Abstract
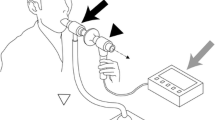
Cough test to screen for silent aspiration (SA) was reported, and the effectiveness was excellent. However, the device was rather large so that the portability was poor. So, the purpose of this study is to investigate the usefulness of a handheld nebulizer for the test and verify the reproducibility of the method. The subjects were 160 patients who were suspected of having dysphagia and underwent videofluorography (VF) or videoendoscopy (VE). They inhaled 1.0 % citric acid-physiologic saline orally for 1 min using a handheld nebulizer, and the examiner observed the number of coughs: more than five coughs was considered as negative (normal), while less than four coughs was regarded as positive. Among the subjects, 70 patients administered the cough test and VF or VE twice or more at some intervals. The k coefficient was calculated in reproducibility. Using the results of the VF or VE examination as the standards, for SA detection, the sensitivity was 0.86, specificity was 0.71, positive predictive value was 0.53, and negative predictive value was 0.93. The k coefficient was 0.79. In conclusion, the handheld nebulizer was useful in the cough test to screen for SA. Furthermore, satisfactory reproducibility was shown.


Similar content being viewed by others
References
Wakasugi Y, Tohara H, Hattori F, Motohashi Y, Nakane A, Goto S, Ouchi Y, Mikushi S, Takeuchi S, Uematsu H. Screening test for silent aspiration at the bedside. Dysphagia. 2008;23:364–70.
Wakasugi Y, Tohara H, Motohashi Y, Tsushima C, Uematsu H. The progress of patients administered the cough test. Dysphagia. 2009;24:469. (abstract).
Sekizawa K, Ujiie Y, Sasaki H. Measurement of cough threshold. Respir Circ. 1992;40:157–9. (in Japanese).
Sekizawa K, Ujiie Y, Itabashi S, Sasaki H, Takishima T. Lack of cough reflex in aspiration pneumonia. Lancet. 1990;335:1228–9.
Arai H, Sato T, Nakajoh K. The standard in decision of appropriateness of ingestion by cough test. A study of nutrition of dyaphagia aged people. 2000; 60–4. (in Japanese)
Tanaka T, Baba T, Saito E, Okui Y, Tohara H, Mizuno M. An investigation of screening test of silent aspiration by cough test: the decision of the concentration of citric acid. Jpn J Dysphagia Rehabil. 2000;4:163. (in Japanese).
Iwata S. Current and attachments of aerosols in the use for allergic laryngitis. Oto-Rhino-Laryngology. 1995;38:169–78. (in Japanese).
Logemann JA. Evalutation and treatment of swallowing disorders. 2nd ed. Austin: Pro-Ed Publishers; 1998.
Langemore SE. Endoscopic evaluation and treatment of swallowing disorders. New York: Thieme Medical Publishers; 2001.
Bastian RW. The videoendoscopic swallowing study: an alternative and partner to the videofluoroscopic swallowing study. Dysphagia. 1993;8:359–67.
Kidder TM, Langmore SE, Martin JW. Indications and techniques of endoscopy in evaluation of cervical dysphagia: comparison with radiographic techniques. Dysphagia. 1994;9:256–61.
Wu CH, Hsiao TY, Chen JC, Chang YC, Lee SY. Evaluation of swallowing safety with fiberoptic endoscope: comparison with videofluoroscopic technique. Laryngoscope. 1997;107:396–401.
Langmore SE. Evalutation of oropharyngeal dysphagia: which diagnostic tool is superior? Curr Opin Otolaryngol Head Neck Surg. 2003;11:485–9.
Langmore SE, Schatz K, Olson N. Endoscopic and videofluoroscopic evaluations of swallowing and aspiration. Ann Otol Rhinol Laryngol. 1991;100:678–81.
Leder SB, Sasaki CT, Burrell MI. Fiberoptic endoscopic evaluation of dysphagia to identify silent aspiration. Dysphagia. 1998;13:19–21.
Hafner G, Neuhuber A, Hirtenfelder S, Schmedler B, Eckel HE. Fiberoptic endoscopic evaluation of swallowing in intensive care unit patients. Laryngology. 2008;265:441–6.
Kelly AM, Drinnan MJ, Leslie P. Assessing penetration and aspiration: how do videofluoroscopy and fiberoptic endoscopic evaluation of swallowing compare? Laryngoscope. 2007;117:1723–7.
Horner J, Massey W. Silent aspiration following stroke. Neurology. 1988;38:317–9.
Leder SB, Suiter DM, Green BG. Silent aspiration risk is volume-dependent. Dysphagia. 2011;26:304–9.
Rosenbek JC, Robbins JA, Roecker EB, Coyle JL, Wood JL. A penetration–aspiration scale. Dysphagia. 1996;11:93–8.
Dhand R, Guntur VP. How best to deliver aerosol medications to mechanically ventilated patients. Clin Chest Med. 2008;29:277–96.
Morice AH, Higgins KS, Yeo WW. Adaption of cough reflex with different types of stimulation. Eur Respir J. 1992;5:841–7.
Ari A, Areabi H, Fink JB. Evalutation of aerosol generator devices at 3 locations in humidified and non-humidified circuits during adult mechanical ventilation. Respir Care. 2010;55:837–44.
Khatri L, Taylor KM, Craig DQ, Palin K. An assessment of jet and ultrasonic nebulizers for the delivery of lactate dehydrogenase solutions. Int J Pharm. 2001;227:21–131.
Arzhavitina A, Steckel H. Surface active drugs significantly alter the drug output rate from medical nebulizers. Int J Pharm. 2010;384:128–36.
Pedersen KM, Handlos VN, Heslet L, Kristensen HG. Factors influencing the in vitro deposition of tobramycin aerosol: a comparison of an ultrasonic nebulizer and a high-frequency vibrating mesh nebulizer. J Aerosol Med. 2006;19:175–83.
Dicpinigaitis PV. Experimentally induced cough. Pulm Pharmacol Ther. 2007;20:319–24.
Schmidt D, Jorres RA, Magnussen H. Citric acid-induced cough thresholds in normal subjects, patients with bronchial asthma, and smokers. Eur J Med Res. 1997;29:384–8.
Auffarth B, de Monchy JG, van der Mark TW, Postma DS, Koeter GH. Citric acid cough threshold and airway responsiveness in asthmatic patients and smokers with chronic airflow obstruction. Thorax. 1991;46(9):638–42.
Barber CM, Curran AD, Bradshaw LM, Morice AH, Rawbone R, Fishwick D. Reproducibility and validity of a Yan-style portable citric acid cough challenge. Pulm Pharmacol Ther. 2005;18:177–80.
Fontana GA, Pantaleo T. Repeatability of cough-related variables during fog challenges at threshold and suprathreshold stimulus intensity in humans. Eur Respir J. 1999;13:1447–50.
Fontana GA, Pantaleo T. A noninvasive electromyographic study on threshold and intensity of cough in humans. Eur Respir J. 1997;10:983–9.
Acknowledgments
This study was supported in part by Grants-in-Aid for young Scientists (B) from Japan Society for the Promotion of Science (21792145).
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wakasugi, Y., Tohara, H., Nakane, A. et al. Usefulness of a handheld nebulizer in cough test to screen for silent aspiration. Odontology 102, 76–80 (2014). https://doi.org/10.1007/s10266-012-0085-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10266-012-0085-y