Abstract
Purpose
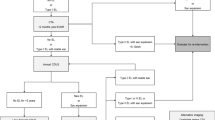
To compare the results of endovascular treatment for unilateral iliac occlusion in types B and D, and confirm its validity for type D.
Methods
Between 2000 and 2011, 108 patients underwent endovascular treatment for unilateral iliac occlusion. 77 were categorized as type B for occlusion of common iliac artery (CIA) or external iliac artery (EIA) and 31 were categorized as type D for occlusion of both CIA and EIA. The initial success rates, procedure time, penetration time, amount of contrast media used, complication rates, and cumulative primary patency rates were determined and compared between these groups.
Results
Between type D and B groups, the initial success rates were 87.1 % (type D) and 89.6 % (type B) (p = 0.9316). The procedure time was 137.0 ± 55.5 and 97.2 ± 47.2 min (p < 0.05). The penetration time was 49.1 ± 40.6 and 31.6 ± 30.1 min (p < 0.05). The amount of contrast agent used was 193.9 ± 103.1 and 156.5 ± 85.0 ml (p = 0.0722). The complication rates were 6.5 and 3.9 % (p = 0.8491). The cumulative primary patency rates, at 1, 3, and 5 years were 91, 85, and 85 % and 100, 96, and 93 %.
Conclusion
Endovascular treatment can be indicated for unilateral occlusion of both CIA and EIA categorized as type D.



Similar content being viewed by others
References
Norgren L, Hiatt WR, Dormandy JA, Nehler MR, Harris KA, Fowkes FG, TASC II Working Group. Inter-Society Consensus for the management of peripheral arterial disease (TASC II). J Vasc Surg. 2007;45(Suppl S):S5–67.
Leville CD, Kashyap VS, Clair DG, Bena JF, Lyden SP, Greenberg RK, O’Hara PJ, Sarac TP, Ouriel K. Endovascular management of iliac artery occlusions: extending treatment to Trans-Atlantic Inter-Society Consensus class C and D patients. J Vasc Surg. 2006;43(1):32–9.
Sixt S, Alawied AK, Rastan A, Schwarzwälder U, Kleim M, Noory E, Schwarz T, Frank U, Müller C, Hauk M, Beschorner U, Nazary T, Bürgelin K, Hauswald K, Leppänen O, Neumann FJ, Zeller T. Acute and long-term outcome of endovascular therapy for aortoiliac occlusive lesions stratified according to the TASC classification: a single-center experience. J Endovasc Ther. 2008;15(4):408–16.
Koizumi A, Kumakura H, Kanai H, Araki Y, Kasama S, Sumino H, Ichikawa S, Kurabayashi M. Ten-year patency and factors causing restenosis after endovascular treatment of iliac artery lesions. Circ J. 2009;73(5):860–6.
Balzer JO, Gastinger V, Ritter R, Herzog C, Mack MG, Schmitz-Rixen T, Vogl TJ. Percutaneous interventional reconstruction of the iliac arteries: primary and long-term success rate in selected TASC C and D lesions. Eur Radiol. 2006;16(1):124–31.
Ichihashi S, Higashiura W, Itoh H, Sakaguchi S, Nishimine K, Kichikawa K. Long-term outcomes for systematic primary stent placement in complex iliac artery occlusive disease classified according to Trans-Atlantic Inter-Society Consensus (TASC)-II. J Vasc Surg. 2011;53(4):992–9.
Kaneoka Y, Maeda A, Sugimoto M, Isogai M, Ishibashi H. Quality of life and the venous function of the lower limb after harvest of autologous external iliac vein grafts: a clinical follow-up study. Surg Today. 2013;43(11):1254–60.
Rutherford RB, Baker JD, Ernst C, Johnston KW, Porter JM, Ahn S, Jones DN. Recommended standards for reports dealing with lower extremity ischemia: revised version. J Vasc Surg. 1997;26(3):517–38.
Staniloae CS, Mody KP, Yadav SS, Han SY, Korabathina R. Endoluminal treatment of peripheral chronic total occlusions using the Crosser® recanalization catheter. J Invasive Cardiol. 2011;23(9):359–62.
Krishnamurthy VN, Eliason JL, Henke PK, Rectenwald JE. Intravascular ultrasound-guided true lumen reentry device for recanalization of unilateral chronic total occlusion of iliac arteries: technique and follow-up. Ann Vasc Surg. 2010;24(4):487–97 [Epub 2010 Apr 2].
Al-Ameri H, Shin V, Mayeda GS, Burstein S, Matthews RV, Kloner RA, Shavelle DM. Peripheral chronic total occlusions treated with subintimal angioplasty and a true lumen re-entry device. J Invasive Cardiol. 2009;21(9):468–72.
Paraskevas KI, Giannoukas AD, Mikhailidis DP. Renal function impairment in peripheral arterial disease: an important parameter that should not be neglected. Ann Vasc Surg. 2009;23(5):690–9.
Ozkan U, Oguzkurt L, Tercan F. Technique, complication, and long-term outcome for endovascular treatment of iliac artery occlusion. Cardiovasc Intervent Radiol. 2010;33(1):18–24.
Gandini R, Fabiano S, Chiocchi M, Chiappa R, Simonetti G. Percutaneous treatment in iliac artery occlusion: long-term results. Cardiovasc Intervent Radiol. 2008;31(6):1069–76.
Carnevale FC, De Blas M, Merino S, Egaña JM, Caldas JG. Percutaneous endovascular treatment of chronic iliac artery occlusion. Cardiovasc Intervent Radiol. 2004;27(5):447–52.
Uher P, Nyman U, Lindh M, Lindblad B, Ivancev K. Long-term results of stenting for chronic iliac artery occlusion. J Endovasc Ther. 2002;9(1):67–75.
AbuRahma AF, Hayes JD, Flaherty SK, Peery W. Primary iliac stenting versus transluminal angioplasty with selective stenting. J Vasc Surg. 2007;46(5):965–70.
van Adrichem LN, van Berge Henegouwen DP, Lobach HJ, van der Werken C. The femoro-femoral cross-over bypass. Neth J Surg. 1991;43(3):67–70.
Fahal AH, McDonald AM, Marston A. Femorofemoral bypass in unilateral iliac artery occlusion. Br J Surg. 1989;76(1):22–5.
Aronow WS, Ahn C. Prevalence of coexistence of coronary artery disease, peripheral arterial disease, and atherothrombotic brain infarction in men and women ≥62 years of age. Am J Cardiol. 1994;74(1):64–5.
Rits J, van Herwaarden JA, Jahrome AK, Krievins D, Moll FL. The incidence of arterial stent fractures with exclusion of coronary, aortic, and non-arterial settings. Eur J Vasc Endovasc Surg. 2008;36(3):339–45.
Lopez JF, Magne JL, Champetier J. The femoral artery and flexion of the hip joint. Surg Radiol Anat. 1989;11(4):275–81.
Ballotta E, Gruppo M, Mazzalai F, Da Giau G. Common femoral artery endarterectomy for occlusive disease: an 8-year single-center prospective study. Surgery. 2010;147(2):268–74.
Conflict of interest
Naokazu Miyamoto and other co-authors have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Miyamoto, N., Kawasaki, R., Fukuda, T. et al. Endovascular treatment for unilateral chronic total occlusions of the iliac artery categorized as TASC II type D lesions. Surg Today 45, 162–167 (2015). https://doi.org/10.1007/s00595-014-0883-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-014-0883-7