Abstract
Background
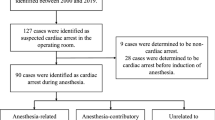
Emergency surgery itself induces high risk for postoperative mortality and morbidities; however, it remains unknown which concomitant pathological conditions of emergency surgeries are causative factors of deteriorating outcomes. This study examined the causal factors of postoperative mortality and morbidity in cases of emergency surgery.
Methods
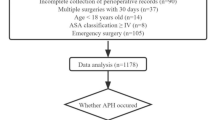
Patients undergoing emergency surgery from January to December 2007 were enrolled in this retrospective cohort study. Causal relationships were analyzed by stepwise multivariate logistic regression analysis between possible independent factors (sex, age, kind of surgical department, timing of surgery, duration of surgery, blood transfusion, deteriorated consciousness level, shock state, abnormal coagulate state, and history of hypertension, diabetes, ischemic heart disease, chronic obstructive pulmonary disease, renal failure, and anemia) and postoperative mortality or morbidities (failure of removal of tracheal tube after operation, tracheotomy, cerebral infarction, massive hemorrhage, severe hypotension, severe hypoxemia, and severe arrhythmia during or after surgery).
Results
Shock, deteriorated consciousness level, chronic obstructive lung disease, and ischemic heart disease were significant risk factors for mortality (OR 14.2, 7.9, 6.4, and 3.8, respectively), and deteriorated consciousness level, blood transfusion, shock, chronic obstructive lung disease, diabetes, cardiovascular surgery, and operation longer than 2 h were significant risk factors for morbidity (OR 19.1, 3.3, 3.0, 2.5, 2.4, 2.4, and 1.8, respectively).
Conclusion
State of shock, deteriorated consciousness level, chronic obstructive lung disease, ischemic heart disease, hemorrhage requiring blood transfusion, age over 80 years, cardiovascular surgery, surgeries at night, and surgeries of duration more than 2 h cause patients to be strongly susceptible to postoperative mortality or morbidity in emergency surgeries.
Similar content being viewed by others
References
Copeland GP, Jones D, Walters M. POSSUM: a scoring system for surgical audit. Br J Surg. 1991;78:355–60.
Gaston MS, Amin AK, Clayton RA, Brenkel IJ. Does a history of cardiac disease or hypertension increase mortality following primary elective total hip arthroplasty? Surgeon. 2007;5:260–5.
Markus PM, Martell J, Leister I, Horstmann O, Brinker J, Becker H. Predicting postoperative morbidity by clinical assessment. Br J Surg. 2005;92:101–6.
Campillo-Soto A, Flores-Pastor B, Soria-Aledo V, Candel-Arenas M, Andrés-García B, Martín-Lorenzo JG, Aguayo-Albasini JL. The POSSUM scoring system: an instrument for measuring quality in surgical patients. Cir Esp. 2006;80:395–9.
Sutton R, Bann S, Brooks M, Sarin S. The Surgical Risk Scale as an improved tool for risk-adjusted analysis in comparative surgical audit. Br J Surg. 2002;89:763–8.
Prause G, Ratzenhofer-Komenda B, Smolle-Juettner F, Krenn H, Pojer H, Toller W, Voit H, Offner A, Smolle J. Operations on patients deemed “unfit for operation and anaesthesia:” what are the consequences? Acta Anaesthesiol Scand. 1998;42:316–22.
Hobson SA, Sutton CD, Garcea G, Thomas WM. Prospective comparison of POSSUM and P-POSSUM with clinical assessment of mortality following emergency surgery. Acta Anaesthesiol Scand. 2007;51:94–100.
Sørensen LT, Malaki A, Wille-Jørgensen P, Kallehave F, Kjaergaard J, Hemmingsen U, Møller LN, Jørgensen T. Risk factors for mortality and postoperative complications after gastrointestinal surgery. J Gastrointest Surg. 2007;11:903–10.
Chavanon O, Costache V, Bach V, Kétata A, Durand M, Hacini R, Thony F, Blin D. Preoperative predictive factors for mortality in acute type A aortic dissection: an institutional report on 217 consecutives cases. Interact Cardiovasc Thorac Surg. 2007;6:43–6.
Lee CC, Chang IJ, Lai YC, Chen SY, Chen SC. Epidemiology and prognostic determinants of patients with bacteremic cholecystitis or cholangitis. Am J Gastroenterol. 2007;102:563–9.
Ramachandran R, Hegde T. Chronic subdural hematomas–causes of morbidity and mortality. Surg Neurol. 2007;67:367–72.
Treacy PJ, Reilly P, Brophy B. Emergency neurosurgery by general surgeons at a remote major hospital. ANZ J Surg. 2005;75:852–7.
Tao LS, Mackenzie CR, Charlson ME. Predictors of postoperative complications in the patient with diabetes mellitus. J Diabetes Complicat. 2008;22:24–8.
Mohammadi S, Dagenais F, Mathieu P, Kingma JG, Doyle D, Lopez S, Baillot R, Perron J, Charbonneau E, Dumont E, Metras J, Desaulniers D, Voisine P. Long-term impact of diabetes and its comorbidities in patients undergoing isolated primary coronary artery bypass graft surgery. Circulation. 2007;116:I220–5.
Greillier L, Thomas P, Loundou A, Doddoli C, Badier M, Auquier P, Barlési F. Pulmonary function tests as a predictor of quantitative and qualitative outcomes after thoracic surgery for lung cancer. Clin Lung Cancer. 2007;8:554–61.
Filsoufi F, Rahmanian PB, Castillo JG, Chikwe J, Carpentier A, Adams DH. Early and late outcomes of cardiac surgery in patients with moderate to severe preoperative renal dysfunction without dialysis. Interact Cardiovasc Thorac Surg. 2008;7:90–5.
Scott BH, Seifert FC, Grimson R. Blood transfusion is associated with increased resource utilisation, morbidity and mortality in cardiac surgery. Ann Card Anaesth. 2008;11:15–9.
Dionigi G, Rovera F, Boni L, Carrafiello G, Recaldini C, Mangini M, Laganà D, Bacuzzi A, Dionigi R. The impact of perioperative blood transfusion on clinical outcomes in colorectal surgery. Surg Oncol. 2007;16:S177–82.
Mynster T, Christensen IJ, Moesgaard F, Nielsen HJ. Effects of the combination of blood transfusion and postoperative infectious complications on prognosis after surgery for colorectal cancer. Danish RANX05 Colorectal Cancer Study Group. Br J Surg. 2000;87:1553–62.
Hirzalla O, Emous M, Ubbink DT, Legemate D. External validation of the Glasgow Aneurysm Score to predict outcome in elective open abdominal aortic aneurysm repair. J Vasc Surg. 2006;44:712–6.
Kocer B, Surmeli S, Solak C, Unal B, Bozkurt B, Yildirim O, Dolapci M, Cengiz O. Factors affecting mortality and morbidity in patients with peptic ulcer perforation. J Gastroenterol Hepatol. 2007;22:565–70.
Silberman S, Oren A, Klutstein MW, Merin O, Fink D, Bitran D. Surgery for ischemic mitral regurgitation: results and long-term follow-up. Harefuah. 2007;146:841–843, 911.
Açil T, Cölkesen Y, Türköz R, Sezgin AT, Baltali M, Gülcan O, Demircan S, Yildirir A, Ozin B, Müderrisoğlu H. Value of preoperative echocardiography in the prediction of postoperative atrial fibrillation following isolated coronary artery bypass grafting. Am J Cardiol. 2007;100:1383–6.
Bose AK, Aitchison JD, Dark JH. Aortic valve replacement in octogenarians. J Cardiothorac Surg. 2007;2:33.
Ford PN, Thomas I, Cook TM, Whitley E, Peden CJ. Determinants of outcome in critically ill octogenarians after surgery: an observational study. Br J Anaesth. 2007;99:824–9.
Carmody IC, Romero J, Velmahos GC. Day for night: should we staff a trauma center like a nightclub? Am Surg. 2002;68:1048–51.
Luyt CE, Combes A, Aegerter P, Guidet B, Trouillet JL, Gibert C, Chastre J. Mortality among patients admitted to intensive care units during weekday day shifts compared with “off” hours. Crit Care Med. 2007;35:3–11.
Dimick JB, Swoboda SM, Pronovost PJ, Lipsett PA. Effect of nurse-to-patient ratio in the intensive care unit on pulmonary complications and resource use after hepatectomy. Am J Crit Care. 2001;10:376–82.
Dzankic S, Pastor D, Gonzalez C, Leung JM. The prevalence and predictive value of abnormal preoperative laboratory tests in elderly surgical patients. Anesth Analg. 2001;93:249–50.
Glance LG, Lustik SJ, Hannan EL, Osler TM, Mukamel DB, Qian F, Dick AW. The Surgical Mortality Probability Model: derivation and validation of a simple risk prediction rule for noncardiac surgery. Ann Surg. 2012;255:696–702.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Matsuyama, T., Iranami, H., Fujii, K. et al. Risk factors for postoperative mortality and morbidities in emergency surgeries. J Anesth 27, 838–843 (2013). https://doi.org/10.1007/s00540-013-1639-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-013-1639-z