberts AC. Nature, frequency and determinants of prescription modifications in Dutch community pharmacies. Br J Clin Pharmacol. 2001;52(1):85–91 Epub 2001/07/17.
Monster TB, Janssen WM, de Jong PE, de Jongvan den Berg LT. Pharmacy data in epidemiological studies: an easy to obtain and reliable tool. Pharmacoepidemiol Drug Saf. 2002;11(5):379–84.
Bereznicki BJ, Peterson GM, Jackson SL, Walters H, Fitzmaurice K, Gee P. Pharmacist-initiated general practitioner referral of patients with suboptimal asthma management. Pharmacy world & science : PWS. 2008;30(6):869–75 Epub 2008/08/06.
Cheung KC dBJ. Apotheker in de WGBO. Praktijk, kennis en verwachtingen van apothekers en apothekersassistenten vóór opname van de apotheker in de WGBO.. 2012 [cited 2007]; Available from: http://www.knmp.nl/downloads/organisatie-regelgeving/organisatie-regelgeving-wet-en-regelgeving/definitief20rapport20wgbo20en20apotheekpraktijk20oktober202007.pdf.
Griens AMGF JJ, Kloon JDL, Lukaart JS, van der Vaart RJ. News and publications. Stichting Farmaceutische Kengetallen 2012; Available from: http://www.sfk.nl/english.
Smeele IJM vWC, van Schayck CP, van der Molen T, Thoonen B, Schermer T, Sachs APE, Muris JWM, Chavannes NH, Kolnaar BGM, Grol MH, Geijer RMM. Guideline for COPD treatment. Huisarts Wetenschap. 2007;50(8):18.
Geijer RMMCN, Muris JWM, Sachs APE, Schermer T, Smeele IJM, Thoonen B, Van der Molen T, van Schayck CP, van Weel C, Kolnaar BGM, Grol MH. Guideline asthma treatment for adults. Huisarts Wetenschap. 2007;50(11):15.
Statistics DAf. Level of urbanity. Available from: http://www.cbs.nl/nl-NL/menu/methoden/toelichtingen/alfabet/p/2009-platteland-toelichting.htm.
Methodology WHOCCfDS. Guidelines for ATC CLassification and DDD Assignment. 2013; Available from: http://www.whocc.no/filearchive/publications/1_2013guidelines.pdf.
Armour CL, Lemay K, Saini B, Reddel HK, Bosnic-Anticevich SZ, Smith LD, et al. Using the community pharmacy to identify patients at risk of poor asthma control and factors which contribute to this poor control. J Asthma. 2011;48(9):914–22 Epub 2011/09/29.
Acknowledgments
The authors wish to thank the KNMP, SFK and GSK for their assistance to perform this study.
Funding
GSK developed the web-based tool and provided a fee of 50 Euro per included patient, with a maximum of 40 patients per asthma or COPD project. The analysis of all data done independent of GSK.
Conflicts of interest
Romy de Groot is employed by GSK. GSK contributed financially to the internship of Stefan Ottebros.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ottenbros, S., Teichert, M., de Groot, R. et al. Pharmacist-led intervention study to improve drug therapy in asthma and COPD patients. Int J Clin Pharm 36, 336–344 (2014). https://doi.org/10.1007/s11096-013-9887-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11096-013-9887-4